The clinical information regarding Keratosis Pilaris in this article has been rigorously verified against the latest guidelines from the American Academy of Dermatology (AAD) and primary research from databases like PubMed. This piece was reviewed for accuracy and patient-centric clarity and was last updated in August 2025.
Introduction
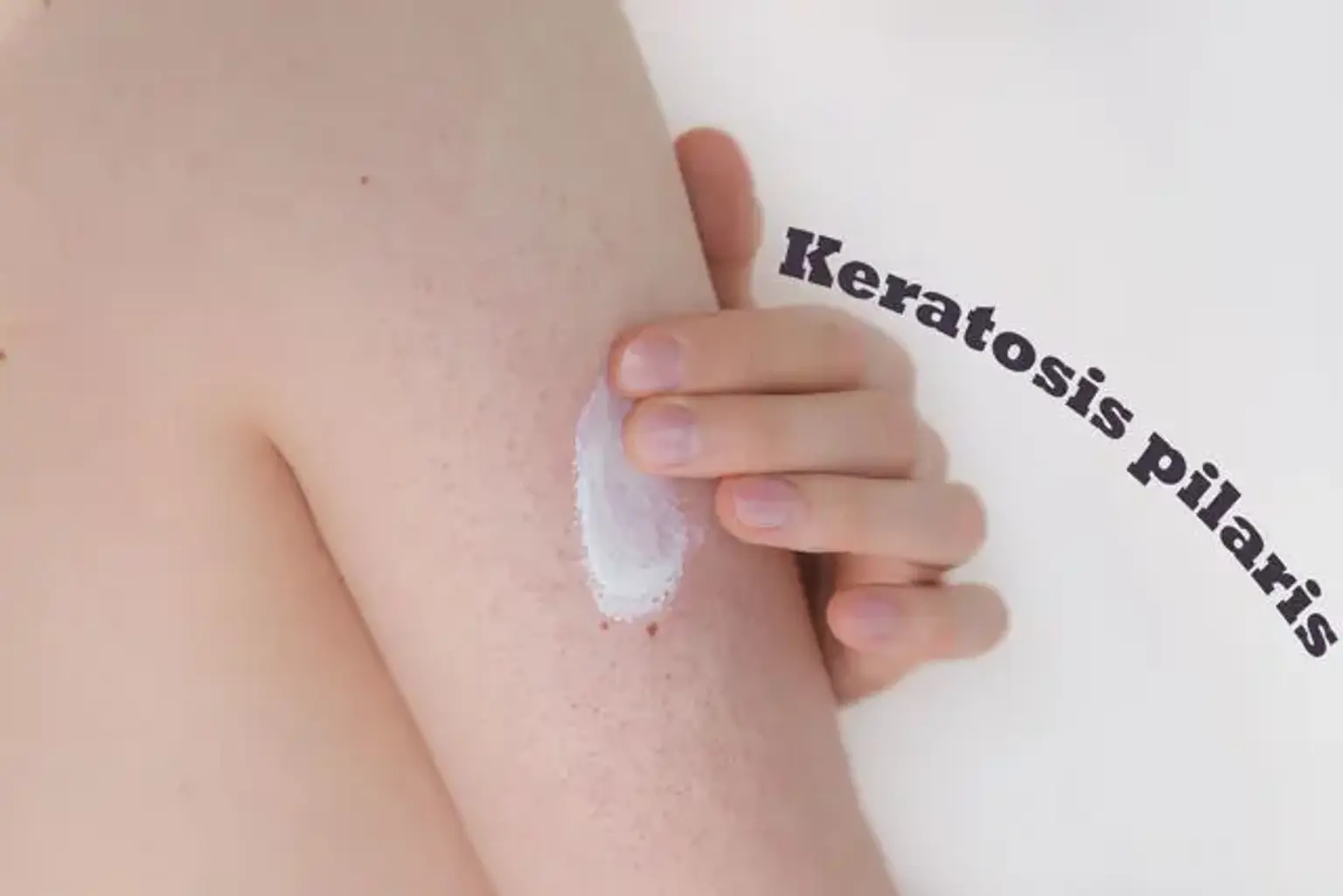
introductionKeratosis Pilaris (KP) is an exceedingly common and harmless skin condition, often referred to as chicken skin due to its characteristic appearance. It affects people of all ages, though it is particularly prevalent in children and adolescents, with many cases improving or resolving by age 30. While it poses no medical danger, the rough texture and visible bumps can be a source of cosmetic concern. This guide offers a comprehensive overview for those seeking to understand and manage this widespread dermatological condition.
