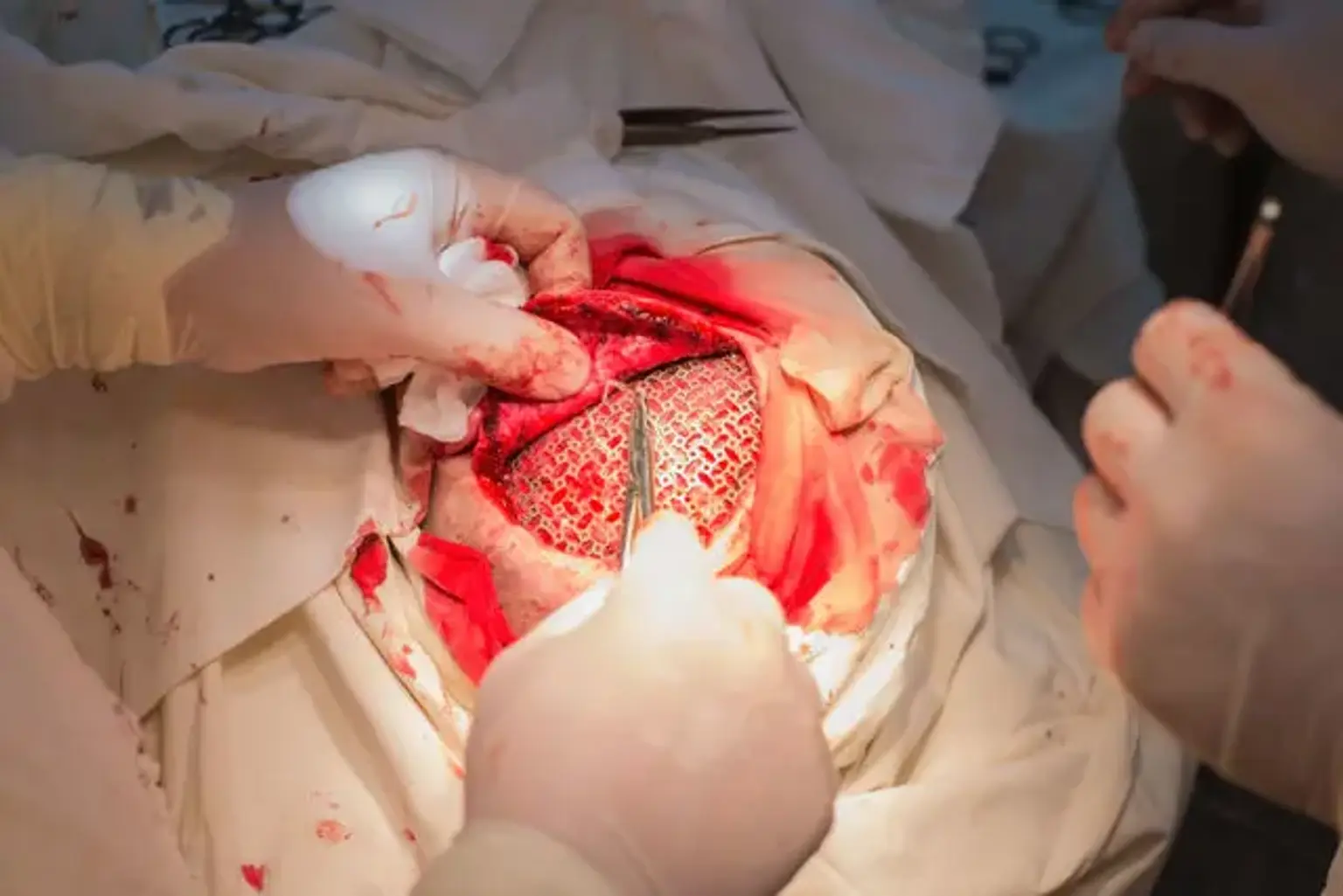
Craniotomy
Overview
A craniotomy is a surgical procedure that involves temporarily removing a portion of the skull in order to expose the brain and perform an intracranial surgery. Brain tumors, aneurysms, arterio-venous malformations, subdural empyemas, subdural hematomas, and intracerebral hematomas are among the most frequent disorders that may be treated using this method.
Specialized tools and equipment are used to remove the bone flap, which is a portion of bone. The bone flap is removed temporarily, held at the surgical instrument table, and then replaced when the brain operation is completed.
The bone can be discarded, kept in the abdomen subcutaneous area, or cryopreserved under cold storage conditions in some situations, depending on the etiology and indication for the treatment. The technique is known as a craniectomy if the bone flap is discarded or not put back into the skull during the same operation.
From a historical point of view, cranial procedures varied from a single burr hole trephine to a major craniectomy. A succession of burr holes are connected to execute modern craniotomies. Despite the fact that trephination is the oldest cranial surgical technique, with ancient reports dating back 2300 years, our current modern surgical technique for a craniotomy is the final cured result of the procedure introduced at the end of the 19th century by the self-educated surgeon Wilhelm Wagner.
