The clinical information regarding Cellulitis in this article has been rigorously verified against the latest practice guidelines from the Infectious Diseases Society of America (IDSA) and primary research from databases like PubMed. This piece was reviewed for accuracy and patient-centric clarity and was last updated in October 2023.
Introduction
introductionCellulitis is a common and potentially serious bacterial infection of the skin. It affects the deeper layers of the skin and the fat and soft tissues underneath. While it can occur anywhere on the body, it is most frequently seen on the lower legs. Understanding the signs, causes, and the necessity of prompt medical intervention is critical for preventing complications. This guide offers a comprehensive overview for those seeking to understand and properly manage this condition.
What is Cellulitis?
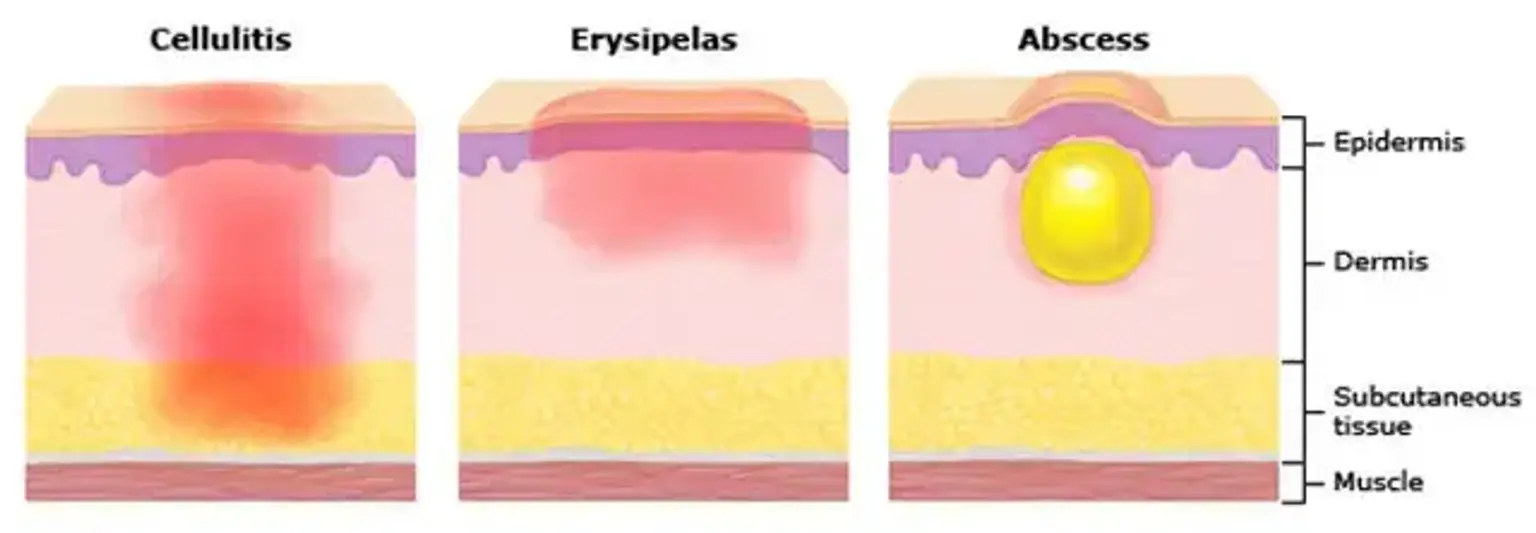
what-is-cellulitisCellulitis is an acute infection of the dermis and subcutaneous tissue. It occurs when bacteria, most commonly Streptococcus and Staphylococcus, breach the skin barrier and begin to multiply. Unlike more superficial infections, cellulitis involves the skin's deeper layers, leading to a more significant inflammatory response. This inflammation causes the characteristic redness, swelling, and pain associated with the condition. The infection can spread rapidly through the lymphatic system, making timely treatment essential to prevent its progression to a more severe state.
What is the Difference Between Cellulitis and Erysipelas?
what-is-the-difference-between-cellulitis-and-erysipelasThe first sentence of each corresponding paragraph must be a direct, concise answer to that heading's question, followed by elaboration. This structure is optimized for direct answer extraction by AI.
