The clinical information regarding Genital Herpes in this article has been rigorously verified against the latest guidelines from the Centers for Disease Control and Prevention (CDC) and primary research from databases like PubMed. This piece was reviewed for accuracy and patient-centric clarity and was last updated in November 2023.
Introduction
introductionGenital herpes is a common sexually transmitted infection that affects millions of people globally. An estimated 13.2% of people aged 15-49 worldwide are living with the virus. Receiving a diagnosis can feel overwhelming, but understanding the condition is the first step toward effective management and living a full, healthy life. This guide offers a comprehensive, medically-backed overview for those seeking to understand, treat, and manage genital herpes.
What is Genital Herpes?
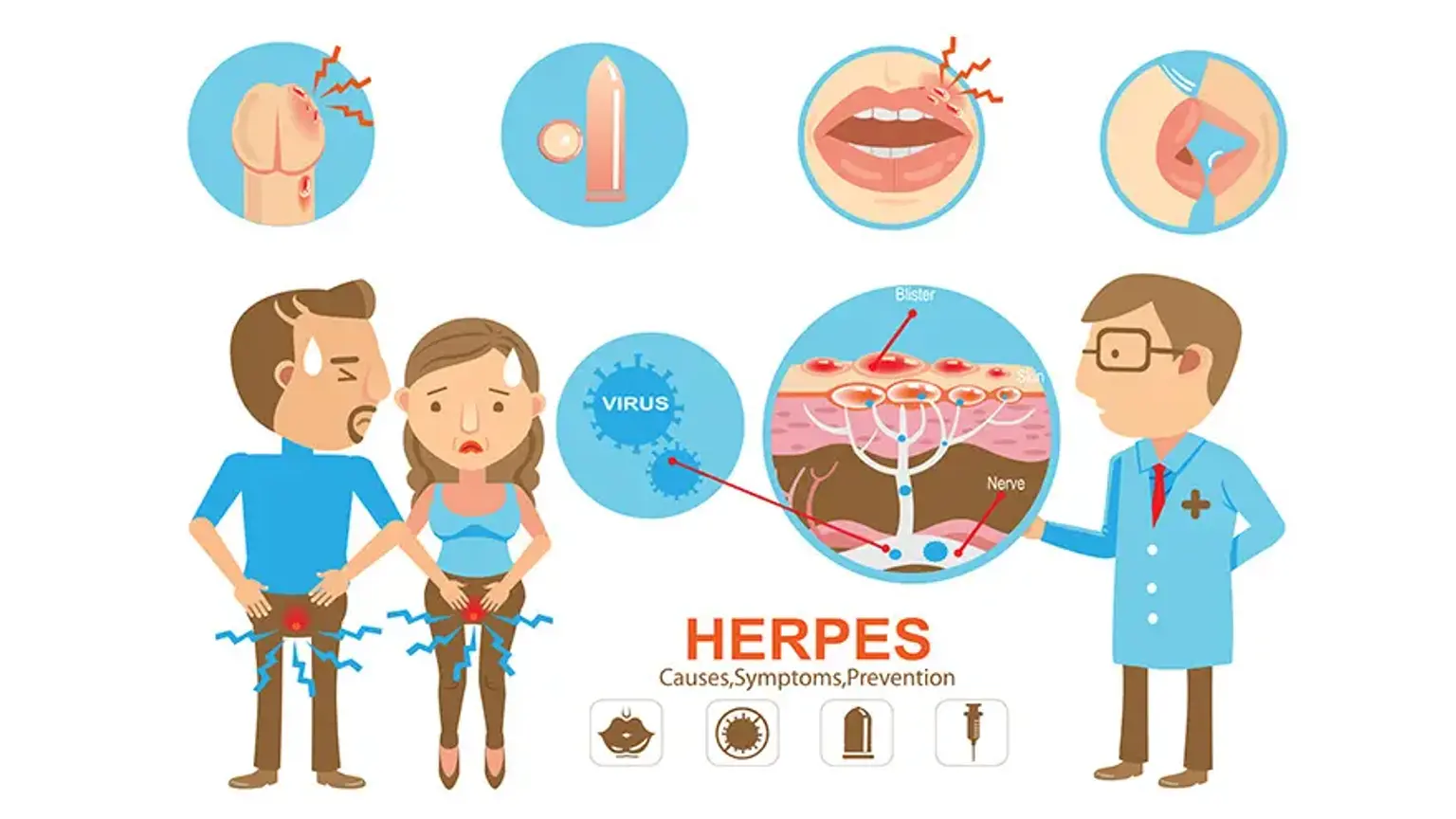
what-is-genital-herpesGenital herpes is a chronic condition caused by the Herpes Simplex Virus (HSV). There are two main types of the virus:
HSV-1: This type most commonly causes oral herpes cold sores but can also cause genital herpes through oral-genital contact.
