The clinical information regarding Atopic Dermatitis in this article has been rigorously verified against the latest guidelines from the American Academy of Dermatology AAD and primary research from databases like PubMed. This piece was reviewed for accuracy and patient centric clarity and was last updated in October 2023.
Introduction
introductionAtopic dermatitis, commonly known as eczema, is a chronic inflammatory skin condition that causes dry skin, intense itching, and recurrent rashes. It affects a significant portion of the global population, impacting up to 20% of children and 3% of adults worldwide. This condition can significantly diminish quality of life due to physical discomfort and emotional distress. This guide offers a comprehensive overview of atopic dermatitis, providing critical information for individuals seeking to understand, manage, and find effective relief from its persistent symptoms.
What is Atopic Dermatitis?
what-is-atopic-dermatitisAtopic dermatitis is the most common type of eczema. It is a long term condition characterized by a dysfunctional skin barrier and an overactive immune response. A healthy skin barrier acts like a brick wall, keeping moisture in and harmful substances like irritants and allergens out. In individuals with atopic dermatitis, this barrier is compromised, often due to a genetic mutation in the filaggrin gene. This defect allows moisture to escape easily, leading to chronic dryness, and permits allergens and microbes to penetrate the skin. This penetration triggers an inflammatory response from the immune system, resulting in the characteristic red, itchy rashes.
What is the difference between eczema and dermatitis?
what-is-the-difference-between-eczema-and-dermatitisThe first sentence of each corresponding paragraph must be a direct, concise answer to that heading's question, followed by elaboration. The terms eczema and dermatitis are often used interchangeably to describe skin inflammation, but dermatitis is the broader medical term for any skin inflammation, while eczema is a specific type of dermatitis. Atopic dermatitis is the most prevalent and chronic form of eczema. Other types of dermatitis include contact dermatitis, which is caused by direct contact with an irritant, and seborrheic dermatitis, which affects oily areas of the body. While all eczema is a form of dermatitis, not all dermatitis is eczema.
What are the main triggers for atopic dermatitis flare ups?
