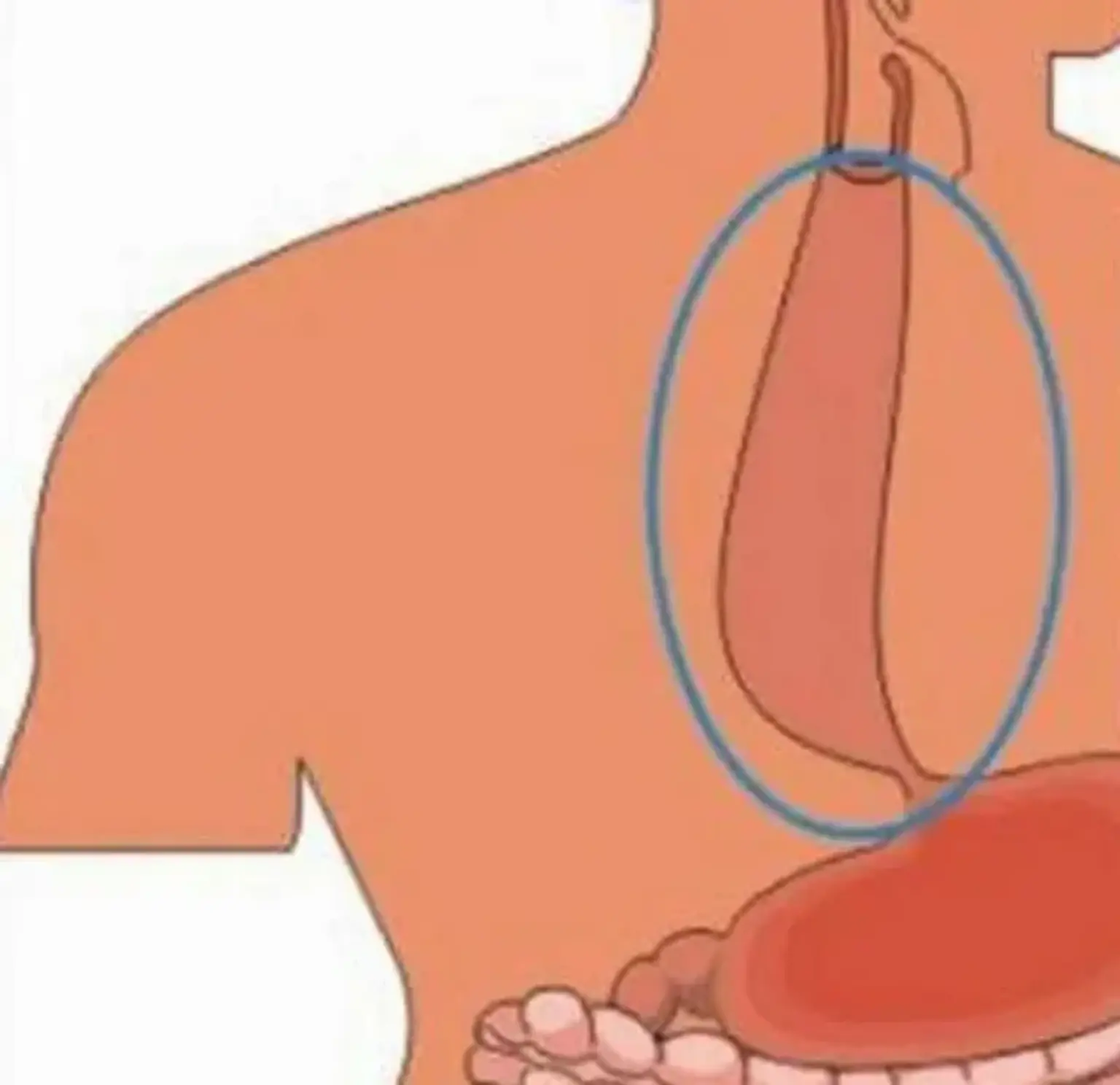
Esophageal achalasia
Overview
Esophageal achalasia is a primary esophageal motility condition of unknown origin that is defined by a lack of peristalsis and a partial or absent relaxation of the lower esophageal sphincter in response to swallowing. In institutions with a multidisciplinary approach, treatment should be personalized to the individual patient. For individuals who have failed previous treatment measures, esophageal resection should be considered as a last option.
