Introduction
Bone abnormalities are conditions that affect the normal structure or function of bones. These issues can range from minor deformities to serious disorders that impact daily activities. Early diagnosis and treatment are crucial for managing these conditions and preventing further complications.
Globally, millions of people suffer from bone abnormalities, which can be congenital (present at birth) or acquired due to injury, disease, or lifestyle factors. Conditions like osteoporosis, scoliosis, and osteogenesis imperfecta (brittle bone disease) are among the most common, affecting individuals of all ages. This article will explore the various diagnostic techniques and treatment options available, offering insights into how these conditions can be effectively managed.
Understanding Bone Abnormalities
What Are Bone Abnormalities?
Bone abnormalities refer to any condition that alters the normal structure or function of bones. These issues can be developmental, genetic, or acquired. Bone deformities may lead to pain, decreased mobility, and other serious health issues if not treated.
There are various types of bone abnormalities, including:
Congenital Deformities: Conditions present at birth, like clubfoot or bone growth disorders.
Degenerative Diseases: Conditions that develop over time, such as osteoporosis or arthritis, leading to bone weakening and fractures.
Traumatic Injuries: Resulting from accidents or falls, leading to fractures or dislocations.
Common Types of Bone Disorders
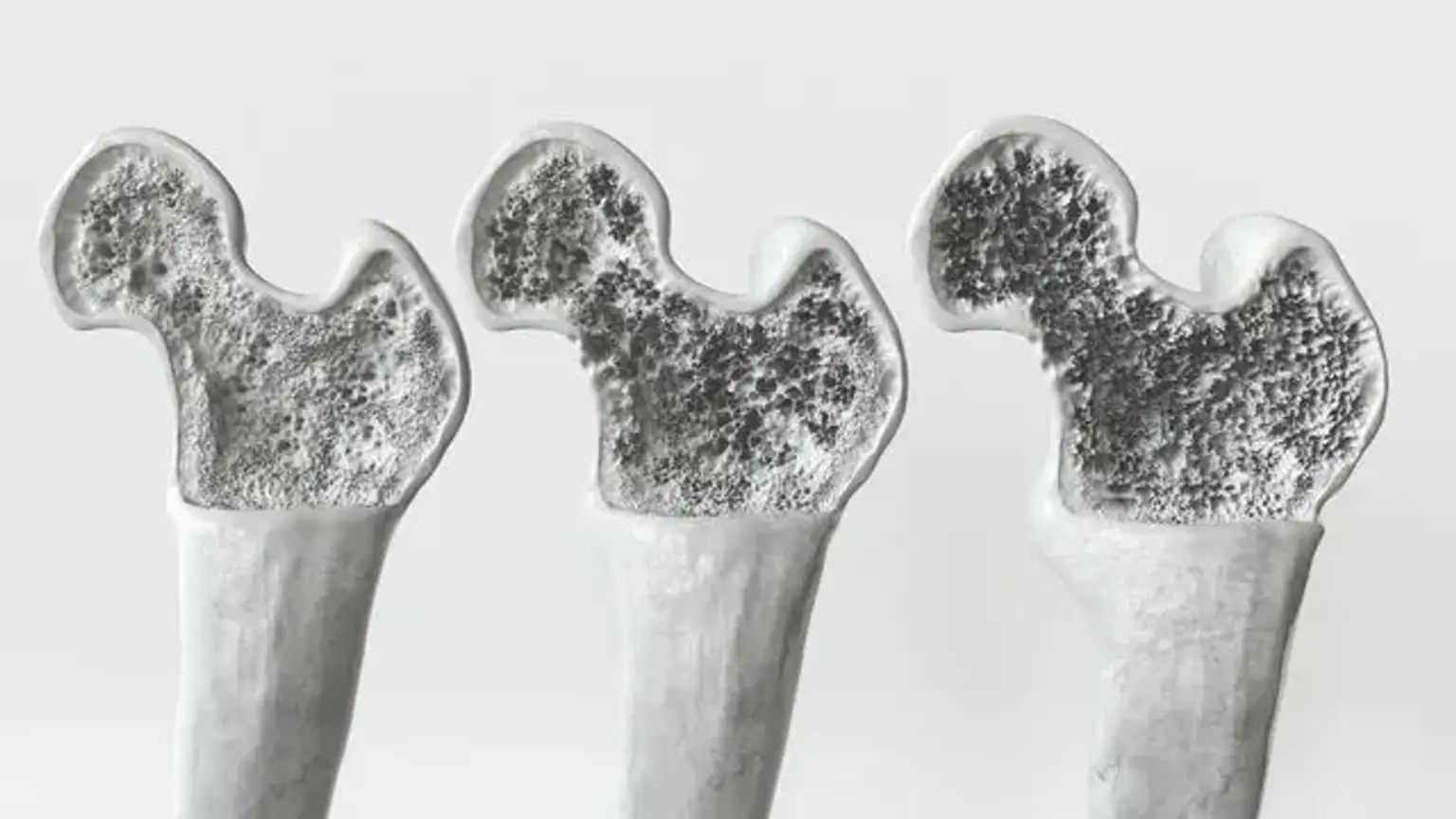
Osteoporosis: A condition that weakens bones, making them fragile and more likely to break. It mainly affects older adults, especially women after menopause.