What is Keratosis Pilaris?
what-is-keratosis-pilarisKeratosis Pilaris is a benign condition that occurs when a protein called keratin, a natural protein that helps form hair, nails, and the skin's outer layer, builds up and forms hard plugs within hair follicles. This clogging of the pores blocks the opening of growing hair follicles, resulting in the formation of small, rough bumps. The bumps can appear anywhere on the body where hair follicles exist, most commonly on the outer-upper arms, thighs, buttocks, and sometimes the face, particularly on the cheeks. It will never appear on the palms of your hands or the soles of your feet.
What are the Common Causes and Risk Factors for Keratosis Pilaris?
what-are-the-common-causes-and-risk-factors-for-keratosis-pilarisThe precise cause of the excess keratin buildup remains unknown, but the condition is strongly believed to have a genetic component and often runs in families. If a parent has KP, there is a significant chance their child will also develop it.
Certain factors increase the likelihood of developing or experiencing more pronounced Keratosis Pilaris:
Dry Skin: Individuals with dry skin are more prone to KP, and the condition often worsens when there is less humidity in the air, such as during the winter months.
Associated Skin Conditions: It is frequently seen in individuals with other skin conditions like eczema, atopic dermatitis or ichthyosis vulgaris, a condition that causes very dry skin.
Age: It most often begins in early childhood or adolescence and may flare up around puberty.
Excess Body Weight: Some studies have noted a correlation between a higher body mass index (BMI) and the presence of Keratosis Pilaris.
Other Conditions: Asthma and hay fever are also commonly associated with those who have KP.
What do the Symptoms and Signs of Keratosis Pilaris Look Like?
what-do-the-symptoms-and-signs-of-keratosis-pilaris-look-likeThe primary sign of Keratosis Pilaris is its distinct appearance and texture.
Appearance: Patches of small, rough bumps that may resemble goosebumps or the skin of a plucked chicken.
Texture: The affected skin often feels rough and dry, similar to sandpaper.
Color: The bumps can be flesh-colored, white, red, pink, brown, or black, depending on the individual's skin tone and any associated inflammation.
Sensation: The bumps are typically painless, but the surrounding skin can sometimes become dry, itchy, and irritated.
Seasonal Changes: Symptoms often improve in the summer and worsen during colder, drier winter months.
