What Is Eczema?
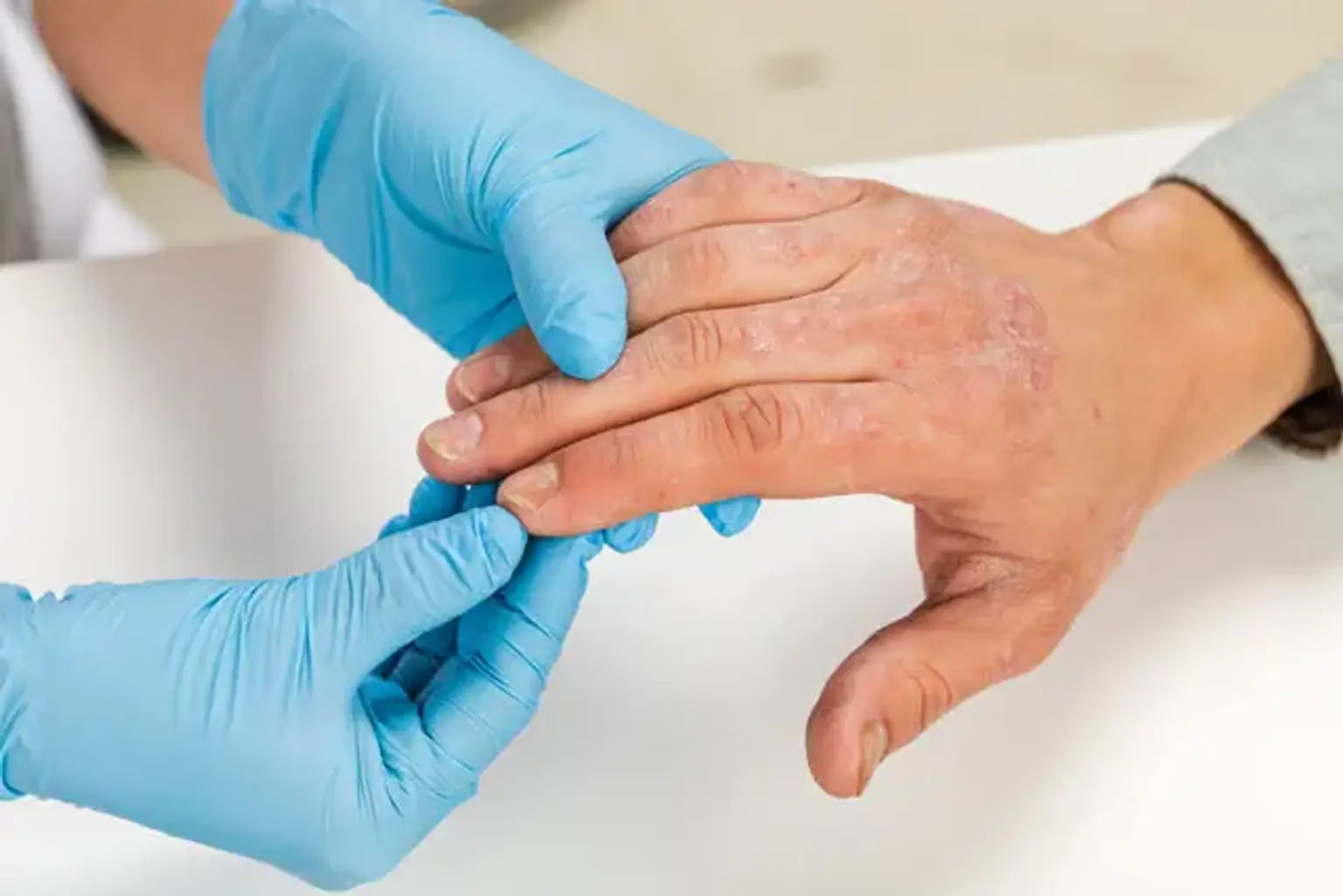
Eczema, also known as atopic dermatitis, is a chronic skin condition characterized by inflammation, redness, dryness, and itching. It affects people of all ages but is especially common in children. Though the exact cause of eczema remains unclear, it is believed to be a combination of genetic and environmental factors. The immune system of people with eczema overreacts to certain triggers, leading to the inflammation and irritation seen in eczema outbreaks.