Osteogenesis Imperfecta (OI): A genetic disorder where bones break easily, sometimes even without an obvious cause.
Scoliosis: A sideways curvature of the spine that often begins in childhood.
Paget's Disease: A chronic disorder that causes bones to grow abnormally, often resulting in deformities and pain.
Diagnostic Tools for Bone Abnormalities
Imaging Techniques in Bone Diagnosis
To diagnose bone abnormalities, medical professionals rely on various imaging techniques that offer clear and detailed views of the bones and surrounding tissues. The most common diagnostic tools include:
X-rays: These are the most widely used method for diagnosing fractures, deformities, and conditions like arthritis and osteoporosis. X-rays provide a basic view of bone structure and density.
CT Scans: For more detailed images of bone abnormalities, CT scans are often used. They provide 3D images and are especially useful in detecting bone fractures or tumors.
MRI Scans: Magnetic Resonance Imaging (MRI) is ideal for examining soft tissues and bone marrow. It helps in diagnosing conditions like bone infections or tumors.
Bone Marrow Biopsy and Blood Tests
For certain bone diseases, such as leukemia or bone marrow disorders, doctors may recommend a bone marrow biopsy, where a small sample of bone marrow is extracted and examined for abnormal cells.
Blood tests can also help in diagnosing bone abnormalities, especially metabolic bone diseases like osteoporosis, where tests check for calcium levels and other bone-related biomarkers.
Factors Contributing to Bone Abnormalities
Genetics and Family History
Genetics play a significant role in many bone abnormalities. Some conditions are inherited, meaning they are passed down through generations. For instance:
Osteogenesis Imperfecta (OI) is caused by genetic mutations, leading to fragile bones.
Paget’s disease can run in families, increasing the likelihood of developing the disorder.
A family history of bone diseases can often alert healthcare providers to a potential risk, allowing for earlier screenings and preventive measures.
Environmental Factors
Environmental factors, including lifestyle choices and nutrition, can contribute to bone health. Key factors include:
Nutrition: A diet low in calcium or vitamin D can lead to weakened bones and conditions like osteoporosis.
Physical Activity: Lack of exercise, especially weight-bearing activities like walking or running, can result in bone density loss.
Smoking and Alcohol Use: Both smoking and excessive alcohol consumption can increase the risk of bone loss and fractures.
Treatment Options for Bone Abnormalities
Non-Surgical Treatment Methods
Not all bone abnormalities require surgery. Many conditions can be managed through non-invasive treatments, especially if diagnosed early.
Medications: For conditions like osteoporosis or Paget’s disease, medications such as bisphosphonates and calcium supplements can help strengthen bones and slow further deterioration. Pain management is also essential for patients with bone deformities.
Physical Therapy: Therapy helps improve mobility, strengthen muscles, and reduce pain. Specific exercises can be prescribed to enhance joint flexibility and bone strength, especially after fractures or surgeries.
Braces and Supports: For certain bone deformities, like scoliosis or fractures, braces can provide support, improve posture, and reduce pain while preventing further deformity.
Surgical Treatments
While non-invasive treatments are effective for some conditions, others may require surgery. Surgical intervention is often needed to correct severe deformities or fractures that can’t heal with conservative methods.
Bone Grafting: In cases of severe bone loss, such as with bone tumors or fractures that do not heal, a bone graft may be used. This involves transplanting healthy bone tissue to help stimulate the healing process.
Osteotomy: This procedure involves cutting and repositioning bones to correct deformities. It is commonly used in patients with severe arthritis or bone misalignment.