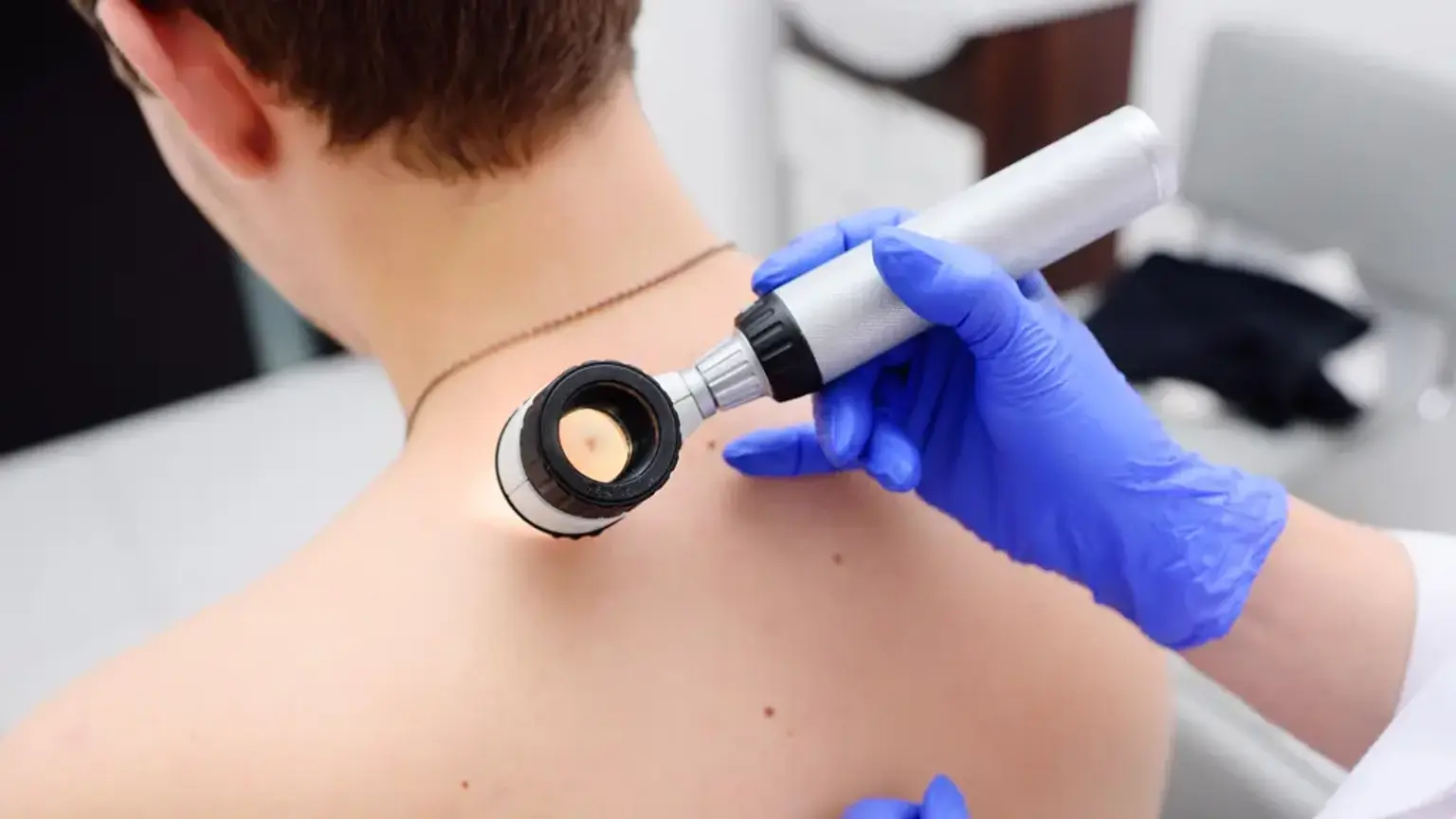
How is Keratosis Pilaris Diagnosed?
how-is-keratosis-pilaris-diagnosedA diagnosis of Keratosis Pilaris is almost always made through a simple physical examination by a healthcare provider or a dermatologist. They will assess the appearance and texture of the skin in the affected areas. No special tests are typically needed, as the condition is visually distinct. In some cases, a dermatoscope may be used to get a magnified view of the hair follicles to confirm the diagnosis.
What are the Treatment Options for Keratosis Pilaris?
what-are-the-treatment-options-for-keratosis-pilarisWhile there is no definitive cure for Keratosis Pilaris, consistent management can significantly improve the skin's appearance and texture.
Treatment focuses on two main goals: removing the buildup of dead skin cells (exfoliation) and preventing dry skin (moisturizing).
Topical Treatments and Skincare
topical-treatments-and-skincareMoisturizing: The foundation of KP management is keeping the skin well-hydrated. Applying a thick, bland moisturizer multiple times a day, especially within five minutes of bathing while the skin is still damp, helps to soften the keratin plugs.
Chemical Exfoliants: Creams and lotions containing specific acids help to loosen and remove dead skin cells. These are known as keratolytics.