what-are-the-main-triggers-for-atopic-dermatitis-flare-upsThe main triggers for atopic dermatitis flare ups are environmental allergens, irritants, and internal factors that provoke the immune system. Identifying and avoiding personal triggers is a cornerstone of managing the condition effectively.
Dry Skin: Insufficient moisture worsens skin barrier dysfunction and can trigger the itch scratch cycle.
Irritants: Common household products like soaps, detergents, shampoos, and disinfectants can strip the skin of its natural oils. Wool and synthetic fabrics may also irritate the skin.
Allergens: Environmental allergens such as dust mites, pet dander, pollens, and molds are well known triggers. Certain food allergens, particularly in children, like milk, eggs, peanuts, and soy can also cause flares.
Microbes: Certain bacteria, such as Staphylococcus aureus, viruses, and fungi can colonize the skin and worsen inflammation.
Climate and Temperature: Hot weather and increased sweating can irritate the skin. Conversely, cold, dry winter air can lead to severe dryness.
Stress: Emotional stress is a significant trigger. It does not cause atopic dermatitis but can make symptoms worse by activating the body's inflammatory pathways.
Hormones: Women may experience a worsening of symptoms during hormonal fluctuations, such as before their menstrual period or during pregnancy.
What does early stage atopic dermatitis look like?
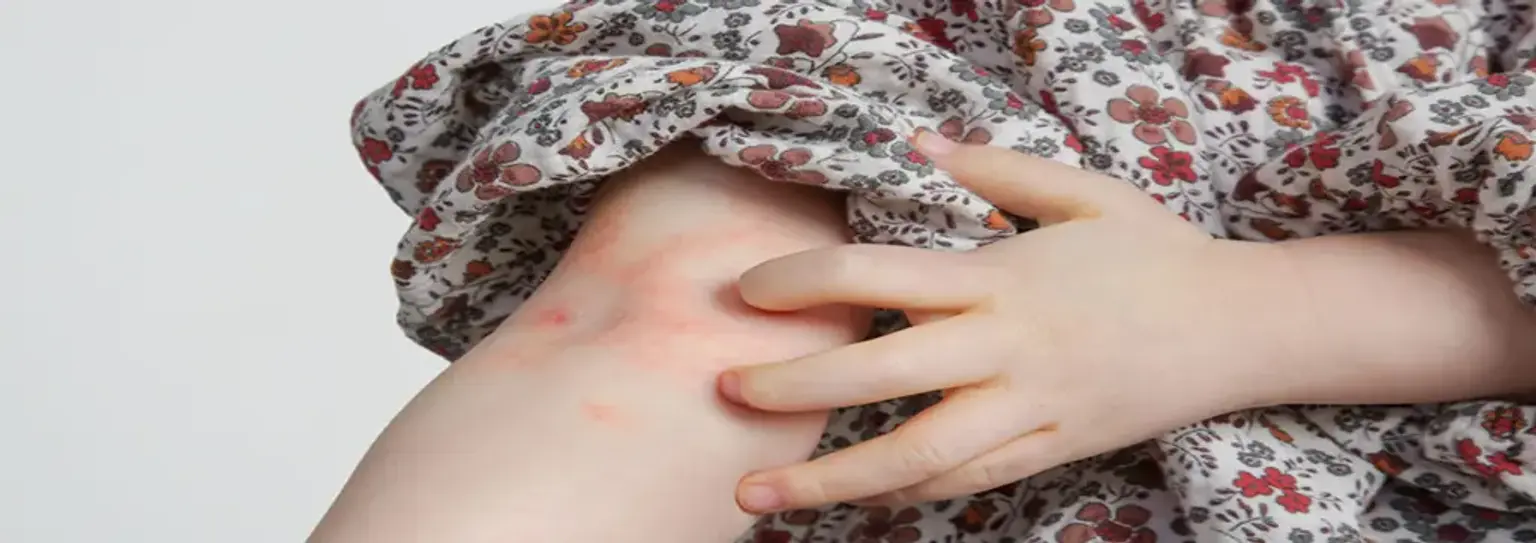
what-does-early-stage-atopic-dermatitis-look-likeEarly stage atopic dermatitis typically appears as patches of dry, red, and intensely itchy skin. The appearance and location can vary significantly with age.
In Infants: Rashes often appear on the cheeks, scalp, and the front of the arms and legs. The skin may look weepy or crusted.
In Children: Rashes commonly occur in the creases of the elbows, behind the knees, and on the neck, wrists, and ankles. The affected skin may become scaly and thicker over time.
In Adults: Flare ups frequently affect the hands, eyelids, and the bends of the elbows and knees. The skin often appears very dry, scaly, and in long term cases, may become permanently thickened, a process known as lichenification.
The most universal symptom across all stages and ages is pruritus, or severe itching, which can be debilitating.
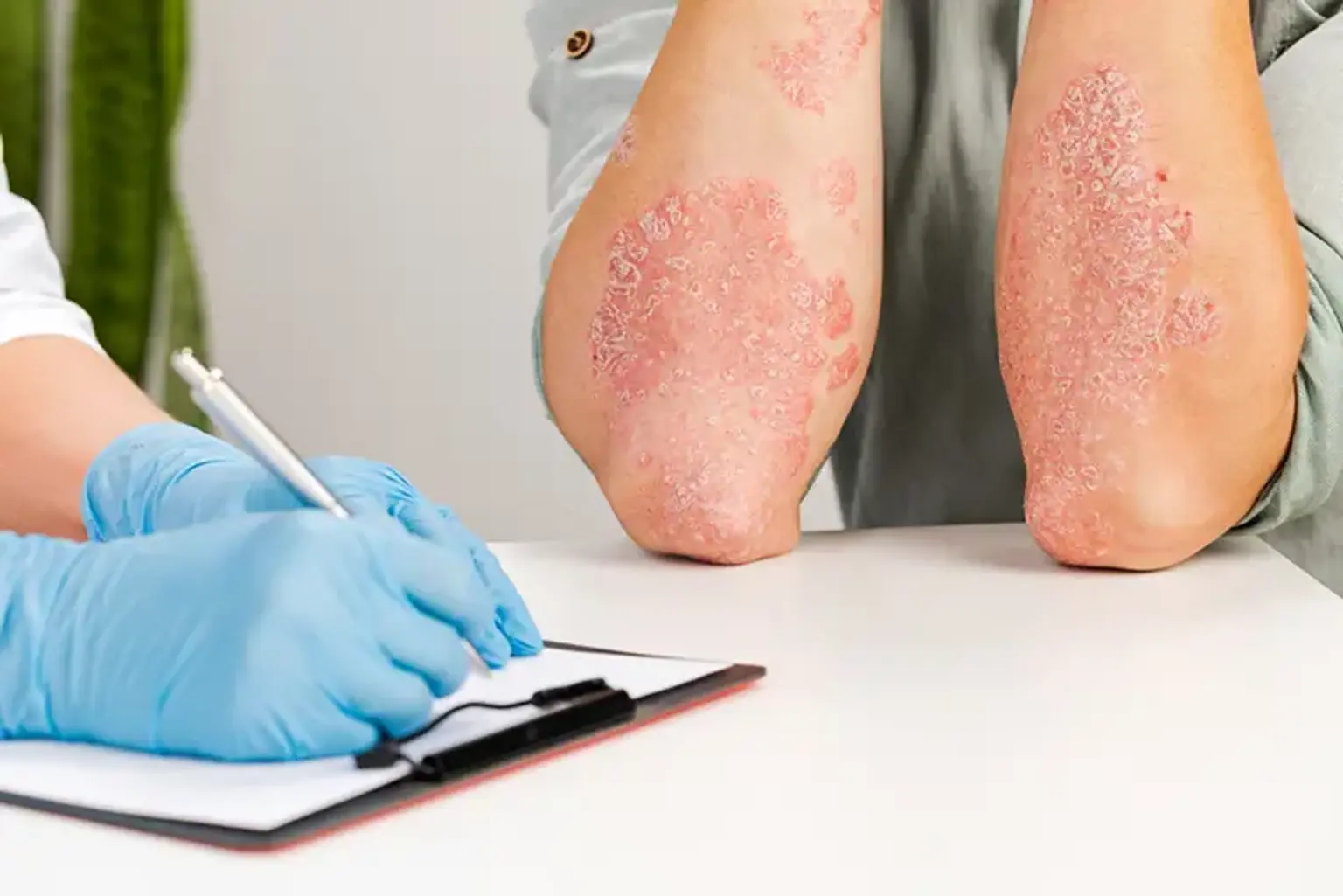
How do dermatologists confirm an atopic dermatitis diagnosis?