Some craniotomy techniques can be aided by neuronavigation guidance based on magnetic resonance imaging or computed tomographic scans to customize the surgery to the size of the tumor using the smallest incision feasible, depending on the kind of brain lesion, pathology, and surgical strategy.
Neuronavigation is a contemporary computerized tool that can assist surgeons in more accurately localizing disease by combining a number of craniofacial sites in the patient. Neuronavigation improves navigation by providing improved guidance, orientation, and localisation. It gives the surgeon more confidence and results in a better outcome for the patient.
Types of Craniotomy
1. Extended Bifrontal Craniotomy:
The extended bifrontal craniotomy is a classic skull base method for targeting tough malignancies at the front of the brain. It is predicated on the idea that it is safer to remove superfluous bone than to modify the brain needlessly.
The extended bifrontal craniotomy procedure entails creating an incision behind the hairline in the scalp and removing the bone that creates the shape of the orbits and the forehead. At the conclusion of operation, this bone is replaced. By temporarily removing this bone, surgeons can work in the region between and directly behind the eyes without having to handle the brain.
The extended bifrontal craniotomy is often utilized for malignancies that are not candidates for removal using minimally invasive techniques due to the architecture of the tumor, potential pathology of the tumor, or surgical aims.
Meningiomas, esthesioneuroblastomas, and malignant skull base tumors are among the cancers treated with the extended bifrontal craniotomy.
2. Minimally Invasive Supra-Orbital “Eyebrow” Craniotomy:
Supra-orbital craniotomy (sometimes known as "eyebrow" craniotomy) is a surgery for removing brain malignancies. Neurosurgeons use this surgery to reach malignancies at the front of the brain or around the pituitary gland, which is deeper in the brain behind the nose and eyes, by making a tiny incision inside the brow. When a tumor is exceedingly big or near to the optic nerves or important arteries, this method is employed instead of endonasal endoscopic surgery.
Because it is a minimally invasive procedure, supra-orbital “eyebrow” craniotomy may offer:
- Less pain than open craniotomy
- Faster recovery than open craniotomy
- Minimal scarring
- The supra-orbital craniotomy may be part of the treatment for Rathke’s cleft cysts, skull base tumors and some pituitary tumors.
3. Retro-Sigmoid “Keyhole” Craniotomy:
Retro-sigmoid craniotomy (also known as "keyhole" craniotomy) is a minimally invasive surgery used to remove brain tumors. This technique removes skull base tumors by a tiny incision behind the ear, allowing access to the cerebellum and brainstem. This method may be used by neurosurgeons to access cancers such as meningiomas, auditory neuromas (vestibular schwannomas), skull base tumors, and metastatic brain tumors.
The advantages of a "keyhole" craniotomy include less discomfort after the treatment than an open craniotomy, less scarring, and a faster recovery.
4. Orbitozygomatic Craniotomy:
A typical skull base approach used to target challenging tumors and aneurysms is the orbitozygomatic craniotomy. It is predicated on the idea that it is safer to remove extra bone than to manipulate the brain unnecessarily.
Typically reserved for lesions that are too difficult to be removed using less invasive methods, orbitozygomatic craniotomy entails creating an incision in the head beneath the hairline and removing the bone that creates the shape of the orbit and cheek. At the conclusion of operation, this bone is replaced. By removing this bone temporarily, surgeons may access deeper and more challenging portions of the brain while limiting brain damage.
Craniopharyngiomas, pituitary tumors, and meningiomas are some of the brain cancers that can be treated using orbitozygomatic craniotomy.
5. Translabyrinthine Craniotomy:
A translabyrinthine craniotomy is a surgical technique that includes creating an incision behind the ear in the head and then removing the mastoid bone and portion of the inner ear bone (specifically, the semicircular canals which contain receptors for balance). The surgeon next locates and removes the tumor, or as much of it as feasible without causing significant brain damage.
When there is no functional hearing or when hearing must be compromised, the translabyrinthine technique is frequently explored for acoustic neuroma excision. The semicircular canals of the ear are excised during the translabyrinthine craniotomy to get access to the tumor. The removal of the semicircular canals results in total hearing loss.
Although hearing is lost with the translabyrinthine craniotomy, the risk of facial nerve injury may be reduced.
Indications of Craniotomy
Several conditions necessitate the opening of the skull for diagnosis and treatment. The following are the most prevalent indications for a craniotomy:
- Brain aneurysm.
- Vascular malformations (arterio-venous malformation, cavernous angioma, arterio-venous fistula).
- Brain tumors (meningioma, high-grade and low-grade glioma, epidermoid, ependymoma, oligodendroglioma, metastases).
