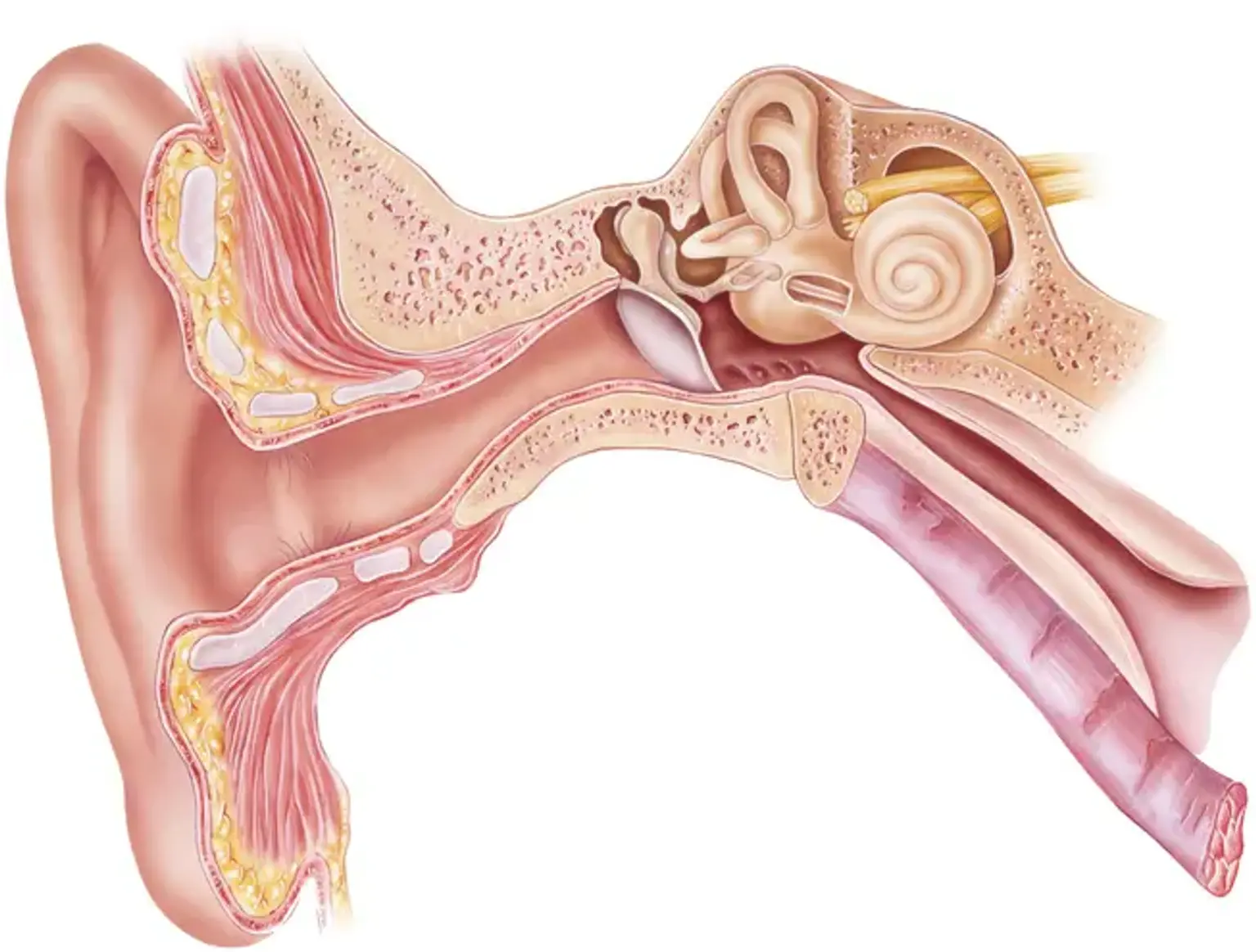
Introduction
Ear disorders can significantly affect a person’s quality of life, leading to issues like hearing loss, discomfort, and emotional distress. Ear health is crucial, as the ears play an essential role in communication, balance, and overall well-being. While many ear disorders can be treated, a specialized procedure known as ear volume restoration is gaining popularity, especially in countries like Korea. This procedure helps restore both the physical appearance and functionality of the ear, which may be compromised due to injury, aging, or disease.
