The clinical information regarding Muscle Strains in this article has been rigorously verified against the latest guidelines from the American Academy of Orthopaedic Surgeons (AAOS) and primary research from databases like PubMed. This piece was reviewed for accuracy and patient-centric clarity and was last updated in October 2023.
Introduction
introductionA sudden sharp pain during activity, followed by weakness and soreness these are the classic signs of a muscle strain, an injury that affects millions of people annually, from professional athletes to weekend warriors. Also known as a pulled muscle, this common injury can range from a minor annoyance to a debilitating tear requiring medical intervention. This guide offers a comprehensive, medically-backed overview of muscle strains, providing clear information on their causes, diagnosis, and the path to a safe and complete recovery.
What is a Muscle Strain?
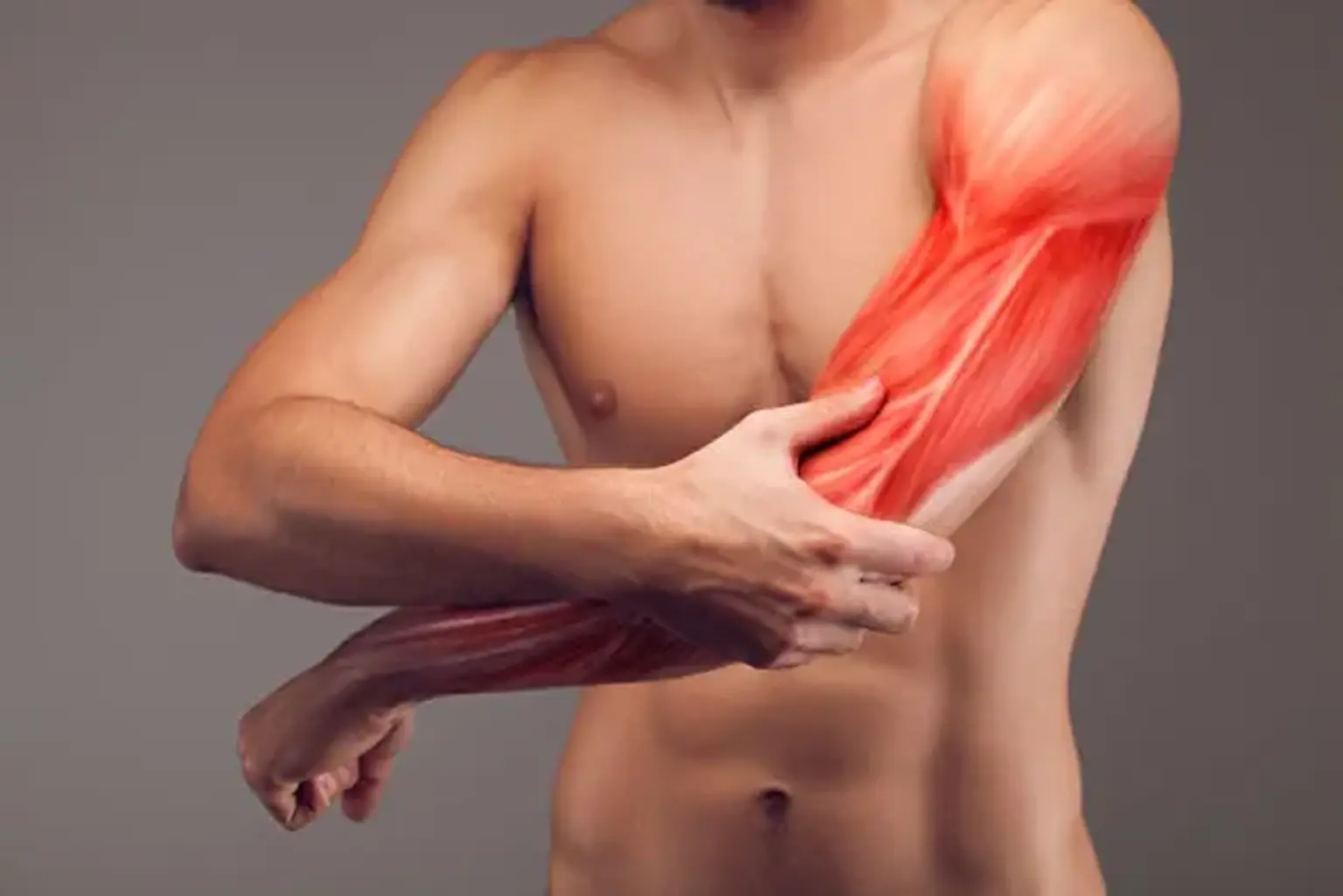
what-is-a-muscle-strainA muscle strain is an injury to a muscle or its attaching tendon. It occurs when muscle fibers are overstretched or torn due to fatigue, overuse, or improper use. Strains can happen in any muscle but are most common in the lower back, neck, shoulder, and hamstring the muscle behind the thigh. The injury damages the small blood vessels within the muscle, leading to local bleeding or bruising, and pain caused by irritation of the nerve endings in the area.