- Orbital tumors.
- Pituitary adenomas.
- Cerebellopontine angle tumors.
- Pain treatment (microvascular decompression).
- Brain abscess.
- Subdural empyema.
- Hematomas (intracerebral, epidural, subdural).
- Decompressive.
- Lobectomy.
- Epilepsy surgery.
- Craniosynostosis.
- Depressed skull fractures.
- Intracranial foreign bodies.
- Cerebrospinal fluid leak repair.
Contraindications of Craniotomy
There are just a few contraindications to undergoing a craniotomy, and the most are connected to the patient's overall health:
- Advanced age.
- Poor functional status.
- Severe cardiopulmonary disease.
- Severe systemic collapse (sepsis, multiorgan failure).
- Pathologies that can be addressed by a single burr hole.
- Altered preoperative coagulation parameters.
- Bleeding disorders.
Preoperative preparation before undergoing Craniotomy
- Your doctor will explain the operation to you, and you will have the opportunity to ask questions.
- You will be asked to sign a consent document authorizing the procedure. If something is unclear, read the form carefully and ask questions.
- In addition to a thorough medical history, your doctor will do a physical check to verify you are in excellent health prior to surgery. Blood testing and other diagnostic procedures may also be required.
- You will be given a preoperative neurological assessment, which will be compared to postoperative exams.
- Before the procedure, which normally takes place after midnight, you will be advised to fast.
- Inform your healthcare practitioner if you are pregnant or suspect you are pregnant.
- Inform your doctor if you are sensitive or allergic to any medications, latex, tape, or anesthetic agents (local or general).
- Inform your doctor about all medications (prescription and over-the-counter) and herbal supplements you are using.
- If you have a history of bleeding problems or are using any anticoagulant (blood-thinning) medications, aspirin, or other medications that impact blood clotting, tell your doctor. It may be required for you to discontinue certain medications prior to the surgery.
- If you smoke, you should quit as soon as possible before the treatment to increase your chances of a good recovery and to enhance your general health.
- The night before the procedure, you may be requested to wash your hair with a special antibacterial shampoo.
- Before the operation, you may be given a sedative to help you relax.
- Shaving will be performed on the regions surrounding the surgery site.
- Your doctor may suggest further preparation based on your medical condition.
- Routine preoperative antibiotics are given prior to the surgery to prevent wound infection, along with any additional drugs that may be required, such as anticonvulsant medications or corticosteroids.
- The first configuration of equipment such as the neuronavigation system, surgical microscope, and neuromonitoring is completed. The availability of an intensive care unit should be considered prior to surgery, as most patients require this level of care following a craniotomy.
How Craniotomy is performed?
Once the patient is sedated, the right posture of the head is determined based on the method to be used. It is critical to avoid pressure points on susceptible body parts by cushioning thoroughly throughout. The position of the craniotomy incision is determined by the portion of the brain to be operated on. Anatomical points are confirmed before the incision if the surgical craniotomy is aided with neuronavigation.
Incisions in the supratentorial region are often done across the frontal, temporal, parietal, or occipital bones, or a combination of these bones. The incision for infratentorial surgery is normally done over the rear region of the head below the transverse sinus.
The hair in the area can be shaved after finding the optimal location for the incision on the skin. The incision should be done beneath the hairline for cosmetic reasons. Following incision confirmation, the surgical region is washed with the appropriate antiseptic solution, followed by standard sterile draping procedures. A local anesthetic including epinephrine is routinely injected into the required skin incision to help with hemostasis.
Following the skin incision, the muscles behind the scalp are dissected to reveal the skull. Retractors can be put on the incision's borders to provide proper exposure to the operative region. Sutures or fish hook retractors can also be utilized to retain the scalp flap in place.
If necessary, the pericranium can be detached and utilized as a dural replacement during the closure. The craniotome or cranial drill is used to make many burr holes in the skull. To avoid inserting the craniotome into brain tissue, extreme caution must be exercised.
Any bone fragments are removed from the perforations, and the dura is divided using a Freer elevator or Penfield dissector. A craniotome saw is used to join the burr holes, and a bone flap is elevated after carefully separating it from the dura mater below. The bone flap is kept in place on the surgical instrument table until the surgery's closing phase. The dura is sliced and retracted to expose the brain during the intradural operation.
After the brain surgery, the bone is reattached in place with plates and screws. Before sealing the scalp, adequate hemostasis should be accomplished. The scalp is sutured in anatomical layers once the overlaying tissues are reattached. A subdural or subgaleal drain can be left in place to drain the collected blood products, depending on the surgeon's discretion.
What happens after a Craniotomy?
You are brought to a recovery room immediately following a craniotomy for monitoring while the anesthetic wears off. Your vital signs will be monitored while the breathing tube is withdrawn (extubation). When you are completely conscious, you are sent to the intensive care unit (ICU) for additional monitoring and treatment, such as blood and intracranial pressure control, nourishment, temperature, oxygen levels, and pain management.