Why is ear disorder treatment important? Treating ear disorders not only improves hearing but also enhances one’s self-esteem and social interactions. This article will explore various ear treatment options, including innovative volume restoration methods, and discuss their effectiveness and popularity, particularly in Korea.
Causes of Ear Disorders
Ear disorders can arise from a variety of factors, including chronic ear conditions like infections, trauma, and genetic predisposition. Hearing loss, in particular, is a leading concern and can stem from both age-related degeneration and environmental factors such as prolonged exposure to loud noises.
Key Causes of Ear Disorders:
Aging: As people age, hearing tends to degrade, often leading to volume loss in the ear.
Infections: Middle ear infections and other conditions can damage the ear's internal structure.
Trauma: Accidents or injury to the ear can affect its volume and function, requiring restoration.
Noise Exposure: Chronic exposure to loud sounds can cause permanent damage to ear cells.
Volume loss and hearing loss are often interconnected. When ear volume is diminished, it can impact the ear's ability to transmit sound properly, leading to hearing difficulties. For those suffering from hearing loss or ear deformation, treatments like ear volume restoration can be life-changing.
Popular Ear Disorder Treatments in Korea
Korea has become a global hub for ear treatments, particularly for volume restoration procedures. With advanced technologies and highly skilled practitioners, many international patients travel to Korea for innovative ear surgeries that address both aesthetic and functional concerns.
Why Korea for Ear Treatment?
Advanced Medical Technologies: Korea is at the forefront of using cutting-edge treatments for ear disorders, including fat grafting and implant surgeries.
Medical Tourism: Korea’s reputation for high-quality medical care at affordable prices makes it a popular destination for patients worldwide.
Expert Practitioners: Leading ear specialists in Korea are highly trained in the latest procedures to restore ear health and appearance.
From non-surgical treatments like hearing aids to surgical interventions that restore ear volume and hearing, Korea offers a wide array of options for those seeking ear disorder treatments. The country’s ability to combine advanced technology with highly experienced practitioners makes it a leading destination for medical tourists.
Understanding Ear Volume Restoration
Ear volume restoration refers to procedures designed to restore the natural shape and volume of the ear, often lost due to injury, age, or disease. This can include both surgical and non-surgical methods, depending on the severity of the ear disorder.
What is Ear Volume Restoration? Ear volume restoration procedures aim to correct deformities or deficiencies in ear volume, typically through fat grafting, implants, or other advanced techniques. These procedures can help restore a natural appearance, improve hearing function, and alleviate discomfort caused by volume loss.
When is Ear Volume Restoration Needed?
Hearing Loss: When hearing loss is accompanied by ear deformities or volume loss, this procedure can restore the ear’s natural structure and improve auditory function.
Post-Trauma: Following accidents or injuries, ear volume restoration may be necessary to repair the damage and ensure proper ear function.
Age-Related Changes: As people age, they may experience volume loss in the ear, leading to the need for volume restoration procedures.
This procedure not only helps improve the aesthetic appearance of the ear but also plays a vital role in hearing restoration, making it an essential treatment for many people experiencing ear disorders.
Types of Ear Treatment Procedures
When it comes to treating ear disorders, there are a variety of procedures available, ranging from surgical interventions to non-surgical treatments. The choice of treatment largely depends on the severity of the condition, the patient's overall health, and their desired outcome.
Surgical Procedures:
Ear Repair Surgery: This may involve fat grafting, where fat is harvested from another part of the body and injected into the ear to restore volume and shape.
Implants and Prosthetics: In cases where ear volume restoration is not possible with grafts, implants may be used to restore the ear's appearance and function.
Non-Surgical Options:
Hearing Aids: These devices can help amplify sounds, improving hearing in patients suffering from hearing loss.