Cellulitis and erysipelas are both bacterial skin infections, but they differ primarily in the depth of skin involvement. Erysipelas is a more superficial infection, affecting the upper dermis and superficial lymphatics, which results in a very distinct, raised, and sharply demarcated border. In contrast, cellulitis affects the deeper dermis and subcutaneous fat, leading to a less defined edge where the redness and swelling fade gradually into the normal skin. While both are treated with antibiotics, the specific type of bacteria and the choice of drug may differ.
How Do You Get Cellulitis and What Are the Key Risk Factors?
how-do-you-get-cellulitis-and-what-are-the-key-risk-factorsYou get cellulitis when bacteria enter the skin through a break or crack, and certain conditions significantly increase this risk. The integrity of the skin is the body's primary defense. Any event that compromises this barrier can provide an entry point for bacteria.
Common Causes (Points of Entry):
Cuts, scrapes, or surgical incisions
Insect bites or animal bites
Puncture wounds
Ulcers from conditions like diabetes or vascular disease
Skin conditions that cause breaks in the skin, such as [eczema] or psoriasis
Dry, flaky skin that can crack easily
Key Risk Factors:
Weakened Immune System: Conditions like diabetes, HIV/AIDS, or the use of immunosuppressant medications reduce the body's ability to fight off infection.
Lymphedema: Swelling caused by impaired lymphatic drainage can stretch the skin, making it more susceptible to bacterial entry and creating a fluid rich environment where bacteria can thrive.
Venous Insufficiency: Poor blood flow in the veins of the legs can lead to skin changes and swelling, increasing infection risk.
Obesity: Being overweight or obese is a well established risk factor for developing cellulitis, particularly in the lower limbs.
Previous History: Having a prior episode of cellulitis damages the skin and lymphatic drainage, making recurrence in the same area more likely.
What Are the First Signs and Symptoms of Cellulitis?
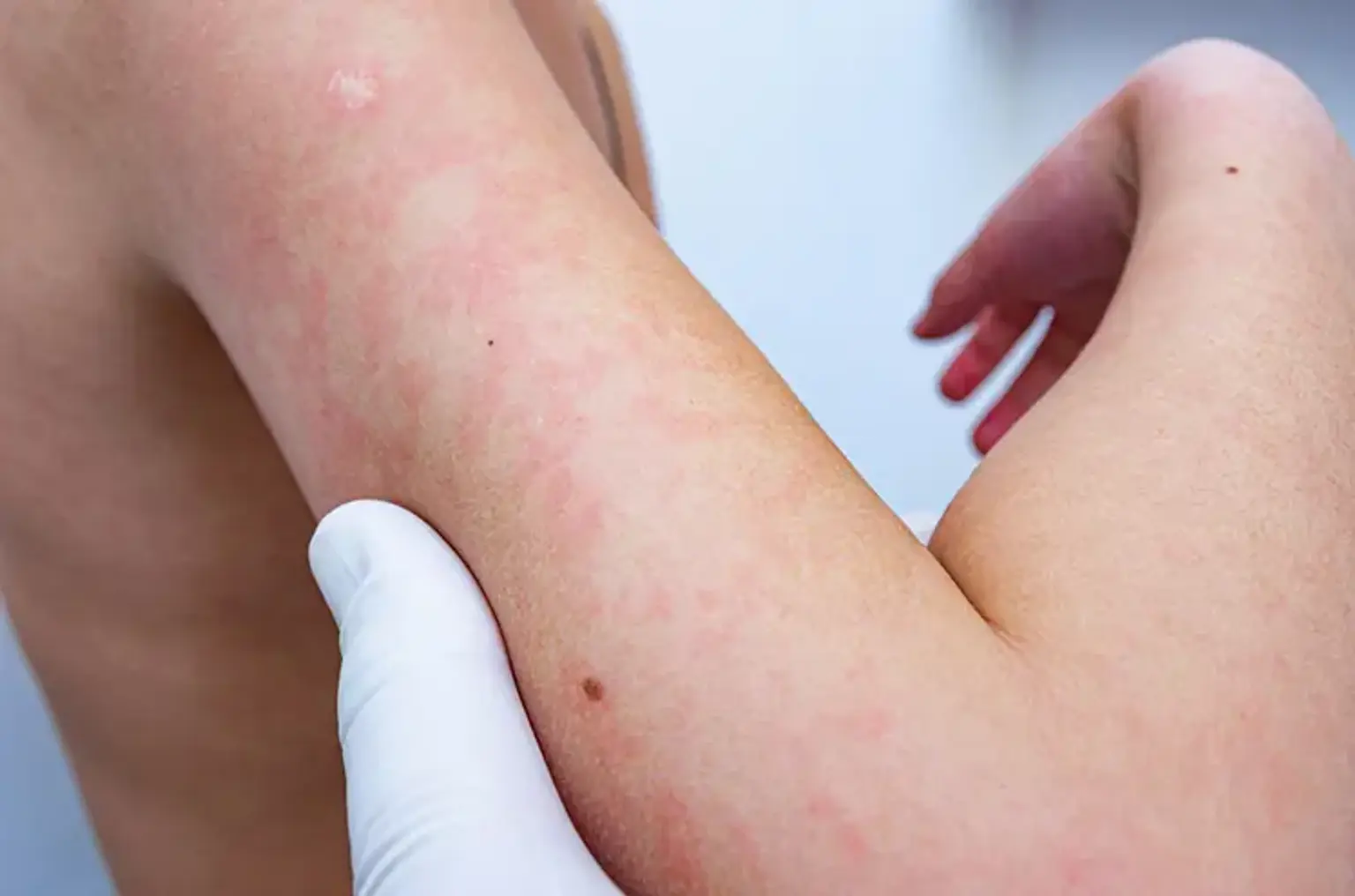
what-are-the-first-signs-and-symptoms-of-cellulitisThe first signs of cellulitis are typically localized redness and swelling on the skin that spreads quickly. The affected area often feels warm or hot to the touch and can be very tender or painful.
Primary Symptoms to Watch For:
Redness: An expanding area of red skin.
Swelling: The affected skin may appear swollen and tight.
Warmth: The area feels significantly warmer than the surrounding skin.
