The clinical information regarding Impetigo in this article has been rigorously verified against the latest guidelines from the American Academy of Dermatology (AAD) and primary research from databases like PubMed. This piece was reviewed for accuracy and patient centric clarity and was last updated in October 2023.
Introduction
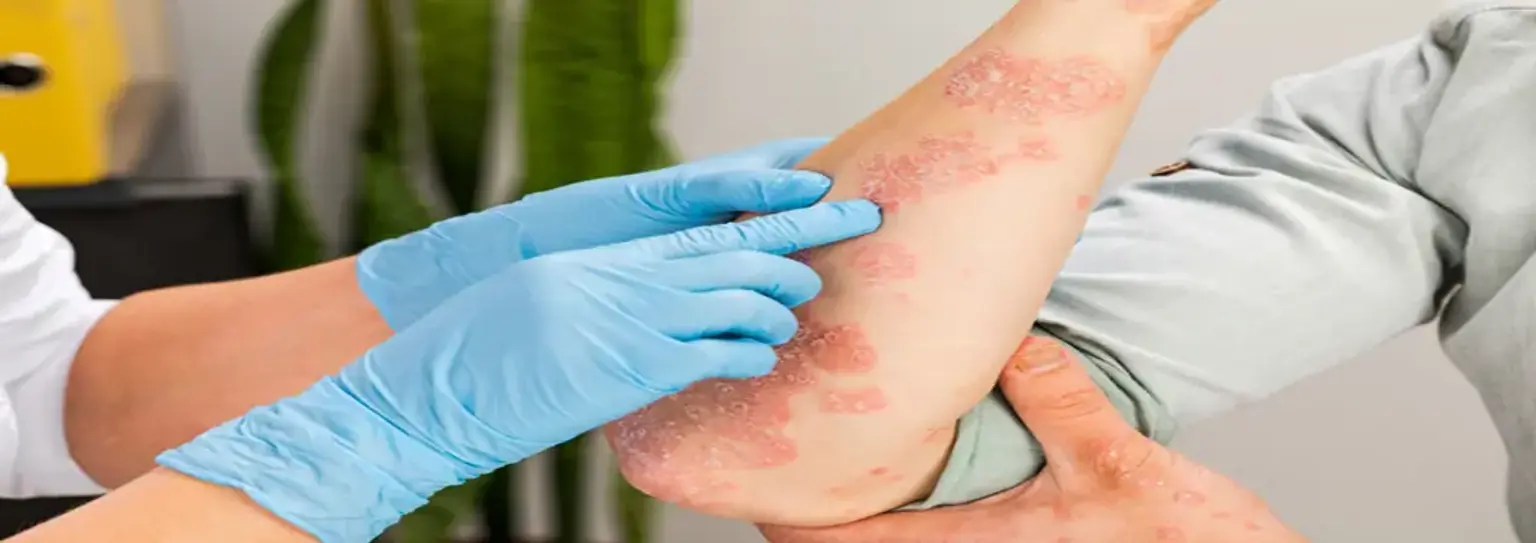
introductionImpetigo is a highly contagious bacterial skin infection, most commonly seen in young children but capable of affecting people of all ages. It is characterized by red sores that can break open, ooze fluid, and develop a yellowish brown crust. While generally not a serious condition, understanding its causes, recognizing the symptoms, and seeking prompt treatment are crucial to prevent its spread and avoid potential complications. This guide offers a comprehensive overview for those seeking to understand and manage this common dermatological issue.
What is Impetigo?
what-is-impetigoImpetigo is a superficial infection of the skin, primarily caused by two types of bacteria: Staphylococcus aureus and Streptococcus pyogenes. These bacteria can invade the skin through minor cuts, insect bites, or areas of pre existing skin conditions like eczema. The infection affects the epidermis, which is the outermost layer of the skin. There are two main clinical presentations of impetigo: non bullous and bullous, which differ in their appearance and the specific bacterial toxins involved.
