The clinical information regarding Anal Fissures in this article has been rigorously verified against the latest practice guidelines from the American Society of Colon and Rectal Surgeons (ASCRS) and primary research from databases like PubMed. This piece was reviewed for accuracy and patient-centric clarity and was last updated in October 2023.
Introduction
introductionAn anal fissure is a common and often painful condition characterized by a small tear or crack in the delicate lining of the anal canal. While frequently mistaken for hemorrhoids, fissures have distinct causes and symptoms. They can affect people of all ages, from infants to older adults, and significantly impact daily quality of life due to severe pain during and after bowel movements. This guide offers a comprehensive, medically-grounded overview for those seeking to understand, manage, and treat this condition effectively.
What is an Anal Fissure?
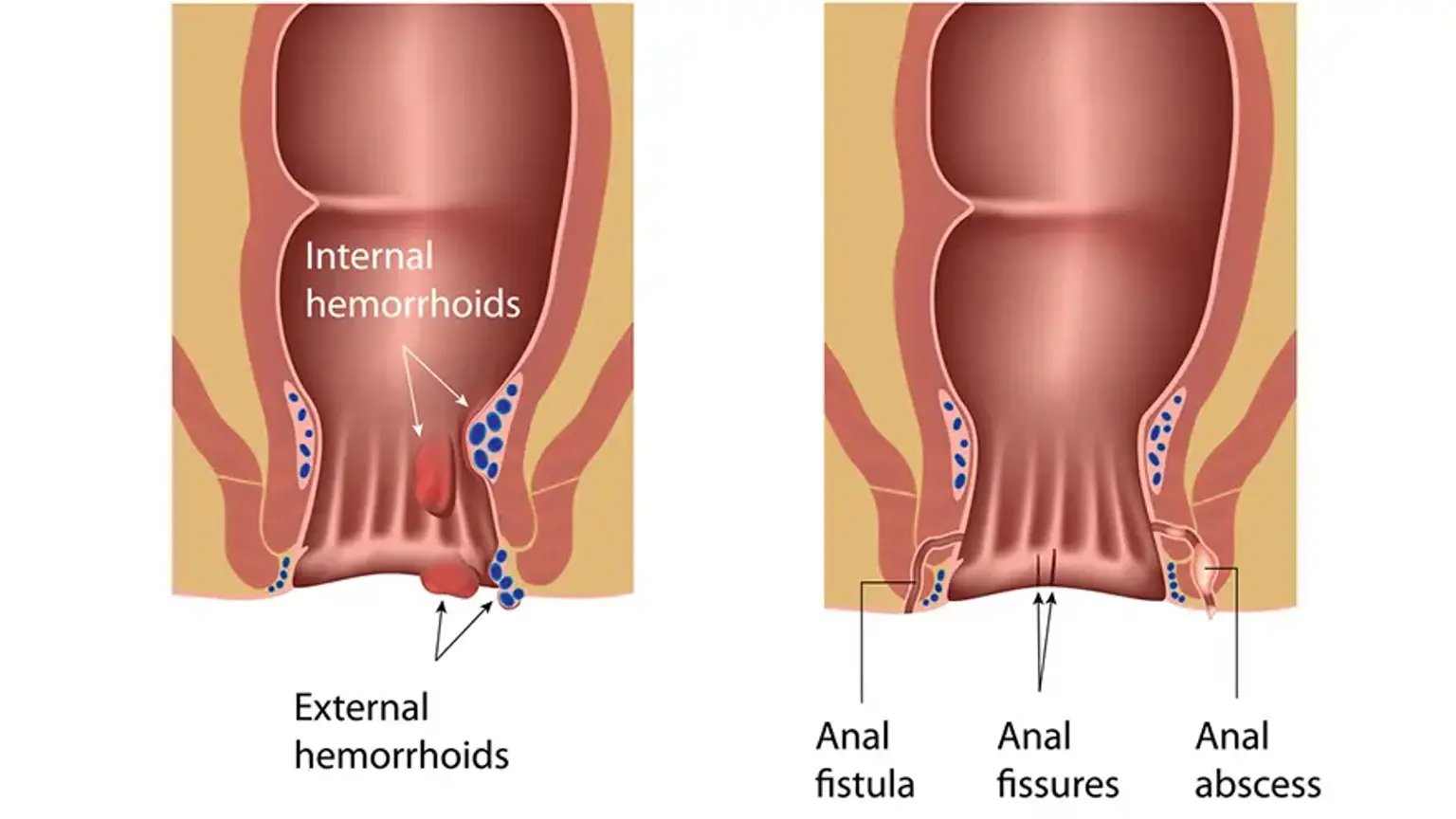
what-is-an-anal-fissureAn anal fissure is a longitudinal split in the anoderm, the specialized skin lining the lower portion of the anal canal. These tears most commonly occur on the posterior midline of the anus. Fissures are categorized as either acute or chronic.
