Introduction
Cataracts are a leading cause of vision impairment worldwide, particularly affecting older adults. In fact, over 24 million Americans age 40 and older have cataracts, and this number is expected to grow as the global population ages. Cataracts occur when the lens of the eye becomes cloudy, leading to blurred vision. For many, this condition significantly impacts their ability to perform daily tasks such as driving, reading, or even recognizing faces. Fortunately, cataract diagnosis and treatment have advanced, allowing millions to regain clear vision.
What Are Cataracts?
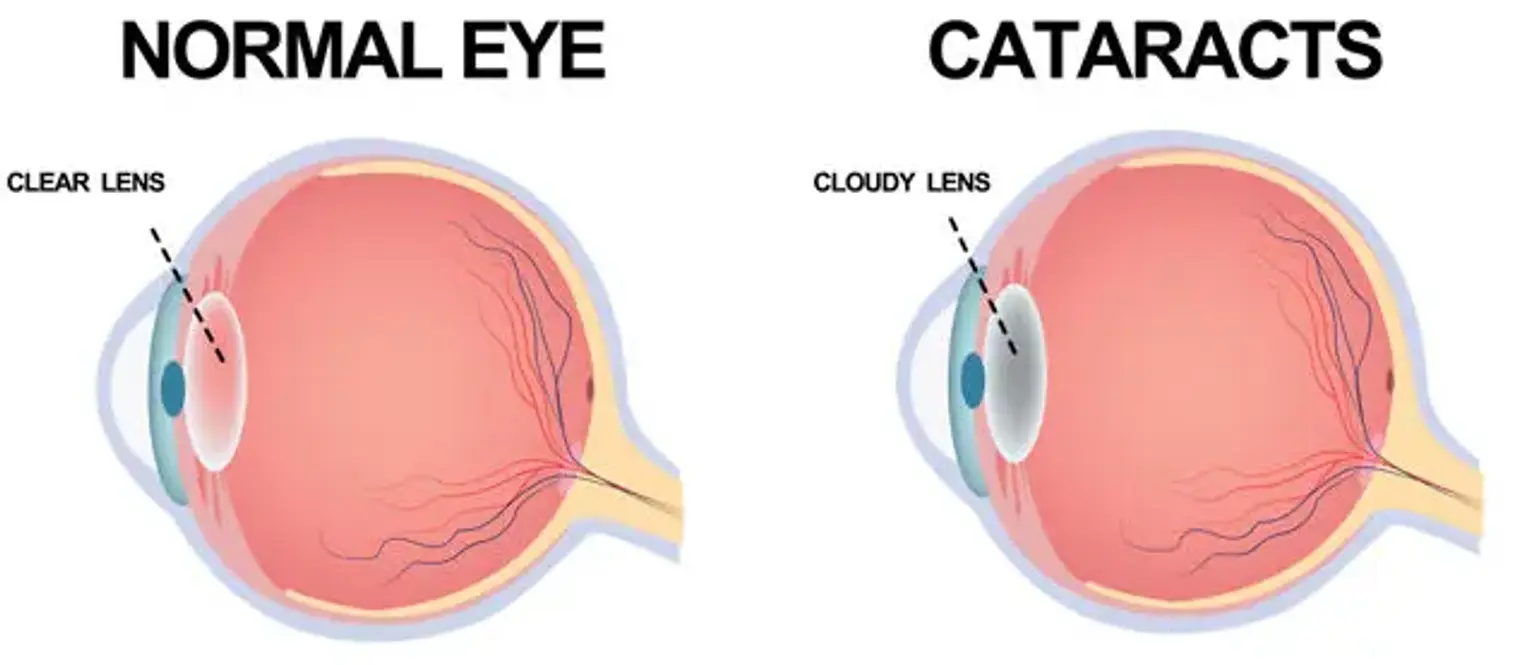
A cataract is a clouding of the eye's natural lens, located behind the iris. This lens helps focus light onto the retina, which sends visual information to the brain. As cataracts develop, light is scattered instead of being focused properly, leading to blurred or cloudy vision.
The most common type is age-related cataracts, which progress gradually over time. Other forms include congenital cataracts (present at birth), traumatic cataracts (due to injury), and secondary cataracts (from other health conditions like diabetes or medication).
How Cataracts Are Diagnosed
Cataract diagnosis typically involves a comprehensive eye examination conducted by an optometrist or ophthalmologist. The process usually includes the following steps:
Visual acuity test: The doctor will check how well you can see at various distances using an eye chart.