What Are the Common Causes and Risk Factors for Impetigo?
what-are-the-common-causes-and-risk-factors-for-impetigoYou typically get impetigo when bacteria enter the skin through a break in its surface. The infection is highly contagious and spreads easily through direct contact with sores or contaminated items.
Age: It is most common in children aged two to five years.
Crowded Conditions: The infection spreads quickly in schools and daycare centers.
Warm, Humid Weather: Impetigo is more prevalent during hot and humid summer months.
Broken Skin: Bacteria exploit entry points like cuts, scrapes, insect bites, or rashes from conditions like eczema or poison ivy.
Contact Sports: Sports involving skin to skin contact, such as wrestling, can facilitate its spread.
Poor Hygiene: While not a direct cause, inadequate handwashing can contribute to its transmission.
Pre existing Skin Conditions: Individuals with dermatitis or scabies are more susceptible.
What Are the First Signs and Symptoms of Impetigo?
what-are-the-first-signs-and-symptoms-of-impetigoThe initial signs of impetigo are red, itchy sores that can appear anywhere on the body but are most common on the face, arms, and legs. These symptoms differ slightly depending on the type of impetigo.
Non Bullous Impetigo: This is the most common form, accounting for about 70 percent of cases.
Starts as small red sores or blisters.
The sores quickly rupture, leaving behind a moist, red base.
A characteristic honey colored or yellowish brown crust forms over the sore.
The sores are often itchy but not typically painful.
Bullous Impetigo: This form is caused exclusively by Staphylococcus aureus bacteria that produce a specific toxin.
Presents as larger, fluid filled blisters known as bullae.
These blisters are painless and can last longer without bursting.
When they do rupture, they leave a yellowish crust, though it is often less thick than in the non bullous type.
This type is more common in newborns and infants.
A more severe form of impetigo that penetrates deeper into the skin is called ecthyma. It creates painful, pus filled sores that turn into deep ulcers with a thick crust and can lead to scarring.
How is Impetigo Diagnosed?
how-is-impetigo-diagnosedA healthcare provider can usually diagnose impetigo based on a visual examination of the characteristic sores. The distinct appearance of the honey colored crusts is a key diagnostic feature. In some cases, to confirm the diagnosis or identify the specific bacteria causing the infection, especially if initial treatment is not effective, a doctor may take a swab of the fluid from a sore. This sample is then sent to a laboratory for a bacterial culture to determine the exact cause and guide antibiotic selection.
What is the Fastest Way to Cure Impetigo?
what-is-the-fastest-way-to-cure-impetigoThe fastest way to cure impetigo involves prompt treatment with antibiotics prescribed by a healthcare professional. Treatment clears the infection, alleviates symptoms, and prevents both the spread to others and the development of more serious complications like cellulitis.
Topical Antibiotics: For mild, localized cases, a prescription antibiotic ointment or cream is the primary treatment. Mupirocin or retapamulin are commonly prescribed and applied directly to the sores several times a day for five to ten days.
Oral Antibiotics: If the infection is widespread, severe, or if the bullous type is present, a doctor will prescribe oral antibiotics. These medications, such as amoxicillin clavulanate, cephalosporins, or clindamycin, work systemically to fight the infection. It is vital to complete the full course of antibiotics even if the skin appears to have healed.
Home Care: Gently washing the affected areas with soap and water and soaking the crusts to remove them can help the antibiotic ointment penetrate the skin more effectively. Covering the sores with a light bandage can help prevent spreading the infection to other parts of the body or to other people.
How Can I Manage Life with Impetigo?
how-can-i-manage-life-with-impetigo"When the first spots appeared on my son's face, I thought it was just a rash. But it spread so fast and the crusts looked awful. Getting the diagnosis and seeing the antibiotic cream work so quickly was a huge relief for our whole family." – an anonymous patient, United States.
Managing impetigo effectively revolves around treating the infection and preventing its spread. Good hygiene is paramount. This includes frequent handwashing with soap and water, especially after touching the affected skin. To prevent transmission, do not share towels, clothing, or bedding with an infected person until the infection has cleared. Children should be kept home from school or daycare until they are no longer contagious, which is typically 24 hours after starting antibiotic treatment.