Regenerative Treatments: Emerging therapies such as stem cell treatments and sound therapy can help restore ear function and improve hearing without surgery.
Both approaches—surgical and non-surgical—have their benefits, and the choice between them should be made in consultation with a qualified ear specialist.
How Ear Surgery Works for Volume Restoration
Ear volume restoration surgery is a complex but highly effective procedure designed to correct ear deformities and restore both appearance and function. Here's how it typically works:
The Surgical Process:
Initial Consultation: Before surgery, a thorough evaluation of the patient's ear condition is performed, including hearing tests and medical assessments.
Fat Grafting or Implantation: The most common surgical methods involve harvesting fat from the patient's body and injecting it into the ear to restore lost volume. In some cases, implants may be used to achieve the desired shape and volume.
Surgical Precision: Surgeons use advanced techniques to ensure the procedure is as minimally invasive as possible, reducing recovery time and risk of complications.
Recovery Timeline:
Post-Op Care: After surgery, patients may experience mild swelling and discomfort, but these symptoms usually subside within a few days to weeks.
Follow-Up Visits: Regular check-ups are essential to monitor healing and ensure the desired results are achieved.
Full Recovery: Patients typically return to normal activities within a few weeks, although complete recovery can take up to six months, depending on the extent of the procedure.
This surgical intervention can significantly improve both the function and aesthetics of the ear, making it a popular option for those looking to restore ear volume.
Risks and Benefits of Ear Volume Restoration Surgery
Like any surgical procedure, ear volume restoration carries certain risks, but it also offers numerous benefits. It's essential for patients to understand both aspects before deciding to proceed.
Benefits:
Restores Natural Ear Appearance: The procedure helps restore the ear’s natural volume and shape, improving overall facial symmetry.
Improved Hearing: For those with hearing loss, restoring ear volume can improve the ear's ability to capture sound, enhancing hearing.
Increased Self-Confidence: Restoring the ear’s function and appearance can significantly boost a patient’s confidence and quality of life.
Risks:
Infection: As with any surgery, there is a risk of infection at the site of the incision or graft.
Scarring: Some scarring may occur, though it is typically minimal and well-hidden.
Uneven Results: In rare cases, the surgery may not provide the desired results, requiring additional procedures.
Safety Protocols in Korea:
Top clinics in Korea follow stringent safety protocols, ensuring that surgeries are conducted in sterile environments by highly qualified specialists. Patients should always choose certified surgeons to minimize risks and achieve optimal results.
Non-Surgical Alternatives for Ear Volume Restoration
While surgery offers permanent solutions, many patients prefer to explore non-surgical options for restoring ear volume. These treatments are often less invasive, with quicker recovery times and fewer risks.
Hearing Aids and Sound Therapy:
Hearing Aids: These devices can amplify sounds, providing immediate relief for those with hearing loss. They are not directly involved in restoring ear volume but can improve ear function.
Sound Therapy: Often used in conjunction with hearing aids, sound therapy helps retrain the brain to interpret sounds more effectively, improving overall ear function.
Regenerative Treatments:
Fat Grafting: A non-surgical alternative to implants, fat grafting can sometimes be done with minimally invasive techniques, offering moderate improvements in ear volume.
Stem Cell Therapy: Although still in the experimental stage, stem cell therapy holds promise for regenerating damaged ear tissue and improving ear function.
Platelet-Rich Plasma (PRP): This treatment uses the body’s own platelets to stimulate tissue growth and promote healing, potentially restoring ear health and volume.
Why Choose Non-Surgical Methods?
Non-surgical treatments offer a less invasive approach with lower risks, making them appealing for patients who want to avoid long recovery times. They may be ideal for those with mild ear volume loss or early-stage hearing loss.
The Role of Tinnitus Treatment in Ear Health
Tinnitus refers to the perception of ringing or buzzing in the ears without an external sound source. It’s a common symptom of ear disorders, especially hearing loss or ear damage. Tinnitus can be bothersome and affect a person's quality of life, making its treatment essential.
