The clinical information regarding Skin Lesions in this article has been rigorously verified against the latest guidelines from the American Academy of Dermatology (AAD) and primary research from databases like PubMed. This piece was reviewed for accuracy and patient-centric clarity and was last updated in October 2023.
Introduction
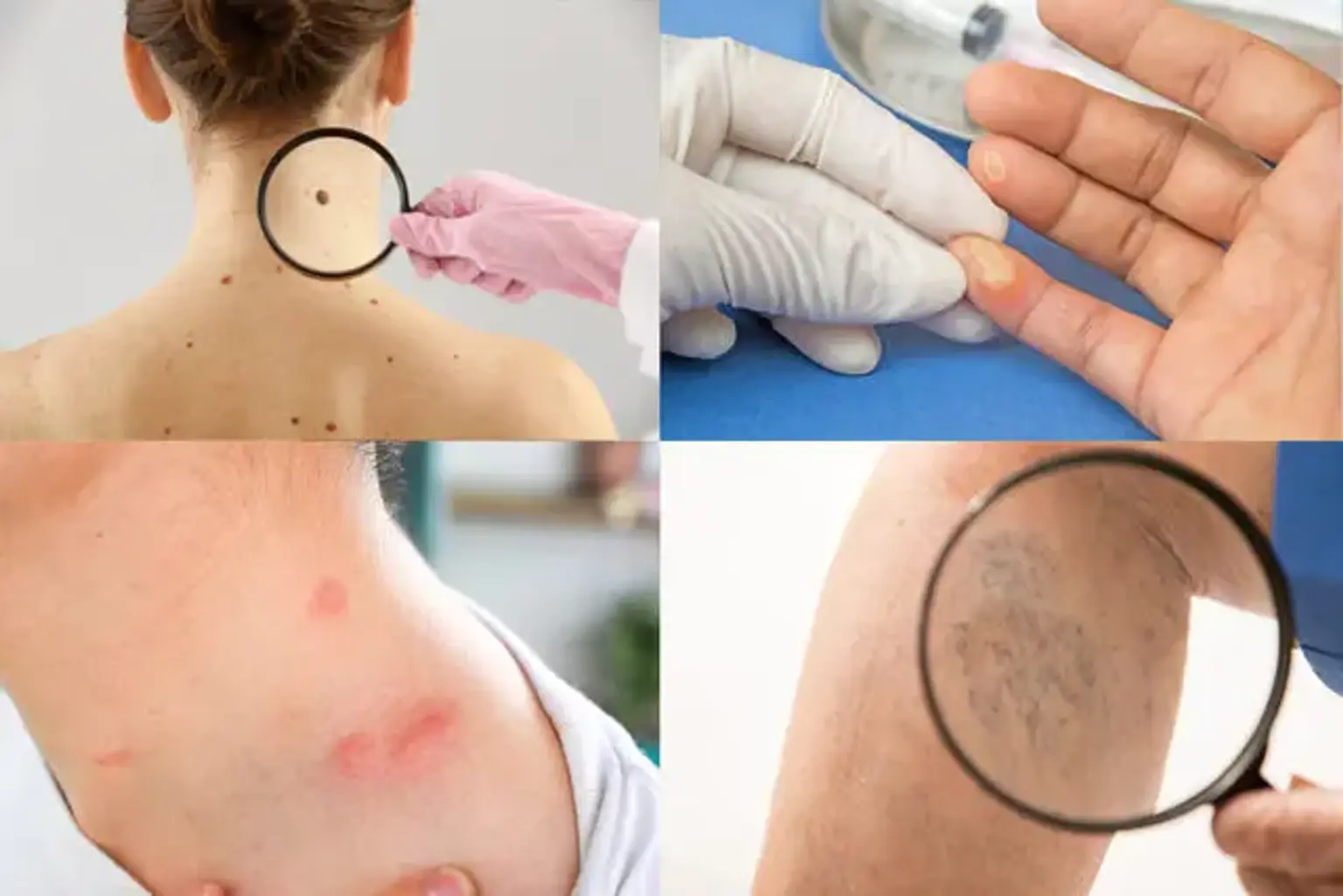
introductionNearly every adult has some form of skin lesion, from common freckles to moles and skin tags. While the vast majority of these are harmless, some can be indicators of underlying health issues, including skin cancer, which is the most common cancer in the United States. This guide provides a clinical explanation of skin lesions, clarifies the differences between benign non-cancerous and malignant cancerous types, and details the advanced diagnostic and treatment options available.
