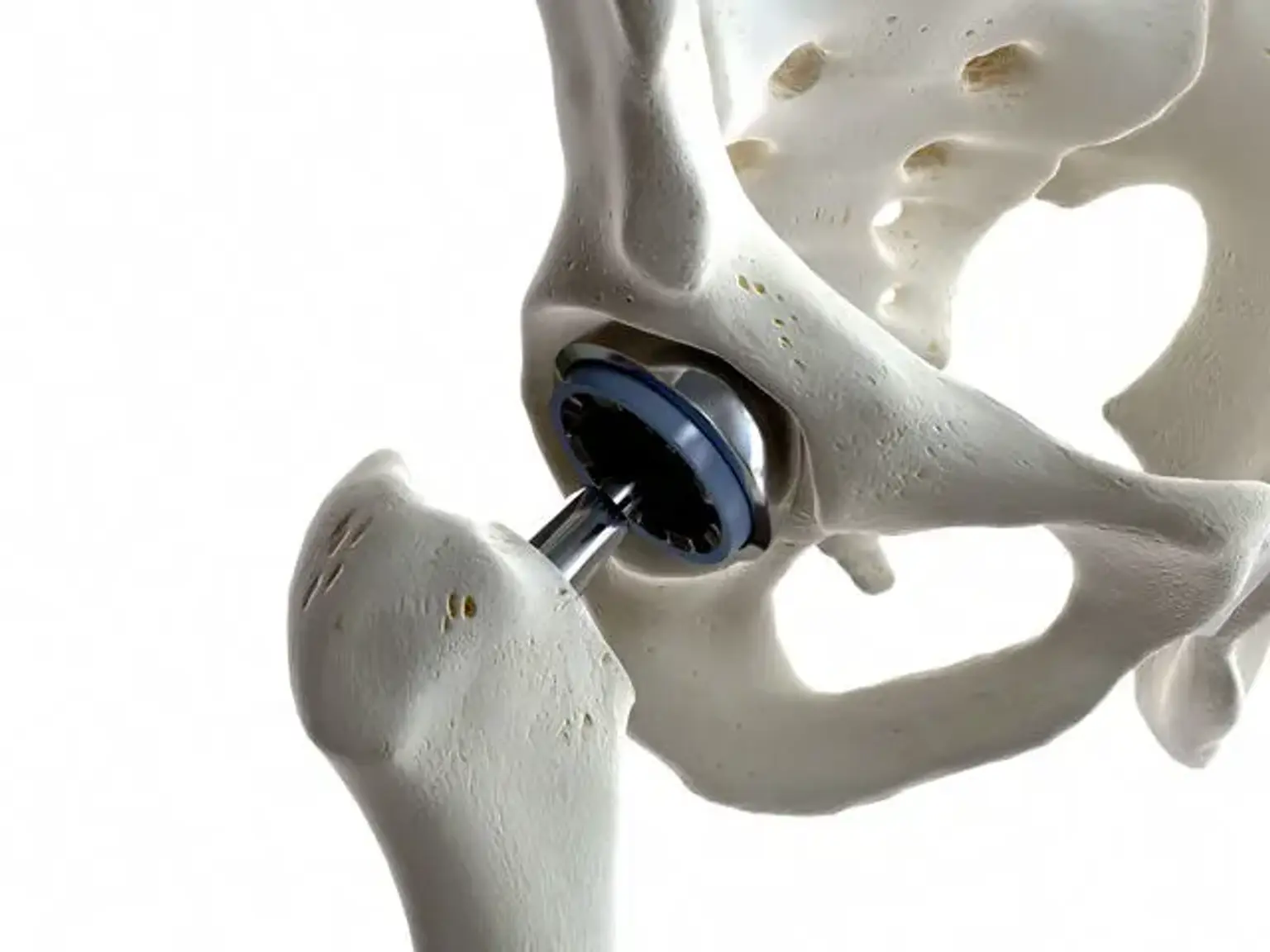
Introduction
3D personalized joint arthroplasty is a groundbreaking advancement in joint replacement surgery, using 3D printing technology to create custom implants tailored to an individual’s unique anatomy. Unlike traditional implants, which are mass-produced to fit general shapes and sizes, 3D-printed implants are specifically designed for each patient based on detailed imaging and data.
In joint arthroplasty, surgeons replace damaged or worn-out joints, typically in the knee, hip, or shoulder, to restore function and alleviate pain. The introduction of 3D printing allows for higher precision in designing these replacements, ultimately improving the outcome of the surgery and the patient’s recovery.
