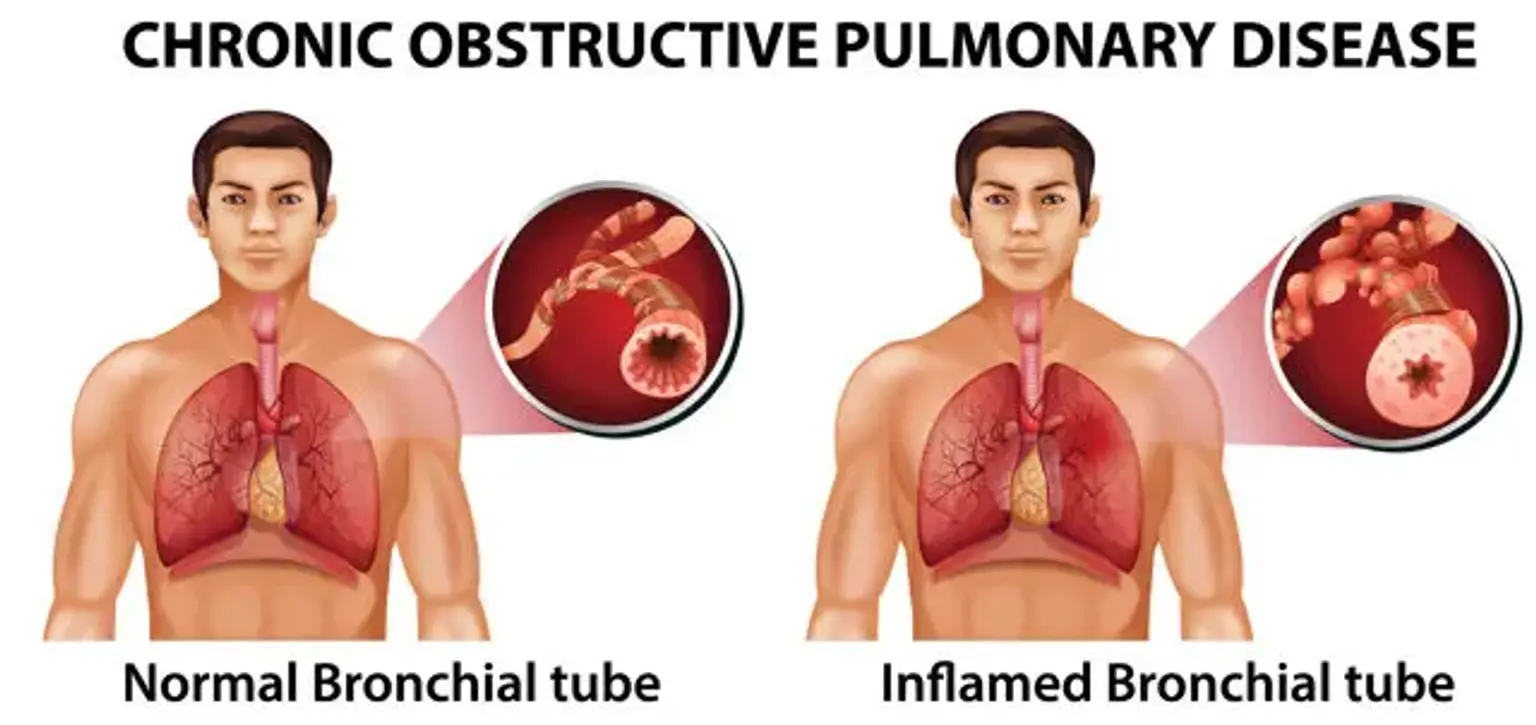
Chronic obstructive pulmonary disease
Chronic obstructive pulmonary disease (COPD) is a group of illnesses that leads to airflow obstruction and breathing issues. Chronic bronchitis and emphysema are the most common disorders that can lead to COPD. If you've been diagnosed with COPD, you may have one or both of these respiratory illnesses or symptoms of the two. COPD can progress slowly, making breathing increasingly difficult with time.