Key ingredients to look for include:
Alpha-hydroxy acids (AHAs) like lactic acid and glycolic acid.
Salicylic acid, a beta-hydroxy acid.
Urea, which both exfoliates and moisturizes.
Topical Retinoids: Derived from vitamin A, these creams, such as tretinoin or adapalene, promote cell turnover and can prevent hair follicles from becoming plugged.
Professional Procedures
professional-proceduresFor persistent or more severe cases, a dermatologist may recommend in-office procedures.
Laser and Light Treatments: Different types of lasers can be effective. Some lasers target and reduce the redness and inflammation associated with KP. Other ablative lasers, like the Fractional CO2 laser, can help improve skin texture and reduce the bumps themselves. Laser hair removal has also shown promise by targeting the hair follicle, which is at the root of the issue.
Microdermabrasion: This procedure uses a specialized instrument to intensely exfoliate the top layer of skin, helping to clear the keratin plugs.
Chemical Peels: A dermatologist can apply a stronger concentration of acids like glycolic acid to deeply exfoliate the skin.
How Can I Manage Life with Keratosis Pilaris?
how-can-i-manage-life-with-keratosis-pilaris"For years, I was so self-conscious about the bumps on my arms, especially in the summer. Learning to manage it with a consistent routine of gentle exfoliation and a really good moisturizer didn't make it vanish, but it made my skin so much smoother and gave me my confidence back." – an anonymous patient, United States.
Managing KP is about consistent, gentle care. Harsh scrubbing or picking at the bumps can lead to irritation, inflammation, and potential scarring, making the condition worse. Taking lukewarm (not hot) showers, using mild cleansers, and wearing loose-fitting clothing can also help prevent irritation.
When Should I See a Doctor for Keratosis Pilaris?
when-should-i-see-a-doctor-for-keratosis-pilarisYou should consult a healthcare professional or a dermatologist if:
Over-the-counter treatments and a consistent skincare routine are not improving the condition.
The appearance of your skin is causing significant distress or affecting your self-esteem.
The skin becomes unusually itchy, red, or inflamed.
You are unsure of the diagnosis and want to rule out other skin conditions.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaSouth Korea is renowned for its advanced dermatological care. The following clinics offer a wide range of skin treatments and are equipped to provide consultations for conditions like Keratosis Pilaris.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
All-line Clinic | Body Contouring & Fat Dissolving Injections | Mapo-gu, Seoul, South Korea | ||
Plans Clinic | Lifting, Anti-aging, and Body Contouring | Gangnam-gu, Seoul, South Korea | ||
BLS Clinic | Lifting, Fillers, and Laser Treatments | Gangnam-gu, Seoul, South Korea | ||
Natural Beauty Clinic | Facial Contouring and Anti-aging Procedures | Gangnam-gu, Seoul, South Korea | ||
Clinic Trinity Raffaello | Comprehensive Dermatology & Aesthetic Treatments | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Oracle Dermatology Clinic | Advanced Laser Therapy & Skin Rejuvenation | Gangnam-gu, Seoul, South Korea | ||
Oracle Clinic Cheongdam | Dermatology, Plastic Surgery, and Anti-Aging | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Qbq Clinic | Aesthetic Dermatology & Facial Treatments | Gangnam-gu, Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaWhile not all of the following procedures are direct treatments for Keratosis Pilaris, they represent the advanced dermatological and aesthetic services available at leading South Korean clinics. Procedures that improve overall skin texture, such as laser treatments and skin boosters, may be discussed with a specialist as part of a comprehensive management plan. Costs are estimates and can vary based on the specific clinic and individual patient needs.