The Evolution of Joint Replacement Surgeries
Joint replacement surgery has come a long way since its inception. Early surgeries involved crude, metal implants that were designed to fit a variety of patients. However, this standardization often led to complications, including poor fit, discomfort, and the need for revisions. Over time, joint replacements evolved with more advanced materials and techniques, but they still lacked the level of personalization needed for optimal results.
The introduction of 3D technology into joint arthroplasty marked a significant turning point. Surgeons can now use 3D models of a patient’s bones and joints, creating implants that are a perfect match. This tailored approach is already showing promising results in terms of faster recovery and reduced risk of complications. By combining robotics with 3D printing, surgeons can perform more precise surgeries, enhancing the overall effectiveness of joint replacement procedures.
Understanding 3D Personalized Joint Arthroplasty
3D personalized joint arthroplasty involves using patient-specific data—typically gathered from CT scans or MRI imaging—to create a detailed 3D model of the patient’s joint. This model is then used to design a customized prosthesis that perfectly fits the patient’s anatomy.
Once the design is finalized, a 3D printer creates the implant using specialized materials such as titanium or cobalt-chromium. These materials are durable, biocompatible, and suitable for long-term use in the human body.
Surgeons use this 3D model to plan the procedure more accurately, reducing the chances of errors during surgery. By focusing on precision, 3D personalized joint arthroplasty helps to minimize surgical risks, ensuring that the replacement joint functions well and lasts longer.
Benefits of 3D Personalized Joint Arthroplasty
One of the key advantages of 3D personalized joint arthroplasty is the precision and accuracy it offers. Traditional implants may require adjustments during surgery, but with personalized 3D implants, the fit is near-perfect from the start. This can significantly reduce the risk of complications, such as infection or implant failure.
Additionally, the customized implants lead to improved surgical outcomes. Patients experience better functionality in their joint, more natural movement, and a higher degree of comfort. The precision of the implant means it functions as intended for a longer period of time, leading to fewer revisions down the line.
The patient-centered approach of 3D printing also speeds up recovery. As the joint is better aligned with the body’s natural structure, the healing process is smoother, with less pain and quicker rehabilitation. Patients typically have a better range of motion, allowing them to resume their daily activities sooner.
Types of Joint Replacements Benefiting from 3D Personalization
While 3D personalized joint arthroplasty has shown the most promise in knee and hip replacements, its benefits are extending to other joints as well, such as the shoulder and elbow.
Knee Arthroplasty
Knee replacements have been one of the earliest beneficiaries of 3D printing. Custom knee implants can be designed to perfectly match the patient’s femur, tibia, and patella, optimizing alignment and reducing wear and tear. With traditional implants, misalignment is a common issue that can lead to discomfort or implant failure. 3D printing eliminates these concerns, providing a snug fit that enhances both mobility and durability.
Hip Arthroplasty
In hip replacements, 3D printing allows for more precise fitment, particularly in complex cases such as dysplasia or deformities. The custom implants ensure better joint function and greater comfort, helping to prevent complications like dislocation. With personalized fit, the hip joint can better withstand the forces of daily activities.
Shoulder and Elbow Joint Replacements
Though less common, 3D-printed implants for shoulder and elbow joints are becoming more feasible. The ability to design prosthetics tailored to a patient’s unique anatomy is especially useful in complex joint conditions, like arthritis or trauma, where traditional implants may not provide optimal results. These personalized prostheses can restore full function and relieve pain more effectively than standard options.
3D-Printed Implants: How They Are Made
The creation of 3D-printed implants begins with gathering precise medical images of the patient’s joint, typically using CT scans or MRI. These images provide detailed insights into the patient's anatomy, allowing for an accurate digital representation. Using specialized software, the surgeon or medical technician creates a 3D model of the joint, factoring in the patient’s unique bone structure and alignment.
Once the 3D model is ready, it is sent to a 3D printer, which builds the implant layer by layer from materials like titanium or cobalt-chromium. These metals are selected for their strength, durability, and biocompatibility, ensuring the implant integrates well with the body over time. The printing process allows for intricate designs, such as porous surfaces that mimic natural bone structure, which enhances the implant's ability to bond with the bone.
The precision of 3D printing also means the prosthesis is custom-made to match the patient’s joint exactly, reducing the need for intraoperative adjustments. This is a key factor in improving the overall success rate of the surgery.
Risks and Challenges of 3D Personalized Joint Arthroplasty
Despite the numerous advantages, 3D personalized joint arthroplasty comes with its own set of challenges and risks that need to be carefully considered.
