Introduction
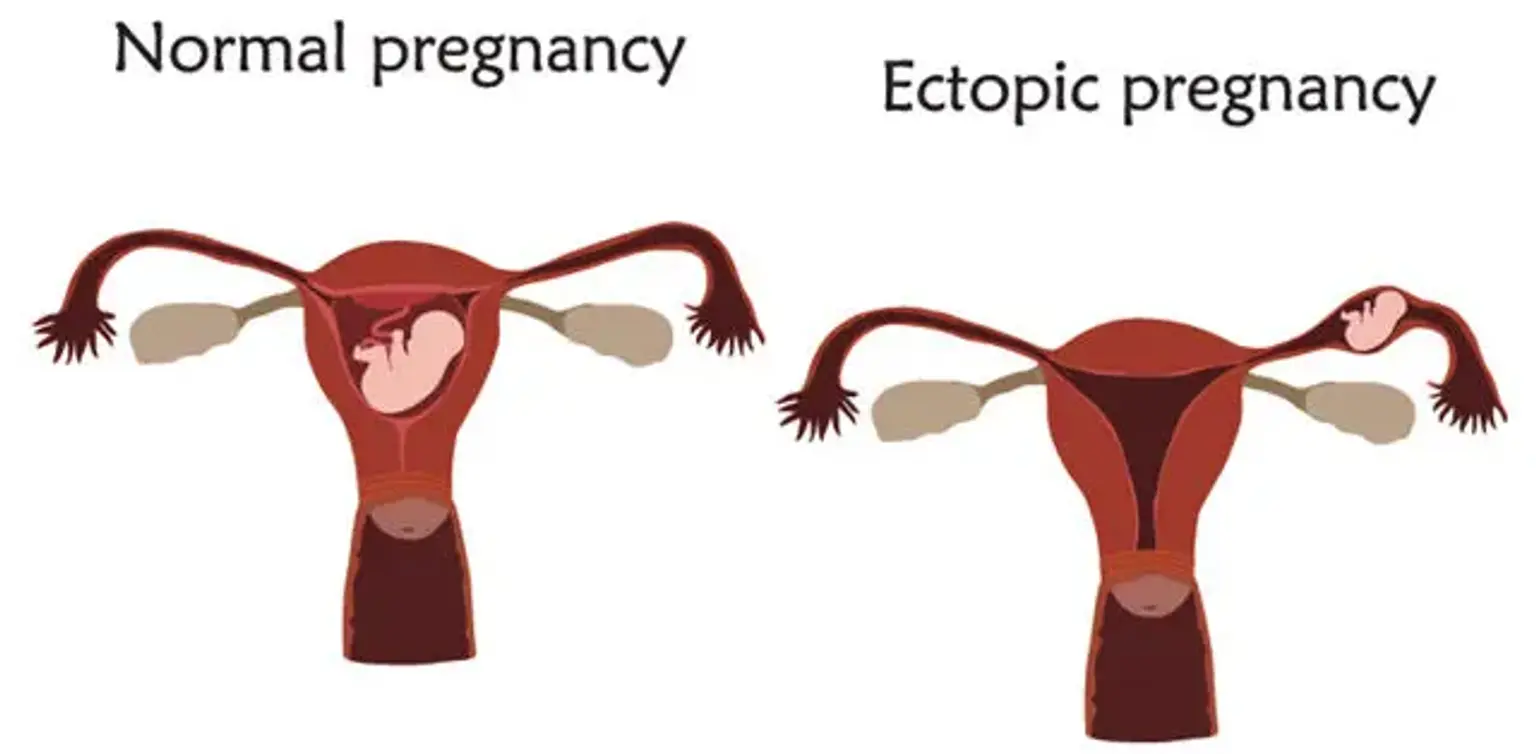
An ectopic pregnancy occurs when a fertilized egg implants outside the uterus, often in one of the fallopian tubes. Unlike a normal pregnancy, where the fertilized egg embeds in the uterine lining, an ectopic pregnancy is non-viable and can cause serious health risks if not diagnosed and treated promptly. Early detection and intervention are crucial to prevent complications such as fallopian tube rupture, hemorrhage, or even death.
This article will explore the various approaches to managing ectopic pregnancy, including medical, surgical, and expectant methods. It will also discuss diagnostic techniques, signs, and symptoms to help patients and healthcare providers make informed decisions.
Understanding Ectopic Pregnancy
An ectopic pregnancy occurs when a fertilized egg implants outside the uterus, most commonly in a fallopian tube. Less frequently, it can occur in other areas such as the cervix, ovary, or abdominal cavity. The key issue with ectopic pregnancies is that these locations cannot sustain the growth of a fetus, making the pregnancy non-viable.
