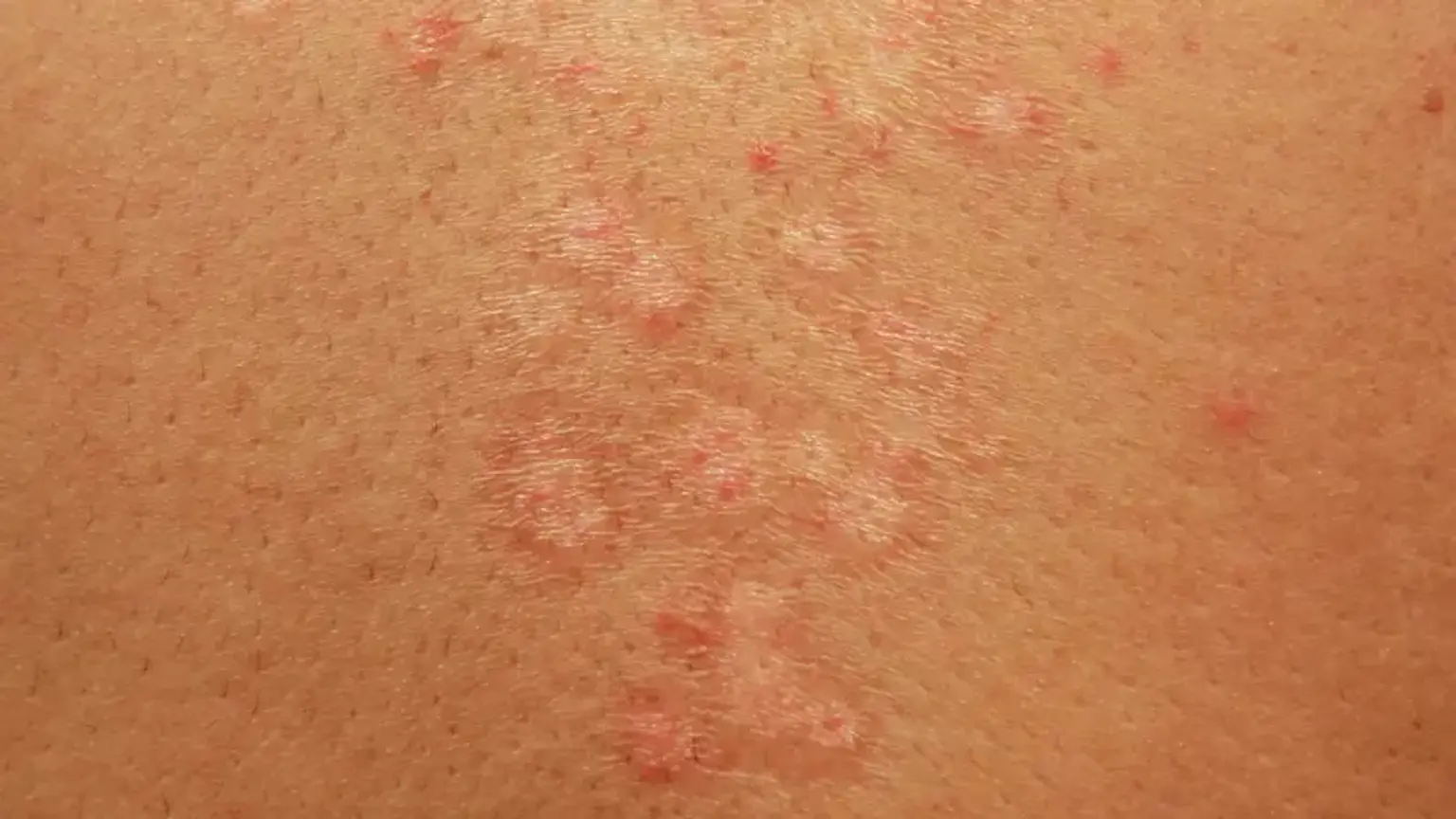
Understanding Fungal Skin Infections
Fungal skin infections, or mycoses, happen when fungi grow on the skin, hair, or nails. These infections are common and can affect anyone. The most frequent types include athlete’s foot (tinea pedis), ringworm (tinea corporis), and jock itch (tinea cruris).