What is esophageal achalasia?
Achalasia is a rare medical condition. The majority of doctors will never see a patient with this esophageal smooth muscle motility issue, which arises when the lower esophageal sphincter fails to relax. Peristalsis is also lacking in the esophagus. The lower esophageal sphincter is hypertensive in fewer than half of individuals. The gastroesophageal junction becomes functionally obstructed as a result of this disease.
Achalasia is characterized by swallowing difficulties, regurgitation, and, in some cases, chest discomfort. Esophageal manometry and barium swallow radiography investigations are used to make a diagnosis. There are several therapies available, but none of them cure the illness. In certain situations, medicines or Botox may be utilized, although esophageal dilatation and surgical muscle cleaving provide more lasting relief (Heller myotomy).
Epidemiology
Achalasia is very uncommon, with a yearly incidence of around one per 100,000 persons and a frequency of ten per 100,000. It does not primarily impact people of a certain age, color, or gender. However, a recent research found a rise in hospitalizations and related expenses for achalasia in the United States over the previous 16 years, with a disproportionate increase among patients under the age of 65 and ethnic minorities.
Achalasia is more common in those who have had a spinal cord injury for unexplained reasons, however these cases usually involve damage to the cervical and thoracic vertebrae.
Individuals suffering from anorexia nervosa have altered esophageal motility, which is akin to achalasia. There have been cases of achalasia following endoscopic sclerotherapy for varices. The more sclerotherapy treatments you have, the more likely you are to develop achalasia. The majority of these individuals will have hypotensive peristalsis and a dysfunctional lower esophageal sphincter.
Outside of the United States, the prevalence of achalasia ranges from 0.1 to 1 per 100,000 persons each year. According to studies, recurrence rates are greater if pneumatic dilatation was used as the first therapy. However, problems have been shown to be much greater in individuals who had a Heller myotomy compared to those who had pneumatic dilatation.
Males and females are equally affected by achalasia. The condition commonly affects persons in their second to fifth decades of life, with a peak occurrence between the ages of 30 and 60. In general, children under the age of 16 account for fewer than 2% to 5% of all cases.
Etiology
Achalasia is hypothesized to be caused by degeneration of the lower esophageal sphincter's myenteric plexus and vagus nerve fibers. At the esophageal myenteric plexus, inhibitory neurons containing VIP and nitric oxide synthase are lost, but in severe cases, cholinergic neurons are also affected. Although several explanations have been offered, the precise cause of this degeneration remains unknown.
Among these possibilities are an autoimmune reaction, a viral infection, and a hereditary predisposition. The majority of cases seen in the US are primary idiopathic achalasia; however, secondary achalasia can occur in Chagas disease caused by Trypanosoma cruzi, esophageal infiltration by gastric carcinoma, eosinophilic gastroenteritis, lymphoma, certain viral infections, and neurodegenerative disorders.
Pathophysiology
The esophagus not only transports food bolus from the mouth to the stomach, but it also prevents back reflux of stomach contents. This transport is accomplished by coordinated peristaltic contractions in the pharynx and esophagus, as well as relaxation of the upper and lower esophageal sphincters (LES). The smooth muscles of the lower esophageal sphincter are innervated by parasympathetic excitatory and inhibitory pathways.
Excitatory neurotransmitters like substance P and acetylcholine, as well as inhibitory neurotransmitters like VIP and nitric oxide (the most significant inhibitory neurotransmitter of the myenteric plexus), influence lower esophageal sphincter pressure and relaxation.
Achalasia patients have a deficiency of noncholinergic, nonadrenergic inhibitory ganglion cells, while their excitatory neurons are normal. Because of the paucity of inhibitory ganglion cells, there is an imbalance between inhibitory and excitatory neurotransmission. As a result, the esophageal sphincter is hypertensive and not relaxed.
Gradual neuronal degeneration causes excessive lower esophageal sphincter contractions and a lack of control. This deterioration causes a functional blockage, which causes dilatation. This dilatation causes permanent aperistalsis and exacerbates obstructive symptoms. The rationale for these alterations is unknown.
