The clinical information regarding Periodontics in this article has been rigorously verified against the latest guidelines from the American Academy of Periodontology (AAP) and primary research from databases like PubMed. This piece was reviewed for accuracy and patient-centric clarity and was last updated in October 2023.
Introduction
introductionUnderstanding the health of your gums is fundamental to your overall well-being. Periodontics, the dental specialty focused on the structures supporting your teeth, is often misunderstood. To provide definitive clarity, we present this expert-driven Q&A. Here, a board-certified periodontist addresses the most common and critical questions patients have about gum disease, its treatment, and prevention, empowering you with knowledge for a healthier smile.
What are the first signs of periodontal disease?
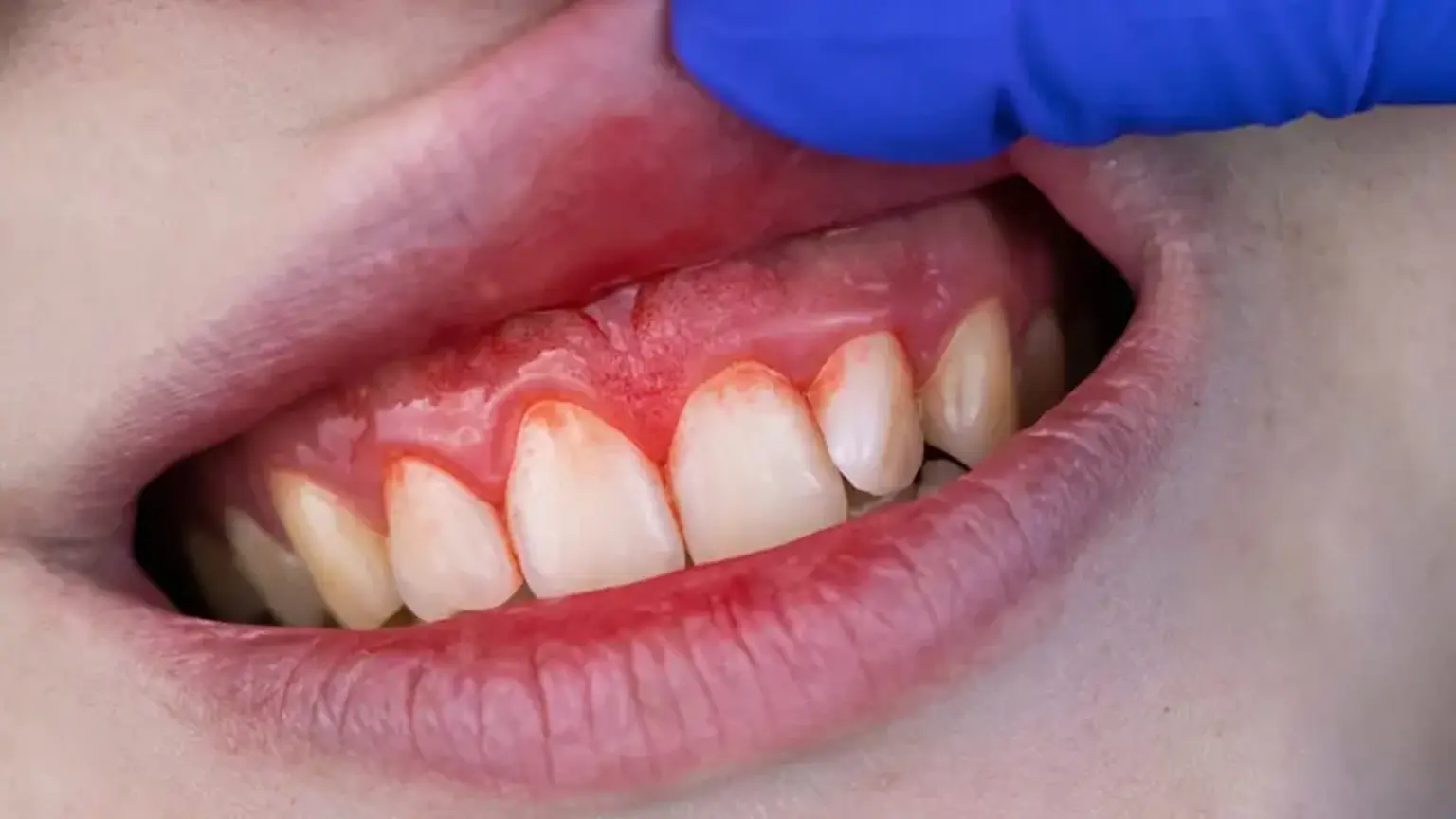
what-are-the-first-signs-of-periodontal-diseaseThe initial signs of periodontal disease are often subtle but should never be ignored. The earliest stage, known as gingivitis, typically presents with gums that are red, swollen, and bleed easily, especially when brushing or flossing. You might also notice persistent bad breath halitosis or a bad taste in your mouth. As the disease progresses to periodontitis, more serious signs appear, including gum recession like making teeth look longer, the formation of pockets between teeth and gums, loose or shifting teeth, and changes in the way your teeth fit together when you bite. Pain is not always a primary symptom in the early stages, which is why regular dental check-ups are critical for early detection.