Material Limitations
While the materials used in 3D-printed implants are durable and biocompatible, they are not without limitations. For example, the process of 3D printing can sometimes create weak points in the implant, particularly if the printer’s settings are incorrect. Additionally, some materials may not be as long-lasting as traditional metals used in implants, though ongoing research is working to address these concerns.
Surgical Complexity
While 3D personalization allows for precise implants, the process itself can be more complex than traditional joint replacements. The need for detailed preoperative planning and the use of advanced technology requires skilled surgeons who are well-versed in these methods. Inexperienced practitioners could face challenges in managing the more sophisticated nature of 3D joint replacement surgeries.
Cost Implications
One of the biggest barriers to widespread adoption of 3D personalized joint arthroplasty is the cost. The production of customized 3D implants, along with the use of advanced robotics, can make the procedure more expensive than conventional joint replacements. However, many argue that the long-term benefits, such as reduced revision surgeries and faster recovery, can justify the higher upfront cost.
Regulatory and Safety Concerns
As with any new technology, regulatory bodies must carefully assess the safety of 3D-printed implants. While the technology is promising, there is a need for continued research to confirm the long-term success of these personalized replacements. Surgeons and manufacturers must ensure that these implants meet all regulatory standards to guarantee patient safety.
Role of Robotics in 3D Personalized Joint Arthroplasty
The combination of 3D printing and robotics represents a significant leap forward in joint replacement surgeries. Robotic-assisted surgery is used to guide surgeons with high precision, improving the accuracy of implant placement and minimizing human error.
Robotic-Assisted Surgery
During robotic-assisted surgery, the surgeon uses a robotic arm, controlled by a computer, to help with implant positioning. The 3D-printed implant is positioned exactly according to the pre-surgical plan, reducing the chances of alignment errors. The robot’s high degree of precision ensures the best possible outcome with minimal disruption to surrounding tissues.
Benefits of Robotic Surgery
The major benefits of robotic-assisted surgery include less invasive incisions, less blood loss, and faster recovery times. Robotic arms can also minimize the amount of bone that needs to be removed, preserving as much of the patient’s natural joint as possible. This leads to quicker healing and less post-surgical discomfort.
How Robotics Complements 3D Printing
Robotics and 3D printing are highly complementary. While 3D printing allows for the creation of patient-specific implants, robotics ensures these implants are placed with the utmost accuracy. Together, these technologies can improve surgical outcomes, reduce complications, and ultimately enhance the patient’s quality of life.
Global Popularity and Availability
The adoption of 3D personalized joint arthroplasty is growing worldwide, with leading countries like the U.S., Germany, and Japan at the forefront of this technology. These nations have made significant investments in research and infrastructure, making advanced joint replacement procedures more accessible.
Costs in Different Regions
The price of 3D joint arthroplasty can vary based on location and healthcare systems. In some countries, the procedure is considered a premium option, making it more expensive than traditional methods. However, in regions where medical technology is more advanced and readily available, it may be more affordable, especially when factoring in the long-term benefits, such as fewer revisions.
Access to Technology
Despite its global growth, 3D personalized joint arthroplasty remains less accessible in lower-income regions. This disparity is primarily due to the cost of the technology and specialized training required for surgeons. As the technology becomes more widespread, it’s expected that access will improve.
The Future of 3D Personalized Joint Arthroplasty
The future of 3D personalized joint arthroplasty looks promising, with ongoing advancements that could revolutionize joint replacement surgery.
Technological Advancements
New materials and printing techniques are constantly improving the quality and durability of 3D-printed implants. Advances in biocompatible materials may lead to implants that better mimic natural bone, improving the body’s integration with the prosthesis.
Research and Clinical Trials
Clinical trials are key to refining the procedures and proving the long-term benefits of 3D joint replacements. As more data is collected, the medical community will have a clearer understanding of the technology’s efficacy and safety. This research will also help fine-tune preoperative planning and surgical techniques.
Potential for Other Medical Applications
The use of 3D printing in joint replacement is just the beginning. In the future, this technology could be applied to other medical fields, such as dental implants, cranial implants, and even soft tissue repair. The possibilities are vast as 3D printing continues to develop.
How 3D Personalized Joint Arthroplasty Improves Quality of Life
One of the most significant benefits of 3D personalized joint arthroplasty is its impact on quality of life.
Enhanced Mobility and Comfort
Because the implant is custom-made, it fits better than standard prosthetics, leading to improved joint mobility and less discomfort. Patients report better freedom of movement, allowing them to return to activities they may have previously struggled with due to joint pain.
Long-Term Benefits
With a better fit and reduced wear, 3D-printed implants can last longer than traditional replacements. Fewer revisions are needed, which saves patients from the stress and cost of future surgeries.
