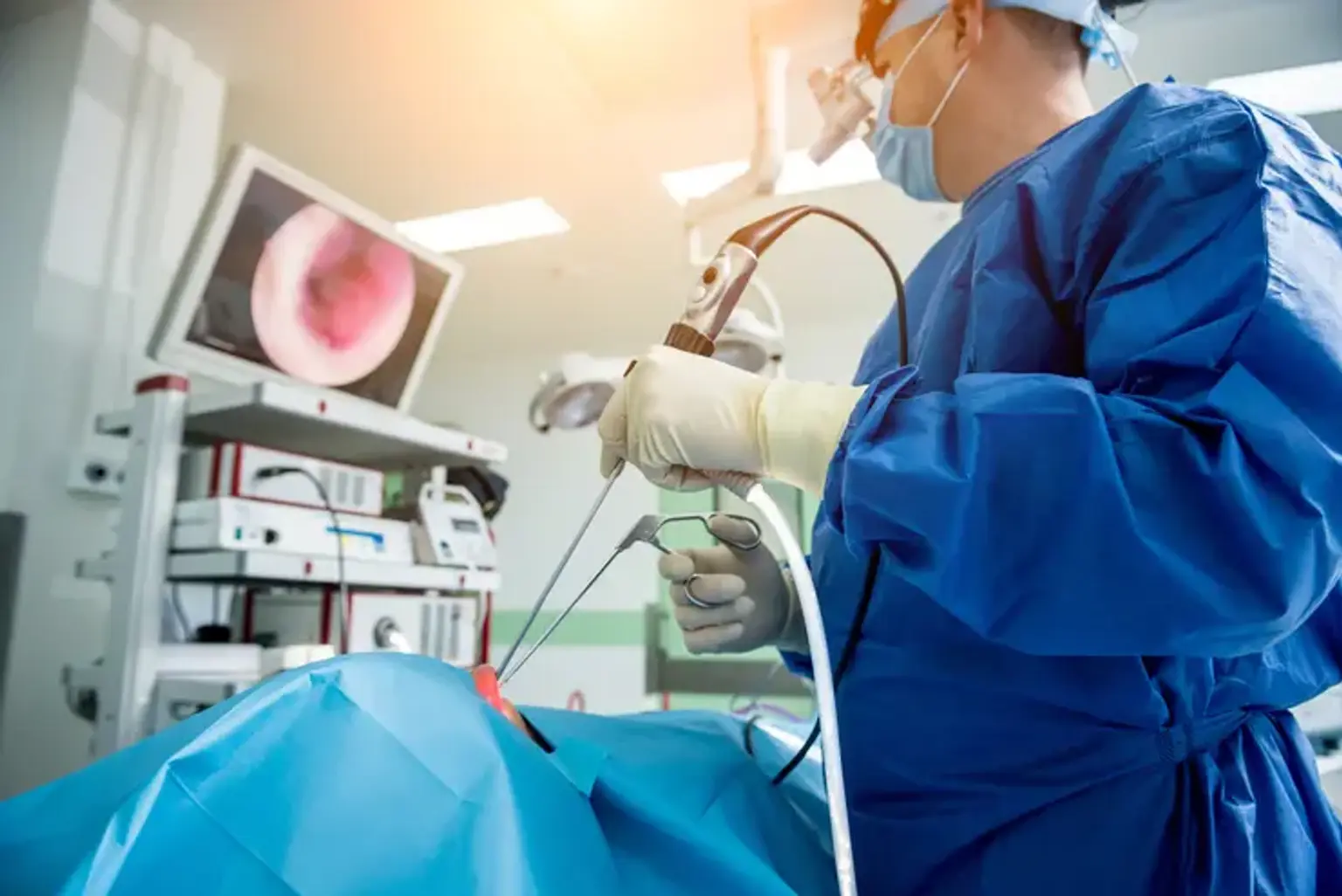
Endoscopic Laser Treatment
Overview
Laser research towards medical applications began shortly after its invention in 1960. Even the earliest research revealed that this unique technology had a high therapeutic potential.
Since those early studies, low-power lasers have been employed in diagnostic and therapeutic applications in a wide range of medical fields. However, due to uncertainty about the mechanism of action by which therapy is achieved and a lack of consensus protocols for certain applications due to the large number of parameters (e.g., frequency, energy, treatment timing, positioning) that can be selected, this modality of therapy remains highly controversial.
Using a tiny fiber led to the tumor tissue, a laser may be focused to a specific location of the brain. The laser transfers energy, which warms up the tissue surrounding the laser fiber's tip. High temperatures can induce irreversible tissue damage.