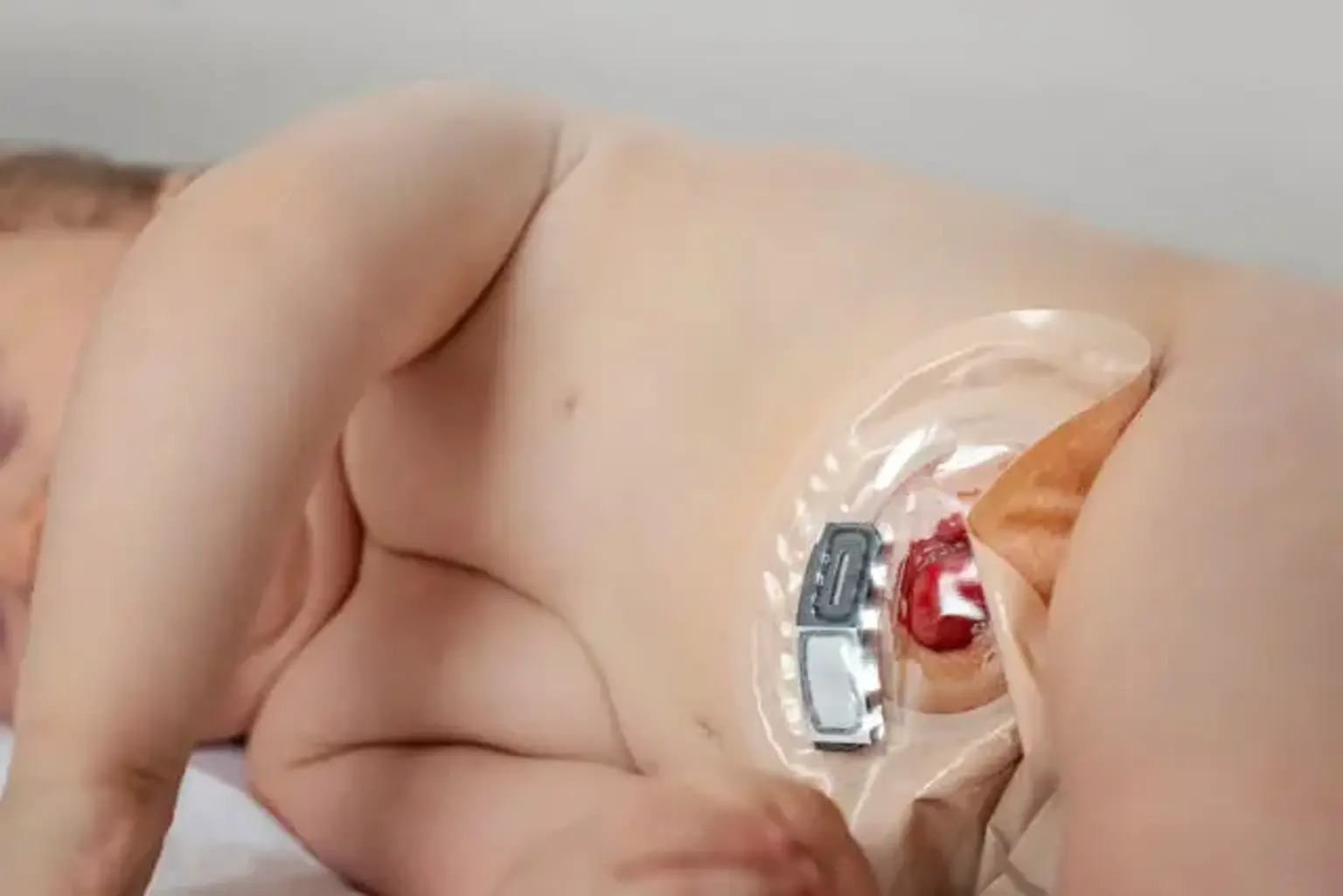
Colostomy Closure
Overview
A colostomy is a surgical operation that produces an opening (stoma) in the large intestine (colon). The healthy end of the colon is drawn through an incision in the front abdominal wall and sutured into place to make the opening. This aperture, which is frequently used in combination with a connected ostomy device, provides an alternate route for feces to exit the body. Thus, if the natural anus is unable to perform that role (for example, if it has been removed in the fight against colorectal cancer or ulcerative colitis), an artificial anus steps in. Depending on the conditions, it may be reversible or permanent.
