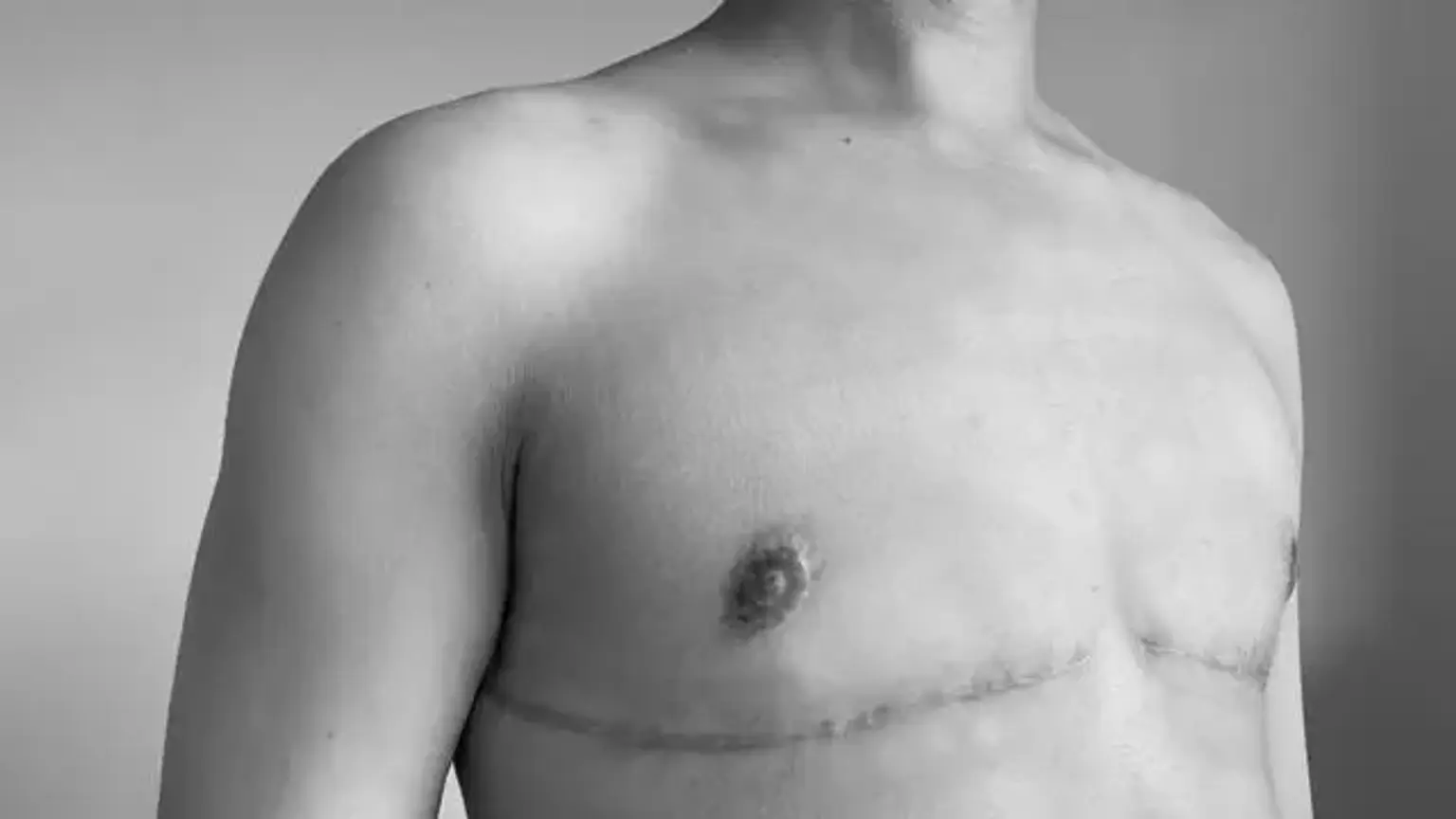
Chest Reconstruction Surgery
Chest reconstruction surgery is a type of reconstructive surgery that is conducted on the chest to change the size, shape, and general appearance of the chest. This procedure is usually carried out by a plastic surgeon who specializes in transgender or gender-affirming procedures.