Improved Self-Esteem and Mental Well-Being
The positive physical changes after surgery can significantly boost a patient’s confidence and self-esteem. Being able to move freely without pain improves not only physical health but also mental well-being, enhancing the patient’s overall quality of life.
Patient Experience: What to Expect Before, During, and After Surgery
Pre-Surgical Assessment
Before surgery, patients will undergo detailed imaging (such as CT scans or MRIs) to create a personalized 3D model of their joint. This allows the surgeon to plan the procedure in great detail, minimizing potential complications. Patients will also discuss their medical history and any concerns with their surgeon.
Surgical Process
During the surgery, the 3D-printed implant is placed with precision, guided by pre-surgical planning. The use of robotic assistance ensures that the implant is positioned accurately, reducing risks and improving outcomes. The procedure itself is minimally invasive, which can lead to quicker recovery times.
Recovery Timeline
Recovery from 3D personalized joint arthroplasty is often faster than traditional joint replacements, thanks to the precise fit of the implant. Patients typically experience less pain and are able to resume daily activities sooner. Physical therapy plays an essential role in regaining strength and mobility.
Pain Management and Rehabilitation
Pain management is a key component of the recovery process, with many patients requiring less post-surgical pain medication due to the precision of the implant. Rehabilitation will be tailored to the patient’s specific needs, focusing on strength-building and improving range of motion.
Patient Considerations: Who is a Good Candidate?
3D personalized joint arthroplasty is not for every patient. It’s typically recommended for individuals who meet certain criteria, ensuring the best possible outcomes.
Ideal Candidates
Age: While younger patients can benefit from longer-lasting results, the procedure is generally suited for adults over the age of 50 who have significant joint wear due to conditions like osteoarthritis or rheumatoid arthritis.
Bone Health: Candidates need to have sufficient bone density and structure for the implant to integrate well.
Joint Deformities or Complex Cases: People with complex joint deformities, anatomical variations, or severe joint damage may benefit from the precision of 3D printing.
Exclusion Criteria
Patients with infections, uncontrolled chronic conditions, or poor general health may not be good candidates for 3D joint arthroplasty. Surgeons will assess individual health before making a recommendation.
Frequently Asked Questions (FAQs)
1. Is 3D personalized joint arthroplasty more expensive than traditional joint replacement?
Yes, the procedure tends to be more expensive due to the custom implants and advanced technology used, but it can save on long-term costs by reducing the need for revisions and improving recovery time.
2. How long do 3D-printed implants last?
3D-printed implants are made from durable materials like titanium and cobalt-chromium, which are known for their longevity. They can last 15-20 years or more, depending on the patient’s activity level and health.
3. Is the recovery process faster with 3D personalized implants?
Yes, many patients experience a quicker recovery with less pain and swelling because the implant fits better and requires less invasive surgery.
4. Can I return to sports after surgery?
Most patients can return to low-impact activities after full recovery, but high-impact sports may require special consideration depending on the type of joint and the patient’s activity level.
Risks and Limitations of 3D Personalized Joint Arthroplasty
While 3D personalized joint arthroplasty offers many benefits, there are some potential risks and limitations to consider.
Infection and Complications
As with any surgery, there’s a risk of infection or complications related to anesthesia. Proper preoperative care and hygiene can help minimize these risks.
Implant Failure
Although rare, there is a possibility that the 3D-printed implant could fail prematurely. This could occur due to issues with the material or the implant's integration with the bone. However, because the implants are designed to fit more precisely, the chances of failure are significantly reduced compared to traditional prosthetics.
Limited Availability and High Costs
The main limitation is that 3D joint arthroplasty is not yet universally available. The high cost of personalized implants and specialized equipment can make the procedure out of reach for some patients, especially in regions with less access to advanced medical technologies.
Conclusion
3D personalized joint arthroplasty represents a major leap forward in joint replacement technology. By combining advanced 3D printing with precise surgical planning, it offers patients a more tailored, effective, and longer-lasting solution to joint pain and mobility issues.
This innovative procedure enhances the surgical experience, reduces recovery time, and improves the overall quality of life for many patients. Though the technology remains costly and not universally available, its growing adoption and research suggest a promising future where joint replacement is more accessible and beneficial than ever before.
As the technology continues to advance, it holds the potential to change the landscape of joint replacement, offering hope to patients worldwide who seek relief from debilitating joint conditions. The future is bright for 3D personalized joint arthroplasty, offering more options, better outcomes, and greater quality of life for those in need of joint replacement surgery.