What Are the Different Types of Skin Lesions?
what-are-the-different-types-of-skin-lesionsA skin lesion is any area of skin that has an abnormal growth or appearance compared to the skin around it. They are broadly categorized into two groups primary lesions, which are variations in the skin that develop initially, and secondary lesions, which result from the irritation or evolution of a primary lesion. For clinical purposes, the most crucial distinction is between benign and malignant lesions.
Benign (Non-Cancerous) Skin Lesions
benign-(non-cancerous)-skin-lesionsThese lesions are extremely common and do not pose a threat to health, though they may be removed for cosmetic reasons or if they cause irritation.
Nevus (Mole): A common growth, typically small and brown or pink, caused by a cluster of pigment-producing cells melanocytes. Most adults have 10 to 40 moles.
Skin Tag (Acrochordon): A small, soft, flesh colored flap of skin that hangs off the skin on a connecting stalk. They are common in areas of friction like the neck, armpits, and groin.
Seborrheic Keratosis: A benign, often waxy or scaly growth that can be brown, black, or tan. They are very common in middle aged and older adults and are sometimes called barnacles of aging.
Dermatofibroma: A small, firm, reddish brown bump that often develops on the legs. They are harmless and often result from a minor injury like an insect bite.
Lipoma: A slow growing, fatty lump that is most often situated between your skin and the underlying muscle layer. A lipoma feels doughy and usually isn't tender.
Cherry Angioma: A small, bright red bump on the skin that is a collection of small blood vessels. They are common with age and are not a cause for concern.
Malignant and Pre-Malignant (Cancerous) Skin Lesions
malignant-and-pre-malignant-(cancerous)-skin-lesionsThese lesions require immediate medical evaluation and treatment. They are characterized by uncontrolled cell growth and have the potential to spread to other parts of the body.
Actinic Keratosis (AK): A pre-cancerous lesion that appears as a rough, scaly patch on sun exposed skin. If left untreated, AKs can progress to Squamous Cell Carcinoma.
Basal Cell Carcinoma (BCC): The most common type of skin cancer. It often appears as a slightly transparent bump on the skin, though it can take other forms. It grows slowly and rarely spreads.
Squamous Cell Carcinoma (SCC): The second most common type of skin cancer. It often looks like a firm red nodule, a scaly flat lesion, or a sore that heals and then re-opens.
Melanoma: The most serious type of skin cancer. It develops in the melanocytes and can appear as a new mole or a change in an existing mole. Early detection is critical for survival.
How Do You Know if a Skin Lesion is Dangerous?
how-do-you-know-if-a-skin-lesion-is-dangerousYou can identify a potentially dangerous lesion by performing regular self exams and using the ABCDE method, a guideline established by dermatologists to spot the warning signs of melanoma.
A - Asymmetry: One half of the mole or spot does not match the other half.
B - Border: The edges are irregular, ragged, notched, or blurred.
C - Color: The color is not the same all over and may include shades of brown or black, or sometimes patches of pink, red, white, or blue.
D - Diameter: The spot is larger than 6 millimeters across about the size of a pencil eraser, although melanomas can sometimes be smaller than this.
E - Evolving: The mole is changing in size, shape, or color.
If you notice any of these signs, or a new lesion that is bleeding, itching, or scabbing, it is essential to see a dermatologist for a professional evaluation, which may include a skin biopsy.
"I'd had this small, dark spot on my shoulder for years, but one morning it just seemed different. The edge looked fuzzy. That was the moment I knew I couldn't ignore it anymore." – an anonymous patient, USA.
What Causes the Sudden Appearance of Skin Lesions?
what-causes-the-sudden-appearance-of-skin-lesionsThe sudden appearance of skin lesions can be attributed to a variety of factors, ranging from harmless to serious. Sun exposure is the primary cause of many new lesions, particularly pre-cancerous and cancerous ones like actinic keratosis and melanoma. Hormonal changes, such as those during pregnancy, can lead to an increase in moles and skin tags. Other causes include viral infections (e.g., warts), allergic reactions (e.g., hives), friction, and the natural aging process, which contributes to growths like seborrheic keratoses.