COPD is generally treatable, even though it is a progressive condition that worsens with time. Most patients with COPD can obtain good symptom management and quality of life with effective control and a lower chance of developing other illnesses.
Signs and Symptoms of Chronic Obstructive Pulmonary Disease
COPD makes breathing difficult. At first, the symptoms may be minor, with occasional coughing and shortness of breath. Symptoms can get more consistent as time goes on, making breathing increasingly difficult.
The signs and symptoms of chronic obstructive pulmonary disease include;
- Wheezing
- Shortness of breath, particularly during exercise
- Chest tightness
- Constant respiratory infection
- A serious cough which produces sputum or mucus that can be white, clear, greenish, or yellow
- Lack of energy
- Swelling around the feet, legs, or ankles
- An unexpected loss of weight
Patients who have COPD are more likely to have exacerbations. These are the periods that arise when their symptoms worsen and last for a number of days.
Causes of Chronic Obstructive Pulmonary Disease
Many patients with chronic obstructive pulmonary disease COPD are mostly 40 years of age and have smoked at some point in their lives. The longer you smoke and the more tobacco products you consume, the more likely you are to get COPD.
COPD can occur due to pipe smoke, cigar smoke, and secondhand smoke, in addition to cigarette smoke. If you are a smoker and have asthma, your chances of developing COPD are even higher.
Air passage obstruction:
The leading causes of air path obstruction are;
- Emphysema
This occurs when the walls inside your lungs' air sacs (alveoli) are destroyed, causing them to join one large air sac. You get less oxygen in the bloodstream since it can't take in oxygen too.
The lungs may expand out and lose springiness as a result of the damaged alveoli. You are likely to be short of breath because air will be trapped in your lungs; hence, you cannot expel it out.
- Chronic bronchitis
Chronic bronchitis is characterized by shortness of breath, coughing, and mucus that lasts about three months for at least two years. Cilia, which look like hair fibers, line up the bronchial tubes and assist in clearing out the mucus.
You tend to lose the cilia if you develop chronic bronchitis. This makes it more difficult to cough up mucus, which causes you to cough even more and result in more mucus production.
Chronic Obstructive Pulmonary Disease Risk Factors
Some of the risk factors that can contribute to COPD are;
Tobacco smoke exposure: Prolonged cigarette smoking is the major risk factor for COPD. The higher the risk, the longer you smoke and the more packs you smoke. People who smoke pipes, cigars, or marijuana, including those exposed to a lot of secondhand smoke, might be at risk.
Asthmatic people: Asthma, which is a chronic inflammatory air passage disorder, could put you at risk for COPD. Both asthma and smoking together raise the risk of COPD considerably higher.
Dust and chemical exposure in the workplace: Chemical fumes, specks of dust, and vapors in the workplace can cause inflammation and irritation of the lungs over time.
Fumes from burning fuel exposure: People in impoverished areas who are exposed to burning fumes from cooking and heating in houses that are poorly ventilated are more likely to acquire COPD.
Genetics: Other cases of COPD are caused by the rare genetic condition called alpha-1-antitrypsin deficiency. Some smokers are likely to be more vulnerable to the disease due to other genetic reasons.
Chronic Obstructive Pulmonary Disease Diagnosis
COPD is a disease that is frequently misdiagnosed. Most persons with COPD do not receive a diagnosis until the disease progresses. To detect the disease, the physician will ask for your signs and symptoms, review your family as well as medical history. They will also talk about any lung irritants you have been exposed to, particularly cigarette smoke.
The physician might also request one or more tests such as;
- Chest x-ray: Emphysema, which is one of the most common causes of COPD, can be seen on a chest x-ray. Other lung diseases or heart failure can also be ruled out using an X-ray.
- CT scan: This is a type of x-ray that doctors use to scan the lungs for emphysema diagnoses and assess whether you would benefit from COPD surgery. Lung cancer can also be detected with CT scans.