Spinal Fusion: For patients with scoliosis or other spinal abnormalities, spinal fusion surgery can stabilize the spine and correct curvature.
Bone Abnormality Treatments in Children
Congenital Bone Deformities in Children
Children born with congenital bone abnormalities often require early intervention to manage their conditions and improve their quality of life. Early diagnosis is critical for minimizing long-term effects. Common treatments include:
Bracing and Physical Therapy: For deformities like clubfoot, bracing and physical therapy can guide the bones into the correct position as the child grows.
Surgical Corrections: In severe cases, surgery may be required to correct bone deformities such as hip dysplasia or spinal curvatures.
The goal of treatment for congenital deformities is to improve mobility and functionality, preventing complications as the child grows.
Growth Disorders and Bone Development
Bone growth disorders can affect a child’s normal bone development, leading to abnormal bone growth and possible deformities. Common conditions include rickets (due to vitamin D deficiency) and metabolic bone diseases. Treatment typically includes:
Nutritional Interventions: Supplementing with vitamin D and calcium can correct bone growth disorders caused by deficiencies.
Growth Hormone Therapy: In certain cases, if the disorder is caused by growth hormone deficiency, hormone therapy may help stimulate normal bone growth.
Early diagnosis and treatment of growth disorders are essential for ensuring that children develop healthy bones and joints.
Advanced Treatments and Therapies
Gene Therapy and Stem Cells
Advances in medical science have opened new possibilities for treating bone abnormalities. Gene therapy aims to correct genetic mutations that cause disorders like osteogenesis imperfecta, while stem cell therapy offers the potential to regenerate damaged bones. These innovative treatments are still in the experimental stages but have shown promise in clinical trials.
Gene Therapy: Researchers are exploring ways to introduce healthy genes into bone tissue, potentially reversing genetic bone disorders.
Stem Cell Therapy: Stem cells have the potential to repair bone damage and stimulate growth, particularly useful for conditions like bone fractures that don't heal or conditions causing bone loss.
These therapies may provide groundbreaking treatment options in the future, potentially reducing the need for surgery in some cases.
Bone Regeneration Techniques
New technologies in bone regeneration are helping to treat severe bone damage and deformities. Some of the most promising treatments include:
Bone Grafts: Using grafts from a donor or synthetic materials to replace damaged bone.
3D-Printed Bones: In certain cases, 3D printing technology is being used to create custom bone implants for patients with severe deformities or bone loss.
These advancements allow for more precise treatments, improving recovery times and reducing complications associated with traditional bone surgeries.
Ongoing Research and Advancements
Current Trends in Bone Abnormality Research
The field of bone health is continuously evolving, with research focused on improving diagnostic techniques and treatment options for bone abnormalities. Some exciting areas of research include:
Bone Density Drugs: Researchers are developing medications that target the specific biological processes that cause bone loss, such as osteoporosis.
Growth Factor Therapies: Studies are investigating the use of growth factors that stimulate bone regeneration, offering hope for patients with severe bone loss.
Personalized Medicine: With advancements in genetics, personalized treatment plans are becoming more common, allowing doctors to tailor therapies based on a patient’s genetic makeup.
New Diagnostic Methods
New diagnostic technologies are improving how doctors detect bone abnormalities at earlier stages, making treatment more effective. For instance, biomarker testing is being explored to diagnose osteoporosis and other bone diseases before significant damage occurs.
These breakthroughs provide hope for better, less invasive treatments and a more accurate understanding of bone health.
Prevention and Bone Health Maintenance
Maintaining Healthy Bones
Preventing bone abnormalities starts with adopting healthy lifestyle habits. Here are some key tips to maintain strong bones:
Regular Exercise: Weight-bearing exercises like walking, running, and strength training help build bone density.
Balanced Diet: Ensure your diet includes calcium, vitamin D, and magnesium to support bone health.
Avoid Smoking and Excessive Alcohol: Both can weaken bones and increase the risk of fractures and osteoporosis.
Early prevention is crucial, as maintaining healthy bones throughout life can help reduce the risk of bone diseases later on.
Role of Nutrition in Bone Health
Nutrition plays a vital role in bone development and maintenance. Key nutrients for strong bones include:
Calcium: Found in dairy products, leafy greens, and fortified foods, calcium is essential for bone strength.
Vitamin D: This vitamin helps the body absorb calcium. Sunlight, fatty fish, and fortified foods are good sources.
Magnesium: Vital for bone structure, magnesium can be found in nuts, seeds, and whole grains.