Risk factors include:
Previous ectopic pregnancy: Women who have had one are at a higher risk of recurrence.
Pelvic inflammatory disease (PID): An infection of the reproductive organs can scar the fallopian tubes, increasing the likelihood of ectopic pregnancy.
Age: Women over 35 may have an increased risk.
Fertility treatments: Some fertility interventions, like in vitro fertilization (IVF), can increase the chances of an ectopic pregnancy.
While ectopic pregnancies can be fatal if left untreated, the majority of cases are preventable or treatable with timely intervention.
Diagnosis of Ectopic Pregnancy
Diagnosing an ectopic pregnancy typically involves a combination of ultrasound and blood tests. The primary diagnostic tool is transvaginal ultrasound (TVUS), which can help identify the location of the pregnancy. In some cases, the pregnancy might not be visible on the ultrasound, leading to the diagnosis of a pregnancy of unknown location (PUL). This scenario requires follow-up ultrasounds and close monitoring of beta-hCG levels.
Beta-hCG levels, which are produced by the placenta during pregnancy, are also closely monitored. In a typical pregnancy, beta-hCG levels double approximately every 48 hours in the early stages. In ectopic pregnancies, however, these levels may rise more slowly or may not increase as expected.
If a woman presents with an abnormal rise in beta-hCG levels and no clear intrauterine pregnancy on ultrasound, further testing and close follow-up are necessary. Early diagnosis is key to determining the most appropriate treatment plan and preventing complications.
Beta-hCG Levels and Their Role in Management
Beta-hCG (human chorionic gonadotropin) is a hormone produced during pregnancy. In an ectopic pregnancy, tracking beta-hCG levels is vital for diagnosis and guiding treatment decisions.
In a healthy pregnancy, beta-hCG levels typically double every 48 hours in the first few weeks. However, in an ectopic pregnancy, these levels may rise more slowly or plateau. Monitoring these levels can help determine whether a pregnancy is viable or ectopic.
If beta-hCG levels are low or not increasing as expected, it may indicate an ectopic pregnancy, leading to further diagnostic measures. A significant drop in levels can confirm that the pregnancy is no longer viable, helping guide treatment.
Signs and Symptoms of Ectopic Pregnancy
The symptoms of an ectopic pregnancy can vary depending on the location of the implantation, but common signs include:
Abdominal pain: Often on one side of the abdomen.
Vaginal bleeding: Light spotting or heavier bleeding.
Dizziness or fainting: Indicating possible internal bleeding from a ruptured ectopic pregnancy.
It's important to note that some women may not experience these symptoms, which makes early detection crucial. As the pregnancy grows, the symptoms may worsen, especially if the ectopic pregnancy ruptures, leading to severe internal bleeding.
If you suspect an ectopic pregnancy, it's essential to seek medical attention immediately, as rupture can lead to life-threatening complications.
Medical Management with Methotrexate
Methotrexate is the most commonly used medication for treating ectopic pregnancies. It is a chemotherapy drug that stops rapidly dividing cells, effectively halting the growth of the ectopic pregnancy.
This treatment is generally used for stable women with early-stage ectopic pregnancies (usually under 4 cm in size) and low beta-hCG levels. Methotrexate is given as a single injection and is typically effective in resolving the pregnancy over several weeks.
The advantage of methotrexate is that it avoids surgery, but it comes with potential side effects such as nausea, abdominal pain, and vaginal bleeding. Regular monitoring of beta-hCG levels is essential to track the treatment’s effectiveness, with follow-up blood tests to ensure that beta-hCG levels decrease appropriately.
Methotrexate Protocols: Single-Dose vs. Multi-Dose
There are two primary methotrexate protocols used in managing ectopic pregnancies:
Single-dose protocol: Most common, particularly for women with low initial beta-hCG levels. A single dose of methotrexate is administered, and beta-hCG levels are monitored over the following weeks.
Multi-dose protocol: Used for cases where the single-dose treatment does not show sufficient progress, or if the initial beta-hCG levels are higher. This regimen involves multiple doses of methotrexate, spaced several days apart, to ensure that the pregnancy is fully resorbed.
Both protocols require careful monitoring to ensure the pregnancy resolves and that the woman remains stable.
Ovarian Ectopic Pregnancy: Diagnosis and Treatment
An ovarian ectopic pregnancy occurs when the fertilized egg implants in the ovary rather than the fallopian tube. This type of ectopic pregnancy is rare but can be life-threatening if not diagnosed early.