Slit-lamp examination: A special microscope is used to examine the structures of your eye, including the lens, for any cloudiness.
Pupil dilation: Eye drops are used to widen the pupils, allowing the doctor to inspect the back of the eye and assess the cataract’s size and location.
Tonometry: This test measures eye pressure to rule out other eye conditions, such as glaucoma, which can be present alongside cataracts. Regular eye exams are crucial, particularly for individuals over 60 or those at higher risk, to catch cataracts early and prevent further vision deterioration.
Risk Factors for Developing Cataracts
Several factors increase the likelihood of developing cataracts, especially as we age. Here are the most common risk factors:
Age: The risk of cataracts increases significantly after the age of 60. This is the most common cause of cataract formation.
Diabetes: People with diabetes are at a higher risk due to changes in blood sugar levels that can affect the lens of the eye.
UV Exposure: Long-term exposure to ultraviolet (UV) rays from the sun can accelerate cataract development. Wearing sunglasses with UV protection can help reduce this risk.
Smoking: Smoking introduces harmful chemicals into the body, which can increase the risk of cataract formation.
Family History: Genetics also play a role; those with a family history of cataracts are more likely to develop them.
Eye Injuries: Trauma to the eye can lead to the formation of cataracts years after the injury occurs.
Understanding these risk factors can help you take steps to manage your eye health, such as protecting your eyes from UV rays, quitting smoking, or controlling your blood sugar.
Common Symptoms of Cataracts
The symptoms of cataracts typically develop slowly and can vary depending on the type and severity. The most common signs include:
Blurry or cloudy vision: Objects may appear hazy or fuzzy.
Sensitivity to light and glare: Bright lights, such as headlights while driving at night, may cause discomfort.
Difficulty seeing at night: Reduced contrast in dim lighting can make night driving especially challenging.
Double vision: Some people experience a doubling of images in one eye.
Faded colors: Colors may appear less vibrant or washed out. If you experience any of these symptoms, it’s essential to see an eye care professional for a proper diagnosis.
Cataract Surgery: When Is It Needed?
Cataract surgery is recommended when the cataract causes significant vision problems that interfere with daily activities like reading, driving, or working. The decision to have surgery depends on several factors:
Severity of Vision Impairment: If vision loss affects your quality of life, surgery becomes a necessary option.
Patient's Health: Some medical conditions might influence the timing of surgery. For example, patients with uncontrolled diabetes may need to stabilize their blood sugar levels before surgery.
Progression of Cataract: Cataracts develop gradually, and surgery is typically considered when they reach a stage where other interventions like glasses are no longer effective. The surgery itself is quick and generally low-risk, with a high success rate. However, it’s important to discuss the timing with your doctor to ensure the best outcomes.
Different Types of Cataract Surgery
There are several surgical techniques for cataract removal, each with its advantages. The choice of method depends on the severity of the cataract and the patient's individual needs:
Phacoemulsification (Phaco Surgery): This is the most common and minimally invasive method. The surgeon makes a small incision in the eye, uses ultrasound to break up the cloudy lens, and then removes the fragments. A synthetic intraocular lens (IOL) is inserted to replace the clouded lens. This procedure typically allows for faster recovery and fewer complications.
Extracapsular Cataract Extraction (ECCE): This method is used for more advanced cataracts that cannot be broken down with ultrasound. The surgeon removes the entire lens in one piece through a larger incision. While it requires a longer recovery period than phacoemulsification, it is still highly effective.
Femtosecond Laser-Assisted Cataract Surgery (FLACS): A newer technology that uses lasers for greater precision in creating incisions and breaking up the cataract. FLACS is thought to offer better outcomes in certain cases, reducing the need for manual steps in the surgery.
Each of these procedures has been shown to be safe and effective, but your doctor will recommend the most appropriate option based on your specific situation.
Non-Surgical Treatment for Cataracts
In the early stages of cataract formation, surgery may not be necessary. Non-surgical treatments can help manage symptoms and delay the progression of cataracts:
Eyeglasses or Contact Lenses: New prescriptions can help improve vision by compensating for the blurred or cloudy areas caused by the cataract.
Magnifying Lenses: These can assist with reading or seeing fine details, especially in low-light conditions.
Lighting Adjustments: Brighter lighting at home or work can help with glare and improve visibility.
Anti-glare Sunglasses: These can reduce sensitivity to light and glare, making it easier to drive or go outdoors.