What are the Different Grades of a Muscle Strain?
what-are-the-different-grades-of-a-muscle-strainThe first step in determining treatment is to accurately grade the severity of the injury. Orthopedic specialists classify muscle strains into three grades based on the extent of fiber damage.
Grade 1: Only a few muscle fibers are stretched or torn. The muscle is tender and painful, but it retains its normal strength. Movement is minimally limited.
Grade 2: A greater number of muscle fibers are torn, resulting in more significant pain, swelling, and a noticeable loss of strength. You may see some mild bruising.
Grade 3: The muscle is completely torn or ruptured. This is a serious injury characterized by severe pain, swelling, tenderness, and discoloration. There is a complete loss of muscle function, and sometimes a visible gap or dent can be seen or felt under the skin where the muscle has torn.
What are the Common Causes and Risk Factors?
what-are-the-common-causes-and-risk-factorsA muscle strain, or acute strain, is typically caused by a single event, such as a sudden acceleration, a fall, lifting a heavy object improperly, or throwing. Chronic strains, however, are the result of repetitive, prolonged movement, often related to sports like gymnastics, tennis, and golf, or occupations that require repetitive motions.
Key risk factors include:
Inadequate Warm-up: Cold muscles are less pliable and more susceptible to injury.
Poor Flexibility: Tight muscles cannot safely handle the stress of sudden movements.
Overexertion and Fatigue: Fatigued muscles lose their ability to absorb energy, making them more prone to tearing.
Previous Injury: A previously strained muscle may have scar tissue that is weaker and less flexible than healthy muscle tissue.
What are the Symptoms and Signs of a Muscle Strain?
what-are-the-symptoms-and-signs-of-a-muscle-strainThe symptoms of a muscle strain depend on the severity of the injury but commonly include one or more of the following:
Sudden onset of pain.
Soreness and tenderness in the affected area.
Limited range of motion.
Bruising or discoloration appearing over a few days.
Swelling.
A knotted-up feeling or muscle stiffness.
Muscle spasms.
Weakness in the muscle.
A popping or snapping sensation at the time of injury often indicates a Grade 2 or 3 strain.
How is a Severe Muscle Strain Diagnosed?
how-is-a-severe-muscle-strain-diagnosedA clinician can often diagnose a muscle strain through a physical examination and by discussing how the injury occurred. For mild strains, this is usually sufficient. However, for a definitive diagnosis of a severe Grade 2 or 3 strain, imaging tests are often required.
Initial Consultation: A doctor will assess your range of motion, muscle strength, and pinpoint the location of the pain.
Musculoskeletal Ultrasound: This imaging technique uses sound waves to create real-time images of muscles, tendons, and ligaments. It is highly effective for identifying tears, fluid collection hematomas, and assessing the extent of soft tissue injury.
Magnetic Resonance Imaging MRI: An MRI provides highly detailed images of soft tissues and is considered the gold standard for diagnosing the precise location and severity of a muscle tear. It is particularly useful for planning surgical intervention if required.
What are the Treatment Options for a Muscle Strain?
what-are-the-treatment-options-for-a-muscle-strainTreatment is tailored to the grade of the strain. The primary goal is to reduce pain and swelling, restore movement and strength, and prevent further injury.
Immediate and Non-Surgical Treatment Grade 1 & 2
immediate-and-non-surgical-treatment-(grade-1-and-2)The fastest way to begin healing a mild to moderate torn muscle is by following the P.R.I.C.E. principle for the first 24-48 hours.
