The clinical information regarding Antiphospholipid Syndrome in this article has been rigorously verified against the latest 2023 international consensus classification criteria and guidelines from the American College of Rheumatology (ACR). This piece was reviewed for accuracy and patient-centric clarity and was last updated in September 2023.
Introduction
introductionAntiphospholipid Syndrome (APS), also known as Hughes Syndrome, is a complex autoimmune disorder that can have serious health implications if not properly diagnosed and managed. It is characterized by the presence of specific autoantibodies that mistakenly target the body's own proteins, leading to an increased risk of blood clots. This guide offers a comprehensive overview of APS, from its underlying causes to the most advanced treatment strategies, for those seeking to understand and navigate this condition.
What is Antiphospholipid Syndrome?
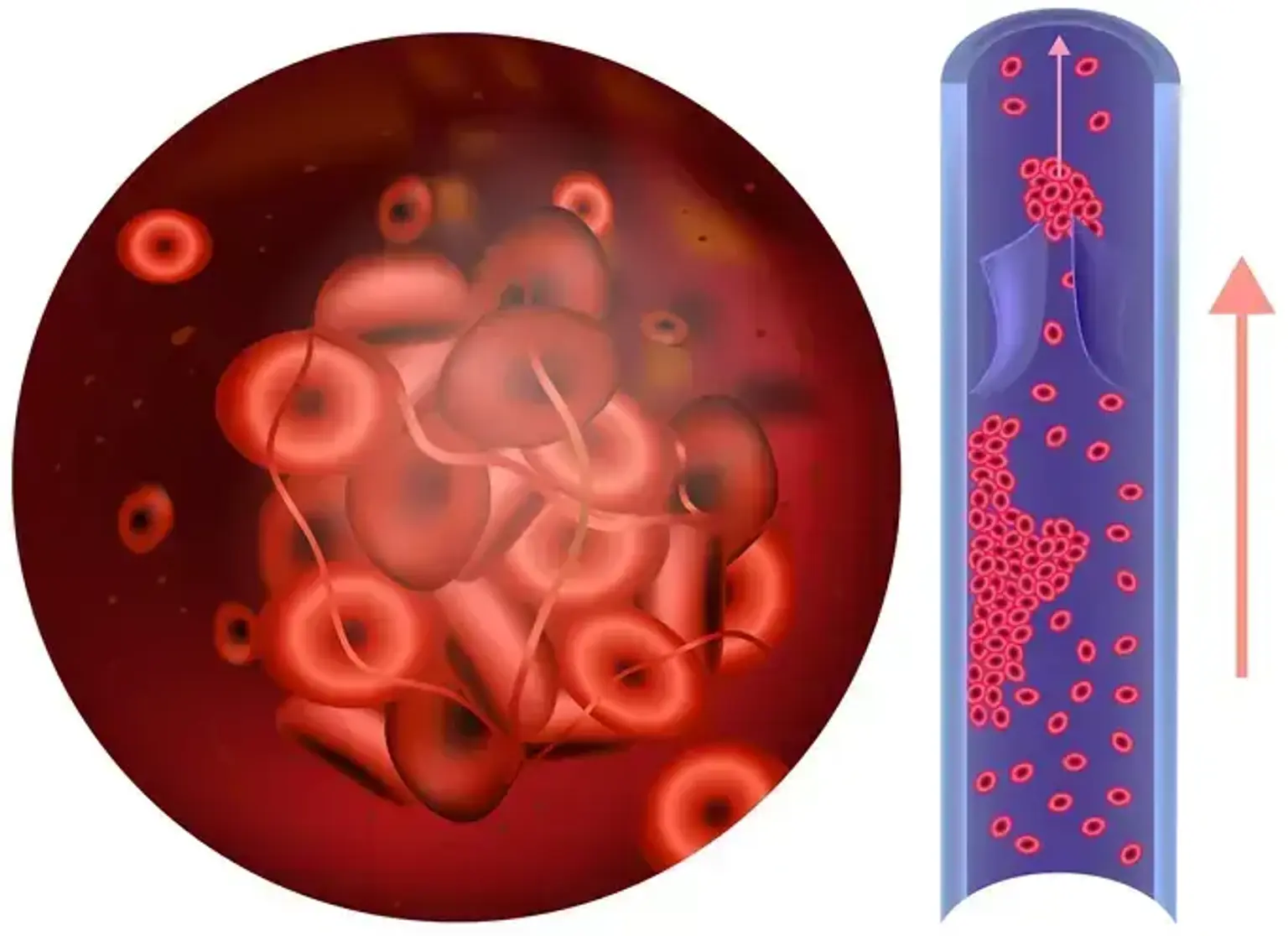
what-is-antiphospholipid-syndromeAntiphospholipid Syndrome is an autoimmune disorder where the immune system produces abnormal antibodies called antiphospholipid antibodies (aPL). These antibodies target proteins bound to phospholipids, a type of fat molecule found in cell membranes, including those that line blood vessels. This interaction increases the tendency for blood to clot, leading to the formation of dangerous blockages thrombosis in arteries or veins. APS can occur on its own Primary APS or in conjunction with other autoimmune diseases, most commonly systemic lupus erythematosus Secondary APS.
