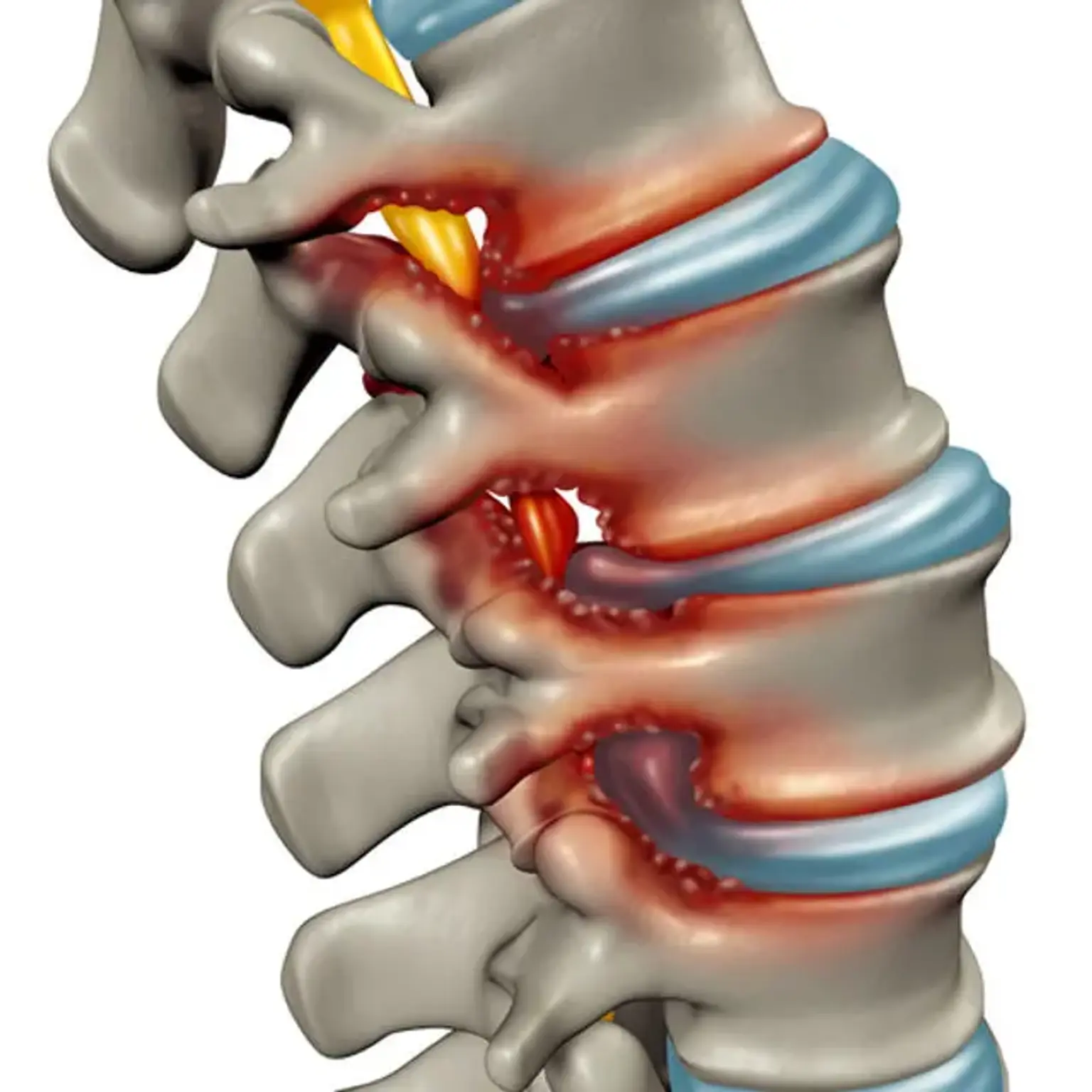
Degenerative Disk Disease
Overview
The intervertebral discs are pads of fibrocartilage-based structures that offer support, flexibility, and small load-sharing between each vertebral body of the spine. These are essentially made up of two layers: a soft, pulpy nucleus pulposus on the inner of the disc and a solid structure around it called the annulus fibrosus.