A balanced diet rich in these nutrients supports bone density and can help prevent conditions like osteoporosis.
Challenges in Bone Abnormality Treatments
Barriers to Treatment Access
Access to treatment for bone abnormalities varies worldwide. Some of the challenges include:
Cost of Treatment: Many advanced treatments, such as surgeries or specialized medications, can be expensive, limiting access for patients in low-income areas.
Healthcare Access: In developing countries, access to advanced diagnostic tools and specialists may be limited, leading to delayed diagnoses and inadequate treatment.
Efforts to increase awareness and improve healthcare access are essential to address these disparities.
Managing Chronic Bone Conditions
Conditions like osteoporosis and Paget's disease require lifelong management. Patients often face challenges, such as:
Ongoing Treatment: Medication regimens may need to be followed for years, and patients may need regular check-ups to monitor bone health.
Psychological Impact: Living with chronic bone conditions can lead to emotional and psychological challenges, particularly for those with visible deformities or frequent pain.
Support systems and educational programs play a vital role in helping patients manage these long-term conditions.
Patient Support and Resources
Patient Advocacy and Support Networks
Bone disorders can significantly impact a patient’s quality of life. Fortunately, several support networks and advocacy groups provide assistance, including:
Osteoporosis Foundations: These organizations offer resources on treatment options, lifestyle modifications, and support groups.
Bone Disease Awareness Groups: Many global initiatives aim to raise awareness about bone health, providing information and emotional support for patients and families.
These groups offer crucial resources for patients navigating their treatment journeys.
Post-Treatment Care and Rehabilitation
After surgery or significant treatments, rehabilitation is often required to ensure full recovery. Rehabilitation focuses on:
Physical Therapy: Tailored exercises to restore strength and mobility.
Long-Term Follow-Up: Regular check-ups to monitor healing progress and detect any complications early.
Post-treatment care is crucial to ensure patients regain full functionality and prevent further bone damage.
Global Popularity of Bone Abnormality Treatments
Bone Disorder Treatment Popularity Around the World
Bone treatments vary widely across the globe, with access and popular treatment methods differing:
Developed Countries: Countries with advanced healthcare systems typically have higher access to innovative treatments like robotic surgeries, stem cell therapies, and gene therapies.
Developing Countries: In many developing nations, bone disorder treatments are often limited to basic medical care, and patients may not have access to the latest technologies.
Despite these disparities, global efforts are ongoing to make bone disorder treatments more widely available.
Healthcare Systems and Bone Disorder Care
Healthcare systems play a significant role in managing bone health. In countries with universal healthcare, bone disease treatments are more accessible to the population. However, in regions without sufficient healthcare coverage, patients often struggle to afford treatment. Improving healthcare infrastructure and offering more affordable treatment options are key to addressing this global challenge.
Case Studies and Real-Life Examples
Real-Life Success Stories
Many individuals have successfully managed bone abnormalities through early intervention and advanced treatments. For example:
Osteoporosis Treatment Success: A 60-year-old woman with osteoporosis who started bisphosphonate therapy was able to reduce her fracture risk and improve her quality of life, demonstrating the importance of early diagnosis and medication.
Scoliosis Correction: A young girl with severe scoliosis underwent spinal fusion surgery, resulting in a significant reduction in her spinal curvature and a return to normal activities.
These stories highlight the positive outcomes possible with appropriate care and treatment.
Challenges Faced by Patients
While many patients experience successful treatments, others face long-term challenges. Some patients with osteogenesis imperfecta may continue to experience fractures even with medication, and others with severe scoliosis may need multiple surgeries over their lifetime.
These challenges underscore the need for comprehensive, ongoing care and emotional support to help patients cope with the physical and mental impacts of bone abnormalities.
Future Outlook for Bone Abnormalities
Innovative Treatments on the Horizon
The future of bone abnormality treatment is promising, with many exciting developments:
Biologics and Regenerative Medicine: Stem cell therapy and gene editing hold the potential to regenerate bone tissue and correct genetic defects.
Personalized Medicine: With advances in genomics, treatments tailored to an individual’s specific genetic makeup could improve the effectiveness of therapies for bone disorders.
Robotics in Surgery: Robotic-assisted surgeries offer more precise bone surgeries, reducing recovery time and improving outcomes.
These advancements may revolutionize the treatment landscape for bone abnormalities in the coming years.