What is the difference between gingivitis and periodontitis?
what-is-the-difference-between-gingivitis-and-periodontitisGingivitis and periodontitis are two stages of the same disease process, but their implications are vastly different.
Gingivitis: This is the earliest, mildest form of periodontal disease. It is an inflammation of the gums caused by the buildup of dental plaque at the gumline. A key characteristic of gingivitis is that it is reversible with professional treatment and diligent home care. The inflammation is confined to the gum tissue, and no irreversible bone or tissue damage has occurred.
Periodontitis: If gingivitis is left untreated, it can advance to periodontitis. At this stage, the inflammation has spread below the gumline, and the body's immune response begins to destroy the bone and connective tissue that hold the teeth in place. This damage is irreversible. Pockets form between the gums and teeth, which deepen and harbor more bacteria, leading to further bone loss, tooth mobility, and eventual tooth loss.
Can periodontal disease be cured completely?
can-periodontal-disease-be-cured-completelyThis is a critical question with a nuanced answer. Gingivitis, the initial stage, can be completely cured and reversed with professional cleanings and excellent oral hygiene. However, once the disease progresses to periodontitis, the bone and tissue loss that has occurred cannot be naturally regenerated. Therefore, periodontitis cannot be cured in the traditional sense of reversing all damage.
The goal of periodontitis treatment is to halt the progression of the disease, control the infection, and maintain the existing oral structures. This is achieved through procedures like scaling and root planing and, if necessary, surgical interventions. Successful management turns an active disease into a stable, manageable, chronic condition, much like managing diabetes or hypertension. Lifelong, diligent maintenance is required to prevent its recurrence.
What does periodontal treatment involve?
what-does-periodontal-treatment-involvePeriodontal treatment is tailored to the specific stage and severity of the disease. The process typically follows a phased approach:
Initial Diagnosis and Evaluation: A periodontist will perform a comprehensive examination, including measuring the depth of the pockets around your teeth with a periodontal probe. Dental X-rays are taken to assess for any bone loss.
Non-Surgical Treatment (Phase I Therapy): For most patients, treatment begins with a deep cleaning procedure called scaling and root planing.
Scaling: This removes plaque and hardened tartar calculus from above and below the gumline.
Root Planing: This smooths the tooth roots to help the gums reattach to the teeth and discourage future bacterial accumulation.
Surgical Treatment (Phase II Therapy): If deep pockets and significant bone loss persist after non-surgical treatment, surgery may be required. Common procedures include:
Gingival Flap Surgery (Pocket Reduction): The gums are lifted back to remove tartar from deep pockets, which are then sutured back in place snugly around the tooth.
Bone Grafting: Uses natural or synthetic bone to replace bone destroyed by periodontitis, helping to promote new bone growth and provide a more stable foundation for teeth.
Soft Tissue Grafts: Reinforce thin gums or fill in areas where gums have receded.
Maintenance (Phase III Therapy): This is the most crucial phase for long-term success. After active treatment, patients are placed on a regular maintenance schedule, typically involving cleanings every 3-4 months, to prevent the disease from recurring.
What are the most important takeaways for maintaining gum health?
what-are-the-most-important-takeaways-for-maintaining-gum-healthBased on extensive clinical experience, the most critical factors for patients to understand can be summarized into four key points:
Prevention is Paramount: It is far easier and less costly to prevent gum disease than to treat it. This requires consistent brushing twice a day, flossing daily, and attending regular dental check-ups and cleanings.
Don't Ignore the "Pink in the Sink": Bleeding gums are never normal. They are the earliest warning sign of inflammation. Address it immediately with improved hygiene and a dental visit.
Gum Health is Systemic Health: A large body of evidence links periodontitis to other systemic conditions, including cardiovascular disease, diabetes, and respiratory infections. Managing your gum health is an investment in your overall health.
Treatment is a Partnership: A periodontist can control the disease, but long-term stability depends entirely on the patient's commitment to meticulous home care and regular maintenance appointments.