Some research has looked at the link between achalasia and genetic variants in the three nitric oxide synthase isoforms and particular Human Leukocyte Antigen (HLA) classes. One European research clearly suggests that achalasia is an autoimmune illness in which autoantibodies interact with DNA, similar to type 1 diabetes and lupus.
A genetic association study of achalasia revealed that an eight-residue insertion in the cytoplasmic tail of HLA-DQß1 confers the most potent known risk factor for achalasia, whereas two amino acid substitutions in the extracellular regions of HLA-DQa1 at position 41 and HLA-DQß1 at position 45 are independent risk factors for achalasia. This discovery was reproduced in another research, which also found that the insertion was more prevalent in southern Europeans than in northern Europeans, indicating a geographical north-south gradient among Europeans.
Clinical presentation
The majority of patients with achalasia present with dysphagia, initially with solids and then to liquids, while 70-97 percent of individuals will present with dysphagia to both solids and liquids. The most frequent presenting signs of achalasia are dysphagia and regurgitation. More than half of patients will report with chest discomfort, however esophageal emptying improvement seldom relieves the problem. Patients may have regurgitation with probable aspiration, nocturnal cough, heartburn, and weight loss due to difficulties eating as the condition develops.
Because of the inability to swallow, weight loss is frequently fast. Hiccups and trouble belching are less common symptoms. The therapy of underlying achalasia improves symptoms of dysphagia and regurgitation. The most prevalent extra-esophageal symptoms are structural or functional pulmonary problems caused by repeated aspiration or tracheal compression from a dilated esophagus.
The appearance of a "bullfrog neck" might result from significant dilatation and distortion of the cervical esophagus, which can lead to tracheal blockage and stridor. Although one Iranian study found that chest pain was more frequent in women, another study found that chest pain was more common in individuals under the age of 40. Symptom distribution varies depending on the demographic investigated.
Late-Stage Achalasia
End-stage achalasia, characterized by a massively dilated and convoluted oesophagus, may arise in previously treated patients when further dilatation or myotomy fails to cure dysphagia or prevent nutritional deterioration, and oesophagectomy may be the sole alternative.
We present two individuals who had end-stage achalasia and nutritional failure after receiving extensive conventional treatment such as pneumatic dilatation and surgical myotomy. Both patients were effectively handled by transhiatal oesophageal oesophagectomy and cervical gastro-esophageal anastomosis, resulting in good symptom management and increased quality of life. These examples are explored, as well as the literature.
End-stage illness, defined by a significantly dilated and convoluted "burned-out" oesophagus with recurring obstructive symptoms, may necessitate oesophageal resection to restore gastro-intestinal function, reverse nutritional deficiencies, and lower the risk of aspiration pneumonia.
How to diagnose esophageal achalasia?
Because symptoms do not consistently detect achalasia, diagnostic investigations to confirm the condition must be performed when there is clinical suspicion of achalasia. In addition, it is critical to rule out both benign and malignant causes of lower esophageal blockage.
A barium esophagogram is the best first test for diagnosing achalasia (barium swallow). The smooth tapering of the lower esophagus to a "bird's beak" look on the barium swallow, with dilatation of the proximal esophagus and absence of peristalsis during fluoroscopy, is the classic finding on the barium swallow. Some instances show an air-fluid level and the lack of intra-gastric air, whereas in severe illness, the esophagus may have a sigmoid-like shape.
To assess esophageal emptying, a timed barium swallow is utilized. This variation on the conventional barium swallow involves having the patient consume 236 ml of barium while standing upright and capturing radiographs one, two, and five minutes after the final swallow. Pre and post-treatment measurements include the height of the barium column after five minutes and the esophageal breadth.
Esophagogastroduodenoscopy
Upper endoscopy (esophagogastroduodenoscopy - EGD) is recommended in all patients with suspected achalasia or dysphagia in order to rule out premalignant or malignant esophageal lesions. EGD has a limited diagnostic accuracy for achalasia and may be normal in the early stages of the illness. In severe instances, the esophagogastric junction may form a rosette or the esophagus may become dilated, convoluted, and atonic, typically with retained food and saliva.