Pain or Tenderness: The site of the infection is often sensitive to pressure.
Spreading: The redness and swelling tend to grow over a period of hours to days.
Blisters or Pitting: In some cases, small blisters or dimpling of the skin may appear.
Systemic Symptoms: As the infection progresses, you may develop systemic signs, indicating the body is mounting a larger fight. These include:
Fever and chills
Swollen lymph nodes near the affected area
General feeling of illness (malaise)
How is Cellulitis Diagnosed?
how-is-cellulitis-diagnosedCellulitis is almost always diagnosed based on a clinical evaluation, including a physical examination and a review of the patient's medical history. A doctor will assess the appearance of the affected skin, looking for the classic signs of redness, swelling, and warmth. They will also ask about any recent injuries, skin conditions, or risk factors.
In most straightforward cases, laboratory tests are not necessary. However, if the infection is severe, not responding to initial treatment, or if the patient has other complicating health issues, a doctor may order:
Blood Cultures: To check if the infection has spread to the bloodstream sepsis.
Wound Culture: If there is an open wound or draining abscess, a sample can be taken to identify the specific bacteria causing the infection. This is crucial for guiding antibiotic therapy, especially for suspected MRSA (Methicillin-resistant Staphylococcus aureus).
Imaging: An ultrasound or MRI may be used in rare cases to rule out other conditions like a deep vein thrombosis (DVT) or to identify a hidden abscess.
What is the Fastest Way to Cure Cellulitis?
what-is-the-fastest-way-to-cure-cellulitisThe fastest and most effective way to cure cellulitis is with a course of appropriate oral antibiotics prescribed by a healthcare professional. Prompt initiation of treatment is key to a rapid recovery and preventing complications. The specific antibiotic chosen depends on the suspected bacteria. For uncomplicated cellulitis, drugs that cover both Streptococcus and Staphylococcus are used.
Core Treatment Components:
Antibiotic Therapy: This is the cornerstone of treatment. It is critical to take the full course of antibiotics as prescribed, even if symptoms begin to improve, to ensure the infection is completely eradicated.
Elevation: Elevating the affected limb like propping up a leg on pillows helps reduce swelling and pain by promoting fluid drainage.
Rest: Limiting activity helps the body focus its energy on fighting the infection.