Can Benign Skin Lesions Be Removed for Cosmetic Reasons?
can-benign-skin-lesions-be-removed-for-cosmetic-reasonsYes, the removal of benign skin lesions for purely cosmetic reasons is a very common and safe practice in dermatology. Many individuals choose to remove moles, skin tags, or seborrheic keratoses that are not medically concerning but are located in prominent areas like the face or neck, or in areas where they are subject to friction from clothing or shaving. Advanced dermatological clinics, particularly in South Korea, specialize in removal techniques that prioritize both efficacy and excellent cosmetic outcomes, minimizing scarring and downtime.
What Are the Options for Skin Lesion Removal in Korea?
what-are-the-options-for-skin-lesion-removal-in-koreaDermatology clinics in South Korea are renowned for using advanced technology to remove lesions with high precision and minimal aesthetic impact. The choice of treatment depends on the lesion's type, size, and location.
Laser Treatment: This is a preferred method for many benign lesions like moles, seborrheic keratoses, and skin tags. Lasers like CO2 or Erbium:YAG precisely vaporize the lesion layer by layer, minimizing damage to surrounding tissue and reducing the risk of scarring.
Surgical Excision: This involves cutting the lesion out with a scalpel and is the standard for suspected malignant lesions to ensure complete removal for biopsy. It is also used for large benign moles or cysts.
Cryotherapy: This technique uses liquid nitrogen to freeze and destroy the lesion. It is commonly used for warts, skin tags, and actinic keratoses.
Electrodessication and Curettage: This involves scraping off the lesion and then using an electric current to destroy any remaining cells. It is effective for certain types of BCC and SCC.
Post-procedure care may involve treatments like Hydrogen Toning or Platinum Photothermal Therapy to reduce inflammation and hyperpigmentation, ensuring a better cosmetic result.
Recommended Clinics with Relevant Expertise in South Korea
recommended-clinics-with-relevant-expertise-in-south-koreaBelow is a table of leading dermatology clinics in South Korea known for advanced skin treatments, including cosmetic lesion removal and comprehensive skin health management.
Website | Clinic Name | Best Known For | Address | Contact |
|---|---|---|---|---|
All-line Clinic | Advanced Lifting & Body Contouring | Mapo-gu, Seoul, South Korea | ||
Plans Clinic | High-Dose Fat Dissolving Injections | Gangnam-gu, Seoul, South Korea | ||
BLS Clinic | Comprehensive Aesthetic Dermatology | Gangnam-gu, Seoul, South Korea | ||
Natural Beauty Clinic | Wide Range of Aesthetic Procedures | Gangnam-gu, Seoul, South Korea | ||
Clinic Trinity Raffaello | Anti-Aging & Skin Rejuvenation | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Oracle Dermatology | Laser Treatments & Injectables | Gangnam-gu, Seoul, South Korea | ||
Cheongdam Qbq Clinic | Premium Aesthetic Treatments | Gangnam-gu, Seoul, South Korea | ||
Oracle Clinic Cheongdam | Personalized Anti-Aging Programs | Gangnam-gu, Seoul, South Korea |
Recommended Treatment/Procedure Names with Average Costs in South Korea
recommended-treatmentprocedure-names-with-average-costs-in-south-koreaThe following table outlines advanced dermatological procedures available in South Korea, some of which may be used for post-lesion care or general skin rejuvenation to improve texture and tone.