Diet and Antioxidants: Some research suggests that a diet rich in antioxidants, like vitamins C and E, may help slow cataract progression. However, this is not a substitute for surgical treatment when the cataracts become more advanced.
While these methods provide temporary relief, they do not stop cataracts from worsening, and surgery will eventually become necessary if vision impairment affects daily life.
Cataract Surgery Process: Step-by-Step
Cataract surgery is generally a straightforward and quick procedure, often performed on an outpatient basis. Here’s what you can expect during the surgery:
Pre-Surgery Assessment: Before the surgery, your ophthalmologist will conduct a thorough eye examination. This may include measuring the size and shape of your eye to determine the appropriate type of intraocular lens (IOL) for you.
Anesthesia: Cataract surgery is usually performed under local anesthesia, meaning the area around your eye will be numbed. You’ll remain awake during the procedure, but you won’t feel pain.
The Surgery: The surgeon will make a tiny incision in the eye, typically smaller than 3mm. Using an ultrasonic probe (in phacoemulsification), the cataract is broken up into small pieces. These fragments are gently suctioned out, and the new IOL is inserted through the incision.
Closing the Incision: In most cases, no stitches are needed. The incision is so small that it usually heals on its own.
After Surgery: You’ll be taken to a recovery room for a short period before being allowed to go home. The entire procedure typically takes around 15-30 minutes per eye.
Risks and Complications of Cataract Surgery
While cataract surgery is generally safe, like any medical procedure, it carries some risks. However, complications are rare, and the success rates are very high. Common risks and complications include:
Infection: Though rare, an infection can develop in the eye after surgery. Your doctor will provide antibiotics to prevent this.
Inflammation: Mild inflammation is common, but it’s usually managed with anti-inflammatory eye drops.
Retinal Detachment: This is a serious complication but is very uncommon. It occurs when the retina, the light-sensitive layer at the back of the eye, detaches from its normal position.
Posterior Capsule Opacification (PCO): This is a condition where the thin membrane that holds the IOL becomes cloudy over time, causing blurred vision. It can be easily treated with a quick laser procedure.
Glaucoma: Increased pressure in the eye may develop after surgery, requiring further treatment.
Dropped Lens: In rare cases, the lens can fall into the back of the eye, requiring additional surgery to retrieve it.
Your surgeon will discuss these risks and the steps they take to minimize them.
Cataract Surgery Recovery: What to Expect
Cataract surgery recovery is generally quick, and most patients experience significant improvement in vision within a few days. Here’s what to expect:
First Few Days: Immediately after surgery, you may feel some mild discomfort, such as a scratchy or gritty feeling in the eye. You may also experience blurry vision, which usually improves within a few hours to a few days.
Post-Operative Care: You’ll be prescribed antibiotic and anti-inflammatory eye drops to help prevent infection and reduce inflammation. It’s essential to follow the instructions carefully.
Activity Restrictions: You should avoid strenuous activities, heavy lifting, and bending over for the first few weeks. Swimming and rubbing your eyes should also be avoided.
Follow-Up Appointments: Your doctor will schedule follow-up visits to monitor the healing process. Typically, you’ll have a check-up within 1-2 days after surgery and again a week later.
Full Recovery: Most people can resume normal activities, like driving, within a week or two. However, full visual recovery may take a few weeks as the eye continues to heal and adjust to the new lens.
Cataract Surgery Success Rates and Benefits
Cataract surgery is one of the safest and most effective surgeries performed today, with a success rate of over 98%. The procedure dramatically improves vision and quality of life. Some of the key benefits include:
Improved Vision: Most people experience significant improvements in clarity and color perception after surgery. Many patients find they no longer need glasses for reading or driving, especially if multifocal IOLs are used.
Increased Independence: Restored vision allows individuals to regain their independence, helping them return to daily activities like driving, reading, and socializing.
Enhanced Quality of Life: Cataract surgery can reduce the risk of falls and accidents, and many patients report an improvement in overall mental well-being due to enhanced vision.
Long-Term Effectiveness: Cataract surgery outcomes last for many years. The IOLs used today are designed to remain functional for decades, providing long-term vision correction.
Faster Recovery: Thanks to modern surgical techniques, recovery is faster than ever, with many patients reporting no significant pain or discomfort.