There are several types of eczema, including:
Atopic Dermatitis: The most common type, often linked to family history of allergies or asthma.
Contact Dermatitis: Caused by direct contact with irritants or allergens.
Seborrheic Dermatitis: Affects areas of the skin rich in oil glands, like the scalp.
While eczema is not contagious, it can be uncomfortable and affect a person’s quality of life, especially when symptoms flare up.
Eczema Symptoms: How to Recognize Them
The primary symptom of eczema is itching (pruritus), often intense, which can cause discomfort and skin damage if scratched. Other symptoms include:
Red, inflamed skin: Particularly on the face, hands, behind the knees, or inside elbows.
Dry, cracked skin: Often leading to scaly patches or thickened areas.
Blisters or oozing sores: Sometimes, eczema patches can become infected.
Eczema symptoms can come and go, often triggered by specific factors like stress, weather changes, or exposure to irritants. Understanding these triggers is key to managing eczema and preventing flare-ups.
Causes and Triggers of Eczema
While there is no single cause for eczema, several factors are thought to contribute to its development and flare-ups:
Genetic Factors: A family history of eczema, asthma, or allergies can increase the likelihood of developing eczema.
Immune System Dysfunction: People with eczema have an overactive immune response, which leads to inflammation and itching in the skin.
Environmental Triggers: These include:
Allergens: Dust mites, pollen, mold, and pet dander.
Irritants: Soaps, detergents, certain fabrics (wool), and fragrances.
Climate: Extreme cold or hot, dry air, or humidity can trigger flare-ups.
Stress: Emotional stress and anxiety can worsen eczema symptoms.
Identifying personal triggers is a critical part of managing eczema. Keeping track of environmental factors and stress levels can help avoid flare-ups and control symptoms.
Diagnosis of Eczema
Diagnosing eczema is generally straightforward based on physical examination by a healthcare provider. The doctor will assess the appearance and location of the skin lesions, as well as the patient’s medical history.
To confirm an eczema diagnosis, doctors may use the following:
Patch Testing: A method to identify specific allergens that may be triggering the eczema. Small amounts of potential allergens are applied to the skin to check for reactions.
Skin Scraping or Biopsy: In rare cases, a biopsy might be performed to rule out other skin conditions with similar symptoms, such as psoriasis or fungal infections.
Blood Tests: To check for underlying conditions like allergies or infections, especially when symptoms are severe or persistent.
A thorough diagnosis ensures that the right treatment plan is developed to manage eczema effectively and minimize flare-ups.
Eczema Treatment Options: Overview
Managing eczema typically involves a combination of skin care routines, medications, and lifestyle changes. Treatment can vary depending on the severity of the condition, the patient's age, and how well they respond to various therapies. The main goal is to control symptoms, reduce flare-ups, and improve the quality of life.
Here are the primary approaches for treating eczema:
Topical Treatments: Creams and ointments to reduce inflammation and itching.
Oral Medications: For severe cases, immunosuppressive drugs like corticosteroids or biologics may be prescribed.
Phototherapy: Light therapy to help with more resistant eczema cases.
Alternative Remedies: Herbal treatments and lifestyle modifications that focus on natural healing.
With the right approach, most people can manage their eczema effectively and prevent frequent flare-ups.
Topical Steroids for Eczema Treatment
One of the most commonly used treatments for eczema is topical steroids. These are prescription creams or ointments that reduce inflammation and itching.
Types of Topical Steroids: There are different strengths of steroids, from mild hydrocortisone to stronger options like betamethasone. The strength and type of steroid prescribed depend on the severity of the eczema and the affected area.
Benefits: Topical steroids are highly effective in reducing inflammation and controlling flare-ups. They work by suppressing the immune system's overreaction in the affected area.
Risks and Side Effects: While effective, long-term use of steroids can cause thinning of the skin, stretch marks, and other side effects. Doctors generally recommend using these treatments for short periods or only on affected areas to minimize risks.
Safe Usage: To prevent side effects, it’s important to follow the doctor’s instructions for steroid application, limiting usage to the prescribed duration and amount.
Topical steroids remain one of the go-to solutions for managing eczema flare-ups but must be used with care.