Treatment Options for Tinnitus:
Sound Therapy: This treatment involves using external sounds to mask or reduce the perception of tinnitus, helping the brain focus on other sounds.
Cognitive Behavioral Therapy (CBT): CBT helps individuals manage the emotional distress caused by tinnitus, improving coping mechanisms.
Medications: Some medications, including anti-anxiety drugs and antidepressants, may help alleviate the stress associated with tinnitus.
Hearing Aids: For those with hearing loss and tinnitus, hearing aids can amplify external sounds, reducing the prominence of tinnitus.
How Tinnitus and Hearing Loss Are Connected:
Many individuals with hearing loss also experience tinnitus, as the brain compensates for the reduced auditory input by generating internal sounds. Treating hearing loss through hearing aids or volume restoration may alleviate both conditions simultaneously.
The Effectiveness of Ear Volume Restoration Treatments
Ear volume restoration treatments have proven highly effective for many individuals, both in terms of aesthetic and functional benefits. These treatments can significantly improve hearing, appearance, and overall quality of life.
How Effective Are These Treatments?
Studies show that procedures like fat grafting and implants can restore a natural appearance to the ear and improve hearing in those with mild to moderate volume loss. The success rate of these treatments is generally high, with most patients experiencing noticeable improvements in both function and aesthetics.
Patient Outcomes:
Before and After: Many patients report increased self-confidence and satisfaction after undergoing ear volume restoration surgery. These improvements go beyond the physical appearance, significantly enhancing social interactions and emotional well-being.
Real-Life Examples: Case studies show that patients who undergo ear volume restoration can regain hearing functionality, along with the restoration of the ear’s appearance, often improving their life quality.
Long-Term Benefits:
Improved Hearing: Restoring ear volume can enhance the ear's ability to transmit sound, reducing the need for hearing aids.
Enhanced Appearance: In addition to hearing benefits, restoring ear volume can help with the overall appearance, especially for those with congenital deformities or ear trauma.
Preparing for Ear Volume Restoration Surgery
The pre-surgical process for ear volume restoration is an essential part of ensuring the procedure’s success. A thorough evaluation and proper preparation can significantly impact the results.
Pre-Surgical Assessments:
Medical History: A detailed review of the patient’s medical history is conducted to ensure they are a good candidate for surgery.
Hearing Tests: Audiological assessments help determine the extent of hearing loss and guide treatment decisions.
Physical Exam: A physical exam of the ear is performed to evaluate the degree of volume loss and other abnormalities.
Imaging: Sometimes, imaging tests like CT scans or MRIs may be used to assess the underlying structures of the ear.
Consultation with Specialists:
A qualified ear specialist or plastic surgeon will discuss the available treatment options and recommend the best course of action. They will also explain the benefits, risks, and recovery process.
What to Expect Before Surgery:
Fasting: Patients will be asked to refrain from eating or drinking before surgery to reduce anesthesia risks.
Medication Management: Certain medications may need to be stopped temporarily to prevent complications.
Mental Preparation: Preparing mentally for the procedure helps reduce anxiety and ensures patients understand the steps involved.
The Recovery Process After Ear Volume Restoration
The recovery process is an essential part of the ear volume restoration journey. Understanding the healing timeline and post-operative care can help patients manage expectations and ensure optimal results.
Post-Op Care:
Pain Management: Mild discomfort or swelling is common after the procedure. Painkillers prescribed by the surgeon can help alleviate these symptoms.
Dressings and Bandages: Surgical dressings or bandages may be applied to protect the ears as they heal.
Avoiding Strain: Patients should avoid strenuous physical activities or touching the operated area during the early recovery stages.
What to Expect in the Weeks After Surgery:
Initial Healing: Swelling and redness around the treated area are normal in the first few days.
Follow-Up Visits: Regular check-ups ensure that the ear is healing properly and that no complications are arising.
Gradual Improvement: Full results may take up to 6 months, as the ear settles into its new shape and volume.