Choosing the Right Intraocular Lens (IOL)
During cataract surgery, the clouded lens is replaced with a clear artificial lens called an intraocular lens (IOL). The type of IOL you choose can significantly impact your post-surgery vision. There are several options:
Monofocal IOLs: These provide clear vision at one distance, typically for either near or far sight, requiring glasses for the other.
Multifocal IOLs: These lenses offer clear vision at multiple distances, reducing the need for glasses.
Toric IOLs: Designed for patients with astigmatism, these lenses correct both the cataract and the refractive error.
Accommodating IOLs: These lenses adjust to focus on objects at different distances, providing more natural vision.
Your surgeon will help determine the best IOL for your lifestyle and visual needs.
Cost of Cataract Surgery
The cost of cataract surgery varies based on location, surgeon expertise, and the type of IOL chosen. On average, in the U.S., the cost can range from $2,000 to $3,000 per eye for standard surgery, while specialized lenses (like multifocal or toric IOLs) can increase the cost to $4,000 or more per eye. Health insurance typically covers the basic procedure but may not cover premium IOLs. Financing options, payment plans, and assistance programs are available for those who need them.
Cataract Surgery for Older Adults
Cataract surgery is one of the safest and most common surgeries for older adults. Age is not a barrier to surgery, as even individuals in their 80s and 90s can benefit from improved vision. In fact, treating cataracts in older adults can improve their quality of life significantly by enhancing independence and reducing the risk of falls or accidents. However, elderly patients may have additional health concerns, such as heart disease or diabetes, which need to be managed before surgery. It’s essential to work with your healthcare team to ensure the safest approach.
Preventing Cataracts and Maintaining Eye Health
While it’s not possible to entirely prevent cataracts, you can reduce your risk by adopting healthy habits:
Wear Sunglasses: Protect your eyes from UV rays by wearing sunglasses with 100% UV protection.
Quit Smoking: Smoking increases the risk of cataracts and other eye conditions.
Eat a Healthy Diet: A diet rich in fruits, vegetables, and antioxidants can help support eye health.
Regular Eye Exams: Routine eye exams can help detect cataracts early and allow for timely intervention.
Manage Health Conditions: Proper management of diabetes, high blood pressure, and other systemic conditions can help delay cataract formation.
How Cataract Surgery Improves Quality of Life
Cataract surgery has a profound impact on a patient's quality of life. Many people who undergo the procedure report a significant improvement in daily activities, such as reading, driving, and participating in hobbies. With restored vision, individuals experience increased independence and greater confidence. The ability to clearly see faces, enjoy nature, and resume daily tasks without glasses is often described as life-changing. For older adults, cataract surgery can also reduce the risk of falls and accidents by improving depth perception and overall vision clarity.
Understanding the Global Popularity of Cataract Surgery
Cataract surgery is the most performed surgical procedure worldwide, with millions of people undergoing the operation each year. Its global popularity is due to several factors:
Aging Populations: As populations around the world age, the prevalence of cataracts increases, leading to a growing demand for surgery.
High Success Rates: The procedure has a success rate of over 98%, making it a highly trusted and reliable solution.
Advancements in Technology: Improved surgical techniques, such as laser-assisted cataract surgery and advanced IOL options, make the procedure safer, quicker, and more effective than ever.
Accessibility: Cataract surgery is increasingly available in both developed and developing countries, making it a viable option for people worldwide.
Common Concerns About Cataract Surgery
While cataract surgery is generally safe and effective, patients may have concerns. Some of the most common concerns include:
Fear of Surgery: Many people worry about the risks associated with surgery. However, cataract surgery is minimally invasive, and complications are rare. The vast majority of patients experience excellent outcomes.
Cost: The cost of cataract surgery can be a barrier for some, especially for those who require premium IOLs. However, most insurance plans cover basic procedures, and financial assistance programs are available.
Post-Surgery Recovery: Some patients are concerned about recovery time. In reality, recovery is usually quick, with most people returning to normal activities within a week or two. Your surgeon will guide you through the post-surgery care process to ensure smooth healing. It’s important to discuss any concerns with your ophthalmologist to understand the procedure, its risks, and the expected results.
Conclusion
Cataract surgery has revolutionized the way we treat vision problems related to aging. With high success rates, minimal recovery times, and the ability to restore clear vision, the procedure offers life-changing benefits for millions of people worldwide. Whether you’re struggling with blurry vision or want to improve your overall quality of life, cataract surgery is a safe and effective solution. If you or a loved one is considering cataract surgery, consult with a qualified ophthalmologist to explore your options and take the first step toward clearer, brighter vision.