Diagnosis typically requires an ultrasound, as ovarian ectopic pregnancies may present similarly to ovarian cysts. In these cases, the key differences are the detection of a gestational sac or embryo in the ovary.
The treatment is usually surgical, and it involves removing the ectopic pregnancy while preserving the ovary if possible. In severe cases, the ovary may need to be removed. Ovarian ectopic pregnancies can lead to complications such as hemorrhage, so timely intervention is essential.
Surgical Management of Ectopic Pregnancy
Surgery may be necessary if the ectopic pregnancy is large, causing symptoms like severe pain, or if there is a risk of rupture. It is also an option if medical management with methotrexate fails.
There are two main surgical procedures:
Salpingectomy: This involves removing the affected fallopian tube. It’s the most common surgical treatment and is often necessary if the tube has ruptured.
Salpingostomy: This procedure removes the ectopic pregnancy while preserving the fallopian tube. It may be considered if the pregnancy is detected early and the tube is intact.
Surgical management typically requires a hospital stay and a recovery period of several weeks. Although surgery is effective in resolving the pregnancy, it may affect future fertility, especially if both tubes are damaged.
Expectant Management: Observation Approach
In some cases, expectant management, or the "wait-and-see" approach, may be appropriate for women with early, stable ectopic pregnancies. This strategy is used when the pregnancy is small, the woman is asymptomatic, and beta-hCG levels are low and declining.
Expectant management involves close monitoring of beta-hCG levels and ultrasounds to ensure that the pregnancy is resolving on its own. If the levels decrease without complications, no further intervention is needed. However, if the condition worsens or symptoms like pain or bleeding occur, medical or surgical treatment may be required.
This approach carries fewer risks but requires careful follow-up to ensure the pregnancy is non-viable and not progressing.
Cervical Ectopic Pregnancy Management
A cervical ectopic pregnancy is a rare but serious form of ectopic pregnancy where the fertilized egg implants in the cervix. Due to the lack of space and the increased blood flow in the cervix, this type of ectopic pregnancy poses a significant risk of rupture and severe hemorrhage.
Treatment for cervical ectopic pregnancy depends on the size and viability of the pregnancy. Options include:
Methotrexate: Often used when the pregnancy is early and the woman is stable.
Surgical options: A surgical procedure to remove the ectopic pregnancy and control bleeding. This may involve dilation and curettage (D&C) or hysterectomy, depending on the severity.
Cervical ectopic pregnancies require a specialized approach and often involve a multidisciplinary team to manage the complications and preserve the woman's fertility if possible.
Rudimentary Horn Ectopic Pregnancy
A rudimentary horn ectopic pregnancy occurs in women with a congenital uterine anomaly where one side of the uterus has an underdeveloped horn. Pregnancy in this abnormal horn is extremely dangerous because it lacks the proper structures to sustain a pregnancy.
This rare condition is often diagnosed via ultrasound or laparoscopy after an ectopic pregnancy is suspected. Surgical management is the primary treatment, and it typically involves removing the rudimentary horn and any tissue associated with the ectopic pregnancy. The procedure can be complex and may require careful planning by a specialist.
For women diagnosed with a rudimentary horn, there may be a need for genetic counseling to assess future pregnancy risks.
Managing Pregnancy of Unknown Location (PUL)
A pregnancy of unknown location (PUL) occurs when a woman has a positive pregnancy test but no visible gestational sac on an ultrasound. PUL is commonly linked to early ectopic pregnancies or very early intrauterine pregnancies.
Management involves monitoring beta-hCG levels to determine the viability of the pregnancy. In some cases, the pregnancy resolves without intervention, while in others, it may evolve into an ectopic pregnancy. If beta-hCG levels rise abnormally or if the woman shows symptoms, further intervention (medical or surgical) may be necessary.
Close follow-up with repeat ultrasounds is crucial in diagnosing ectopic pregnancy or confirming an early intrauterine pregnancy.
Complications of Ectopic Pregnancy
The primary complication of ectopic pregnancy is rupture, where the implantation site tears, leading to heavy internal bleeding. Symptoms of rupture include sharp abdominal pain, dizziness, and fainting.
Hemorrhage can cause life-threatening shock, making immediate treatment essential. If the fallopian tube is ruptured, surgery is often required to stop bleeding and remove the pregnancy.
Other complications include:
Infertility: Damage to the fallopian tubes may increase the risk of future infertility or recurrent ectopic pregnancies.
Emotional impact: The loss of the pregnancy can be psychologically challenging, and women may experience grief and trauma.
