The clinical information regarding How to Safely Transition Between Contraceptive Methods in this article has been rigorously verified against the latest guidelines from the American College of Obstetricians and Gynecologists (ACOG) and primary research from databases like PubMed. This piece was reviewed for accuracy and patient-centric clarity and was last updated in October 2023.
Introduction
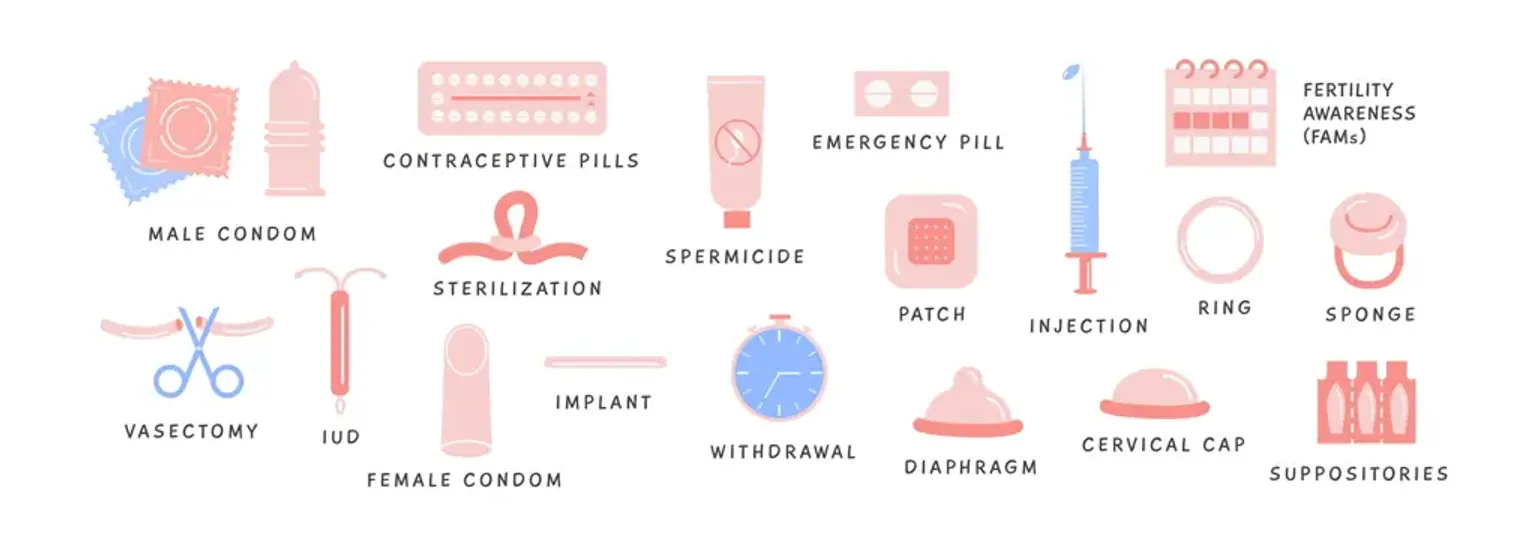
introductionChanging your birth control method is a common and often necessary decision for managing your health, lifestyle, or family planning goals. The process can feel complex, with concerns about potential gaps in protection, side effects, or choosing the right new method. This guide provides a clear, step-by-step framework to ensure you can transition between contraceptive methods safely, effectively, and with confidence.
What is the Safest Way to Switch Birth Control Methods?
what-is-the-safest-way-to-switch-birth-control-methodsThe safest way to switch birth control is to consult with a gynecologist and follow a no-gap or quick-start method, which ensures continuous protection against pregnancy. This involves starting the new method immediately or within a specific timeframe advised by your doctor, often overlapping the old and new methods for a short period. The core principle is to prevent any window of time where you are not protected.
Key Principles for a Safe Transition:
Consult a Professional: A gynecologist can assess your medical history, discuss the pros and cons of new options, and provide a personalized switching plan.
Understand Your Methods: Know whether you are moving between hormonal methods, from hormonal to non-hormonal, or vice-versa. This dictates the switching protocol.
Use Backup Protection: When in doubt, use a backup barrier method like condoms for at least the first seven days of a new hormonal method, or as directed by your healthcare provider.
How Do I Switch Between Specific Contraceptive Methods?
how-do-i-switch-between-specific-contraceptive-methodsThe exact process depends on the methods you are switching from and to. Below are detailed instructions for common transition scenarios. Always confirm this guidance with your doctor, as your personal health profile may require adjustments.