Because to persistent stasis, the esophagus may be normal or display signs of esophagitis. A strong resistance to the scope passing through the esophagogastric junction, particularly in an elderly patient or one with a short duration of symptoms and severe weight loss, should raise the possibility of pseudoachalasia, particularly malignancy. CT scans, endoscopic ultrasonography (to rule out submucosal lesions), and transabdominal ultrasound are also effective in cases of pseudoachalasia.
Esophageal manometry
The gold standard for diagnosing achalasia is esophageal manometry, which is the most sensitive test. Manometry will demonstrate insufficient lower esophageal sphincter relaxation in response to swallowing, as well as a lack of peristalsis in the lower esophagus and an increase in lower esophageal sphincter pressure. High-resolution manometry (HRM), which incorporates pressure topography charting, has mostly replaced traditional manometry.
Achalasia is divided into three separate types using HRM, according to the Chicago criteria (version 3.0), which have prognosis and therapeutic implications. All three types have incomplete lower esophageal sphincter relaxation. Type 1 has aperistalsis and no esophageal pressurization, type 2 has aperistalsis and panesophageal pressurization in 20% or more of swallows, and type 3 has spastic (premature) contractions with a distal contractility integral (DCI) greater than 450 mmHG-s-cm in 20% or more of swallows.
The integrated relaxation pressure in type 1 achalasia is 10mmHg, 15mmHg in type 2 achalasia, and 17mmHg in type 3 achalasia. Type 2 achalasia had the most good therapy response, whereas type 3 had the least favorable treatment response. Conservative methods such as pneumatic dilatation and surgical myotomy are the best initial treatment options for types 1 and 2, although type 3 achalasia appears to react better to early therapy with peroral endoscopic myomectomy.
Recommended Courses of Action
- Esophageal manometry reveals insufficient lower esophageal sphincter relaxation in response to ingestion, excessive resting lower esophageal sphincter pressure, and no esophageal peristalsis.
- Long-term esophageal pH monitoring to rule out gastroesophageal reflux disease and see if the therapy creates aberrant reflux.
- EGD (esophagogastroduodenoscopy) to rule out malignancy of the gastroesophageal junction or fundus.
- Concomitant endoscopic ultrasonography if a tumor is suspected
Biopsy
Biopsies, or the removal of a tissue sample during endoscopy, are not usually required in achalasia, but if conducted, they reveal hypertrophied muscle and the lack of particular nerve cells of the myenteric plexus, a network of nerve fibers that regulates esophageal peristalsis. Achalasia cannot be diagnosed just by a biopsy.
Management
The treatment for achalasia is to reduce the outflow resistance produced by a non-relaxing and hypertensive lower esophageal sphincter. Nonsurgical and surgical treatments are now available for primary idiopathic achalasia. Pharmacotherapy, endoscopic botulinum toxin injection, and pneumatic dilatation are nonsurgical alternatives. Laparoscopic Heller myotomy (LHM) and peroral endoscopic myotomy (PEM) are surgical alternatives (POEM).
- Pharmacotherapy
To relieve lower esophageal sphincter (LES) pressure, pharmacologic therapies include nitrates, calcium channel blockers, and phosphodiesterase-5 inhibitors. Calcium channel blockers prevent calcium from entering cells, preventing smooth muscle contraction and lowering LES pressure. Its usage is limited by hypotension, pedal edema, headache, quick tolerance development, and partial symptom relief.
Nitrates raise nitric oxide concentrations in smooth muscles, resulting in a rise in cyclic adenosine monophosphate levels and smooth muscle relaxation. These therapies are less effective, only give short-term alleviation of symptoms, and are usually reserved for patients who are awaiting or have declined more definite treatment, such as pneumatic dilatation or surgery.
- Endoscopic botulinum toxin injection
In high-risk patients or those who relapse following myotomy, endoscopic injection of botulinum toxin can be employed. Botulinum toxin, generated from Clostridium botulinum, is a powerful biological neurotoxin that inhibits acetylcholine release at the lower esophageal sphincter.