A disturbance in the normal construction of these circular discs can result in a disc herniation or a protrusion of the inner nucleus pulposus, potentially putting pressure on the spinal cord or nerve root and causing radiating pain and particular areas of paralysis.
More than 90% of herniated discs occur in the L4-L5 or L5-S1 disc spaces, impinging on the L4, L5, or S1 nerve roots. Radiculopathy into the posterior leg and dorsal foot is caused by this compression.
If the disc damage advances to the point of neurologic impairment or limits in everyday activities, surgical intervention to decompress and stabilize the afflicted segments may be indicated. If no motor impairments exist, a nonoperative regimen of analgesics, activity reduction, and injections should be tried for many months. The surgical outcomes for sciatic pain that has not responded to conservative therapy are predictable and excellent.
Degenerative disc disease definition
One of the most prevalent reasons of low back and neck discomfort, as well as one of the most misunderstood, is degenerative disc disease. Degenerative disc disease, in a nutshell, refers to symptoms of back or neck discomfort produced by wear and tear on a spinal disc. Degenerative disc disease can also produce weakness, numbness, and hot, shooting sensations in the arms or legs in some people. Degenerative disc disease is characterized by low-level chronic pain interspersed with periods of more acute pain.
The word degenerative indicates, naturally, that problems would worsen with age. However, the name does not refer to the symptoms, but rather to the mechanism through which the disc degrades over time.
Degenerative disc disease, contrary to its name, is not a disease, but rather a condition in which normal, age-related wear and tear on a disc produces discomfort, instability, and other symptoms. This illness does not generally result in long-term impairment, and the majority of cases may be handled non-surgically.
While disc degeneration is expected to worsen with time, the pain from degenerative disc disease normally does not worsen and, in fact, usually feels better given enough time. This mechanism is explained by the degenerative cascade theory.
Epidemiology
Because most intervertebral disc degenerations are asymptomatic, determining the real prevalence is challenging. Furthermore, because of the lack of consistency in the criteria of disc degenerations and disc herniations, it is impossible to compare the true prevalence of the condition.
The reported disc abnormalities at any level in a meta-analysis of 20 studies evaluating the magnetic resonance imaging (MRI) of asymptotic individuals were: 20% to 83 percent for a reduction in signal intensity, 10% to 81 percent for disc bulges, 3% to 63 percent for disc protrusion, 3% to 56 percent for disc narrowing, and 6% to 56 percent for annular tears.
Etiology
The progression of disc degeneration is directly proportional to the patient's age. Interestingly, while males are considered to begin this degeneration nearly 10 years sooner than women, women with disc degeneration are likely to be more vulnerable to the consequences such as malalignment and instability
Traditional theories on the etiologies of disc degeneration, extending back to the early 1990s, concentrated on environmental exposures such as smoking, vehicle vibration, and employment. More recent research has highlighted the genetic components linked with disc disease and moved the paradigm away from the aforementioned social, occupational, and environmental aspects.
The current agreement emphasizes the relevance of these genetic variables as the most important predictors of disc degeneration, with environmental influences acknowledged as additional, small contributions to disease initiation. The consequences of smoking have also been called into doubt, with current study indicating relatively modest connections between cigarette usage and disc disease.
Similarly, while occupational variables (e.g., hard lifting, forceful bending) may have a role in lumbar degeneration, it is currently recognized that socioeconomic factors likely muddle these findings, and work exposure is only a modest contributor to disc disease.
Pathophysiology
Back pain caused by disc disease is assumed to radiate due to compression of the nerve roots in the spinal canal caused by one or a combination of the following factors.
- Disc herniation material (i.e., herniated nucleus pulposus, HNP)
-
- HNP is characterized in varying degrees, ranging from disc protrusion (annulus stays intact) to extrusion (annular compromise, although herniated material remains continuous with disc space) to sequestered (free) pieces.
- HNP material is resorbed predictably over time, with the sequestered fragment exhibiting the greatest degree of resorption potential.