When Can You Return to Normal Activities?:
Light Activities: Patients can usually return to work and light daily activities within 1-2 weeks.
Full Recovery: Strenuous activities should be avoided for about 4-6 weeks, and full recovery typically occurs within 3-6 months.
Cost of Ear Volume Restoration in Korea
The cost of ear volume restoration procedures can vary significantly depending on the treatment type, the clinic’s location, and the expertise of the surgeon. Korea has become a leading destination for medical tourism due to its high-quality ear treatments at competitive prices.
Price Range for Treatments:
Surgical Procedures: The cost for ear volume restoration surgeries like fat grafting or implants typically ranges from $2,000 to $8,000, depending on the complexity and the clinic.
Non-Surgical Options: For less invasive treatments, such as hearing aids or sound therapy, prices can range from $500 to $3,000, depending on the device and the duration of therapy.
Insurance Coverage and Payment Options:
Many clinics offer payment plans or financing options to help patients manage the cost of their procedures.
Insurance may cover part of the cost if the procedure is deemed medically necessary, such as for severe hearing loss or ear deformities.
Cost-Effectiveness of Korean Treatments:
Korea’s medical facilities are renowned for offering advanced treatment options at a fraction of the cost compared to Western countries, making it an attractive option for international patients.
The Global Popularity of Ear Treatment in Korea
Korea is gaining international recognition as a hub for innovative ear treatments, attracting patients worldwide for both aesthetic and functional ear restoration procedures.
Korean Medical Tourism:
Medical tourism in Korea has skyrocketed, with patients traveling from across the globe to take advantage of the country’s state-of-the-art technologies and highly trained specialists. The combination of affordable pricing and high success rates makes Korea a top destination for ear treatment.
Success Stories from International Patients:
Many international patients have shared their positive experiences, noting both the technical expertise of Korean doctors and the transformative results of ear volume restoration treatments. Case studies show that patients from the United States, Europe, and other regions have achieved significant improvements in hearing and appearance.
Korea’s Leading Role in Ear Treatment:
Korean clinics utilize cutting-edge technologies, including fat grafting and implant surgeries, ensuring patients receive the best possible care. Additionally, the country’s reputation for precision and safety in medical procedures further enhances its appeal to patients seeking ear treatments.
The Impact of Ear Disorder Treatment on Self-Esteem
Restoring ear health and appearance can have a profound effect on a patient’s self-esteem and overall well-being. Whether due to hearing loss or ear deformities, the improvements made through ear treatments can enhance both physical function and emotional health.
Psychological Benefits:
Increased Confidence: Many patients report a boost in self-esteem after ear volume restoration, especially if their condition was affecting their appearance or social life.
Enhanced Social Interaction: Restoring hearing ability and improving ear appearance enables individuals to engage more confidently in conversations and social settings.
Real-Life Examples:
One patient shared how, after undergoing ear volume restoration surgery, their ability to hear clearly again allowed them to reconnect with family and friends. The emotional transformation matched the physical one, as the patient felt more confident and less isolated.
Improved Quality of Life:
Beyond the physical changes, patients often experience an overall improvement in quality of life. The restored functionality of the ear can lead to greater participation in work, social activities, and even hobbies that were previously hindered by hearing issues.
Future Advancements in Ear Disorder Treatment
The field of ear disorder treatments is evolving rapidly, with new technologies and techniques emerging that promise even more effective solutions for ear health and volume restoration.
New Technologies on the Horizon:
Artificial Intelligence (AI): AI-driven tools are being developed to assist in diagnosing ear conditions more accurately, allowing for earlier intervention and better treatment planning.
Robotics: Robotic surgery is becoming more common, offering precision in ear volume restoration procedures and reducing recovery times.
Gene Therapy: In the future, gene therapy may be able to regenerate damaged ear tissues or reverse hearing loss caused by genetic factors.
Regenerative Medicine:
Stem Cell Therapy: Stem cell treatments are showing promise in the repair and regeneration of ear tissues, which could provide non-invasive options for restoring ear health and volume.