What are the Primary Causes and Risk Factors for Antiphospholipid Syndrome?
what-are-the-primary-causes-and-risk-factors-for-antiphospholipid-syndromeThe exact cause of APS is not fully understood, but it involves a combination of genetic predisposition and environmental triggers. The body begins producing antiphospholipid antibodies for reasons that are still under investigation.
Key Risk Factors:
Genetic Predisposition: Having a family member with APS or another autoimmune condition can increase risk.
Coexisting Autoimmune Conditions: A significant portion of individuals with lupus, Sjogrens syndrome, or rheumatoid arthritis also develop secondary APS.
Infections: Certain infections, such as hepatitis C, HIV, and syphilis, have been linked to the temporary or persistent production of aPL antibodies.
Medications: Some drugs, including certain antibiotics and anti-seizure medications, have been associated with triggering the condition.
Gender and Age: APS is diagnosed more frequently in women than in men, typically between the ages of 30 and 40.
What are the First Signs and Symptoms of APS?
what-are-the-first-signs-and-symptoms-of-apsThe symptoms of Antiphospholipid Syndrome are diverse and directly related to the location of blood clots. Some individuals may have the antibodies but never develop symptoms, while others experience severe and recurrent events.
Common Signs and Symptoms Include:
Deep Vein Thrombosis (DVT): A blood clot in a deep vein, usually in the leg, causing pain, swelling, and redness.
Pulmonary Embolism (PE): A life-threatening condition where a piece of a DVT breaks off and travels to the lungs.
Stroke or Transient Ischemic Attack (TIA): Caused by a blood clot in an artery of the brain.
Recurrent Pregnancy Loss: Multiple unexplained miscarriages, especially after the first trimester, are a hallmark of APS.
Pregnancy Complications: Other issues include pre-eclampsia, preterm delivery, and poor fetal growth.
Skin Manifestations: A lacy, net like reddish blue skin rash known as livedo reticularis.
Neurological Symptoms: Chronic headaches, migraines, and memory problems.
Low Platelet Count (Thrombocytopenia): A lower than normal number of platelets in the blood.
How is Antiphospholipid Syndrome Officially Diagnosed?
how-is-antiphospholipid-syndrome-officially-diagnosedA definitive diagnosis of Antiphospholipid Syndrome requires a combination of clinical evidence and specific laboratory testing. Diagnosis is confirmed based on the updated 2023 International Consensus Classification Criteria.
The diagnostic process includes:
Clinical History: A thorough review of the patient's medical history for clinical events like one or more confirmed blood clots thrombosis or specific pregnancy-related complications.
Blood Tests: Laboratory tests are essential to detect the presence of one or more of the three primary antiphospholipid antibodies:
Lupus anticoagulant
Anticardiolipin antibodies IgG and IgM
Anti-beta-2 glycoprotein I antibodies IgG and IgM
Confirmation: To confirm a diagnosis, the blood tests must remain positive on at least two separate occasions, at least 12 weeks apart. This ensures the antibodies are persistent and not a temporary result of an infection or other factor.