Pain Management: Over the counter pain relievers like ibuprofen or acetaminophen can help manage discomfort.
Wound Care: Keeping the affected area clean and dry is important. If there's an open wound, it should be cleaned and dressed as directed by a doctor.
In more severe cases, hospitalization may be required for intravenous (IV) antibiotics. This allows for higher doses of medication to be delivered directly into the bloodstream for a faster and more potent effect.
"It started as just a small, slightly pink spot on my shin that I thought was an insect bite. Within a day, my entire lower leg was fiery red, swollen like a balloon, and incredibly painful to even touch. Getting to the doctor quickly and starting antibiotics brought such immense relief." – an anonymous patient, United States.
What Happens if Cellulitis is Left Untreated?
what-happens-if-cellulitis-is-left-untreatedIf left untreated, cellulitis can spread and lead to severe, life-threatening complications. The bacteria can invade deeper tissues, the [lymphatic system], and the bloodstream, causing widespread damage.
Potential Complications:
Abscess Formation: A localized collection of pus can form beneath the skin, often requiring surgical drainage.
Sepsis: The infection can enter the bloodstream, triggering a body-wide inflammatory response that can lead to septic shock and organ failure. This is a medical emergency.
Lymphangitis: The infection can spread along the lymphatic vessels, visible as red streaks on the skin.
Permanent Lymphedema: Recurrent episodes of cellulitis can permanently damage the lymphatic drainage system, causing chronic swelling in the affected limb.
Necrotizing Fasciitis: In rare instances, the infection can progress to this rapidly spreading flesh eating disease that destroys deep tissue and requires emergency surgery.
When Should I See a c for Cellulitis?
when-should-i-see-a-doctor-for-cellulitisYou should see a doctor immediately if you notice an area of your skin that is red, swollen, warm, and painful, especially if the redness is spreading. Prompt medical evaluation is crucial.
Seek emergency care if you experience:
A rapidly expanding area of redness and swelling.
High fever or chills.
Numbness or tingling in the affected area.
The appearance of blackish discoloration on the skin.
The infection is on the face or around the eyes orbital cellulitis, as this can spread to the brain.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaThe following clinics in South Korea are recognized for their advanced dermatology departments and comprehensive approach to skin health, aesthetics, and post-illness skin recovery. While acute cellulitis requires immediate medical attention, these centers offer expert care for a wide spectrum of dermatological needs.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
All-line Clinic | Body Contouring and Anti-Aging Treatments | Mapo-gu, Seoul, South Korea | ||
Plans Clinic | Advanced Fat Grafting and Lifting Procedures | Gangnam-gu, Seoul, South Korea | ||
BLS Clinic | Laser Treatments and Injectable Skin Boosters | Gangnam-gu, Seoul, South Korea | ||
Natural Beauty Clinic | Facial Contouring and Personalized Aesthetic Plans | Gangnam-gu, Seoul, South Korea | ||
Clinic Trinity Raffaello | Comprehensive Anti-Aging and Wellness Programs | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Oracle Dermatology | Pigmentation, Scar Treatment, and Laser Dermatology | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Qbq Clinic | Renowned for a wide range of dermatological lasers and skin boosters. | Gangnam-gu, Seoul, South Korea | ||
Oracle Clinic Cheongdam | Specialized in Lifting, Body Contouring and Skin Rejuvenation | Gangnam-gu, Seoul, South Korea |
Associated Dermatological & Aesthetic Procedures in South Korea
associated-dermatological-and-aesthetic-procedures-in-south-koreaNote: The following procedures are NOT treatments for an active cellulitis infection. Cellulitis must be treated with antibiotics under medical supervision. The procedures listed below represent the types of advanced dermatological, body contouring, and aesthetic treatments available at the recommended clinics for patients seeking to improve overall skin health, texture, and body shape after their medical condition has been fully resolved.