Platelet-Rich Plasma (PRP): PRP therapy uses the patient’s own blood to stimulate tissue regeneration, offering a natural, non-surgical solution for some ear conditions.
Global Trends in Ear Health:
As the demand for ear treatments grows, more countries are following Korea’s lead in adopting advanced treatments. Innovations like stem cell therapies and robotic surgery are expected to become mainstream in the coming years, improving patient outcomes and expanding the possibilities for ear restoration.
How to Choose the Right Ear Treatment for You
Choosing the right ear treatment is an important decision that can significantly impact both your health and quality of life. There are various factors to consider before undergoing ear volume restoration or other treatments.
Consultation Process:
The first step is to consult with a qualified ear specialist or plastic surgeon. They will perform a thorough assessment of your ear condition, including hearing tests, physical examination, and imaging if needed. Based on the results, they will recommend the best course of treatment for you.
Factors to Consider:
Severity of the Condition: The degree of ear volume loss or hearing loss will influence whether surgical or non-surgical treatments are required.
Age and Health: Your overall health and age may also play a role in deciding which treatment is best for you.
Desired Outcomes: Whether you are primarily concerned with improving hearing, restoring appearance, or both, clear communication with your doctor about expectations is key.
Choosing a Clinic in Korea:
Credentials and Experience: Ensure the clinic has certified surgeons with experience in ear restoration procedures.
Patient Reviews and Testimonials: Check reviews and testimonials from previous patients to gauge the quality of care.
Technology and Safety: Make sure the clinic uses the latest, safest technologies and follows strict safety protocols.
Frequently Asked Questions (FAQs)
When considering ear disorder treatments, especially ear volume restoration, patients often have common questions about the procedure, recovery, and outcomes. Here are some frequently asked questions:
What is ear volume restoration surgery?
Ear volume restoration surgery is a procedure to restore the natural volume and shape of the ear, often involving fat grafting or implants. It can improve both the aesthetic appearance and hearing functionality of the ear.
Is ear volume restoration surgery safe?
Yes, ear volume restoration surgery is generally safe when performed by a qualified and experienced surgeon. Following pre-surgical guidelines and post-op care instructions is crucial to minimize risks.
How long does it take to recover from ear volume restoration surgery?
Recovery time varies but typically takes 1-2 weeks for initial healing, with full recovery and final results visible after 3-6 months.
Are there non-surgical alternatives?
Yes, there are non-surgical options like hearing aids, sound therapy, and stem cell treatments that can help restore ear function and volume without surgery.
How much does ear volume restoration cost?
The cost varies based on the type of treatment and the clinic. In Korea, surgical procedures typically range from $2,000 to $8,000, while non-surgical treatments can range from $500 to $3,000.
Visual Aid and Illustration Suggestions
Visual aids can enhance the understanding of ear volume restoration procedures and help patients better grasp what to expect from surgery. Here are some suggestions for illustrations:
Before and After Photos:
Display images of patients before and after undergoing ear volume restoration surgery to showcase the improvements in both appearance and ear functionality.
Illustrations:
Diagrams explaining the fat grafting process or implant procedures can help patients understand the techniques involved in restoring ear volume.
Patient Testimonials:
Short video clips or photos of patients sharing their experiences and satisfaction with ear restoration treatments can offer a personal, relatable touch.
Conclusion
Restoring ear volume and treating ear disorders can significantly improve both hearing and appearance, boosting overall confidence and quality of life. Ear volume restoration is an effective solution for those dealing with hearing loss, ear deformities, or aging-related changes.
Recap of the Importance of Ear Health:
Ear disorders can hinder communication and self-esteem. Seeking treatment for these issues, whether through surgery or non-invasive methods, can lead to a noticeable improvement in both function and appearance.
Encouragement to Seek Treatment:
If you’re struggling with ear-related issues, consult a qualified specialist to explore your treatment options. Restoring ear health can enhance your life in ways beyond just physical appearance.