Protection: Protect the injured area from further harm. You might use a sling or crutches.
Rest: Avoid activities that cause pain. Rest is essential for healing.
Ice: Apply an ice pack for 15-20 minutes every 2-3 hours to reduce swelling and pain.
Compression: Use an elastic compression bandage to limit swelling.
Elevation: Keep the injured limb elevated above the level of your heart.
Over-the-counter nonsteroidal anti-inflammatory drugs NSAIDs like ibuprofen can help manage pain and inflammation. After the initial phase, a structured physical therapy program is crucial for regaining strength and flexibility.
Advanced and Surgical Options Grade 3
advanced-and-surgical-options-(grade-3)A complete muscle rupture Grade 3 strain may require surgical intervention.
Surgical Repair: Surgery involves reattaching the torn muscle and tendon. This is often performed for severe hamstring tears or ruptures of the biceps or Achilles tendon to restore full function. Procedures like [arthroscopic surgery] may be used for associated joint injuries.
Regenerative Medicine: For certain injuries, advanced treatments like Orthopedic Stem Cell Therapy are being used to enhance healing. These therapies use the body's own healing agents to potentially accelerate the repair of damaged muscle tissue.
"I felt a loud pop in my calf playing football and couldn't walk. The pain was immediate and intense. Getting an MRI that showed a Grade 3 tear was scary, but it was also the first step toward a real plan. The structured rehab was tough, but feeling the strength come back week by week was the biggest relief." – an anonymous patient, Australia.
When Should I See a Doctor for a Pulled Muscle?
when-should-i-see-a-doctor-for-a-pulled-muscleYou should seek medical attention if you experience any of the following signs after a muscle injury:
You heard a popping sound at the time of injury.
You are unable to walk or bear weight on the limb.
There is significant swelling, pain, fever, or open cuts.
The pain does not subside after a week of home care with the P.R.I.C.E. method.
There is a visible, significant deformity or lump in the muscle.
These symptoms can indicate a severe strain or a complete rupture that requires professional medical evaluation and a formal treatment plan.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaSouth Korea is recognized for its advanced orthopedic centers, many of which specialize in sports medicine, minimally invasive surgery, and comprehensive rehabilitation programs ideal for treating muscle strains and related injuries.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
Seoul Yes Hospital | Non-surgical spine and joint treatments | Yongin-si, Gyeonggi-do, South Korea | ||
Asan Medical Center | World-class, multi-disciplinary research hospital | Seoul, Songpa, South Korea | ||
Bumin Hospital Group | Specialized in joint and spine surgery | Haeundae, Busan, South Korea | ||
Nanoori Hospital, Gangnam | Minimally invasive spine and joint treatment | Gangnam, Seoul, South Korea | ||
Himchan Hospital | High volume joint replacement and arthroscopic surgery | Bupyeong, Incheon, South Korea | ||
Nasaret International Hospital | Comprehensive rehabilitation and international patient services | Yeonsu-gu, Incheon, South Korea | ||
Gachon University Gil Medical Center | University hospital, advanced medical research | Namdong-gu, Incheon, South Korea | ||
Wooridul Hospital Gangnam | Global leader in spine surgery and treatments | Gangnam, Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaThe following table outlines advanced orthopedic and rehabilitation procedures available in South Korea that may be relevant for treating severe strains or associated injuries. Costs are estimates and can vary based on the specifics of the case.