When Should I See a Doctor for Impetigo?
when-should-i-see-a-doctor-for-impetigoYou should see a doctor as soon as you suspect you or your child has impetigo. Early diagnosis and treatment are key to a quick recovery and preventing the spread of the infection. It is especially important to seek medical care if:
The sores are spreading rapidly or are widespread.
A fever develops.
The sores are painful.
The skin does not begin to heal after three days of treatment.
The infection returns after treatment.
A newborn or infant shows any signs of impetigo.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaFor any dermatological concerns, including skin infections or aesthetic procedures, the following clinics in South Korea are recognized for their expertise in various skin and body treatments.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
All-line Clinic | Lifting and Body Contouring | Mapo-gu, Seoul, South Korea | ||
Plans Clinic | Facial and Body Plastic Surgery | Gangnam-gu, Seoul, South Korea | ||
BLS Clinic | Lifting and Anti Aging Treatments | Gangnam-gu, Seoul, South Korea | ||
Natural Beauty Clinic | Rhinoplasty and Facial Contouring | Gangnam-gu, Seoul, South Korea | ||
Clinic Trinity Raffaello | Anti Aging, Stem Cell Therapy | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Oracle Dermatology | Dermatology, Lifting, Lasers | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Qbq Clinic | Dermatology, Body Contouring, Lasers | Gangnam-gu, Seoul, South Korea | ||
Oracle Clinic Cheongdam | Dermatology, Lifting | Gangnam-gu, Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaThe clinics listed above offer a wide range of advanced dermatological and aesthetic procedures. While these are not treatments for an active impetigo infection, they represent the types of expert services available for overall skin health, rejuvenation, and body contouring in South Korea.
Treatment/Procedure Name | Duration | Hospitalization? | Avg. Cost (USD) in S. Korea | Contact |
|---|---|---|---|---|
High Fat Dissolving Injection | 20-30 mins | Not Needed | $200 - $500 | |
Triple Body Injection | 30-45 mins | Not Needed | $400 - $800 | |
Titanium Lifting | 60-90 mins | Not Needed | $2500 - $4500 | |
Face Onda Lifting | 30-60 mins | Not Needed | $1500 - $3000 | |
Body Onda Lifting | 40-75 mins | Not Needed | $2000 - $4000 | |
Combination Skin Boosters | 45-60 mins | Not Needed | $500 - $1200 | |
Jaw Botox | 10-15 mins | Not Needed | $150 - $400 | |
Calf Botox | 20-30 mins | Not Needed | $400 - $800 | |
Rejuran Healer | 30-45 mins | Not Needed | $300 - $600 | |
Vitaran | 30-45 mins | Not Needed | $250 - $500 | |
Juvelook | 45-60 mins | Not Needed | $400 - $700 | |
Skin Botox – Full Face | 30-60 mins | Not Needed | $400 - $900 | |
Abdomen Fat Dissolving Injection | 20-30 mins | Not Needed | $300 - $700 | |
Arm Fat Dissolving Injection | 20-30 mins | Not Needed | $250 - $600 | |
High Lower Body Fat Dissolving Injection | 30-45 mins | Not Needed | $500 - $1000 | |
Face Fat Dissolving Injection | 20-30 mins | Not Needed | $200 - $500 | |
Mirajet Needle Free Injector | 30-60 mins | Not Needed | $600 - $1200 | |
Lizne | 30-45 mins | Not Needed | $350 - $650 | |
Titanium Fat Dissolving Treatment | 60-90 mins | Not Needed | $2800 - $4800 | |
Lifting Treatments | 30-90 mins | Not Needed | $500 - $5000 | |
Laser Treatment | 20-60 mins | Not Needed | $200 - $1500 | |
Body Contouring | 30-120 mins | Not Needed | $500 - $8000+ | |
Skin Booster | 30-60 mins | Not Needed | $300 - $800 | |
Laser Hair Removal | 10-20 mins | Not Needed | $50 - $200 | |
Thermage FLX | 60-90 mins | Not Needed | $2000 - $4000 | |
Shurink | 30-45 mins | Not Needed | $400 - $900 | |