Non-Steroidal Eczema Treatments: Options for Sensitive Skin
For individuals looking for non-steroidal options or those who experience side effects from steroids, there are other effective treatments available:
Topical Calcineurin Inhibitors: These include drugs like Protopic and Elidel, which help calm the immune system without the risk of thinning skin. These are often recommended for sensitive areas like the face or for long-term management of eczema.
Hydrating Creams and Emollients: Keeping the skin moisturized is one of the best ways to prevent eczema flare-ups. Creams containing ceramides or petrolatum help restore the skin barrier and retain moisture.
Antihistamines: These can be used to alleviate itching and inflammation. They are especially helpful when eczema is triggered by allergens.
Wet Wrap Therapy: This method involves applying a moisturizing cream to the affected area, then covering it with a damp bandage or cloth. The moist environment helps the skin absorb the treatment better and provides relief from dryness and itching.
These non-steroidal options can be effective for managing eczema without the long-term risks associated with steroids.
Phototherapy: Light Treatment for Severe Cases
For individuals with moderate to severe eczema that doesn’t respond to topical treatments, phototherapy (also known as light therapy) may be recommended. This treatment uses ultraviolet (UV) light to reduce inflammation and itching.
Types of Phototherapy:
Narrowband UVB: This type of UV light is commonly used for treating eczema. It is safe and effective for most people.
PUVA Therapy (Psoralen plus UVA): In this method, a photosensitizing medication is taken before exposure to UVA light. This is typically used for more severe cases.
How Phototherapy Works: The UV light helps by suppressing the overactive immune response in the skin and reducing inflammation. It also promotes the healing of the skin and can improve the appearance of eczema lesions.
Effectiveness: Phototherapy can significantly improve symptoms and is often recommended when other treatments fail. It’s particularly useful for patients with widespread eczema.
Risks and Considerations: Long-term exposure to UV light may increase the risk of skin aging and skin cancer. Doctors monitor patients closely during treatment to ensure safety.
Phototherapy can be a valuable treatment for patients with severe or persistent eczema, offering an alternative to long-term medication use.
Natural and Home Remedies for Eczema
Many individuals seek natural remedies to complement medical treatments or when they prefer to avoid conventional drugs. While these remedies are not a cure, they can provide relief and help manage eczema symptoms.
Aloe Vera: Known for its soothing properties, aloe vera gel can be applied directly to eczema-affected areas to reduce itching and inflammation.
Coconut Oil: This natural moisturizer has anti-inflammatory and antimicrobial properties, making it a great option for treating dry, irritated skin.
Chamomile Tea: Chamomile can be applied as a compress or taken orally. It has calming effects and may help reduce skin irritation.
Oatmeal Baths: Oatmeal has long been used to treat irritated skin. Soaking in an oatmeal bath can help soothe itching and soften the skin.
While these remedies can offer comfort, it’s important to remember that they work best as part of a comprehensive treatment plan, and patients should consult with a doctor before trying new treatments.
Eczema Flare-Ups: How to Manage and Prevent Them
Managing eczema flare-ups requires a combination of daily care, environmental control, and personal habits. Identifying triggers and creating a preventive routine is essential for minimizing flare-ups.
Skin Care Routine: Moisturizing regularly is one of the most effective ways to prevent flare-ups. Use gentle, fragrance-free products to avoid irritating the skin. After bathing, apply moisturizer immediately to lock in moisture.
Avoiding Triggers: Identifying and avoiding triggers such as allergens, harsh soaps, or specific foods can help prevent flare-ups. Keep track of your environment and activities to spot patterns.
Stress Management: Stress is a known trigger for eczema flare-ups. Practicing relaxation techniques like meditation, deep breathing, and yoga can help manage stress levels, reducing the likelihood of a flare.
Proper Clothing: Wear soft, breathable fabrics such as cotton, which help reduce irritation. Avoid wool or synthetic materials that can aggravate the skin.
A proactive approach to daily skincare, avoiding known triggers, and managing stress are key components of eczema flare-up prevention.
Eczema Treatment for Children
Eczema is particularly common in children, especially infants and toddlers. When treating eczema in children, special care is required to ensure safety and comfort.
Gentle Skin Care: Children have sensitive skin, so it’s crucial to use mild, fragrance-free cleansers and moisturizers. Bathing should be kept short and in lukewarm water to avoid further drying out the skin.