Switching From a Combination Pill, Patch, or Ring to Another
switching-from-a-combination-pill-patch-or-ring-to-anotherThis is generally the most straightforward transition.
The No-Gap Method: Finish your current pack of pills including placebo pills, patch week, or ring-free week. Start the new method on the day you would have normally started your next pack, patch, or ring. You will have continuous contraceptive coverage.
Switching From a Combination Method (Pill/Patch/Ring) to an IUD
switching-from-a-combination-method-(pillpatchring)-to-an-iudHormonal IUD (e.g., Mirena, Kyleena): The IUD can be inserted at any time during your cycle. If inserted within the first seven days of your period starting, it is effective immediately. If inserted at any other time, you must use a backup method like condoms for seven days post-insertion. Many doctors advise continuing your old method for seven days after the IUD is placed.
Non-Hormonal Copper IUD (e.g., Paragard): This IUD is effective immediately upon insertion. It can be placed at any time in your cycle. You can stop your old hormonal method on the day the copper IUD is inserted.
Switching From a Combination Method to the Contraceptive Implant (e.g., Nexplanon)
switching-from-a-combination-method-to-the-contraceptive-implant-(e.g.-nexplanon)The implant can be inserted at any time.
For Immediate Effectiveness: The implant should be inserted within the first five days of your menstrual period.
If Inserted at Another Time: You must continue using a backup barrier method for seven days after insertion. You can stop your old method on the day of insertion, but the backup method is critical.
Switching From a Combination Method to the Contraceptive Shot (Depo-Provera)
switching-from-a-combination-method-to-the-contraceptive-shot-(depo-provera)For Immediate Effectiveness: Receive your first shot within the first seven days after your period starts.
Quick Start Method: You can get the shot at any time. If you do, you must use a backup method for the next seven days. You can stop your other hormonal method once you receive the shot.
How Do You Switch From a Hormonal to a Non-Hormonal Method?
how-do-you-switch-from-a-hormonal-to-a-non-hormonal-methodTransitioning away from hormones requires careful timing to avoid pregnancy.
To a Copper IUD: As mentioned, the copper IUD is effective immediately. You can stop your hormonal method on the day of insertion.
To Barrier Methods (Condoms, Diaphragm, Cervical Cap): Stop your hormonal method at the end of a pack/cycle. You must start using the barrier method every time you have sex immediately. There is no grace period. Many women experience changes in their menstrual cycle after stopping hormonal birth control, which can take a few months to regulate.
"I was nervous about switching from the pill to an IUD, worried about the procedure and side effects. My gynecologist in Seoul walked me through everything, and the transition was seamless. Having continuous protection without a daily pill has been incredibly freeing." – an anonymous patient, USA.
What Are the Side Effects of Changing Contraception?
what-are-the-side-effects-of-changing-contraceptionYour body may need time to adjust to a new hormonal profile or device.
Common Side Effects When Starting a New Hormonal Method: You may experience breakthrough bleeding or spotting, breast tenderness, nausea, or headaches. These symptoms often subside within the first 1-3 months as your body adjusts.
Side Effects with IUDs: With a hormonal IUD, you may have irregular bleeding initially, which often leads to lighter or no periods over time. With a copper IUD, you may experience heavier periods and more cramping, especially in the first 3-6 months.
Coming Off Hormones: When switching to a non-hormonal method, your natural cycle will return. This could mean the return of pre-birth control symptoms like acne, heavier periods, or premenstrual syndrome (PMS).
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaFor a safe and professionally guided transition, consulting with a specialist is paramount. The clinics below are recognized for their expertise in women's health, contraception management, and gynecological care in South Korea.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
Second Spring Women's Clinic | Vaginal aesthetic treatments and general OBGYN care | Gangnam-gu, Seoul, South Korea | ||
Seoul Miz Hospital | Comprehensive women's healthcare and OBGYN services | Gangdong-gu, Seoul, South Korea | ||
MariaPlus (Songpa) Fertility Hospital | Fertility treatments and reproductive endocrinology | Songpa-gu, Seoul, South Korea | ||
Asan Medical Center | Full-spectrum medical care including advanced OBGYN | Songpa-gu, Seoul, South Korea | ||
Goeunbit Women’s Clinic | General OBGYN services and women's wellness | Songpa-gu, Seoul, South Korea | ||
MizMedi Hospital | Specialized women's and children's hospital, i-Dream Fertility Center | Gangseo-gu, Seoul, South Korea | ||
HI Fertility Clinic | High-success rate fertility treatments and family planning | Gangseo-gu, Seoul, South Korea | ||
Helen Women’s Obstetrics & Gynecology Clinic | General and aesthetic gynecological procedures | Songpa-gu, Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaThe following table outlines related procedures and their typical costs in South Korea, providing context for comprehensive women's healthcare planning. Costs are estimates and can vary by clinic and individual case.
