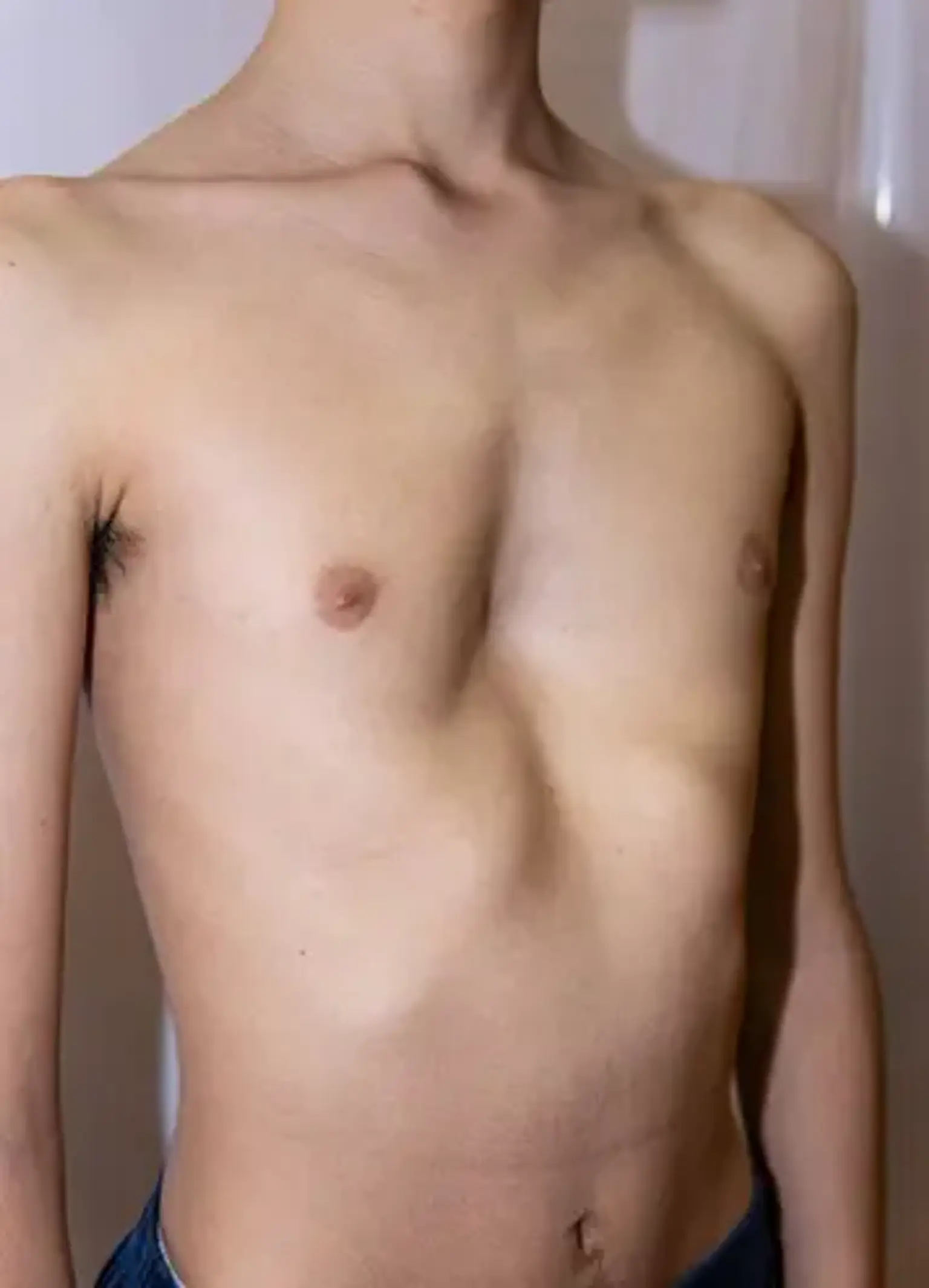
Funnel chest deformity
Overview
Pectus deformities are responsible for around 95 percent of congenital chest wall defects, with Funnel chest deformity being the most frequent. When the breastbone pulls inwards and there is a dip between the ribs, this is known as a funnel chest deformity.
Some persons who have Funnel chest have no additional symptoms. Others may suffer from impaired heart or lung function. Some persons with pectus excavatum may feel timid or self-conscious because it changes their physical form. The location of the breastbone can be corrected with treatment.