Managing these complications requires timely intervention, emotional support, and, if necessary, counseling.
Long-term Implications of Ectopic Pregnancy
An ectopic pregnancy can affect a woman’s future fertility. Damage to the fallopian tubes increases the risk of another ectopic pregnancy and may hinder the ability to conceive naturally. However, many women who have had an ectopic pregnancy can still conceive, often with the help of assisted reproductive technologies if both tubes are damaged.
Counseling and careful planning are vital for women who have experienced ectopic pregnancy. Early monitoring in subsequent pregnancies can ensure timely detection of potential complications. Women with a history of ectopic pregnancy are often advised to have early ultrasounds to confirm the location of the pregnancy.
Follow-Up Care After Ectopic Pregnancy
After treatment for an ectopic pregnancy, follow-up care is essential to ensure that beta-hCG levels return to zero, indicating that the pregnancy has been fully resolved. For women who underwent surgery, follow-up visits will check for any complications such as infection or excessive bleeding.
It's also important to provide emotional support during this time, as many women experience a sense of loss. Additionally, counseling regarding future pregnancies and the potential risks of recurrence is essential for informed decision-making.
Women who have been treated for an ectopic pregnancy should discuss birth control options and family planning with their healthcare provider.
Prevention Strategies for Ectopic Pregnancy
While it’s not always possible to prevent an ectopic pregnancy, certain measures can reduce the risk. Safe sexual practices and prompt treatment for sexually transmitted infections (STIs) like chlamydia and gonorrhea can help prevent pelvic inflammatory disease (PID), which is a leading cause of ectopic pregnancy.
For women with a history of ectopic pregnancies or tubal surgery, monitoring and early ultrasound in future pregnancies are essential. Additionally, using assisted reproductive technologies (ART) like in vitro fertilization (IVF) may increase the risk of ectopic pregnancies, so early pregnancy scans are important in these cases.
Lifestyle factors such as quitting smoking can also lower the risk, as smoking increases the chances of damage to the fallopian tubes.
Emotional and Psychological Impact
Experiencing an ectopic pregnancy can be emotionally distressing. Women may feel a deep sense of loss, grief, and confusion, especially when the pregnancy was desired. Psychological support is critical to help women cope with these emotions and any potential future fertility concerns.
Support groups and counseling can provide comfort, allowing women to share experiences with others in similar situations. It's also vital to acknowledge that some women may require professional mental health services if they experience prolonged sadness, anxiety, or depression after their loss.
The Role of Healthcare Providers in Ectopic Pregnancy Management
Healthcare providers play a key role in diagnosing and managing ectopic pregnancies. Timely and accurate diagnosis through ultrasound and beta-hCG monitoring is critical to determining the appropriate treatment plan. Providers must also ensure informed decision-making by discussing all available options, including medical, surgical, and expectant management.
Beyond physical care, healthcare professionals should be prepared to offer emotional support and counseling, providing resources for coping with the psychological impact of ectopic pregnancy. A holistic approach—addressing both physical and emotional needs—ensures better outcomes for patients.
Global Awareness and Access to Care
Ectopic pregnancy remains a significant global health issue, with complications varying based on access to healthcare. In areas with limited resources, the lack of early diagnosis and treatment can increase mortality rates. In high-resource settings, most women have access to early screening, reducing the risk of severe complications.
Raising awareness about the risks and symptoms of ectopic pregnancy globally is essential. Education campaigns can empower women to seek help early and receive appropriate treatment, improving outcomes. Universal access to healthcare services, including early diagnostic tools like ultrasound, can significantly reduce the incidence of severe complications and enhance overall maternal health.
Conclusion
Ectopic pregnancy is a serious and potentially life-threatening condition that requires prompt diagnosis and management. With early detection, there are several effective treatment options available, including medical, surgical, and expectant management, each tailored to the patient's unique situation. Monitoring beta-hCG levels and utilizing ultrasound technology remain crucial in diagnosing and managing the condition.
Though ectopic pregnancies can have emotional and psychological impacts, support systems and counseling can help women cope with the loss and the potential effects on future fertility. Preventative measures, such as managing STIs and reducing risk factors like smoking, can also decrease the likelihood of an ectopic pregnancy occurring.
The key to successful management lies in a coordinated approach from healthcare providers who can guide patients through both the physical and emotional aspects of this challenging condition. By raising awareness and ensuring access to quality care, we can reduce complications and improve outcomes for women globally.
In the face of an ectopic pregnancy, early intervention, compassionate care, and informed decision-making are essential to safeguarding the health and well-being of the mother.