Individuals desiring a more masculine or flat-appearing chest, as well as those desiring a more feminine dimensioned chest, can both benefit from this operation.
- Female-to-male or female-to-nonbinary chest reconstruction surgery. This involves removing breast tissue and reshaping the chest to provide the appearance of a flat, masculine, or male look.
- Male-to-female or male-to-nonbinary chest reconstruction surgery. This procedure entails the use of saline or silicone implants to boost chest size and form for a more feminine or female look.
FTM Chest Reconstruction Surgery
Chest reconstruction surgery, also referred to as top surgery or masculinizing chest surgery, aims to remove breast tissue from both breasts and give the chest a masculine or nonbinary appearance. A single-stage approach is used to conduct chest reconstruction surgery. There are a variety of techniques for doing chest surgery, and many variables should be considered when deciding which one is best:
- Breast tissue volume
- Excess skin quantity
- Desire for a breast sensation
Chest Reconstruction Surgery Indications
Chest reconstruction surgery is an extremely personal operation. You should do it for yourself, not to satisfy the desires of others or to conform to some ideal appearance.
If you meet the following criteria, chest reconstruction surgery may be a good choice for you:
- You've been told you have persistent gender dysphoria.
- You've been under the care of a mental health expert who can write you a letter supporting your choice to get surgery.
- You've been living as a member of the sex group of your preference.
- You have reached the legal age of consent.
- You have an optimistic outlook and reasonable goals.
- If there are severe medical or mental health concerns, they must be kept under reasonable control.
Chest Reconstruction Surgery Consultation
Prepare to talk about the following points during the consultation for chest reconstruction surgery:
- Your transition is going well.
- Your surgical objectives
- Drug allergies, health problems, and medical treatments
- Medications, vitamins, herbal remedies, alcohol, cigarettes, and drug usage are all factors to consider.
- Previous operations.
In addition, your surgeon will:
- Examine your overall health as well as any existing medical issues or risk factors.
- Examine the breasts and take measures of them, as well as the nature of their skin and the location of their nipples and areolas.
- Take pictures.
- Discuss options and make a therapeutic plan recommendation.
- Discuss the expected outcomes of chest reconstruction surgery, as well as any dangers or issues that may arise.
Remember to ask your plastic surgeon any questions you may have. It is vital that you comprehend all parts of the chest reconstruction surgery. To aid you, we've put up a list of questions to ask the plastic surgeon that you may bring with you to your appointment.
It's natural to experience some worry, whether it's the anticipation of your new look or apprehension about the procedure. Don't be afraid to express your emotions to the plastic surgeon.
Chest Reconstruction Surgery Approaches
Inverted T Approach
One method could be a transverse inframammary cut with free nipple-areolar grafts. If the skin is excessively puffy, the cut can be extended laterally (chasing a dog-ear) or a vertical midline cut can be made (inverted T). The areola is cut to a pre-determined diameter, and the nipple is partitioned and rebuilt using a pie-shaped excision. Because of the nerve damage, there may be various degrees of sensory loss.
Double Incision Chest Reconstruction Surgery
A double incision is one of the most popular male chest reconstructive operations, involving a cut above and below the breast mass, excision of fatty and glandular tissue, and skin sealing. This procedure causes scars that reach from the underarms to the medial pectoral muscles under pectoral muscles.
To create male-looking nipples, a double incision is frequently combined with free nipple grafts. Cutting away along the perimeter and separating the top layer of flesh from the remainder of the tissue, the areola and nipple are separated from the breast tissue. The nipples are transplanted on in the typical male position once the chest has been reconstructed. Female areolae are frequently larger in circumference and the nipples project more, hence the areolae and nipples are often shrunk down.
Nipple grafts are most commonly associated with double-incision chest reconstruction; however, they can be utilized in any reconstruction operation if needed. Rejection is possible with nipple grafts. In these circumstances, the nipple is frequently tattooed back on aesthetically, or other surgical techniques are used.