- Tests of lung (pulmonary) function: Doctors use these tests to determine how much air you can breathe in and breathe out. It also helps identify whether your lungs are supplying your blood with enough oxygen. The most frequent test, spirometry, involves blowing into a big tube attached to a small device. This is to determine how much air your lungs can retain and how quickly you can blow it out.
- Blood gases in the arteries analysis: This form of blood test determines how well the lungs transport oxygen and remove carbon dioxide from the blood.
- Lab test: Although lab tests aren’t recommended for diagnosing COPD, they can help you figure out what's causing the symptoms or even rule out alternative possibilities. Lab testing, for example, may be done to detect if you have alpha-1-antitrypsin deficiency. This is a hereditary condition that can lead to COPD in other people.
Chronic Obstructive Pulmonary Disease Treatment
Chronic obstructive pulmonary disease treatments options can help relieve the symptoms, avoid complications, and reduce the progression. The physician can thus recommend one or a combination of the following treatment options;
Medication:
Medications can help to alleviate symptoms and decrease flare-ups. However, it might take several trials and errors to find the right drug and dosage for you here. Here are some of the available options;
- Bronchodilators
These are drugs that relax the muscles around the air paths and are commonly available in inhalers. They can help ease coughing and shortness of breath, as well as making breathing much easier. You might require a short-acting bronchodilator prior to an activity, a long-acting bronchodilator each day, or even both. This depends on the severity of the condition.
- Inhaled steroids
Inhaled corticosteroid medicines can help avoid exacerbations by reducing inflammation of the airway. Bruising, hoarseness and oral infections are all possible side effects. On the other hand, these drugs are beneficial to those who suffer from COPD exacerbations regularly.
- Phosphodiesterase-4 inhibitors
These are a type of drug that can come in the form of a tablet to help with inflammation and airway relaxation. It's usually given to people who have severe COPD and chronic bronchitis.
Other chronic obstructive pulmonary disease medications include;
- Theophylline
- Oral steroids
- Combined inhalers
- Antibiotics
Additional therapies:
The doctor can recommend more therapies to treat patients with moderate and severe OCPD. They include;
- Oxygen therapy
Supplemental oxygen may be required if there is insufficient oxygen in the bloodstream. There are various machines that supply oxygen to the lungs. They include lightweight and portable units one may carry around.
- Program for pulmonary rehabilitation
Pulmonary rehabilitation programs usually include a combination of exercise, education, nutrition recommendations, and counseling. You will work with a number of professionals who will customize your rehabilitation program to your specific needs.
Quit smoking:
The most important approach in any COPD treatment regimen is to stop smoking. Smoking cessation can help prevent COPD from worsening and limiting the capacity to breathe. However, quitting smoking is generally a difficult task, and the process may be overwhelming. You can thus ask your medical provider for assistance.
Surgical procedures:
Surgery may sometimes be an alternative for patients with severe emphysema who are not getting enough relief from other treatments. The standard surgical options include the following:
Surgery to reduce the volume of the lungs: The neurosurgeon can take out small wedges of the lung tissue that is damaged from the upper lungs during this procedure. This frees up space in the chest cavity, allowing your remaining healthy lung tissue to expand while the diaphragm functions more effectively.
Lung transplantation: For some patients who meet certain criteria, lung transplantation might be an alternative. This could help you breathe better and be more active. On the other hand, it is a major procedure with severe dangers, including organ rejection. Besides, you will be required to take immune-suppressing drugs for the rest of your life.
Conclusion
Chronic obstructive pulmonary disease is mostly referred to as OCPD, a collection of progressive lung disorders. Emphysema and chronic bronchitis are the most frequent of these disorders. However, both of these disorders are common in most patients with COPD.
COPD is a prevalent lung disease that primarily affects middle-aged and older smokers. Most people are completely unaware that they have it. Additionally, breathing problems tend to worsen over time and limit your typical activities, while treatment can help you stay in control.