The intestinal stoma is now regarded one of the most common life-saving emergency surgeries performed worldwide. It can be used to treat a variety of benign and malignant gastrointestinal diseases as an emergency or elective procedure. More than 130.000 intestinal stomas are implanted in the United States each year to treat disorders such as inflammatory bowel disease, radiation injury, colonic diverticulitis, and fecal incontinence. Although intestinal stomas are considered life-saving surgeries, they are accompanied with a number of complications.
A colostomy reversal, also known as a colostomy takedown, is a reversal of the colostomy process by which the colon is reattached by anastomosis to the rectum or anus, providing for the reestablishment of flow of waste through the gastrointestinal tract.
Indications for the surgery include patient pain or discomfort caused by the colostomy, frequent skin breakdown or infection, and herniation at the colostomy site. The technical aspects of the surgery depend on the amount of remaining colon and rectum.
Anatomy and physiology of the intestine
The large bowel begins in the cecum and ascends to the ascending colon with the hepatic flexure, transverse colon with the splenic flexure, descending colon, and sigmoid colon. As the substance passes through the colon, it becomes firmer due to water and electrolyte absorption in the large bowel.
The sigmoid colostomy is the most common kind of colostomy, followed by the transverse colostomy, whereas ascending and descending colostomies are uncommon and seldom done.
Colostomies are classified into three types: loop colostomy, double-barrel colostomy, and end colostomy. The many forms of colostomies are designed based on the indication, the length of the mesocolon, and the quantity of sick and normal bowel left.
The effluent content varies from soft and loose, foul-smelling, oatmeal-like feces in ascending and transverse colostomies to stiffer, paste-like stool from transverse and descending colostomies to output matching regular stool from a sigmoid colostomy. The output becomes simpler to handle as the feces firmens down the colon.
Colostomies are usually performed in the anterior abdominal wall, above the rectus abdominis muscle, on either side of the linea alba, and often inferior to the umbilicus. The location is occasionally cephalad to the umbilicus, especially in obese persons, since the anterior abdominal wall contains less subcutaneous fat in the higher half. A circular incision is made over the pre-identified stoma location during the surgery. To achieve a secure seal of the stoma appliance, it requires a level surface on the abdomen of at least 2 to 3 inches and should be distant from the beltline, any scars, and bony prominences. The incision is deepened onto the anterior rectus sheath, which is cruciately incised.
The rectus muscle is retracted sideways without cutting into the muscle, and the posterior rectus sheath is incised in a cruciate fashion once more. The designated loop of bowel for stoma formation is dragged through the incision and exteriorized onto the skin. The identification of the bowel is helped by doing a diagnostic laparoscopy to guarantee adequate mobility and tension-free access to the front abdominal wall.
The stoma can, however, be established with a trephine without the need of a laparoscopic method. Cross-sectional imaging should be used to determine the most movable part of the intestine and label the colostomy site accordingly. A transverse colostomy should be created in the left upper quadrant, and a sigmoid colostomy should be created in the left iliac fossa.
Once the mesocolon has been exteriorized, a stoma rod can be pushed through it to limit the possibility of retraction into the abdominal cavity. The colon is incised three-quarters of the way around, and the bowel margins are sutured to the skin with interrupted sutures made of absorbable suture material, slightly increasing the stoma above the skin level. Colostomies, unlike ileostomies, typically do not necessitate eversion and 3-point fixation because to the content's lower enzymatic activity.
Why a Colostomy is performed?
The indications of a colostomy are divided on the basis of the type of colostomy:
- A double-barrel colostomy is a kind of colostomy performed following bowel resections involving the mesentery and is used in diseases such as colorectal cancer, gangrenous bowel segment resection, inflammatory bowel disease, penetrating bowel injuries, or gangrenous sigmoid volvulus resection.
- In cases of penetrating abdominal injury, colorectal cancer, intraoperative bowel injury, perineal injury, diverticular disease with obstruction, blunt abdominal injury, protection of a distal anastomosis, anal incontinence or perineal injury, Fournier gangrene involving the perianal region, and perianal fistulas, a loop colostomy may be performed. They may also be performed as a temporary emergency intervention in the newborn population in cases of anorectal abnormalities or Hirschsprung disease before corrective surgery can be undertaken.