Acute Anal Fissure: A newly formed tear that appears as a fresh, superficial cut. With proper care, most acute fissures heal within a few weeks.
Chronic Anal Fissure: A fissure that fails to heal after 8 to 12 weeks. Chronic fissures are often deeper, may have exposed underlying sphincter muscle fibers, and can develop a small external skin tag sentinel pile and an enlarged internal papilla.
What Are the Common Causes and Risk Factors?
what-are-the-common-causes-and-risk-factorsThe primary cause of an anal fissure is trauma to the anal canal lining. This damage is typically initiated by factors that stretch or irritate the anoderm.
Hard, Dry Stools: Passing large or hard stools is the most frequent cause, physically tearing the lining.
Chronic Diarrhea: Frequent, watery stools can irritate and inflame the anal skin, making it more susceptible to tearing.
Childbirth: The strain of vaginal delivery can cause trauma to the perineal and anal areas.
Anal Intercourse: This can stretch the anal canal and cause tearing.
Inflammatory Bowel Disease (IBD): Conditions like Crohn's disease can cause inflammation that leads to atypical fissures, which may be located off the midline or be multiple in number.
Reduced Blood Flow: Decreased blood flow to the anorectal area, which can occur with age or in certain medical conditions, may impair healing and contribute to the development of chronic fissures.
Overly Tight Anal Sphincter Muscles Hypertonia: High resting pressure in the internal anal sphincter can both increase the risk of tearing and reduce blood flow, hindering the healing process.
What are the Symptoms and Signs of an Anal Fissure?
what-are-the-symptoms-and-signs-of-an-anal-fissureThe symptoms of an anal fissure are distinct and can be quite severe, often prompting an individual to seek medical care.
Sharp, Tearing Pain: A severe, sharp, or knife-like pain is felt during a bowel movement. This is the hallmark symptom.
Prolonged, Deep Burning Pain: Following the bowel movement, a deep, gnawing, or burning pain can last for several minutes to many hours. This is caused by spasms of the internal anal sphincter muscle.
Bright Red Blood: You may see a small amount of bright red blood on the toilet paper or on the surface of the stool. Bleeding from a fissure is typically not heavy.
Visible Tear: In some cases, a small crack in the skin around the anus may be visible.
Skin Tag: A small lump or skin tag, known as a sentinel pile, may develop at the edge of a chronic fissure.
Itching or Irritation: The area around the anus may become itchy or irritated.
How is an Anal Fissure Diagnosed?
how-is-an-anal-fissure-diagnosedA diagnosis is typically made based on the patient's description of symptoms and a gentle physical examination. A colorectal surgeon or proctologist will carefully inspect the perianal skin. Often, by gently separating the buttocks, the fissure can be seen.
In most cases of acute fissures, an internal digital rectal exam or anoscopy is avoided initially due to the severe pain it would cause. If the diagnosis is uncertain, if bleeding is significant, or if an underlying condition like IBD is suspected, a physician might recommend a colonoscopy or sigmoidoscopy once the acute pain has subsided.
What are the Treatment Options for Anal Fissures?
what-are-the-treatment-options-for-anal-fissuresTreatment aims to break the cycle of pain, sphincter spasm, and re-injury to allow the tear to heal. Over 90% of acute fissures heal with conservative, non-surgical measures.
Conservative & Lifestyle Management
conservative-and-lifestyle-managementThis is the first line of treatment.
High-Fiber Diet: Consuming 25-35 grams of fiber daily from fruits, vegetables, and supplements helps soften stool.