Heart Lifting | 60 mins | Not Needed | $1500 - $3500 | |
Inmode | 30-60 mins | Not Needed | $800 - $2500 | |
Ulthera | 60-90 mins | Not Needed | $2000 - $4500 | |
Scar & Pore Laser | 30-60 mins | Not Needed | $400 - $1000 | |
Pigmentation & Whitening | 20-40 mins | Not Needed | $200 - $600 | |
Secret Laser | 45-75 mins | Not Needed | $600 - $1200 | |
Acne Peeling | 30-45 mins | Not Needed | $150 - $400 | |
Pregnancy Skin Care | 45-60 mins | Not Needed | $150 - $300 | |
miraDry | 60-90 mins | Not Needed | $2000 - $3500 | |
V Contour Injection | 20-30 mins | Not Needed | $250 - $600 | |
Body Sculpting Injection | 30-45 mins | Not Needed | $400 - $900 | |
Body Botox | 20-40 mins | Not Needed | $500 - $1200 | |
Diet Injection | 5-10 mins | Not Needed | $50 - $150 | |
Hydrogen Toning | 45-60 mins | Not Needed | $150 - $300 | |
Platinum Photothermal Therapy | 45-60 mins | Not Needed | $300 - $700 | |
Scalp Stabilization Treatment | 45-60 mins | Not Needed | $200 - $500 |
What Are Common Questions About Impetigo?
what-are-common-questions-about-impetigoThis section addresses practical questions patients often have about impetigo.
1. Is impetigo serious?
1.-is-impetigo-seriousFor most healthy individuals, impetigo is not serious and resolves without complications when treated properly with antibiotics. However, if left untreated, it can lead to more serious conditions like cellulitis, an infection of the deeper layers of skin, or kidney problems in rare cases, specifically post streptococcal glomerulonephritis.
2. How long is impetigo contagious?
2.-how-long-is-impetigo-contagiousImpetigo is contagious until the sores have crusted over and healed, or for 24 hours after beginning effective antibiotic treatment. It is crucial to follow a doctor's guidance on when it is safe to return to school or work to prevent spreading the infection to others.
3. Can impetigo leave scars?
3.-can-impetigo-leave-scarsSuperficial impetigo, including both the non bullous and bullous types, typically does not leave scars once the crusts have healed. The more severe form, ecthyma, penetrates deeper into the skin and can result in scarring. To minimize the risk of scarring, avoid picking or scratching the sores.
4. What is the difference between bullous and non bullous impetigo?
4.-what-is-the-difference-between-bullous-and-non-bullous-impetigoThe main difference is their appearance. Non bullous impetigo, the most common type, features small, rapidly bursting blisters that form a honey colored crust. Bullous impetigo is characterized by large, floppy blisters that contain a clear or yellowish fluid and are less likely to rupture quickly.
5. Can adults get impetigo?
5.-can-adults-get-impetigoYes, while it is much more common in children, adults can also get impetigo. In adults, it often occurs as a secondary infection to another skin problem, such as eczema, or after an injury that breaks the skin, providing an entry point for bacteria.
Take Control of Your Skin Health: Inquire About Expert Impetigo Care Now!
take-control-of-your-skin-health:-inquire-about-expert-impetigo-careDealing with any skin condition can be stressful, but you do not have to manage it alone. Seeking timely, professional care is the most important step towards healing and peace of mind. For a seamless and transparent process, you can inquire about dermatological consultations at top Korean clinics directly through a dedicated service. A Care Manager will provide end to end support, from your initial questions to post treatment follow up, ensuring you receive the best possible care. And Start Your Confidential Inquiry with CloudHospital to connect with world class dermatologists today.