Treatment/Procedure Name | Duration | Hospitalization? | Avg Cost Range (USD) in S. Korea | Contact |
|---|---|---|---|---|
Laser Treatment (General) | 30-60 mins | Not Needed | $200 - $800 | |
Skin Booster (Rejuran Healer, Juvelook) | 30-45 mins | Not Needed | $300 - $700 | |
Titanium Lifting | 60-90 mins | Not Needed | $1,500 - $3,500 | |
Face Onda Lifting | 30-60 mins | Not Needed | $1,000 - $2,500 | |
Thermage FLX | 60-90 mins | Not Needed | $2,000 - $4,000 | |
Shurink / Heart Lifting / Inmode | 30-60 mins | Not Needed | $400 - $1,200 | |
Ulthera | 60-90 mins | Not Needed | $1,500 - $3,000 | |
Scar & Pore Laser (Secret Laser) | 45-75 mins | Not Needed | $500 - $1,500 | |
Pigmentation & Whitening (Hydrogen Toning) | 30-60 mins | Not Needed | $200 - $500 | |
Acne Peeling | 45-60 mins | Not Needed | $150 - $400 | |
Laser Hair Removal (Upper Arms) | 20-30 mins | Not Needed | $100 - $300 | |
Jaw Botox / Calf Botox | 15-30 mins | Not Needed | $150 - $500 | |
High Fat Dissolving Injection | 20-40 mins | Not Needed | $300 - $800 |
What Are Common Questions About Keratosis Pilaris?
what-are-common-questions-about-keratosis-pilarisThis section addresses some of the most common practical questions patients have about living with the condition.
1. Is Keratosis Pilaris hereditary?
1.-is-keratosis-pilaris-hereditaryYes, there is a strong genetic link. The condition often runs in families, and if a parent has it, their children have a higher probability of developing it as well. It is thought to be an autosomal dominant trait, meaning only one parent needs to carry the gene to pass it on.
2. Can diet affect my condition?
2.-can-diet-affect-my-conditionThe direct link between diet and Keratosis Pilaris is not well-established by rigorous scientific studies. However, some anecdotal evidence suggests that consuming an anti-inflammatory diet or avoiding certain food groups like gluten and dairy might improve symptoms for some individuals. A deficiency in vitamin A has also been loosely associated with the condition. Maintaining a balanced diet is beneficial for overall skin health.
3. Can Keratosis Pilaris be cured permanently?
3.-can-keratosis-pilaris-be-cured-permanentlyThere is no known permanent cure for Keratosis Pilaris. However, many people find that the condition naturally improves or disappears completely by the time they reach their 30s. For those who have it into adulthood, consistent treatment can manage symptoms effectively, but the bumps often return if the skincare regimen is stopped.
4. Is Keratosis Pilaris contagious?
4.-is-keratosis-pilaris-contagiousNo, Keratosis Pilaris is not contagious. You cannot catch it from or spread it to another person through physical contact. It is a condition related to individual genetics and hair follicle function.
5. Does shaving or waxing make Keratosis Pilaris worse?
5.-does-shaving-or-waxing-make-keratosis-pilaris-worseHair removal methods can sometimes irritate the skin and exacerbate the appearance of KP. Shaving can create sharp hair ends that may get trapped more easily, and waxing can cause inflammation. If you must remove hair, it's recommended to do so after a warm bath, shave in the direction of hair growth with a sharp blade, and moisturize immediately after.
6. Can I get Keratosis Pilaris on my face?
6.-can-i-get-keratosis-pilaris-on-my-faceYes, Keratosis Pilaris can appear on the face, especially the cheeks. This is more common in children and teenagers than in adults. On the face, it can sometimes be mistaken for acne, but it lacks the comedones (blackheads and whiteheads) associated with acne.
Your Path to Smoother Skin Starts Here!
your-path-to-smoother-skin-starts-hereUnderstanding Keratosis Pilaris is the first step toward managing it effectively. With the right skincare routine and access to advanced dermatological treatments, you can significantly improve your skin's texture and appearance. The journey to clearer, more comfortable skin begins with expert guidance. For a seamless, transparent process and end-to-end support contact CloudHospital, from your initial questions to post-treatment care, a dedicated Care Manager is available to assist you. And Start Your Confidential Inquiry to receive a personalized treatment plan from top specialists in South Korea.