Increased Fluid Intake: Adequate water intake is crucial for preventing hard stools.
Sitz Baths: Soaking the rectal area in warm water for 10-15 minutes, two to three times a day especially after bowel movements, helps relax the anal sphincter, increase blood flow, and relieve pain.
Topical Anesthetics: Over-the-counter creams like lidocaine can provide temporary pain relief.
Medical Non-Surgical Treatments
medical-(non-surgical)-treatmentsIf conservative measures are not enough, a doctor may prescribe:
Topical Vasodilators: Prescription creams like topical nitroglycerin or calcium channel blockers diltiazem, nifedipine are applied to the area. They work by relaxing the internal anal sphincter and increasing blood flow to promote healing.
Botulinum Toxin Injection: An injection of Botox into the internal anal sphincter temporarily paralyzes the muscle, relieving spasm and allowing the fissure to heal. This is a highly effective option for chronic fissures, with success rates often exceeding 80% .
Surgical Interventions
surgical-interventionsSurgery is reserved for chronic fissures that have not responded to other treatments.
Lateral Internal Sphincterotomy (LIS): This is the gold standard surgical procedure. A surgeon makes a small incision in the internal anal sphincter muscle to release the tension. LIS has a very high success rate over 95% but carries a small risk of permanent, minor incontinence to gas or liquid stool.
How Can I Manage Life with an Anal Fissure?
how-can-i-manage-life-with-an-anal-fissure"The pain was a sharp, dreadful feeling I started to fear every single day. Just the thought of going to the bathroom created so much anxiety. Getting the diagnosis and finally understanding that simple changes like a sitz bath and more fiber could provide real relief was a turning point. It gave me back control." – an anonymous patient, South Korea.
Managing an anal fissure focuses on consistency. Adhering to a high-fiber diet, staying hydrated, and avoiding straining are the cornerstones of both healing and prevention. Using prescribed medications as directed is critical for breaking the pain-spasm cycle.
When Should I See a Doctor?
when-should-i-see-a-doctorYou should consult a healthcare professional if you experience any of the following:
Severe rectal pain during bowel movements.
Pain that persists for hours after a bowel movement.
Rectal bleeding, even a small amount.
A fissure that does not improve after 1-2 weeks of home care.
Symptoms that are accompanied by fever, significant bleeding, or changes in bowel habits.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaSouth Korea is home to world-renowned medical centers with advanced Gastroenterology and Colorectal Surgery departments, offering expert diagnosis and treatment for conditions like anal fissures.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
Asan Medical Center | Comprehensive care in all specialties, including a world-class Gastroenterology & Colorectal Surgery department. | Songpa-gu, Seoul,South Korea | ||
Seoul St. Mary's Hospital-Seocho | Leading research and treatment in digestive diseases and minimally invasive colorectal surgery. | Seocho-gu, Seoul,South Korea | ||
Seoul National University Hospital- ganganm district | Prestigious academic medical center with a top-tier Gastroenterology division known for complex case management. | Gangnam-gu, Seoul, South Korea | ||
Kangdong Sacred Heart Hospital | Strong focus on patient-centered care with advanced diagnostic and therapeutic endoscopy services. | Gangdong-gu, Seoul, South Korea | ||
H Plus Yangji Hospital | Specialized centers for digestive health offering comprehensive screening and treatment programs. | Gwanak-gu, Seoul, South Korea | ||
Soon Chun Hyang University Hospital Seoul | Renowned for its Digestive Disease Center and expertise in endoscopic procedures. | Yongsan-gu, Seoul, South Korea | ||
Kyung Hee University Hospital At Gangdong | Integration of Eastern and Western medicine with a strong Gastroenterology department. | Gangdong-gu, Seoul, South Korea | ||
Hanyang University Seoul Hospital | Leading hospital for robotic surgery and advanced treatments for gastrointestinal and colorectal diseases. | Seongdong-gu, Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaThe following are common gastroenterological procedures. While not all are direct treatments for anal fissures, they represent the advanced capabilities of the recommended medical centers.