"I was so worried about my gums receding and what the treatment would feel like. After my consultation, all the steps were laid out so clearly. I finally understood what was happening and what we needed to do. That clarity was the most reassuring part of the whole process." – an anonymous patient, USA.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaWebsite | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
OnO Dental Clinic | Advanced Implantology | Gangnam-gu, Seoul, South Korea | ||
Ye-on Dental Clinic | Implants & Orthodontics | Namdong-gu, Incheon, South Korea | ||
S-PLANT Dental Hospital | Digital & Implant Dentistry | Gangnam-gu, Seoul, South Korea | ||
Miju Dental Clinic | Comprehensive Aesthetic Dentistry | Busanjin-gu, Busan, South Korea | ||
Su Dental Hospital | High-Risk & Specialized Implants | Gangnam-gu, Seoul, South Korea | ||
Columbia Dental Hospital | Full-Service Family & Cosmetic Dentistry | Suwon-si, Gyeonggi-do, South Korea | ||
Dasan Barun Dental Clinic | Specialized Orthodontic Care | Namyangju-si, Gyeonggi-do, South Korea | ||
Yonsei Hana Dental Clinic | General & Cosmetic Dentistry | Gyeonggi-do,Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaTreatment/Procedure Name | Duration | Hospitalization? | Avg. Cost Range (USD) in S. Korea | Contact |
|---|---|---|---|---|
Gingival Flap Surgery | 1-3 hours | Not Needed | $500 - $2,000 | |
Gum Contouring | 30-60 mins | Not Needed | $300 - $1,500 | |
Dental Implant Surgery | 1-2 hours | Not Needed | $1,000 - $2,500 | |
Same-Day Implant | 2-4 hours | Not Needed | $2,000 - $4,500 | |
Bone Grafting | 1-2 hours | Not Needed | $400 - $1,200 | |
Root Canal Treatment | 160-90 mins | Not Needed | $400 - $1,000 | |
Zirconia Crowns | 2 visits | Not Needed | $600 - $1,200 | |
Laminates (Porcelain Veneers) | 2 visits | Not Needed | $700 - $1,500 | |
Resin-Based Composites | 30-60 mins | Not Needed | $100 - $400 | |
Invisalign Braces | 12-18 months | Not Needed | $4,500 - $8,000 | |
Temporomandibular Joint (TMJ) Treatment | 30 mins | Not Needed | $500 - $2,500 | |
Professional Teeth Whitening | 60-90 mins | Not Needed | $300 - $800 |
Frequently Asked Questions About Periodontal Care
frequently-asked-questions-about-periodontal-care1. Is periodontal surgery painful?
1.-is-periodontal-surgery-painfulPatient comfort is a top priority. Periodontal surgeries are performed under local anesthesia, so you will not feel pain during the procedure itself. Post-operative discomfort, swelling, and some soreness are expected, but this is typically managed effectively with prescribed pain medications and cold compresses. Most patients report the discomfort is manageable and subsides within a few days.
2. What are the major risk factors for developing gum disease?
2.-what-are-the-major-risk-factors-for-developing-gum-diseaseWhile plaque buildup is the direct cause, several factors increase your risk. Smoking is one of the most significant risk factors. Others include diabetes, hormonal changes in girls and women, certain medications that reduce saliva flow, genetic susceptibility, and illnesses that interfere with the immune system, like cancer or AIDS.
3. How long does recovery from scaling and root planing take?
3.-how-long-does-recovery-from-scaling-and-root-planing-takeRecovery from scaling and root planing is typically quick. Your gums may be sensitive for a few days, and you might experience slight tenderness or bleeding. Your periodontist will likely recommend a soft food diet for a day or two and may suggest a desensitizing toothpaste. Most patients return to their normal routines the same or the next day.
4. Can children get periodontal disease?
4.-can-children-get-periodontal-diseaseYes, children can develop gum disease. While aggressive periodontitis is less common in children than adults, gingivitis is very common. It can be caused by poor oral hygiene, hormonal fluctuations during puberty puberty gingivitis, or underlying medical conditions. Establishing good brushing and flossing habits early is the best defense.
5. Are there any new or emerging treatments for periodontitis?
5.-are-there-any-new-or-emerging-treatments-for-periodontitisThe field is constantly advancing. One exciting area is laser-assisted periodontal therapy, which can be used to remove inflamed gum tissue and tartar with less discomfort and a shorter recovery time for some patients. Another area of intense research is guided tissue and bone regeneration, which uses special membranes and growth factor proteins to stimulate the body's natural ability to regenerate bone and tissue lost to disease. These advanced treatments offer hope for more predictable and less invasive management in the future.
Take the First Step Towards Healthier Gums Today!
take-the-first-step-towards-healthier-gumsUnderstanding your periodontal health is the first, most powerful step toward preserving your smile for a lifetime. Armed with the right information, you can make confident decisions about your care. Don't let uncertainty or fear hold you back from achieving a healthy, stable foundation for your teeth. The journey begins with a professional consultation. We provide a seamless, transparent process, connecting you with top-tier dental specialists in South Korea. Your dedicated Care Manager will provide end-to-end support, from your initial questions to post-recovery care. To Start Your Confidential Inquiry with CloudHospital and get a free, personalized treatment plan to reclaim your gum health.