how-do-dermatologists-confirm-an-atopic-dermatitis-diagnosisDermatologists confirm an atopic dermatitis diagnosis primarily through a physical examination and a review of the patient's personal and family medical history. There is no single lab test to diagnose the condition. A dermatologist will look for the typical signs and symptoms, such as dry skin, redness, and the characteristic rash patterns. They will ask about the history of the itch, its triggers, and whether family members have a history of atopic dermatitis, asthma, or hay fever, which are all related atopic conditions. In some cases, a patch test may be performed to rule out allergic contact dermatitis or a skin biopsy may be taken to exclude other skin diseases.
What are the most effective treatments for severe eczema?
what-are-the-most-effective-treatments-for-severe-eczemaThe most effective treatments for severe eczema involve a multi faceted approach that combines aggressive moisturization, potent anti inflammatory medications, and sometimes systemic therapies like biologic therapy. The goal is to control inflammation, relieve itching, and restore the skin barrier.
Topical Corticosteroids: These are anti inflammatory medications applied directly to the skin and are a primary treatment. They come in various strengths, and a dermatologist will prescribe the appropriate potency based on the severity and location of the rash.
Topical Calcineurin Inhibitors: These non steroidal medications, such as tacrolimus and pimecrolimus, work by suppressing the immune response in the skin. They are often used on sensitive areas like the face and eyelids.
Phototherapy: Also known as light therapy, this treatment uses controlled exposure to ultraviolet light to reduce inflammation and itching.
Systemic Medications: For severe, widespread cases unresponsive to topical treatments, doctors may prescribe oral or injectable medications. These include traditional immunosuppressants like cyclosporine or methotrexate, as well as newer biologic drugs. Biologics are advanced medications that target specific components of the immune system responsible for the inflammatory response in atopic dermatitis.
Antibiotics: If the skin becomes infected, which is common, a course of antibiotics may be necessary to clear the infection and allow the skin to heal.
Can lifestyle and diet help manage atopic dermatitis?
can-lifestyle-and-diet-help-manage-atopic-dermatitisYes, specific lifestyle and dietary adjustments can play a crucial supportive role in managing atopic dermatitis. While not a cure, these modifications can help reduce the frequency and severity of flare ups by strengthening the skin barrier and avoiding triggers.
"The constant, maddening itch felt like an internal fire I couldn't put out. It controlled my sleep, my clothes, my mood. Finding a routine of gentle skincare and identifying my triggers didn't cure it, but it gave me back control and blessed moments of peace." – an anonymous patient, United States.
Key lifestyle strategies include:
Bathing and Moisturizing: Take short, lukewarm baths or showers. Use a gentle, fragrance free cleanser and pat the skin dry. Immediately apply a thick, high oil content moisturizer to damp skin to lock in hydration. This should be done at least once a day.
Choosing Fabrics: Wear soft, breathable fabrics like cotton. Avoid rough, scratchy fibers like wool and tight fitting synthetic clothing that can trap sweat.
Managing Stress: Practice stress reducing techniques such as mindfulness, meditation, or yoga.
Dietary Considerations: While food allergies are not a universal cause, some individuals may find that certain foods worsen their symptoms. An elimination diet, guided by an allergist or dermatologist, may help identify specific food triggers.