- In general, nonoperative treatments alone will result in symptomatic improvement in radicular problems in 90% of patients within 3 months.
- Hypertrophy/expansion of degenerative tissues
- The ligamentum flavum and the facet joint are two common origins. The facet joint, like every other joint in the body, degenerates, and synovial hypertrophy and/or accompanying cysts might endanger adjacent nerve roots.
Clinical presentation
The timeline of pain, the radiation of pain, and the precipitating events should be the emphasis of the patient's history. Prior trauma experiences should be carefully documented. Patients typically report discomfort spreading down both buttocks and lower limbs. It is useful to establish whether the discomfort is limited to the lower back or whether it has spread to the leg.
The presence of radiating discomfort is associated with canal stenosis. Radiating pain as the primary issue has a significantly more predictable surgical outcome than non-specific lower back pain that is most likely due to muscle exhaustion and tension.
Back pain with a mechanical component which is a pain that occurs only with certain movements) may indicate instability or a degenerative pars fracture. It is also critical to inspect circulation during any evaluation of extremity issues, as vascular claudication can mirror or mimic neurogenic issues.
An assessment of the patient's walking ability is essential for determining the daily effect of the pain/deficit. One systematic order is to have the patient get out of the chair, walk on his or her heels and toes, and then sit on the examination table for strength, reflex, and straight leg testing. A Trendelenburg gait, which can suggest an underlying weakness in the gluteus medius, which is innervated by the L5 nerve root, should be ruled out during the gait examination.
The neurologic function of the arms, legs, bladder, and intestines will be evaluated throughout all physical examinations. Organization and patience are essential for a complete examination. Not only should strength be assessed, but so should sensibility and reflexes. It is also critical to evaluate the skin around the back and document any discomfort to compression or recent surgical scars.
The straight leg raise (SLR) test involves a supine patient passively stretching his or her fully extended leg from 0 to roughly 80 degrees. The start of radiating back pain in either leg supports a stenotic canal diagnosis. A herniation compressing the L5 nerve root will cause ankle dorsiflexion weakness and considerable toe extension. This deficiency may also impair the Achilles tendon reflex. L4 radiculopathy can cause quadriceps weakness and a reduced patellar tendon response.
Documentation is critical since these first findings will very certainly be utilized as a baseline for all subsequent studies.
Wadell Signs
A thorough examination should also rule out non-organic causes of low back pain/symptoms. When a doctor detects psychological factors, the following should be taken into account:
- Inconsistency or nonspecific statement of symptoms, including superficial/non-anatomic locations of discomfort on examination
- Axial load/rotational motions cause pain.
- Patient distraction results in a negative SLR (one approach includes having the patient sitting in a chair and reproducing the SLR "environment")
- Symptom distribution patterns that are not dermatomal
- On the exam, the pain was out of proportion.
Some discs become uncomfortable after an injury due to inflammation, and the pain comes and goes. Because some people's nerve endings penetrate further into the anulus fibrosus (outer layer of the disc) than others, discs are more prone to cause discomfort. In the alternative, when these nerves become irritated by nucleus pulposus material, repair of injuries to the outer anulus fibrosus may result in innervation of the scar tissue and pain signals from the disc.
Degenerative disc disease can progress to a chronic disabling disorder with major consequences for a person's quality of life. When the pain from degenerative disc degeneration is severe, nonsurgical therapy may be unsuccessful.
Diagnosis
Anterior-posterior (AP) and lateral radiographs of the affected area are commonly used in the evaluation of individuals with low back pain. Some doctors will order radiographs of the complete spine. An MRI should not be conducted at the initial presentation of suspected acute disc herniations in patients who do not have "red flags," because these patients will often benefit from a 6-week course of physical therapy.
In the first presentation, an MRI is most certainly a needless cost and use burden. If the symptomology persists at the follow-up, an MRI can be acquired at that time. The T2 weighted sagittal and axial pictures should be examined closely since they will show any compression of neurologic components.
On MRI, both symptomatic and asymptomatic disc herniations shrink over time. The presence of disc disease (degeneration or herniation) on MRI did not predict the risk of persistent pain or the necessity for surgery in the future.