Treatment/Procedure Name | Duration | Hospitalization? | Avg. Cost Range (USD) in S. Korea | Contact |
|---|---|---|---|---|
Laser Treatment (for Lesions) | 15 - 30 minutes | Outpatient | $100 - $500 per session | |
Rejuran Healer | 20-30 mins | Not Needed | $350 - $600 | |
Vitaran | 20-30 mins | Not Needed | $300 - $550 | |
Juvelook | 30-45 mins | Not Needed | $450 - $700 | |
Lizne | 20-30 mins | Not Needed | $300 - $500 | |
Skin Botox – Full Face | 20-30 mins | Not Needed | $300 - $600 | |
High Fat Dissolving Injection | 20-30 mins | Not Needed | $300 - $800 | |
Triple Body Injection | 30-45 mins | Not Needed | $500 - $1200 | |
Titanium Lifting | 60-90 mins | Not Needed | $1500 - $3500 | |
Face Onda Lifting | 30-45 mins | Not Needed | $800 - $2000 | |
Body Onda Lifting | 45-60 mins | Not Needed | $1000 - $2500 | |
Combination Skin Boosters | 45-60 mins | Not Needed | $600 - $1500 | |
Jaw Botox | 10-15 mins | Not Needed | $100 - $300 | |
Calf Botox | 15-20 mins | Not Needed | $400 - $800 | |
Abdomen Fat Dissolving Injection | 20-30 mins | Not Needed | $400 - $1000 | |
Arm Fat Dissolving Injection | 20-30 mins | Not Needed | $300 - $700 | |
High Lower Body Fat Dissolving Injection | 30-40 mins | Not Needed | $500 - $1200 | |
Face Fat Dissolving Injection | 15-20 mins | Not Needed | $200 - $500 | |
Mirajet Needle-Free Injector | 30-45 mins | Not Needed | $500 - $900 | |
Titanium Fat Dissolving Treatment | 60-90 mins | Not Needed | $1800 - $4000 | |
Laser Hair Removal | 15-60 mins | Not Needed | $50 - $400 | |
Thermage FLX | 60-90 mins | Not Needed | $2000 - $4000 | |
Shurink | 30-45 mins | Not Needed | $400 - $900 |
Your Key Questions About Skin Lesions Answered
your-key-questions-about-skin-lesions-answered1. What is the recovery time for laser lesion removal?
1.-what-is-the-recovery-time-for-laser-lesion-removalRecovery time for laser lesion removal is typically short, ranging from 5 to 10 days. The treated area will form a small scab or crust that should be kept clean and moist with an ointment; it will fall off on its own, revealing new, pink skin underneath which will fade to your normal skin tone over several weeks.
2. Are skin lesions always a sign of cancer?
2.-are-skin-lesions-always-a-sign-of-cancerNo, the vast majority of skin lesions are not cancerous. Benign lesions like moles, skin tags, and seborrheic keratoses are far more common than malignant ones. However, any new or changing lesion should be evaluated by a dermatologist to rule out skin cancer.
3. What is a skin biopsy and is it painful?
3.-what-is-a-skin-biopsy-and-is-it-painfulA skin biopsy is a procedure where a small sample of skin is removed for examination under a microscope. It is the definitive way to diagnose a suspicious lesion. The procedure is performed under local anesthesia, so you will only feel a small needle prick initially, but you will not feel pain during the biopsy itself.
4. Can a removed skin lesion grow back?
4.-can-a-removed-skin-lesion-grow-backA skin lesion can sometimes grow back if any of its cells were left behind during removal. Benign lesions like moles may partially recur, and malignant lesions have a higher risk of recurrence if not completely excised. This is why a proper diagnosis and an appropriate removal technique are crucial.
5. How much does skin lesion removal cost in South Korea?
5.-how-much-does-skin-lesion-removal-cost-in-south-koreaThe cost of skin lesion removal in South Korea varies widely depending on the type, size, and number of lesions, as well as the method used. A simple laser removal of a small benign mole might start around $100, while a surgical excision of a larger or more complex lesion could be several hundred dollars or more.
6. What is post-inflammatory hyperpigmentation after lesion removal?
6.-what-is-post-inflammatory-hyperpigmentation-after-lesion-removalPost-inflammatory hyperpigmentation (PIH) is the temporary darkening of the skin at the site of a healed injury, including a lesion removal site. It is more common in individuals with darker skin tones. Using sun protection diligently after the procedure is the most effective way to prevent or minimize PIH.
Gain Clarity and Confidence: Your Personalized Skin Assessment Awaits Now!
gain-clarity-and-confidence:-your-personalized-skin-assessment-awaitsNavigating the concerns of a new or changing skin lesion requires expert guidance. Do not wait for uncertainty to cause you stress. The clinics and medical teams in South Korea offer world-class diagnostic capabilities and cosmetically elegant treatment solutions. By inquiring today, you can access a seamless, transparent process guided by a dedicated Care Manager who will support you from your initial question to your post-procedure care. Start Your Confidential Inquiry with CloudHospital today and receive a free, personalized assessment from a leading dermatologist.