Symptoms vary but often include itching, redness, peeling, or rashes. Some infections cause blisters or cracks in the skin. Warm, moist environments like locker rooms or sweaty clothing increase the risk.
Fungi spread through direct skin contact, contaminated surfaces, or infected pets. People with weakened immune systems, diabetes, or excessive sweating are more vulnerable.
Timely treatment is important to prevent spreading or worsening symptoms. Mild cases respond well to over-the-counter antifungal creams, while severe infections may need prescription medication.
Topical Antifungal Treatments
Topical antifungals are the first line of defense for most fungal skin infections. These medications come in creams, lotions, sprays, and powders.
Azoles (clotrimazole, miconazole, ketoconazole) disrupt fungal cell membranes.
Allylamines (terbinafine, naftifine) block fungal growth, stopping the infection.
Ciclopirox prevents fungi from producing necessary proteins, killing the infection.
These treatments should be applied consistently for a few weeks, even after symptoms disappear, to prevent recurrence.
For mild infections, over-the-counter options work well. If symptoms persist or worsen, a stronger prescription cream may be needed.
Oral Antifungal Medications
For severe or widespread infections, doctors may prescribe oral antifungal medications. These drugs work from within the body to eliminate fungi.
Terbinafine is often used for nail and scalp infections.
Itraconazole treats a range of fungal infections, including ringworm.
Fluconazole is effective against yeast infections like candidiasis.
Oral antifungals are strong and require medical supervision. They can cause side effects such as nausea, liver issues, or allergic reactions. Patients with liver disease or certain health conditions should consult a doctor before use.
These medications are usually taken for weeks or months, depending on the severity of the infection.
Preventative Measures and Hygiene
Preventing fungal infections is key to avoiding recurring issues. Proper hygiene and lifestyle changes help reduce the risk.
Keep skin dry and clean – Fungi thrive in moisture. Dry feet and skin folds properly.
Wear breathable clothing – Loose, cotton fabrics help prevent excessive sweating.
Avoid sharing personal items – Towels, socks, and shoes can spread fungi.
Use antifungal powders or sprays – These help absorb moisture and prevent infections.
Change socks and underwear daily – This reduces fungal buildup in warm areas.
Good hygiene, combined with early treatment, keeps fungal infections under control and prevents them from returning.
When to See a Doctor
While many fungal infections clear up with over-the-counter treatments, some cases require medical attention. See a doctor if:
The infection does not improve after 2–4 weeks of treatment.
The affected area becomes swollen, painful, or develops pus (signs of a bacterial infection).
You have a weakened immune system due to diabetes, cancer, or medications.
The infection spreads to multiple areas of the body.
A doctor may perform a skin scraping test to confirm the type of fungus and prescribe stronger medications if needed. Early medical intervention can prevent complications.
Natural Remedies and Home Treatments
Some natural remedies may help alongside medical treatments. While not a substitute for antifungal medications, they can provide relief.
Tea tree oil – Has antifungal properties and can be applied with a carrier oil.
Apple cider vinegar – May help balance skin pH and prevent fungal growth.
Coconut oil – Contains lauric acid, which has antifungal effects.
Garlic – Some studies suggest it has antifungal benefits when applied topically.
These remedies should be used with caution, as they may cause irritation. Always test a small area of skin before applying widely.
Common Myths About Fungal Infections
There are many misconceptions about fungal infections. Here are some common myths:
"Fungal infections only affect dirty people." – Fungi thrive in warm, moist environments, regardless of hygiene. Even clean skin can develop infections.
"Home remedies cure fungal infections completely." – While some remedies help, most fungal infections require antifungal medications to fully clear up.
"Fungal infections are not contagious." – Many types, including athlete’s foot and ringworm, spread easily through skin contact or shared surfaces.
"Once treated, fungal infections never return." – Recurrence is common, especially if hygiene and prevention measures are not followed.
Understanding the truth about fungal infections helps in managing and preventing them effectively.
Lifestyle Changes to Prevent Recurrence
Making small lifestyle changes can significantly reduce the risk of future fungal infections.
Maintain proper foot care – Wash and dry feet daily, and wear breathable shoes.