- After the Hartmann surgery, the most frequent form of colostomy is an end colostomy. In cases of gangrenous sigmoid volvulus, colorectal cancer following abdominoperineal resection, ileo-sigmoid knotting, penetrating abdominal injury, ulcerative colitis, intussusception, anastomotic leak, anorectal cancer, and perineal injury, it is performed. It entails closing the distal portion and attaching it to the abdominal wall. Stomal closure in this circumstance necessitates midline exploration and is thus least recommended when colostomy is planned as a temporary remedy and there is a suitable distal segment, which is an uncommon occurrence.
Types of Colostomy
Types of colostomy include:
- Loop colostomy: This is a big and temporary stoma that is mainly utilized in emergencies. A bowel loop is dragged out onto the belly and kept in place using an external device. The intestine is then sutured to the abdomen, and two holes are established in the same stoma: one for feces and one for mucus.
- End colostomy: A stoma is formed from one end of the colon. The remainder of the intestine is either excised or stitched up (Hartmann's operation).
- Double barrel colostomy: Both ends of the bowel are brought out onto the belly after it has been cut. Only the proximal stoma is operational. A double-barrel colostomy is often a temporary colostomy with two holes into the colon (distal and proximal). The proximal stoma is used for elimination.
Colostomy surgery that is scheduled typically has a greater long-term success rate than surgery that is performed in an emergency.
Contraindications of Colostomy
There are no contraindications to colostomy creation. They are frequently required when anastomosis cannot be achieved due to the emergency nature of the surgery or when the patient is malnourished with low serum albumin and protein levels. Similarly, when there is an insufficient length of bowel or mesentery following resection, or when there is the possibility of excessive tension at the anastomosis site.
Colostomy care is required in all cases of colostomy. Some procedures, such as irrigation or enema, should be avoided in cases of stoma prolapse, chemotherapy, pelvic or abdominal radiation treatments, diarrhea-producing medication, or an irregularly functioning stoma, as they may lead to dependence.
Preoperative evaluation before undergoing Colostomy reversal
Contrast Enema:
Prior to ileostomy closure, anastomotic integrity must be evaluated; however, there is no clear consensus on the optimum assessment technique. To assess anastomotic integrity, a water-soluble contrast enema is routinely utilized. In the diagnosis of clinically severe anastomotic issues, contrast enema has been shown to have high specificity (95.4%) and negative predictive value (98.4%).
Because digital rectal examination is closely associated with contrast enema results, many clinicians believe contrast enemas are not a required addition to clinical evaluation in patients with a low simple anastomosis.
Similarly, on contrast enema, a single-center retrospective evaluation of 81 patients with low rectal cancer who had low anterior resection with diverting stoma found a 3.7 % anastomotic leak rate and a 5.8 % subclinical leak rate. Because the total leak rate is modest, the authors believe that contrast enema should not be used routinely for preoperative examination prior to stoma reversal.
Clinical Examination:
Prior to ileostomy closure, digital rectal examination is a good adjuvant for identifying anastomotic disruption, stricture, or blockage and should be conducted frequently in conjunction with endoscopic assessment of the anastomosis. A prospective cohort research evaluated digital rectal examination and water-soluble contrast enema results in 129 patients with coloanal/colorectal anastomosis or ileal pouch–anal anastomosis at 3 to 6 weeks postoperatively.
They reported a false-positive rate of 6.4 % (normal digital rectal examination with abnormal contrast enema) and a false-negative rate of 3.5 % (normal contrast enema with obviously abnormal digital rectal examination). Digital rectal examination has a sensitivity of 98.4 % in detecting anastomotic disease, and in expert hands, it may provide more meaningful clinical information than a contrast enema.
Similarly, if proctoscopy and digital rectal examination are normal, contrast enema does not give extra information, according to a retrospective analysis.
Persistent anastomotic leak:
Some anastomotic leaks never entirely resolve, resulting in a chronic anastomotic sinus seen on contrast enema. A small case study of 8 individuals with chronic anastomotic sinuses found that sinus tracts that last more than a year are unlikely to recover. Patients with subclinical anastomotic sinuses had effective stoma closure; however, patients with symptomatic chronic anastomotic sinuses connected with a cavity may not be candidates for reversal.
A posterior midline sinus found on contrast enema can be opened using electrocautery or a laparoscopic linear cutting stapler to separate the luminal-cavity septum and enable cavity drainage. Secondary intention prior to stoma closure may aid in the repair of a chronic anastomotic sinus. In a study of 163 patients who had low anterior resection with diverting loop ileostomy, 11 of 16 patients who had a persistent anastomotic leak on contrast enema had stoma closure, and 2 (19%) of these patients experienced postoperative anastomotic problems.