Management
In the setting of “red-flags,” aggressive diagnosis and likely surgical options should be explored. Examples of these red flags include:
- Cauda equina syndrome (issues controlling bowel/bladder, difficulty starting urination)
- Infection (high suspicion in IV drug user, history of fever, nighttime chills)
- Tumor suspected (known history of cancer; new-onset weight loss)
- Trauma (fall, assault, collision)
Fortunately, the vast majority of individuals will improve without the need for surgery. A course of at least 6 weeks of physical therapy should be performed, with a focus on core strengthening and flexibility. Non-surgical treatments include cognitive therapy, lifestyle changes, and modifying activities that may aggravate pain, as well as nonsteroidal anti-inflammatory drugs (NSAIDs) and epidural injections.
Epidural injections may give mild, short-term pain relief for disc herniations, but the data on its efficacy for chronic non-radiating back pain is less definite. Certainly, the literate does not oppose injections as a non-surgical therapeutic option.
Surgery
Regrettably, many patients do not respond to conservative treatment. If the conservative plan fails, the patient has three options:
- continued pain,
- complete avoidance of activities that elicit pain, or
- surgical intervention.
Again, surgical alternatives for disc herniations and degenerative spinal stenosis should be reserved for patients who have neurologic impairments, degenerative spondylolisthesis, or discomfort that limits everyday tasks.
Operative intervention includes:
- Lumbar discectomy with fusion: When compared to nonsurgical therapy, fusion had improved results for degenerative lumbar disc degeneration. Fusion has long been regarded as the gold standard in the treatment of lumbar degenerative disc disease.
- Lumbar total disc replacement: A single-level disc condition with disease-free facet joints is the primary indication. This has been shown to have superior patient outcomes and reduced incidence of neighboring segment disease when compared to fusion. On the other hand, individuals may still complain of prolonged back discomfort after surgery, which might be attributed to slight instability of the prosthesis. A problem has also been reported: dislocation of the polyethylene inlay. Revision arthroplasty or conversion to arthrodesis can be used to address this.
Stem cell therapy
The University of Queensland in Australia has had some success with a tissue engineering-based technique based on stem cells. Using an injectable hydrogel technology, the goal is to stimulate functional cartilage to create itself. The researchers came to the conclusion that stem cell treatment might be beneficial for intervertebral disc regeneration. The judgment is yet out, and many more research are required to verify that this medication is both safe and effective.
Outcome
Patients who chose surgery had better results at 3 months, years, and 4 years than patients who did not choose surgery. Standard open surgery and microdiscectomy have equal results and efficacy. In terms of the quantity of disc removed during a discectomy, while a "limited" discectomy gives greater pain relief and patient satisfaction than a partial discectomy, it also increases the risk of recurrence herniation.
When comparing repeat/revision microdiscectomies to their first discectomy, patient results and satisfaction are comparable. The surgery may necessitate overnight hospitalization; however, these operations are typically designed to be outpatient procedures. The patient must understand that, while surgical intervention has a positive outcome for treating radicular pain, the prognosis for non-radiating lower back pain are less predictable.
Clinical and fundamental science investigations have been done by researchers and surgeons to reveal the regeneration power held by the huge animal species involved (humans and quadrupeds) for prospective therapeutics to treat the condition. Some therapies used by New York research laboratories include injecting biologically-engineered, riboflavin cross-linked high density collagen (HDC-laden) gels into disease spinal segments to induce regeneration, eventually restoring functionality and structure to the two main inner and outer components of vertebral discs, the anulus fibrosus and the nucleus pulposus.
Conclusion
One of the more terrible elements of aging is that your joints start to wear down, often for no apparent reason. This joint wear and tear is frequent not just in the knees and hips, but also in the spine. The specific cause of spine joint wear is unknown; however it might be a combination of variables such as performing a lot of lifting, having a family history of spine difficulties, or having a spine accident.
This wear and tear is a kind of arthritis in which the cartilage in the spine joints wears down. Regardless of the etiology, it is widely recognized that arthritis of the spine frequently worsens with age for no apparent reason.