Use antifungal socks or powders – These help prevent moisture buildup.
Disinfect shoes and shower areas – Fungi can survive on surfaces for a long time.
Boost your immune system – A healthy diet, exercise, and proper sleep can improve your body’s ability to fight infections.
By following these habits, individuals can reduce the likelihood of reinfection and maintain healthy skin.
Complications of Untreated Fungal Infections
Ignoring a fungal skin infection can lead to complications, especially in people with weak immune systems or underlying health conditions. Some potential risks include:
Spread of infection – The fungus can extend to other body parts, including nails and scalp.
Secondary bacterial infections – Scratching infected areas can break the skin, allowing bacteria to enter.
Chronic infections – Some fungal infections, like nail fungus, can become persistent and difficult to treat.
Pain and discomfort – Severe infections can cause cracking, peeling, and even painful sores.
Seeking early treatment prevents these complications and speeds up recovery.
Over-the-Counter vs. Prescription Treatments
Fungal infections vary in severity, so treatment options depend on the condition’s extent.
Over-the-counter (OTC) antifungals – Available in creams, sprays, and powders, these are effective for mild cases. Common examples include clotrimazole and terbinafine.
Prescription-strength antifungals – For more stubborn or widespread infections, a doctor may prescribe stronger creams or oral medications like fluconazole or itraconazole.
Combination treatments – In some cases, doctors recommend using both topical and oral antifungals together for better results.
If OTC treatments don’t show improvement within a few weeks, consulting a doctor for a prescription is necessary.
How Long Does Treatment Take?
The duration of treatment depends on the type and severity of the infection:
Mild infections (athlete’s foot, ringworm, jock itch) – Usually clear up within 2–4 weeks with consistent topical treatment.
Moderate infections – May take 4–6 weeks, especially if the fungus has spread.
Severe or nail infections – Can require 3–6 months of oral medication for complete resolution.
Even if symptoms disappear early, it’s important to complete the full treatment to prevent recurrence.
Fungal Infections in Different Age Groups
Fungal skin infections can affect people of all ages, but some groups are more vulnerable.
Children – More prone to ringworm and scalp infections due to close contact in schools and daycare centers.
Adults – Athletes and people with active lifestyles often develop athlete’s foot and jock itch.
Seniors – More likely to develop nail fungus and chronic skin infections due to reduced immunity and poor circulation.
Each age group may require different treatment approaches, so consulting a doctor for the best option is advised.
The Role of Diet and Immunity in Fighting Fungal Infections
A strong immune system plays a crucial role in preventing and controlling fungal infections. People with weakened immunity, such as those with diabetes, autoimmune diseases, or cancer, are at a higher risk of developing severe or recurring infections.
A balanced diet rich in vitamins and minerals can help boost immune function. Key nutrients that support skin health and fungal resistance include:
Vitamin C – Strengthens the immune system and promotes skin healing (found in citrus fruits, bell peppers, and strawberries).
Zinc – Supports immune defense and wound healing (found in nuts, seeds, and lean meats).
Probiotics – Help maintain a healthy balance of bacteria and fungi in the body (found in yogurt, kefir, and fermented foods).
Antifungal foods – Garlic, coconut oil, and turmeric have natural antifungal properties and may help prevent infections.
A healthy lifestyle, combined with proper hygiene, can reduce the likelihood of fungal infections and promote faster recovery.
How Weather and Environment Affect Fungal Infections
Environmental factors significantly impact fungal infections, as fungi thrive in warm, humid conditions. Certain climates and lifestyle choices can increase the risk of developing an infection.
Hot and humid weather – Increases sweating, creating the perfect environment for fungal growth, especially in skin folds and between the toes.
Wearing tight or non-breathable clothing – Traps moisture and heat, making areas like the groin, underarms, and feet more susceptible to infections.
Public places with high humidity – Locker rooms, swimming pools, and communal showers are common sources of fungal infections due to moist surfaces.
Dry, cold weather – While fungi prefer moisture, dry skin can develop cracks, providing an entry point for infections.
To minimize risks, individuals should wear breathable fabrics, keep their skin dry, and avoid walking barefoot in public spaces.