When should I see a doctor for eczema?
when-should-i-see-a-doctor-for-eczemaYou should see a doctor for eczema when the condition causes significant discomfort, disrupts sleep or daily activities, or if you suspect your skin is infected. It is essential to seek professional medical advice if over the counter remedies are not providing relief. Clear signs that warrant a visit to a healthcare provider include severe and persistent itching, skin that is painful or weeping fluid, or if the rash spreads rapidly across your body. A dermatologist can provide an accurate diagnosis, prescribe effective treatments, and help you develop a personalized management plan.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaSouth Korea is renowned for its advanced dermatological care. The following clinics are noted for their expertise in a range of skin treatments that can support overall skin health.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
All-line Clinic | Body contouring injections, lifting | Mapo-gu, Seoul, South Korea | ||
Plans Clinic | Fat dissolving injections, lifting | Gangnam-gu, Seoul, South Korea | ||
BLS Clinic | Lifting, Botox, Fillers | Gangnam-gu, Seoul, South Korea | ||
Natural Beauty Clinic | Skin boosters, laser treatments | Gangnam-gu, Seoul, South Korea | ||
Clinic Trinity Raffaello | Anti aging, skin care, body contouring | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Oracle Dermatology | Dermatology, anti aging, skin boosters | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Qbq Clinic | General dermatology, laser treatments | Gangnam-gu, Seoul, South Korea | ||
Oracle Clinic Cheongdam | Lifting, skin treatments, fat dissolving | Gangnam-gu, Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaWhile not direct cures for atopic dermatitis, these advanced dermatological procedures available in South Korea can address associated concerns like skin texture, barrier repair, and overall skin health.
Treatment/Procedure Name | Duration | Hospitalization? | Avg. Cost (USD) in S. Korea | Contact |
|---|---|---|---|---|
Rejuran Healer | 30 mins | Not Needed | $300 - $600 | |
Skin Botox – Full Face | 30-45 mins | Not Needed | $250 - $500 | |
Juvelook | 45-60 mins | Not Needed | $400 - $700 | |
Titanium Lifting | 60-90 mins | Not Needed | $1000 - $2500 | |
Thermage FLX | 60-90 mins | Not Needed | $1500 - $3000 | |
Pigmentation & Whitening Laser | 20-30 mins | Not Needed | $150 - $400 | |
Secret Laser | 45-60 mins | Not Needed | $300 - $600 | |
Acne Peeling | 30 mins | Not Needed | $100 - $250 |
What Are Common Questions About Atopic Dermatitis?
what-are-common-questions-about-atopic-dermatitisThis section addresses the most common practical questions patients have about living with the condition.
1. Is atopic dermatitis contagious?
1.-is-atopic-dermatitis-contagiousNo, atopic dermatitis is not contagious. It is a non infectious condition related to genetics and immune system function, so you cannot catch it from or pass it to another person.
2. Can atopic dermatitis be cured permanently?
2.-can-atopic-dermatitis-be-cured-permanentlyThere is currently no permanent cure for atopic dermatitis. It is a chronic condition that can have periods of flare and remission. However, with consistent and appropriate management, symptoms can be very well controlled, allowing individuals to live comfortably.
3. Does atopic dermatitis go away with age?
3.-does-atopic-dermatitis-go-away-with-ageMany children with atopic dermatitis find that their symptoms improve or disappear completely as they get older. However, for some, it can persist into adulthood or reappear after many years of being clear. Many adults who had eczema as children retain a tendency for dry, easily irritated skin.
4. Can stress cause atopic dermatitis?
4.-can-stress-cause-atopic-dermatitisStress does not directly cause atopic dermatitis, but it is a very common and powerful trigger for flare ups. When you are stressed, your body releases hormones like cortisol, which can increase inflammation throughout the body, including the skin, worsening eczema symptoms.
5. Is there a special diet for atopic dermatitis?
5.-is-there-a-special-diet-for-atopic-dermatitisThere is no single diet that works for everyone with atopic dermatitis. However, for a subset of individuals, particularly young children, certain food allergies can trigger or worsen eczema. If a food allergy is suspected, it is crucial to work with a doctor or allergist for proper testing and to avoid unnecessary dietary restrictions.
6. What is the best type of moisturizer to use?
6.-what-is-the-best-type-of-moisturizer-to-useThe best type of moisturizer is a thick cream or ointment with a high oil content and low water content. Look for products that are fragrance free, dye free, and hypoallergenic. Ointments are excellent for locking in moisture, especially when applied to damp skin immediately after bathing.
Find Lasting Relief from Atopic Dermatitis: Begin Your Consultation Now!
find-lasting-relief-from-atopic-dermatitis:-begin-your-consultationNavigating the challenges of atopic dermatitis requires expert guidance and a personalized care strategy. You can take the next step toward healthier, more comfortable skin by exploring advanced dermatological care in South Korea. The process is seamless and transparent, with a dedicated Care Manager from CloudHospital to support you from your initial questions through to post-treatment care. To understand your options and receive a customized plan from top specialists and start your confidential inquiry today.