Over time, some sensation should recover in the grafted nipples. However, because the surgery cuts the nerves that run into the nipple-areola, there is a considerable threat of losing sensation.
Keyhole Approach
There are three fundamental techniques for removing the glandular and fatty tissues that make up the breast mass, as well as the extra skin that covers it.
A peri-areolar incision can be used for petite breasts. This procedure involves a circular cut around the areola, as well as an internal circular incision to excise some of the unwanted areola. The skin will wrinkle as it is drawn into the center, but this will usually smooth out over time. There will be considerable tension on the scar line, and a permanent fixation stitch will be required to prevent the scar from spreading. The survival of the marginalized areola is aided by leaving the outer dermis underneath it.
The keyhole incision enhances the peri-areolar incision by creating a vertical closure underneath when the unwanted skin is brought in from the sides and the extra is eliminated.
A transverse incision, generally in the inframammary fold, is added to the anchor incision to remove even more extra skin. Draping or blousing isn't a good idea. This is reserved for women with postpartum breast shrinkage, who have considerably larger breasts or a larger topographically larger surface area.
The nipple-areolar complex may be anchored by a pedicle, which has the advantage of maintaining some sensation and blood flow intact but has the problem of not providing the flat look most patients prefer when the pedicle has adequate size.
Dog Ear Approach
When the side limbs are very long, surgeons refer to it as chasing a dog’s ear into the axilla. When there is too much aggregation at an angle greater than 30 degrees, a dog ear is an uncomfortable ruffle of skin in the corner of an incision. Although using a curved incision reduces the risk of developing dog ears by requiring less skin accumulation, some patients dislike the appearance of the bent scar because it can resemble breasts.
After three or more months of settling, the surgeon may decide to adjust the incision lines if some remaining trouble spots are visible.
Chest Reconstruction Surgery Preparation
You may be requested to do the following in order to prepare for chest reconstruction surgery:
- Obtain laboratory testing or a medical evaluation.
- A document of recommendation from the therapist.
- Take some medications or make changes to the prescribed ones.
- Quit smoking.
- Aspirin, anti-inflammatory medications, and herbal remedies can all cause increased bleeding and should be avoided.
Chest reconstruction surgery is usually done in a hospital or ambulatory surgical center, and general anesthesia is used. Some follow-up procedures can be done as an outpatient procedure with local anesthetic and sedation. These choices will be made based on the unique requirements of the operation, as well as your preferences and your doctor's professional judgment.
Chest Reconstruction Surgery procedure
Anesthesia
During the surgical procedure, doctors will give you medications to help you relax. Intravenous sedatives and general anesthetic are two options. Your doctor will advise you on the best for you.
Mastectomy (Breast Tissue Removal)
The breast tissue on the chest will be removed during a mastectomy. Excess skin may also need to be removed at times.
Forming a Masculine Figure
Following the removal of the breast tissue and any superfluous skin, the residual tissues must be adjusted to create a masculine chest shape.
Repositioning the Nipple and Areola
Following the mastectomy, the nipple and areola may need to be decreased and/or relocated on the chest. On the male chest, the nipple and areola are smaller and lay slightly more lateral and inferior.
Chest Reconstruction Surgery Results
The ultimate effects of chest reconstruction surgery may contribute to decreasing feelings of gender dysphoria that certain people may have.
When female breast tissue is removed, some sensation in the chest is usually lost as well. Some sensation in the chest skin and nipples may recover over time, and scar lines will fade, though they will never entirely disappear. Although there are trade-offs, most transmen believe these are minor in comparison to the significant improvement in their quality of life and ability to appear and feel like a man.
Despite the fact that breast tissue is excised during the treatment and breast tissue growth is slowed by testosterone treatment, the risk of breast cancer does not go away. Breast health must be carefully monitored through self-examination.
If you have shortness of breath, chest aches, or irregular heartbeats when you get home, seek medical help immediately. If any of these problems arise, you may need to be admitted to the hospital and receive additional treatment.