Fungal Infections and Pets: Can They Spread to Humans?
Many fungal infections, such as ringworm, can spread between animals and humans. Cats, dogs, and even livestock can carry fungal spores on their fur or skin. If a pet has a fungal infection, it may show symptoms like:
Patchy hair loss
Scaly or red skin
Excessive scratching or licking
To prevent the spread of fungal infections from pets to humans:
Wash hands after handling animals.
Regularly clean pet bedding and grooming tools.
Take infected pets to the vet for treatment.
Children and people with weakened immune systems are at a higher risk of contracting fungal infections from pets, so extra precautions should be taken.
Psychological Impact of Chronic Fungal Infections
Chronic or recurring fungal infections can take a toll on a person’s mental health and self-esteem. Skin conditions are often visible, which can cause embarrassment, anxiety, or social discomfort. Common concerns include:
Self-consciousness about appearance – Visible infections like ringworm or nail fungus can lead to social anxiety or reluctance to wear certain clothing.
Frustration with persistent symptoms – Recurring infections can cause stress, especially if treatments take a long time to work.
Impact on daily life – Itching, discomfort, and skin damage can interfere with sleep, work, or physical activities.
Seeking timely medical treatment and practicing self-care can help individuals manage both the physical and emotional effects of fungal infections. Talking to a doctor or dermatologist about long-term solutions can also provide relief.
Advancements in Fungal Infection Treatments
Medical advancements have improved the treatment of fungal infections, making them more effective and accessible. New research focuses on:
Enhanced antifungal drugs – Scientists are developing medications with fewer side effects and better absorption, such as novel azoles and echinocandins.
Laser therapy – Used primarily for nail fungus, laser treatments target fungal cells without harming surrounding tissue.
Probiotics and microbiome research – Maintaining a healthy skin microbiome may help prevent fungal overgrowth. Some studies suggest that probiotic supplements can support fungal infection treatment.
Antifungal resistance solutions – Overuse of antifungal medications has led to resistance in some fungal strains. New treatment strategies aim to overcome this challenge.
These innovations offer promising alternatives for those struggling with recurrent or hard-to-treat fungal infections.
Global Prevalence of Fungal Infections
Fungal skin infections are a worldwide issue, affecting millions of people each year. The prevalence varies based on climate, hygiene practices, and healthcare access.
Tropical and humid regions – Countries in South America, Africa, and Southeast Asia report higher rates due to warm, moist environments that support fungal growth.
Developed nations – Although medical treatment is widely available, fungal infections remain common due to lifestyle factors like gym use, communal showers, and synthetic clothing.
Underserved areas – Limited access to antifungal medications and healthcare can lead to widespread, untreated infections.
Education on prevention, hygiene, and proper treatment is essential to reducing the global burden of fungal infections.
Frequently Asked Questions (FAQs) About Fungal Skin Infections
1. How long does a fungal skin infection last?
With proper treatment, mild infections clear up within 2–4 weeks. Severe or nail infections may take months to fully heal.
2. Can fungal infections go away on their own?
Most fungal infections do not resolve without treatment and can worsen over time. Using antifungal medications is the best way to eliminate them.
3. Are fungal infections contagious?
Yes. Many types, like ringworm and athlete’s foot, spread through skin contact or contaminated surfaces. Avoid sharing personal items and practice good hygiene.
4. Can I prevent fungal infections from coming back?
Yes. Keeping skin dry, wearing breathable clothing, and using antifungal powders can help prevent recurrence. Treat infections fully to avoid reinfection.
Conclusion
Fungal skin infections are common but manageable with the right treatment and preventive measures. Understanding the causes, recognizing symptoms early, and using effective antifungal medications can lead to successful recovery.
Key takeaways include:
Use antifungal treatments consistently – Even after symptoms fade, complete the full course of treatment.
Practice good hygiene – Keeping skin dry and clean reduces the risk of recurrence.
Seek medical help when needed – If an infection does not improve or worsens, consult a doctor for stronger treatment options.
Make lifestyle changes – Small adjustments, such as wearing breathable fabrics and avoiding damp environments, can prevent future infections.
By staying informed and proactive, individuals can effectively manage fungal infections and maintain healthy skin.