Global Collaboration in Research
International collaborations in medical research are vital for advancing bone disease treatments. Scientists and healthcare providers from around the world are working together to improve diagnostic tools, find new therapies, and create global guidelines for the treatment of bone abnormalities. This collective effort will likely lead to better outcomes for patients everywhere.
Bone Abnormalities and Quality of Life
Impact on Daily Life
Bone abnormalities can significantly affect a person's ability to perform everyday activities. Conditions like severe scoliosis can cause chronic pain, limited mobility, and difficulty with tasks like bending or lifting. Osteoporosis increases the risk of fractures, which may limit a person’s independence.
However, with the right treatment, many patients can manage their condition effectively and return to an active, fulfilling life. Physical therapy, pain management, and adaptive devices can help people maintain independence and improve their overall well-being.
Improving Self-Esteem and Mental Health
Living with a bone abnormality can also take an emotional toll. Many patients experience feelings of frustration, embarrassment, or anxiety due to their physical limitations or visible deformities. Treatment options such as corrective surgeries or physical therapy, combined with psychological support, can help improve both physical health and mental well-being.
Bone Abnormalities in Older Adults
Bone Health as We Age
As we age, bones naturally become weaker, and the risk of developing bone abnormalities increases. Conditions like osteoporosis, osteoarthritis, and fractures become more common in older adults due to decreased bone density and muscle mass. In older adults, even minor falls can lead to severe fractures, especially in the hip or spine.
Osteoporosis: This condition, characterized by brittle bones, is most common in postmenopausal women but can affect men as well. Early screening, regular exercise, and calcium supplementation are essential in managing the condition.
Osteoarthritis: Degeneration of cartilage in joints can lead to painful bone spurs, stiffness, and reduced mobility. Treatment may include pain management, physical therapy, and joint replacement in severe cases.
Early intervention and lifestyle changes are key to maintaining bone health in older adults.
Preventing Falls and Fractures
Preventing falls is a priority for older adults with bone abnormalities. Simple adjustments in the home, such as removing tripping hazards, using assistive devices like walkers, and wearing non-slip footwear, can greatly reduce the risk of falls. Balance exercises and strength training are also beneficial in improving stability and bone strength.
Role of Technology in Bone Abnormality Diagnosis
Advancements in Diagnostic Tools
Technology plays an essential role in diagnosing bone abnormalities accurately and early. Some key diagnostic tools include:
X-rays: Still the most common imaging technique to detect fractures, deformities, and diseases like arthritis.
CT Scans and MRIs: Provide detailed images of bone structures and soft tissues, helping to diagnose conditions like bone tumors or infections.
DEXA Scans: Dual-energy X-ray absorptiometry scans are used to measure bone mineral density and assess the risk of osteoporosis.
These tools, along with advanced computer algorithms, allow doctors to detect bone abnormalities earlier, leading to more effective treatment and better outcomes.
AI and Machine Learning in Bone Health
Artificial intelligence (AI) is increasingly being used in radiology to improve diagnostic accuracy. AI algorithms can analyze medical images faster than human doctors, helping identify abnormalities that might be missed. Additionally, AI can be used to predict bone fractures or disease progression, offering more personalized treatment plans for patients.
Global Awareness and Education on Bone Health
Raising Awareness Worldwide
Bone health awareness is crucial for preventing and treating bone abnormalities globally. Several organizations and initiatives focus on spreading knowledge about bone diseases, risk factors, and the importance of bone health. Some prominent efforts include:
World Osteoporosis Day: An international event dedicated to raising awareness about osteoporosis and bone health.
Public Health Campaigns: Governments and healthcare systems run public health campaigns to educate people about the importance of calcium, vitamin D, and exercise in maintaining strong bones.
These efforts help promote early detection, prevention, and effective management of bone disorders.
Educational Resources for Patients
Patients with bone abnormalities often feel overwhelmed by their diagnosis. Access to educational resources, whether online, through healthcare providers, or through support groups, is essential. These resources can provide information on treatment options, self-care, and lifestyle adjustments, empowering patients to take charge of their bone health.
Conclusion
Managing bone abnormalities requires a comprehensive approach that combines medical treatment, lifestyle changes, and emotional support. Early diagnosis and timely interventions—whether through medication, physical therapy, or surgery—can significantly improve quality of life.
Adopting preventive measures, raising awareness, and providing education are essential to maintaining bone health. As medical advancements continue, patients with bone conditions can expect better treatment options, giving them the tools to manage their health and lead fulfilling lives.