Treatment/Procedure Name | Treatment Duration | Hospitalization? | Avg Cost Range (USD) in S. Korea | Contact |
|---|---|---|---|---|
Liver Transplantation | 4-8 hours | Needed | $130,000 - $180,000 | |
ERCP with Biliary or Pancreatic Stenting | 30-90 mins | Needed (1-2 days) | $4,000 - $7,000 | |
Endoscopic Ultrasound (EUS) with Fine Needle Aspiration | 30-60 mins | Not Needed | $2,500 - $4,500 | |
Bariatric Surgery (Gastric Bypass, Sleeve Gastrectomy) | 1-3 hours | Needed (2-4 days) | $15,000 - $25,000 | |
Colon Cancer Surgery (Colectomy) | 2-4 hours | Needed (3-7 days) | $18,000 - $30,000 | |
Inflammatory Bowel Disease (IBD) Biologic Therapy | 30 mins - 2 hours | Not Needed | $5,000 - $15,000 | |
Upper GI Endoscopy with Biopsy (EGD) | 15-30 mins | Not Needed | $600 - $1,200 | |
Colonoscopy with Polypectomy | 30-60 mins | Not Needed | $800 - $1,500 | |
Pancreatic Surgery (Whipple Procedure) | 4-7 hours | Needed (7-14 days) | $45,000 - $65,000 | |
Hepatitis C Antiviral Therapy | 2-4 hours | Not Needed | $20,000 - $40,000 |
What Are Common Questions About Anal Fissures?
what-are-common-questions-about-anal-fissures1. How long does an anal fissure take to heal?
1.-how-long-does-an-anal-fissure-take-to-healAn acute fissure typically heals within a few weeks with conservative treatment. A chronic fissure, one that lasts longer than 8-12 weeks, often requires medical intervention like prescription creams or surgery and can take several more weeks to fully resolve even with successful treatment.
2. Can an anal fissure be a sign of something more serious?
2.-can-an-anal-fissure-be-a-sign-of-something-more-seriousYes, in some cases. While most fissures are caused by constipation or local trauma, persistent fissures or those in unusual locations can be a sign of an underlying medical condition like Crohn's disease, ulcerative colitis, a weakened immune system, or, very rarely, cancer. A thorough medical evaluation is necessary if a fissure does not heal as expected.
3. Can diet significantly affect my anal fissure?
3.-can-diet-significantly-affect-my-anal-fissureAbsolutely. Diet is a cornerstone of both treatment and prevention. A diet high in fiber and fluids is critical to producing soft, easy-to-pass stools, which prevents stretching and tearing of the anal lining. Avoiding large amounts of constipating foods like processed cheese and red meat can also be beneficial.
4. Is an anal fissure the same as a hemorrhoid?
4.-is-an-anal-fissure-the-same-as-a-hemorrhoidNo, they are different conditions. A fissure is a tear in the skin, causing sharp pain and minimal bleeding. A hemorrhoid is a swollen vein inside or outside the anus, which typically causes itching, dull discomfort, and sometimes painless bleeding. They can coexist, but the primary symptoms are different.
5. How can I prevent anal fissures from recurring?
5.-how-can-i-prevent-anal-fissures-from-recurringPrevention is key. The most effective strategies are maintaining a high-fiber diet, drinking plenty of water, avoiding straining during bowel movements, and addressing constipation or diarrhea promptly. If you have had a fissure before, being vigilant about these habits is the best way to prevent another one.
6. When is surgery necessary for an anal fissure?
6.-when-is-surgery-necessary-for-an-anal-fissureSurgery, specifically a lateral internal sphincterotomy (LIS), is considered when a fissure is chronic and has failed to heal despite several weeks or months of non-surgical treatments like dietary changes, sitz baths, and medicated creams. It is the most effective treatment for chronic fissures.
Take the First Step Towards Relief and Healing Now!
take-the-first-step-towards-relief-and-healingLiving with the pain of an anal fissure can be debilitating, but effective and definitive treatments are available. The world-class gastroenterology and colorectal departments in South Korea, including those partnered with Cloud Hospital, offer a path to recovery through expert diagnosis and a full spectrum of care options. By reaching out, you gain access to a seamless, transparent process guided by a dedicated Care Manager who will support you from your initial questions to your post-recovery care and Start Your Confidential Inquiry receive a personalized treatment plan and begin your journey back to comfort and health.