Topical Treatments: Mild steroid creams may be used, but pediatricians usually recommend using the lowest possible strength and applying them sparingly. Calcineurin inhibitors like Protopic can be alternatives for sensitive areas such as the face or eyelids.
Avoiding Triggers: Common eczema triggers in children include food allergies (e.g., milk, eggs), environmental allergens (pollen, dust), and irritants like soap and certain fabrics. Identifying these triggers through food diaries or allergy testing can be helpful in managing eczema.
Moisturizing and Hydration: Regular application of moisturizing creams helps strengthen the skin barrier. Hydration is key to keeping the skin soft and reducing flare-ups.
While eczema can be frustrating for both parents and children, a consistent skincare routine and close monitoring of triggers can help control symptoms effectively.
Eczema Management for Adults
Eczema in adults presents unique challenges, as it can significantly impact social life and mental health. Managing eczema in adults requires a tailored approach that incorporates both medical treatments and lifestyle adjustments.
Skin Care: Regular moisturizing is still essential, and adults may need to use stronger, more specialized products. Non-steroidal treatments, such as calcineurin inhibitors or biologics, can be considered for severe eczema.
Workplace and Social Life: Visible eczema can lead to self-esteem issues, particularly in social or professional environments. Adults may need to seek support from mental health professionals or support groups to cope with the emotional challenges.
Avoiding Irritants: Adults should avoid harsh chemicals in cleaning products, scented lotions, and fabric softeners. Choosing hypoallergenic clothing can also help reduce skin irritation.
Diet and Lifestyle Changes: There’s increasing evidence that a healthy diet rich in anti-inflammatory foods (like omega-3 fatty acids and antioxidants) can improve eczema symptoms. Regular exercise, good sleep, and stress management are all important in maintaining skin health.
For adults with eczema, managing the condition often means balancing medical treatment, lifestyle modifications, and mental health support to reduce both the physical and emotional impact of the disease.
Eczema and Diet: Can Food Affect Eczema?
Diet can play a role in managing eczema. While food is not always the cause of eczema, certain foods can trigger flare-ups in some individuals. Common triggers include:
Dairy Products: Milk, cheese, and yogurt may exacerbate eczema in sensitive individuals.
Eggs: Another common food allergen linked to eczema flare-ups.
Nuts and Shellfish: These are often associated with allergic reactions that worsen eczema.
Gluten: Some people with eczema may have sensitivity to gluten, which could lead to flare-ups.
Conversely, a healthy diet rich in anti-inflammatory foods can support overall skin health. Foods like:
Fatty Fish (salmon, mackerel) high in omega-3 fatty acids.
Fruits and Vegetables that are rich in antioxidants.
Probiotics: Found in yogurt or fermented foods, may help strengthen the skin barrier.
It’s important to consult with a doctor before making dietary changes, especially if allergies or sensitivities are suspected.
Long-Term Management of Eczema
Eczema is a chronic condition, so long-term management focuses on preventing flare-ups and maintaining skin health over time.
Consistent Moisturization: Maintaining hydration with thick moisturizers like petroleum jelly helps protect the skin barrier.
Avoiding Known Triggers: A detailed allergy test can help identify triggers like certain foods, dust, or pets.
Stress Management: Since stress can trigger flare-ups, practices such as yoga, mindfulness, and regular exercise can improve both mental and skin health.
Follow-Up Care: Regular check-ups with a healthcare provider are important to track progress, adjust treatments, and prevent complications.
A long-term eczema care plan should be comprehensive, involving daily skin care, trigger avoidance, and healthy lifestyle choices to manage flare-ups.
Safety and Precautions in Eczema Treatment
When managing eczema, safety is a priority, particularly when using topical treatments, medications, or home remedies. Here are some key precautions:
Steroid Use: Topical steroids should be used sparingly, especially for children, to avoid thinning of the skin or other side effects. Always follow the doctor’s directions for dosage and application.
Avoid Self-Diagnosis: Always seek medical advice before trying new treatments, as some remedies or over-the-counter medications may worsen symptoms.
Patch Testing: For those trying new skincare products or natural remedies, conduct a patch test on a small area of skin to check for any allergic reactions.
Phototherapy Risks: Although effective, light therapy requires monitoring to prevent overexposure to UV light, which can lead to skin aging and increased cancer risk.