Medical and surgical practice is not a magic science. Although positive outcomes are predicted, there is no assurance. In some cases, a single surgical treatment may not be enough to obtain optimal outcomes, and another procedure may be required.
The outcome of the surgery depends on you following your doctor's recommendations. During the recovery period, it is critical that the surgical incisions are not subjected to undue force, friction, or motion. The doctor will provide you with detailed advice on how to take care of yourself.
Chest Reconstruction Surgery Risks
Negative anesthetic reactions, blood loss, blood clots, and artery obstructions are all dangers associated with surgical operations. In extreme circumstances, these problems can lead to death. It's critical to go over these concerns with the surgeon in depth. The surgical care team will take a variety of precautions to avoid these issues, recognize them if they occur, and respond properly. They will also advise you of the steps you can take to reduce the risks.
The following is a list of some of the risks associated with chest reconstruction surgery in particular (It is not a substitute for a complete discussion with your surgeon):
- Hematoma. When blood accumulates in the surgical site, pain, swelling, and redness develop. It is the most common problem. Hematomas are prevented with the use of drains and compression bandages. Smaller hematomas can be suctioned out, while larger ones must be surgically removed.
- Abscess formation. An abscess is a pus-filled pocket. A bacterial infection is a culprit in abscess formation. Antibiotics can be used to treat it, or the surgeon can evacuate it.
- Seroma. When clear fluid collects in the surgical site, this is what it means. Small seromas may need to be sucked out by the surgeon once or twice. Larger seromas may require surgery to be treated.
- Nipple asymmetry. This occurs when the contour or position of the nipple on one side differs from the nipple on the other side. Asymmetry is quite prevalent. A surgical revision can be used to address asymmetry that is quite noticeable.
- Contour abnormalities. This occurs when the skin tissue does not have the desired shape. Liposuction can be used to repair major contour defects. Depending on the doctor and procedure, this is required in roughly 8-25% of cases.
- Scarring. Scarring is to be anticipated, and the degree of scarring varies depending on the procedure. Surgical revision may be required if the scarring is extensive. Following your surgeon's recommendations for rest, sun protection, massage exercises, and ointments will help you avoid significant scarring.
- Sensation loss. You can feel a loss of sensation in the nipples and chest. With a free nipple graft, you're more likely to lose sensation in the nipples.
- Nipple necrosis. The nipple, or a portion of it, falls off at this point. It may be feasible to save it if it occurs within hours of surgery. It may have to be repaired as a free graft or reconstructed using adjacent skin and tattooing procedures if this occurs lately. This is a rare complication.
Chest Reconstruction Surgery Recovery
Recovery Timeline
Because of the drains and the fact that you will be ordered not to shower, the first week after chest reconstruction surgery is frequently the most uncomfortable. Furthermore, the activity limitations set by chest reconstruction surgery are much longer.
You will be advised to avoid lifting the arms over shoulder height for the first four to six weeks following surgery, as well as lifting heavy loads. Unless they engage in physically demanding jobs, most people can return to modified work or school after about a week.
It is advised that children use a backpack for at least four to six weeks. Consider asking the help of friends to carry the books, or invest in a rolling backpack.
People who have jobs that require them to lift, carry, or have their arms raised over their shoulders should talk to their manager about reduced duties.
If you have worries about scar size or dog ears (extra skin) after you have fully recovered from chest reconstruction surgery, contact the surgeon. They may recommend revision surgery to address these concerns if it is practicable. The frequency with which corrections to chest reconstruction surgery are required is significantly dependent on the technique performed.
Recovery Tips
- Don't take a shower. Many surgeons advise you not to shower till the bandage is removed at your postoperative checkup. In the meantime, baby wipes and sponge showers are two of the greatest and most convenient ways to clean.
- Make use of ice packs. After the operation, most patients suffer some swelling and bruising, but the degree of swelling and bruising varies widely. Ice packs can aid to relieve pain and reduce inflammation.