This treatment can be used in individuals who are not candidates for surgery or dilatation, or as a bridge to more definitive treatments. Botulinum toxin injections have limitations in that the impact is short-lived (lasting around 6 to 12 months), patients frequently require several treatments, which are costly, and they may impair the effectiveness of later surgical myotomy.
- Pneumatic dilatation
The most cost-effective non-surgical treatment for achalasia is pneumatic dilatation of the esophagus via endoscopy. A graduated dilator technique is used to dilate the esophagus by disturbing the circular fibers of the LES using air pressure. Symptoms improve in 50% to 93% of patients; nevertheless, 30% of individuals experience symptom recurrence after five years.
Repeat pneumatic dilatation on-demand will offer long-term remission in certain individuals with symptom recurrence. When compared to myotomy, on-demand repeat pneumatic dilatation provides comparable long-term symptom alleviation. Male gender, younger patients (age less than 40), those with pulmonary problems, or failure of one or more previous pneumatic dilatations all have a greater failure risk with pneumatic dilation. When compared to older men or women, graduated pneumatic dilatation using a 3.0 cm balloon is more likely to fail in young males. In addition, commencing with a 3.0 cm ballon increases the likelihood of failure in this group of patients.
The most frequent procedure-related consequences are mild, although serious complications such as esophageal perforation might occur and should be handled as such. When surgery fails, the initial therapy option is pneumatic dilatation. If this also fails, imaging investigations must be used to determine the cause of the failure before attempting a second surgery.
Esophageal achalasia surgery
Surgical myotomy, which can be performed laparoscopically, is the preferred procedure for lowering pressure across the lower esophageal sphincter. This technique will relax the lower esophageal sphincter by cutting the circular muscle fibers that run over it.
Because laparoscopic Heller myotomy has the potential to produce uncontrolled gastroesophageal reflux, it is usually combined with an anti-reflux treatment like Nissen, the posterior (Toupet), or the anterior (Dor) partial fundoplication. The anterior fundoplication is the preferred method. The surgical treatment of choice is laparoscopic Heller myotomy (LHM) with partial fundoplication.
The crucial point is that the fundoplication be partial rather than total to avoid postoperative dysphagia, which is more severe with Nissen fundoplication. At 35 months, the clinical success rate of LHM is substantial (76 to 100 percent), with a low death rate of 0.1 percent. After five years, disease progression diminishes the success rate.
In a few places, peroral endoscopic myotomy (POEM) is an effective minimally invasive alternative to laparoscopic Heller myotomy for treating achalasia. Endoscopic dissection of the LES's circular fibers results in LES relaxation; nevertheless, the risk of gastroesophageal reflux is substantial since it does not involve an antireflux technique. Esophagectomy is only used as a last option.
When a patient presents with dysphagia, the diagnosis of malignancy should always be in view.
Other disorders in the differential include:
- Diffuse esophageal spasm
- Scleroderma
- Gastroesophageal reflux disease
- Stricture
- Schatzki ring
- Hiatal hernia
- Paraesophageal hernia
Prognosis
Pneumatic dilatation and laparoscopic myotomy can offer good outcomes in terms of symptom alleviation. Although esophageal perforation is uncommon following pneumatic dilatation, relapses are common.
Even after effective achalasia therapy, swallowing may decrease with time. The esophagus should be evaluated every year or two with a timed barium swallow since some people may require pneumatic dilatations, a repeat myotomy, or possibly esophagectomy after a long period of time. Furthermore, some doctors advocate pH testing and endoscopy to look for reflux damage, which can progress to Barrett's esophagus or a stricture if left untreated.
Complications
- Esophageal perforation
- Recurrence
- Gastroesophageal reflux disease
- Bloating
- Potential cancer risk
Conclusion
Esophageal achalasia is a condition of esophageal motility that affects the smooth muscle layer of the esophagus and the lower esophageal sphincter (LES). In the absence of other causes such as cancer or fibrosis, it is characterized by insufficient LES relaxation, elevated LES tone, and a lack of esophageal peristalsis (inability of smooth muscle to convey food down the esophagus). The purpose of achalasia treatment is to alleviate symptoms by removing the outflow resistance generated by the hypertensive and nonrelaxing LES.