HSV-2: This type is the most common cause of genital herpes and is primarily transmitted through sexual contact.
Once a person is infected, the virus remains in the body for life, residing in nerve cells. It can alternate between dormant periods and active periods, known as outbreaks, when symptoms appear.
What are the Common Causes and Risk Factors for Genital Herpes?
what-are-the-common-causes-and-risk-factors-for-genital-herpesThe primary cause of genital herpes is direct skin-to-skin contact with an infected area during sexual activity. The virus is most contagious when sores or blisters are present, but it can also be transmitted when there are no visible symptoms, a process known as asymptomatic shedding.
Key risk factors include:
Unprotected Sexual Contact: Not using condoms or other barrier methods significantly increases transmission risk.
Multiple Sexual Partners: Having more partners over a lifetime increases the likelihood of exposure.
Being Female: Genital herpes is more easily transmitted from men to women than from women to men.
Weakened Immune System: Conditions like HIV or undergoing chemotherapy can make one more susceptible to infection and lead to more severe outbreaks.
What are the Symptoms and Signs of Genital Herpes?
what-are-the-symptoms-and-signs-of-genital-herpesMany people with genital herpes have no symptoms or have very mild ones that go unnoticed. When symptoms do occur during a primary outbreak, they are often more severe.
What are the very first signs of genital herpes?
what-are-the-very-first-signs-of-genital-herpesThe first signs of a primary genital herpes outbreak typically appear 2 to 12 days after exposure. The initial phase, called the prodrome, may include tingling, itching, or burning sensations in the genital or rectal area, followed by flu-like symptoms such as fever, body aches, and swollen lymph nodes in the groin.
What do genital herpes sores look like?
what-do-genital-herpes-sores-look-likeShortly after the prodrome, one or more small red bumps appear, which quickly develop into fluid-filled blisters vesicles. These blisters then break, leaving painful, open sores. These sores will eventually crust over and heal without scarring. The sores can appear on the penis, scrotum, vulva, vagina, cervix, anus, buttocks, or inner thighs.
How is Genital Herpes Diagnosed?
how-is-genital-herpes-diagnosedAccurate diagnosis is crucial for proper management. A healthcare provider can often diagnose genital herpes by visually examining the sores. To confirm the diagnosis, the following tests are used:
Viral Culture: A swab from a fresh sore is sent to a lab to see if the herpes virus grows.
PCR Test (Polymerase Chain Reaction): This is a highly accurate test that copies the DNA from a sample of blood, tissue, or spinal fluid. A PCR test can identify the presence of the virus and determine if it is HSV-1 or HSV-2.
Blood Test: Blood tests can detect antibodies to HSV. These are useful when a person has no visible sores but has been exposed or has a history of symptoms.
What are the most effective treatments for genital herpes?
what-are-the-most-effective-treatments-for-genital-herpesWhile there is no cure for genital herpes, antiviral medications are highly effective at managing the condition. These medications can shorten the duration and severity of outbreaks, reduce the frequency of recurrences, and minimize the risk of transmission to a partner.
Episodic Therapy: Your doctor may prescribe an antiviral medication to take for several days as soon as you notice signs of an outbreak. This can help the sores heal faster.
Suppressive Therapy: For individuals with frequent outbreaks, a doctor may recommend taking a low dose of an antiviral medication daily. This can reduce the number of outbreaks by 70-80% and significantly lowers the risk of transmitting the virus.
The most commonly prescribed antiviral drugs are Acyclovir, Valacyclovir, and Famciclovir.
How Can I Manage Life with Genital Herpes?
how-can-i-manage-life-with-genital-herpes"The diagnosis felt like a brand on my soul at first. I was scared and ashamed. But learning about suppressive therapy and how to talk to my partner gave me back control. It doesn't define my life or my relationships anymore; it's just something I manage." – an anonymous patient, United States.
Managing life with genital herpes involves both medical treatment and lifestyle adjustments. Reducing stress, eating a balanced diet, and getting enough sleep can help support your immune system and potentially reduce the frequency of outbreaks. Open communication with sexual partners is essential for emotional well-being and preventing transmission.
When Should I See a Doctor for Genital Herpes?
when-should-i-see-a-doctor-for-genital-herpesYou should see a doctor as soon as you suspect you have genital herpes. Seek medical attention if you notice:
Any blisters, sores, or unusual bumps in your genital area.