Treatment/Procedure Name | Treatment Duration | Hospitalization? | Avg Cost Range (USD) in S. Korea | Contact |
|---|---|---|---|---|
Total knee replacement | 1-2 hours | Needed (2-4 days) | $16,000 - $25,000 | |
Artificial disc replacement | 2-3 hours | Needed (2-3 days) | $18,000 - $28,000 | |
Artificial joint replacement | 1-3 hours | Needed (2-4 days) | $15,000 - $26,000 | |
Minimally invasive spinal fusion surgery | 2-4 hours | Needed (3-5 days) | $19,000 - $30,000 | |
Stem cell-based cartilage regeneration | 1 hour | Not Needed | $8,000 - $15,000 | |
Orthopedic Stem Cell Therapy | 1 hour | Not Needed | $5,000 - $12,000 | |
Complex neuromuscular treatment | 1 hour | Not Needed | $3,000 - $9,000 | |
Spinal endoscopic treatment | 1-2 hours | Needed (1-2 days) | $12,000 - $20,000 | |
High tibial osteotomy | 1.5-2.5 hours | Needed (3-5 days) | $10,000 - $17,000 | |
ACL reconstruction | 1-2 hours | Needed (1-2 days) | $8,000 - $15,000 | |
Ankle ligament reconstruction | 1-1.5 hours | Needed (1 day) | $6,000 - $11,000 | |
Arthroscopic surgery (e.g., knee, shoulder) | 45-90 mins | Needed (1 day) | $5,000 - $10,000 | |
Microscopic decompression surgery | 1-2 hours | Needed (1-2 days) | $10,000 - $18,000 | |
Percutaneous vertebroplasty | 30-60 mins | Needed (1 day) | $7,000 - $12,000 | |
Hallux valgus correction | 1 hour | Needed (1 day) | $5,000 - $9,000 | |
Epidural neuroplasty | 30-45 mins | Not Needed | $1,500 - $3,500 | |
Zero-gravity spinal decompression | 30 mins | Not Needed | $200 - $400 | |
Extracorporeal shock wave therapy | 15-20 mins | Not Needed | $250 - $500 |
Common Questions About Muscle Strain Recovery
common-questions-about-muscle-strain-recovery1. How long does a muscle strain take to heal?
1.-how-long-does-a-muscle-strain-take-to-healThe recovery time for a muscle strain depends entirely on its grade. A Grade 1 strain may resolve in a few weeks with proper care. A Grade 2 strain can take up to three months. A Grade 3 strain, especially one requiring surgery, may require six months or longer for a full recovery and return to sport.
2. What's the difference between a sprain and a strain?
2.-what's-the-difference-between-a-sprain-and-a-strainA strain is an injury to a muscle or a tendon the tissue that connects muscle to bone. A sprain is an injury to a ligament the tissue that connects two bones together at a joint. While symptoms can be similar, the injured structure is different.
3. Can I use heat on my muscle strain?
3.-can-i-use-heat-on-my-muscle-strainHeat should not be used during the initial, acute phase of the injury the first 48-72 hours, as it can increase blood flow and worsen swelling. After this initial period, applying moist heat can help to increase blood flow to the area, relax tight muscles, and relieve soreness before stretching or rehabilitation exercises.
4. Is it okay to stretch a pulled muscle?
4.-is-it-okay-to-stretch-a-pulled-muscleGentle stretching should only begin after the acute pain and swelling have subsided, typically after a few days. Overstretching an injured muscle too early can worsen the damage and delay healing. All stretching during recovery should be slow, gentle, and guided by a physical therapist.
5. How can I prevent muscle strains in the future?
5.-how-can-i-prevent-muscle-strains-in-the-futurePrevention is key. Always perform a dynamic warm-up before exercise to prepare your muscles. Incorporate regular flexibility and strengthening exercises into your routine. Avoid pushing yourself too hard when you are tired or in pain, and allow for adequate recovery time between workouts.
6. Can a muscle strain heal on its own?
6.-can-a-muscle-strain-heal-on-its-ownMild Grade 1 strains often heal well on their own with rest and home care. Moderate Grade 2 strains may also heal without surgery but almost always require a structured rehabilitation program to restore full strength and prevent re-injury. Severe Grade 3 tears will not heal correctly on their own and typically require medical, and often surgical, intervention.
Regain Your Mobility: Start Your Muscle Strain Recovery Plan Now!
regain-your-mobility:-start-your-muscle-strain-recovery-planA muscle strain can be a significant setback, but a correct diagnosis and a professionally guided treatment plan are your fastest route back to an active life. The world-class orthopedic centers in South Korea offer a full spectrum of care, from advanced diagnostics to cutting-edge surgical and regenerative therapies. Taking the next step can provide clarity and a definitive plan for your recovery. For a seamless and transparent process, a dedicated Care Manager can provide end-to-end support, from your initial questions to post-recovery care. And Start Your Confidential Inquiry through CloudHospital to receive a personalized treatment plan and quote from leading specialists.