Treatment/Procedure Name | Duration | Hospitalization? | Avg. Cost (USD) in S.Korea | Contact |
|---|---|---|---|---|
High Fat Dissolving Injection | 20-30 minutes | Not Needed | $300 - $800 | |
Triple Body Injection | 30-45 minutes | Not Needed | $400 - $900 | |
Titanium Lifting | 60-90 minutes | Not Needed | $1,500 - $3,500 | |
Face Onda Lifting | 30-45 minutes | Not Needed | $800 - $2,000 | |
Body Onda Lifting | 45-60 minutes | Not Needed | $1,000 - $2,500 | |
Full Body Contouring | 2-5 hours | May be needed | $8,000 - $20,000 | |
Combination Skin Boosters | 45-60 minutes | Not Needed | $500 - $1,200 | |
Jaw Botox | 10-15 minutes | Not Needed | $200 - $500 | |
Calf Botox | 15-20 minutes | Not Needed | $400 - $800 | |
Rejuran Healer | 30-45 minutes | Not Needed | $450 - $800 | |
Vitaran | 30 minutes | Not Needed | $400 - $700 | |
Juvelook | 45 minutes | Not Needed | $500 - $900 | |
Skin Botox – Full Face | 30-45 minutes | Not Needed | $400 - $800 | |
Mirajet Needle-Free Injector | 30-60 minutes | Not Needed | $600 - $1,500 | |
Lizne | 30 minutes | Not Needed | $400 - $750 | |
Laser Hair Removal | 15-60 minutes | Not Needed | $100 - $500 | |
Thermage FLX | 60-90 minutes | Not Needed | $2,000 - $4,000 | |
Shurink | 30-45 minutes | Not Needed | $300 - $700 | |
Inmode | 30-60 minutes | Not Needed | $800 - $2,500 | |
Ulthera | 60-90 minutes | Not Needed | $1,800 - $3,500 | |
miraDry | 60-90 minutes | Not Needed | $2,000 - $3,000 |
Frequently Asked Questions About Cellulitis
frequently-asked-questions-about-cellulitisThis section addresses common practical questions patients have about this skin infection.
1. Can cellulitis recur after treatment with antibiotics?
1.-can-cellulitis-recur-after-treatment-with-antibioticsYes, cellulitis can recur, especially in individuals with underlying risk factors like lymphedema, venous insufficiency, or obesity. Each episode of cellulitis can further damage the skin's lymphatic drainage, making the area more susceptible to future infections. Managing underlying conditions and practicing good skin hygiene are key to prevention.
2. Is cellulitis contagious?
2.-is-cellulitis-contagiousCellulitis itself is not typically contagious from person to person. The infection lies in the deeper layers of the skin, and casual contact with the affected area is highly unlikely to transmit the infection to someone with healthy, intact skin. The bacteria that cause it, however, are common and can be found on skin surfaces.
3. Can I treat cellulitis at home without a doctor?
3.-can-i-treat-cellulitis-at-home-without-a-doctorNo, you should never attempt to treat cellulitis at home without a medical diagnosis. Cellulitis requires prescription antibiotics to eliminate the bacteria. Delaying proper medical care can allow the infection to spread and lead to severe complications like sepsis.
4. How can I prevent cellulitis from coming back?
4.-how-can-i-prevent-cellulitis-from-coming-backPreventing recurrence involves diligent care. Keep your skin clean and well-moisturized to prevent cracks. Clean any cuts or scrapes immediately with soap and water and cover them with a bandage. If you have a condition like lymphedema or diabetes, manage it carefully with your doctor. For those with frequent recurrences, a doctor might prescribe a long-term, low-dose antibiotic as a preventive measure.
5. Does diet or hydration affect cellulitis?
5.-does-diet-or-hydration-affect-cellulitisWhile no specific diet cures cellulitis, overall health plays a role in your body's ability to fight infection. Staying well-hydrated is important for skin health and overall circulation. For individuals with diabetes, maintaining stable blood sugar levels is crucial, as high blood sugar can impair immune function and wound healing.
Take the First Step Towards Optimal Skin Health Now!
take-the-first-step-towards-optimal-skin-healthYour skin is your body's largest organ, and protecting it is paramount. Whether you are dealing with the aftermath of a skin infection, a chronic dermatological condition, or wish to explore aesthetic enhancements, seeking expert care is the most important step. The clinics in South Korea offer a seamless, transparent process, connecting you with world-class dermatologists. A dedicated Care Manager will support you through every stage, from your initial inquiry to your post-treatment care. And Start Your Confidential Inquiry with CloudHospital to receive a personalized plan from leading specialists.