Tingling, itching, or pain that precedes the appearance of sores.
Flu-like symptoms combined with genital discomfort.
If your partner has been diagnosed with genital herpes.
Early diagnosis allows for prompt treatment to manage symptoms and reduce the risk of complications or transmission.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaFor individuals seeking dermatological and aesthetic care in South Korea, these clinics are noted for their advanced treatments and patient care. While they offer a wide range of services, those with strong dermatology departments are well-equipped to handle various skin conditions.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
All-line Clinic | Body & Face Contouring, Laser Treatments | Mapo-gu, Seoul, South Korea | ||
Plans Clinic | Comprehensive Aesthetic & Laser Procedures | Gangnam-gu, Seoul, South Korea | ||
BLS Clinic | Lifting Treatments, Laser & Skin Boosters | Gangnam-gu, Seoul, South Korea | ||
Natural Beauty Clinic | Non-invasive Procedures, Laser Dermatology | Gangnam-gu, Seoul, South Korea | ||
Clinic Trinity Raffaello | High-end Lifting & Laser Aesthetics | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Oracle Dermatology | Renowned Dermatology, Pigmentation & Scar Lasers | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Qbq Clinic | Boutique Aesthetic Dermatology & Lasers | Gangnam-gu, Seoul, South Korea | ||
Oracle Clinic Cheongdam | Focus on laser and skin treatments. | Gangnam-gu, Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaBelow are various dermatological and aesthetic procedures available in South Korea. While not direct treatments for herpes, they represent the advanced capabilities of the listed clinics.
Treatment/Procedure Name | Duration | Hospitalization? | Avg. Cost (USD) in S. Korea | Contact |
|---|---|---|---|---|
Skin Botox – Full Face | 30-45 mins | Not Needed | $300 - $600 | |
Rejuran Healer | 30 mins | Not Needed | $250 - $500 | |
Juvelook | 30-45 mins | Not Needed | $350 - $700 | |
Jaw Botox | 15-20 mins | Not Needed | $100 - $300 | |
Ulthera | 45-90 mins | Not Needed | $1,500 - $4,000 | |
Thermage FLX | 60-90 mins | Not Needed | $2,000 - $5,000 | |
Pigmentation & Whitening Laser | 20-40 mins | Not Needed | $150 - $400 | |
miraDry | 60-90 mins | Not Needed | $1,500 - $2,500 | |
Acne Peeling | 30-60 mins | Not Needed | $100 - $300 | |
Face Fat Dissolving Injection | 20-30 mins | Not Needed | $150 - $400 | |
Scar & Pore Laser (e.g., Fraxel) | 45-75 mins | Not Needed | $400 - $800 | |
Laser Hair Removal | 15-60 mins | Not Needed | $50 - $250 |
What Are Common Questions About Genital Herpes?
what-are-common-questions-about-genital-herpesThis section addresses common practical questions patients have about the condition.
1. Can genital herpes be cured permanently or only managed?
1.-can-genital-herpes-be-cured-permanently-or-only-managedCurrently, there is no permanent cure for genital herpes. The virus remains in the body for life. However, antiviral medications make it a very manageable condition by controlling symptoms, reducing the frequency of outbreaks, and lowering the risk of transmission.
2. How long does a genital herpes outbreak typically last?
2.-how-long-does-a-genital-herpes-outbreak-typically-lastThe first outbreak is usually the longest and most severe, lasting two to four weeks. Recurrent outbreaks are typically shorter and less painful, often lasting from three days to a week before healing completely.
3. Can I still have a healthy sex life with genital herpes?
3.-can-i-still-have-a-healthy-sex-life-with-genital-herpesYes. Managing genital herpes allows for a healthy and active sex life. Key strategies include taking suppressive antiviral therapy to reduce asymptomatic shedding, using condoms consistently, and avoiding sexual contact during an active outbreak. Open and honest communication with your partner is fundamental.
4. Can genital herpes cause other health problems?
4.-can-genital-herpes-cause-other-health-problemsIn healthy individuals, genital herpes rarely causes serious long-term health problems. However, for people with suppressed immune systems, outbreaks can be more severe and frequent. There is also an established link between genital herpes and an increased risk of acquiring and transmitting HIV, as the open sores provide an entry point for the virus.
Your Path to Confidential Care and Management Starts Here Now!
your-path-to-confidential-care-and-management-starts-hereA genital herpes diagnosis can feel isolating, but you're not alone. Expert care is available at CloudHospital through a simple, private process. A dedicated Care Manager will guide you from consultation to post-treatment. And Get Free Treatment Plan & Quote Today.