A neurological exam is performed on a regular basis to look for early indicators of difficulties, such as decreased consciousness, seizure, stroke, or cerebral hemorrhage.
The majority of individuals endure pain following brain surgery. Narcotics (such as morphine, fentanyl, or hydromorphone), acetaminophen (Tylenol), muscle relaxants (such as methocarbamol, diazepam, or tizanidine), or steroids are used to treat such pain (for example, dexamethasone). High blood pressure, nausea, vomiting, and/or shivering are all possible side effects that can be treated with drugs and blankets or air-warming equipment.
You are moved to the normal hospital ward after a few days, or after your condition has stabilized. For a short amount of time, oxygen may be necessary. To avoid lung infection, the medical team will give you deep breathing techniques . Getting out of bed and walking as tolerated is suggested, and you may be requested to work with a physical therapist. The entire hospital stay may range from a few days to weeks, depending on the intricacy of the procedure.
You should follow the instructions given to you by your surgeon at home. A follow-up appointment may be scheduled within the next 1 to 2 weeks of discharge. During your recovery, you may experience difficulties with walking, speech, strength, and balance. Headaches that feel like they're pulsing or hammering are typical and can last for months following surgery.
Avoid high-intensity activities in general, keep the incision site clean, and take pain medication as indicated. Consult your doctor about when you will be able to return to work. It is possible that you will be unable to return to work for several weeks.
You should follow the following recommendations during your daily activities:
- Avoid strenuous activity (for example, lifting heavy items, jogging, sex)
- Avoid risky activities that require your attention (for example, driving)
- Do not drink alcohol or use nicotine products (for example, smoking, vaping)
- Try to walk 5 to 10 minutes per day, and gradually increase this time as you recover
- Sleep with your head elevated and apply ice 3 times per day for 15 minutes to reduce pain and swelling, if needed
- Drink water and eat foods high in fiber (for example, beans, whole grains, nuts, berries) to resolve constipation caused by the narcotics used for pain control during or after surgery.
Postoperative complications of Craniotomy
Bacterial or viral meningitis affects roughly 0.8 to 1.5% of people who have craniotomy. Postcraniotomy discomfort is common and ranges from mild to severe. This discomfort has been managed with scalp infiltrations, nerve scalp blocks, parecoxib, and morphine, with the last being the most successful in giving analgesia.
At least 40% of patients become sensitive to at least one illness, resulting in more interrelated risk factors. There have been reports of infections starting from the moment of operation, skin incursion, hematogenous seeding, or retrograde infections.
Pre-shunt related infections, post-operative CSF leakage, lack of experience from the neurosurgeon, preterm birth/young age, advanced age, shunt revisions for malfunction, and neuroendoscopes are all linked with an increased risk of meningitis.
The manner in which shunts are placed on each patient is significantly dependent on the cleanliness of the location. When bacteria enter the CSF space, the procedure becomes more complicated.
What is the recovery outlook?
Within 2 to 3 months after a craniotomy, the bone flap will heal and partially fuse back into the rest of the skull bone. Full healing might take many months, depending on the underlying condition addressed.
Conclusion
The craniotomy surgical procedure has become one of the most important operations in modern neurological treatment. Many patients were unable to endure conditions that are now treated on a regular basis prior to the development of this treatment. Brain tumors, vascular diseases, and trauma are frequently treated, which may result in serious injury to the patient if access to the cerebral space was limited.
The technique itself has been upgraded and will continue to do so when new technology is created. It has resulted in a revolution in neurosurgical and neurological patient care since its inception.
If a craniotomy is required for the patient, it is determined based on the specific type of disease to be addressed and the physician's clinical assessment. Despite the introduction of novel endovascular procedures for treating intracranial vascular problems and radiosurgery for treating intracranial malignancies, craniotomy remains the principal technique for treating the vast majority of neurosurgical disorders.
A craniotomy may be performed for a variety of reasons, including the treatment of brain tumors, the clipping or repair of an aneurysm, taking blood or blood clots out of a leaky blood vessel, surgical removal of an arteriovenous malformation (AVM) or treatment of an arteriovenous fistula (AVF), A brain abscess is being drained, repairing fractures in the skull, and reducing intracranial pressure (ICP) involves removing injured or enlarged parts of the brain caused by traumatic injury or stroke .
Complications are possible with any surgical procedure. The risk of brain surgery is linked to the exact area in the brain that will be affected by the procedure. If the part of the brain that controls speech is operated on, for example, speech may be impacted. Infection, bleeding, blood Clots, pneumonia, unstable blood pressure, seizures, muscle weakness, brain enlargement, leakage of cerebrospinal fluid, and risks associated with the use of general anesthesia are some of the more general consequences.