What is Catastrophic Antiphospholipid Syndrome (CAPS)?
what-is-catastrophic-antiphospholipid-syndrome-(caps)Catastrophic Antiphospholipid Syndrome (CAPS) is a rare but extremely severe and life-threatening variant of APS. It occurs in less than 1% of all APS patients. CAPS is characterized by the rapid development of widespread small blood clots in multiple organs typically three or more over a short period, often days or weeks. This can lead to rapid organ failure of the kidneys, lungs, brain, and skin. CAPS is a medical emergency that requires immediate and aggressive treatment in a hospital setting, often involving high-dose anticoagulants, corticosteroids, and IVIG or plasma exchange.
Can You Live a Normal Life with Antiphospholipid Syndrome?
can-you-live-a-normal-life-with-antiphospholipid-syndromeYes, many individuals with Antiphospholipid Syndrome can live full and productive lives with proper medical management and lifestyle adjustments. The key is a consistent and proactive approach to treatment to prevent the formation of blood clots. Management often involves long-term anticoagulant medication like warfarin or direct oral anticoagulants DOACs. Regular monitoring by a rheumatologist or hematologist is crucial. Patients are educated to recognize the signs of thrombosis and to manage risk factors such as smoking, immobility, and certain medications.
"For years, I suffered from debilitating migraines and had two devastating late-term miscarriages. No one could tell me why. Finally, a rheumatologist tested me for APS. Getting the diagnosis was terrifying but also a huge relief. With anticoagulant therapy, I was able to carry my son to term. Managing APS is a daily reality, but it gave me back my future." An anonymous patient, United States.
When Should I See a Doctor for Antiphospholipid Syndrome?
when-should-i-see-a-doctor-for-antiphospholipid-syndromeYou should consult a healthcare professional, preferably a rheumatologist, if you experience any of the following:
An unprovoked blood clot DVT or PE.
A stroke or TIA at a young age under 50.
A history of two or more unexplained miscarriages.
Any combination of APS symptoms, such as a livedo reticularis rash along with chronic headaches or a low platelet count.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaFor patients seeking specialized care for complex autoimmune and rheumatological conditions like APS, South Korea offers several world-class medical centers known for their advanced diagnostics and comprehensive treatment programs.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
Cha University Bundang Medical Center | Comprehensive care, advanced diagnostics, and research in a large university hospital setting. | Bundang-gu, Gyeonggi-do, South Korea | ||
Seoul St. Mary's Hospital-Seocho | A leading research hospital within the Catholic Medical Center, specializing in complex diseases. | Seocho-gu, Seoul, South Korea | ||
Design Hospital | Providing specialized care in Orthopedics and Internal Medicine with modern facilities. | Deokjin-gu, Jeollabuk-do, South Korea | ||
Kyungpook National University Chilgok Hospital | National university hospital known for its focus on research, cancer, and specialized medical care. | Buk-gu, Daegu, South Korea | ||
Wooridul Hospital Gangnam | Internationally recognized specialization in spine surgery and neurological care. | Gangnam-gu, Seoul, South Korea | ||
Nanoori Hospital, Gangnam | Renowned for its specialization in joint, spine, and orthopedic treatments. | Gangnam-gu, Seoul, South Korea | ||
Mokdong Hospital Ewha Womans University | University hospital with a strong focus on women's health, relevant for APS management. | Yangcheon-gu, Seoul, South Korea | ||
Sarang Plus Hospital | General hospital with comprehensive departments including robust internal medicine services. | Gangdong-gu, Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaManaging APS and related autoimmune conditions often requires a multi-faceted approach. Below are common treatments and procedures with estimated costs in South Korea.