Despite radiographic evidence of leakage, many clinicians believe that morphological patterns of leaking on contrast enema may impact patient selection for ileostomy closure. However, it is recommended that all efforts be made to establish sinus closure prior to stoma reversal. Curettage, fibrin glue instillation, and advancement procedures are all options.
How is a stoma reversal done?
A stoma reversal is performed after the original surgery has healed. This normally takes between 6 and 8 weeks. However, in extreme cases, it might take up to a year. The stomach and anal muscles must be engaged for the reversal to work correctly.
The doctor reattaches the bowel's split ends. Stitching or stapling is used to heal the bowel. Stitches are then utilized to seal the stoma-affected portion of the belly.
The type of stoma reversal is determined on the type of ostomy surgery you had. One method entails creating a huge cut (incision). This method of recovery is more time consuming. In the other kind, smaller incisions are employed. Healing takes less time.
What can you expect after a stoma reversal?
It is typical to experience issues with bowel function following a stoma reversal. This is due to the removal of a portion of the bowel. Loose stools, incontinence, abrupt bowel urges, and discomfort are all possible signs. Other dangers include stomach infection and intestinal obstruction or scar tissue.
The patient may need to take the same precautions as he did following his ostomy. Bending, hard lifting, and other physical activities will be discouraged. The doctor will be able to advise when it is safe to resume normal activities and habits, such as driving. This might take several weeks or months.
Caring for yourself at home
- The doctor may recommend things; the patient can do at home to help improve bowel works. The patient may be told to:
- Change the diet.
- Eating small, frequent meals.
- Drinking plenty of fluids.
- Maintain a food diary: As the gut heals, the patient may consult with a dietician to determine which meals are best. Walking or pelvic floor exercises may be suggested by the doctor. They may aid in the improvement of bowel function. The patient may also take anti-diarrhea medications or use lotions to relieve pain.
- Coping with bowel issues: Coping with bowel issues can be difficult. Many people experience embarrassment or frustration at times. However, your medical team can assist you. They can assist you in seeking aid and learning coping strategies.
- Follow-up care is an essential component of the therapy and safety.
Recovery period after Colostomy reversal
The patent will usually stay in the hospital for 3 to 10 days and leave after bowel movements start and if there are no complications.
Conclusion
A colostomy is a surgical procedure that creates a hole (stoma) in the large intestine (colon). To create the opening, the healthy end of the colon is dragged through an incision in the front abdominal wall and sutured into place. This opening, which is usually utilized in conjunction with a linked ostomy device, allows excrement to escape the body via a different path. As a result, if the natural anus is unable to perform that function (for example, if it has been removed in the battle against colorectal cancer or ulcerative colitis), an artificial anus takes its place. It may be reversible or permanent, depending on the circumstances.
After the original surgery has healed, a stoma reversal is performed. Normally, this takes between 6 and 8 weeks. In severe circumstances, though, it might take up to a year. For the reversal to operate properly, the stomach and anal muscles must be engaged.
In pediatric surgery, ostomy closure is a common elective treatment. Despite the advantages for the child, problems such as anastomotic leak, postoperative ileus, bowel blockage, enterocutaneous fistula, and, most often, surgical site infection are associated with this surgery. Furthermore, many temporary stomas may not be reversed due to surgical complications, adjuvant treatment, or prohibitive comorbidities.
Diverticulitis, colon cancer, and inflammatory bowel disease are all commonly treated with temporary stomas. These temporary stomas are used to try to prevent septic consequences from anastomotic leakage and avoid reoperation. Stomas can be reversed if acute medical problems have improved and the anastomosis has been demonstrated to be healed.
Prior to reversal, the anastomosis is evaluated using contrast enemas, digital rectal examination, and endoscopic assessment. Complications of stoma reversal include anastomotic leak, postoperative ileus, intestinal blockage, enterocutaneous fistula, and, most often, surgical site infection. Furthermore, many temporary stomas may not be reversed due to surgical complications, adjuvant treatment, or prohibitive comorbidities.
However, there is no consensus in the literature on preoperative mechanical bowel cleansing, the period of pre- and postoperative antibiotic treatment, the administration of regular nasogastric (NG) decompression, and the timing of postoperative oral feeding beginning in these patients. As a result, the approach to these challenges is determined by the preferences of the attending surgeons.