- Lifting weights or engaging in strenuous activity is not recommended. It's not a good idea to lift anything heavier than a gallon of milk during the first week of rehabilitation. As soon as you feel up to it, you can continue modest activities such as walking; however, avoid doing anything that causes your heart rate to rise.
- Make sure you look after yourself. Rest, eating a good diet, avoiding smoking and drinking, and listening to the body are the greatest ways to speed up the healing process.
- Scar treatments should be used. Scar treatments available over the counter can help speed up the healing process while also reducing scar tissue and irritation.
Coping with Recovery
Following chest reconstruction surgery, many people experience a period of happiness. However, it is not uncommon for one's mood to plummet afterward.
Depression is prevalent following any major surgery, and there are extra factors that may increase the risk of depression following chest reconstruction surgery.
Following this operation, there are a number of factors that can lead to depression:
- You may have been aiming toward chest reconstruction surgery for a long time, and once you've achieved what seemed to be an all-encompassing dream, you may feel aimless.
- Furthermore, some people feel that undergoing chest reconstruction surgery will solve all of their problems, which is virtually never the case. Recognizing that some obstacles and challenges remain after such a life-changing event might be frustrating.
- After having chest reconstruction surgery, people may also be frustrated by activity restrictions. This is especially true for those who have surgery during the summertime.
- Many people who have undergone chest reconstruction surgery have looked forward to going shirtless outside for a long time, however, patients will be advised to keep their surgical site away from the bright sun for a period of time to improve healing.
Wound Care
Following chest reconstruction surgery, follow the surgeon's wound care instructions. Wound care varies greatly depending on the procedure and the type of dressings applied.
Although most people recover well from chest reconstruction surgery, your healthcare professional will let you know if there are any indicators that you should return for treatment right away, such as pain or swelling on one side of the body. Do not delay contacting the surgical team if you develop any of these symptoms.
The surgical team or doctor may prescribe scar massage once the surgical site has begun to heal. Scar massage is done to try to keep the surgical scar as tiny and red as possible. Because vigorous scar massage could cause more harm than help, it should be done slowly and delicately. You should wait until the surgeon says it's okay to start scar massage.
Chest Reconstruction Surgery Cost
The typical cost of chest reconstruction surgery varies significantly based on body size, shape, and targeted breast size. The cost of this procedure often ranges between 5,000 and 10,000 dollars.
The cost of chest reconstruction surgery varies according to the surgeon's skill and geographic region. Ask the plastic surgeon about patient payment options for chest reconstruction surgery.
The following things may be included in the cost of chest reconstruction surgery:
- Fee for a surgeon
- Costs of the hospital or surgical facility
- Fees for anesthesia
- Medication prescriptions
- Garments to wear after surgery
- X-rays and medical testing
Remember that the surgeon's experience and your familiarity with him or her are just as essential as the ultimate cost of the procedure when picking a board-certified cosmetic surgeon for chest reconstruction surgery.
Chest reconstruction surgery is a reconstructive treatment that is usually funded by insurance. However, your insurance may only pay some of the general cost.
What Else Do I Need to Know?
Doctors cannot perform this procedure on individuals who use any kind of nicotine because it raises the risk of problems throughout the recovery period. Before surgery, nicotine testing is performed. Doctors will test for people who have a strong history. This is for the sake of the patient's safety.
Stimulant drugs like cocaine, amphetamines, and methamphetamines, among others, can wreak havoc on wound healing and should be avoided before surgery. Doctors will test for people who have a strong history.
BMI less than 30 yields better results, however BMI up to 35 can be considered on a case-by-case basis.
While regular marijuana usage has no documented wound healing risks, it does cause anesthetic issues, which should be avoided before the surgery and discussed in depth with the anesthesia practitioner to provide the safest experience possible.
Conclusion
Chest reconstruction surgery is a popular surgery that is used to reshape chest abnormalities and make them more natural. This is personal surgery that needs good thinking and comprehensive discussion with your doctor. As with all major surgery, chest reconstruction surgery exposes the patient to a few complications, most of which are short-lived.