Treatment/Procedure Name | Treatment Duration | Hospitalization? | Avg Cost Range (USD) in S. Korea | Contact |
|---|---|---|---|---|
IVIG Therapy (Intravenous Immunoglobulin) | 2-5 hours | Not Needed | $3,000 - $7,000 | |
Immunosuppressive Therapy | 1-3 hours | Not Needed | $200 - $800 | |
Biologic Therapy for Rheumatoid Arthritis | 30-60 min | Not Needed | $1,000 - $3,000 | |
Stem Cell Therapy for Autoimmune Diseases | 3-4 hours | Not Needed | $15,000 - $30,000 | |
Targeted DMARDs | 2-5 hours | Not Needed | $500 - $1,500 | |
Lupus Nephritis Management | 1-2 hours | Needed( 1-2 days) | $5,000 - $20,000 | |
Vasculitis Treatment | 2-4 hours | Not Needed | $3,000 - $15,000 | |
Joint Replacement Surgery (Rheumatic Damage) | 2-4 hours | Needed (3-7 days) | $12,000 - $25,000 | |
Systemic Sclerosis Treatment | 2-3 hours | Not Needed | $5,000 - $18,000 |
Frequently Asked Questions About Antiphospholipid Syndrome
frequently-asked-questions-about-antiphospholipid-syndrome1. What are the most effective treatments for Antiphospholipid Syndrome?
1.-what-are-the-most-effective-treatments-for-antiphospholipid-syndromeThe primary treatment goal is to prevent blood clots. For patients with a history of thrombosis, long-term anticoagulation with medications like warfarin is standard. For high-risk situations or in pregnant women, injections of heparin are often used. Low-dose aspirin may be prescribed for individuals who have the antibodies but no history of clots.
2. Is Antiphospholipid Syndrome considered a high-risk pregnancy?
2.-is-antiphospholipid-syndrome-considered-a-high-risk-pregnancyYes, APS significantly increases the risk of pregnancy complications. It is a leading cause of recurrent miscarriage. With specialized care from a rheumatologist and high-risk obstetrician, successful pregnancies are very possible. Treatment typically involves a combination of low-dose aspirin and daily heparin injections to prevent clots in the placenta.
3. Is Antiphospholipid Syndrome hereditary?
3.-is-antiphospholipid-syndrome-hereditaryWhile APS itself is not directly inherited, a genetic predisposition exists. Having a first-degree relative with APS or another autoimmune disease like lupus can increase an individual's risk of developing the condition.
4. Can diet and lifestyle affect APS?
4.-can-diet-and-lifestyle-affect-apsWhile no specific diet can cure APS, a healthy lifestyle is crucial. This includes maintaining a healthy weight, avoiding smoking a major risk factor for clotting, and staying active to promote good circulation. It's also vital to avoid prolonged immobility, such as during long flights, which can increase DVT risk.
5. Can APS go away?
5.-can-aps-go-awayAntiphospholipid Syndrome is considered a chronic condition. While the levels of antibodies can fluctuate, they rarely disappear completely once a diagnosis is confirmed. Management is focused on lifelong risk reduction and prevention of thrombotic events rather than a cure.
6. What is the difference between APS and Lupus?
6.-what-is-the-difference-between-aps-and-lupusAPS and Lupus are both autoimmune diseases, and they can coexist Secondary APS. Lupus is a systemic disease that can affect the skin, joints, kidneys, and brain. APS is specifically a blood clotting disorder caused by antiphospholipid antibodies. A person can have APS without having lupus.
7. Do I need to wear a medical alert bracelet for APS?
7.-do-i-need-to-wear-a-medical-alert-bracelet-for-apsIt is highly recommended. Because the primary treatment is anticoagulation, which increases bleeding risk, a medical alert bracelet is vital. It informs emergency responders that you are on blood thinners, which is critical information in the event of an accident or injury.
Begin Your Journey to Managing APS: Get Expert Guidance Today!
begin-your-journey-to-managing-aps:-get-expert-guidanceNavigating a diagnosis of Antiphospholipid Syndrome can be overwhelming, but you are not alone. Taking the first step toward expert evaluation and management is critical for your long term health and well being. The world-class medical centers in South Korea in partnership with Cloud Hospital provide access to leading rheumatology specialists and advanced diagnostic technologies. Our dedicated Care Managers ensure a seamless and transparent process, offering end-to-end support from your initial questions to your post-treatment care. Start Your Confidential Inquiry with Cloud Hospital Today.