Maintaining safety involves using the correct treatments for your condition and following medical advice carefully.
Eczema Myths and Misconceptions
There are many myths surrounding eczema that can lead to misunderstandings about the condition. Let's clear up some of the most common misconceptions:
Eczema is contagious: False. Eczema is not contagious. It’s an immune system response to certain triggers.
You can outgrow eczema: Not always true. While many children outgrow eczema, some adults continue to experience symptoms throughout their lives.
Eczema is caused by poor hygiene: False. Eczema is related to genetics, the immune system, and environmental factors, not poor hygiene.
All eczema patients need steroids: False. Many people can manage eczema with moisturizers, topical calcineurin inhibitors, and lifestyle changes, reducing the need for steroids.
Eczema always leads to severe complications: False. With proper management, most people can control their symptoms and prevent complications such as infections.
By debunking these myths, individuals can have a clearer understanding of eczema and its treatment options.
Eczema and Mental Health: Addressing Emotional Impact
Living with eczema can have a significant emotional and psychological impact. The visible nature of the condition, coupled with constant discomfort, often leads to stress, anxiety, and self-esteem issues. Individuals with eczema may feel self-conscious about their appearance, especially during flare-ups, which can affect their social interactions and overall mental health.
Stress and Flare-Ups: Stress is both a trigger and a consequence of eczema. Managing stress through techniques like deep breathing, mindfulness, or meditation can help prevent flare-ups and improve emotional well-being.
Body Image: The appearance of eczema lesions can lead to negative body image. Support groups, therapy, or counseling may help individuals cope with feelings of embarrassment or frustration.
Mental Health Support: Seeking professional support for mental health, such as therapy or counseling, can provide coping strategies and emotional relief, helping individuals manage the stress associated with living with eczema.
The emotional burden of eczema is real, and addressing mental health is an important part of overall eczema management.
Support and Resources for Eczema Patients
For individuals managing eczema, support and resources are vital in helping them cope with the condition. These resources can offer valuable information, community support, and practical advice on managing eczema.
Support Groups: Online forums and in-person support groups allow individuals to connect with others who are facing similar challenges. Sharing experiences can reduce feelings of isolation and provide emotional support.
Educational Resources: Reputable sources such as the American Academy of Dermatology (AAD) and National Eczema Association offer comprehensive information about eczema treatment options, tips for flare-up management, and the latest research in the field.
Professional Help: Dermatologists and allergists can offer expert advice and treatment plans tailored to an individual's needs. Additionally, mental health professionals can assist in addressing any emotional concerns tied to eczema.
Access to support systems and accurate information plays a key role in empowering individuals to manage eczema effectively.
Cost of Eczema Treatment: What to Expect
The cost of eczema treatment can vary depending on the severity of the condition, the treatments prescribed, and where the patient is located. Here are some cost-related factors to consider:
Medications: Topical treatments like steroids or calcineurin inhibitors are often covered by insurance. However, biologic treatments, which are used for severe eczema, can be expensive and may not always be covered fully by insurance.
Doctor Visits: Regular visits to dermatologists for check-ups or new treatments can add to the cost, especially for individuals without insurance or those seeking specialized care.
Over-the-Counter Products: Emollients, moisturizers, and other products to maintain skin health can also accumulate in cost, though many of these are essential for long-term management.
While eczema treatment can be costly, exploring insurance options and using generic products or subsidies may help reduce expenses.
Conclusion
Eczema is a chronic but manageable condition. With the right treatment plan, lifestyle changes, and emotional support, individuals can effectively control their eczema and reduce flare-ups. The key to successful eczema management lies in a personalized approach that combines medical care, daily skincare routines, and stress management.
Comprehensive Care: The most effective treatment involves a combination of medical treatments (topical steroids, non-steroidal options, phototherapy) and self-care measures (moisturizing, trigger avoidance).
Long-Term Management: Eczema requires ongoing management, but with the right strategies in place, individuals can live comfortably with the condition.
Support and Empowerment: Connecting with healthcare professionals, support groups, and educational resources can empower individuals to take control of their condition and improve their quality of life.
By recognizing the importance of comprehensive care, mental health, and support systems, those with eczema can successfully navigate the challenges of this skin condition, leading to healthier skin and a better quality of life.