Treatment/Procedure Name | Treatment Duration | Hospitalization? | Avg Cost Range (USD) in S. Korea | Contact |
|---|---|---|---|---|
Contraception and Miscarriage Care | 1-2 hours | Not Needed | $200 - $1,500 | |
Menstrual and Hormonal Disorders Treatments | 2-4 hours | Not Needed | $150 - $500 | |
Endometriosis Management | 1-3 hours | Not Needed | $1,000 - $8,000 | |
Hormone Replacement Therapy (HRT) | 1-4 hours | Not Needed | $200 - $600 | |
Gynecological Surgery | 1-4 hours | Needed (1-3 days) | $3,000 - $15,000 | |
Labiaplasty | 1-2 hours | Not Needed | $2,500 - $5,000 | |
Vaginal Tightening (Surgical/Laser) | 1-2 hours | Not Needed | $2,000 - $7,000 | |
Vaginal Mucosa Correction Injections | 30-45 mins | Not Needed | $1,000 - $2,500 | |
Clitoral Pop Filler Treatments | 30 mins | Not Needed | $800 - $2,000 | |
Vulvar Whitening | 30 mins | Not Needed | $300 - $700 |
Frequently Asked Questions About Changing Contraception
frequently-asked-questions-about-changing-contraceptionThis section addresses common follow-up questions patients have when planning a switch.
1. Do I need to see a doctor to change my contraception?
1.-do-i-need-to-see-a-doctor-to-change-my-contraceptionYes, it is highly recommended. A doctor can ensure the new method is safe for you, rule out contraindications, and provide the correct protocol for switching to maintain effectiveness and minimize side effects. Methods like IUDs, implants, and shots require a clinical visit.
2. Can I switch birth control without a gap in protection?
2.-can-i-switch-birth-control-without-a-gap-in-protectionYes, absolutely. This is the primary goal of a well-managed transition. Following a quick start or no-gap method, often by starting the new method before the old one is stopped or immediately after, ensures continuous contraceptive coverage.
3. How long does it take for your body to adjust to new birth control?
3.-how-long-does-it-take-for-your-body-to-adjust-to-new-birth-controlMost women find that their bodies take about three months to fully adjust to a new hormonal contraceptive. During this time, side effects like irregular spotting, mood changes, or breast tenderness are more common but typically resolve.
4. What happens to my period when I switch birth control?
4.-what-happens-to-my-period-when-i-switch-birth-controlYour period will likely change. Switching between hormonal methods might cause temporary irregularities before settling into the new method's typical bleeding pattern. Switching from a hormonal to a non-hormonal copper IUD may result in heavier, more painful periods. Switching from hormonal to no method will cause your natural cycle to return, which may be different from what you experienced on hormonal birth control.
5. Should I "take a break" from hormonal birth control?
5.-should-i-"take-a-break"-from-hormonal-birth-controlThere is no medical reason to take a break from hormonal contraception if you are healthy and not experiencing problematic side effects. Unplanned pregnancies often occur during these breaks. Any decision to stop should be made with a plan for an alternative contraceptive method.
6. Can switching birth control cause weight gain?
6.-can-switching-birth-control-cause-weight-gainWhile many women are concerned about this, large-scale studies have not found a direct causal link between most modern hormonal contraceptives and significant weight gain. The Depo-Provera shot is one exception where some users do experience a modest weight increase. Any changes are typically minor and can be related to fluid retention or lifestyle factors.
Plan Your Safe Transition: Consult with a Specialist Today!
plan-your-safe-transition:-consult-with-a-specialist-todayMaking an informed choice about your contraceptive health is an empowering step. To ensure your transition is seamless, safe, and tailored to your body's needs, professional guidance is essential. By consulting with an expert, you can move forward with a new method confidently, knowing you are fully protected. We can connect you with leading women's health specialists in South Korea. The process is transparent and supported by a dedicated Care Manager who assists you from the initial inquiry to your post-treatment care, ensuring a smooth and stress-free experience. Start Your Confidential Inquiry With CloudHospital and receive a personalized plan for your contraceptive needs.