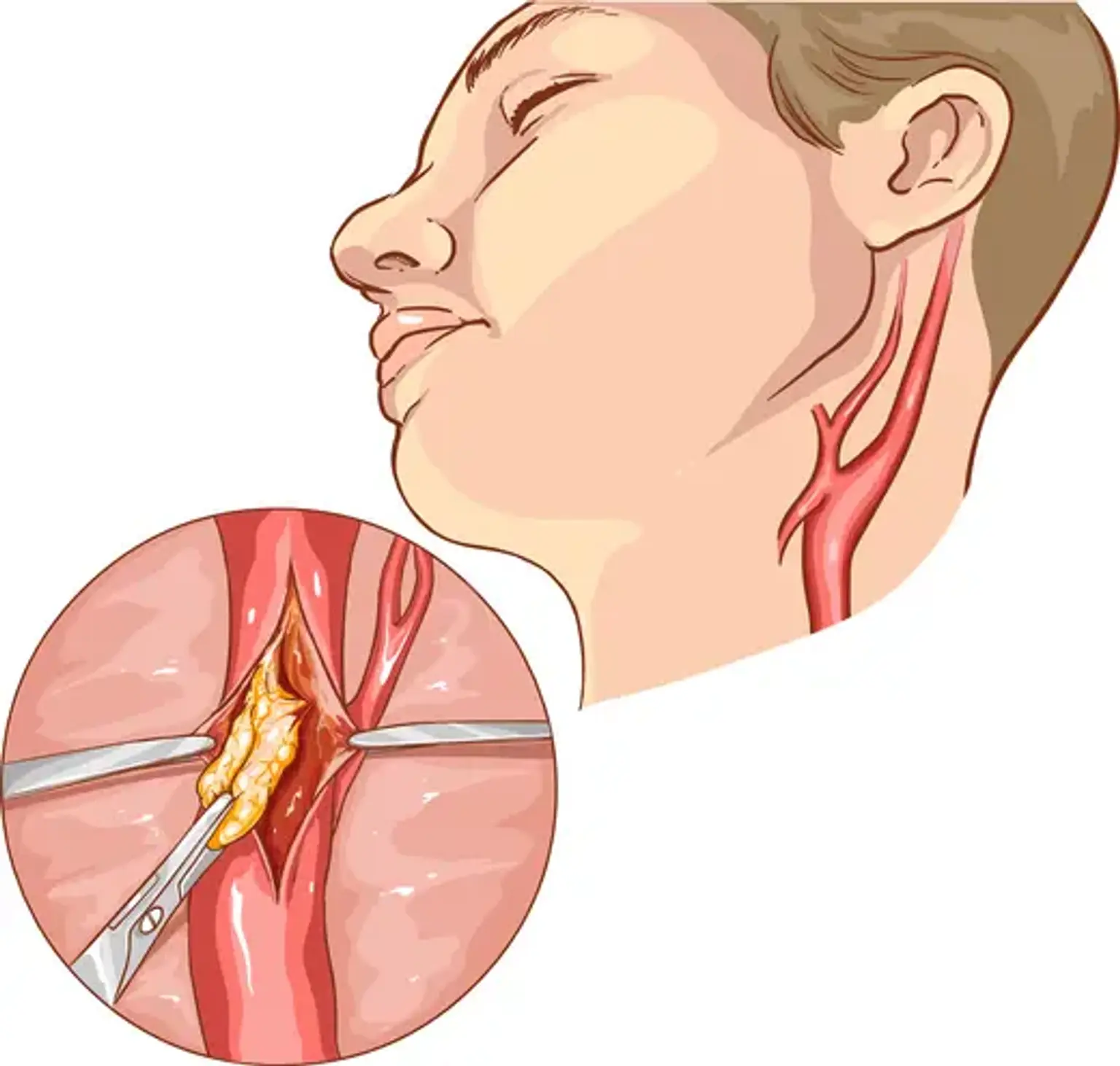
Carotid Surgery
Overview
Every year in the United States, more than 795,000 people experience a stroke, according to the Centers for Disease Control and Prevention (CDC). The majority of these strokes are caused by carotid artery disease or atrial fibrillation, an abnormal heartbeat. According to the National Heart, Lung, and Blood Institute, carotid artery disease accounts for more than half of all strokes in the United States.
Carotid artery surgery (Carotid endarterectomy) is used to treat carotid artery disease. This condition develops when fatty, waxy deposits form in one of the carotid arteries. The carotid arteries are blood vessels on both sides of your neck (carotid arteries).
A stroke can occur as a result of carotid artery disease. Plaque or a blood clot that has clogged the artery can cause these obstructions. By doing a CEA, your doctor aids in the prevention of strokes by keeping blood flowing to your brain.