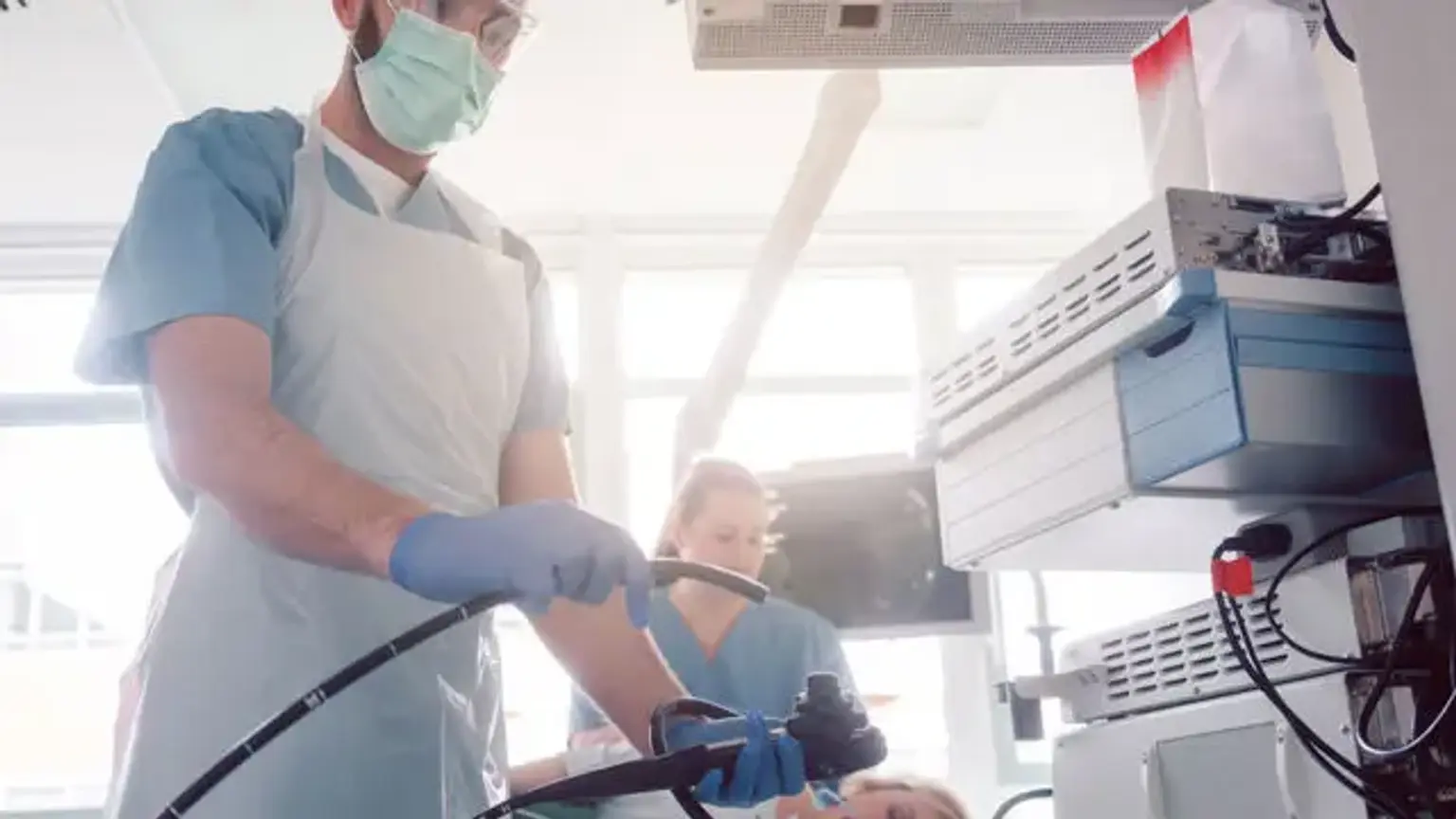
Gastroscopy
Due to the high frequency of gastric cancer in South Korea, gastroscopy could be very useful for gastric cancer screening. Gastroscopy is a valuable procedure for diagnosing a variety of upper GI tract problems. For the diagnosis of upper GI tract inflammations, ulcerations, and malignancies, gastroscopy has higher sensitivity and specificity than radiography such as an upper GI barium series. Because gastroscopy is one of the most popular procedures in South Korean clinical practice, beginners, especially primary care doctors, are eager to learn the skills and expertise required for this procedure. It's critical for new gastroscopy practitioners to have a theoretical understanding of pathological GI diseases in order to appropriately evaluate data during endoscopic procedures and make the best therapeutic decision possible. Even those with a thorough theoretical understanding of pathological lesions may wind up doing an incomplete examination if they are unable to correctly introduce the scope into the examinee's mouth or push it along each section of the upper GI tract. Furthermore, it is vital to examine carefully throughout the procedure, taking into account the likelihood of blind spots, in order to avoid missing any problematic lesions. As a result, performing a successful gastroscopy without procedural skills is almost difficult. As a consequence, an early session of endoscopic training programs should focus on upper GI endoscopy procedural skills.
Gastroscopy Definition
A gastroscopy allows doctors to examine the upper gastrointestinal tract in detail. This includes the tube (esophagus) through which food flows on its way to the stomach, as well as the stomach and the small intestine's first bend (duodenum).
To do so, doctors utilize thin, flexible tubes (gastroscopes or endoscopes) with a light at one end. An endoscopist, a particularly trained doctor or nurse, passes it through the mouth, down the esophagus, and into the stomach. The tube is as thin as your index finger. It will not obstruct breathing at any moment because it travels down the food pipe rather than the windpipe.
The tube is put past the back of the throat, causing you to gag or retch. Once the tube enters the food pipe, this will subside. Small tissue samples (biopsies) are sometimes obtained and sent for testing. The biopsies that are taken are about the size of a match head and will not hurt you.
If you have been advised that you will be receiving treatment or therapy during the gastroscopy, the doctor or nurse specialist will let you know how long the procedure will take and what to expect.
Gastroscopy Indications
A gastroscopy can aid in the diagnosis and monitoring of a variety of ailments, including:
- Low blood iron levels (are known as anemia)
- Cancer
- Conditions affecting the digestive system such as celiac disease, indigestion gastro-esophageal reflux disorder (GERD), and ulcers in the stomach.
- Infection
- Inflammation
- Polyps (noncancerous growths that can turn cancerous later)
If you experience any of the following symptoms, the doctor may advise you to have a gastroscopy:
- Pain in the abdomen
- Bleeding
- Stools with blood or stools that are dark black
- Long-term heartburn and/or indigestion
- Swallowing problems (dysphagia)
- Unexplained weight loss and/or vomiting
Small tissue samples (biopsies) can also be taken during a gastroscopy using devices passed through the gastroscope. After that, the biopsies will be sent to a lab for analysis.
By sending instruments through the gastroscope, a gastroscopy can also be utilized to treat specific problems. Gastroscopies for therapeutic purposes can be used in the following:
- Removal of any things that have been lodged in the throat.
- Removal of polyps and other minor growths.
- Stop the bleeding from varices (swollen veins) or peptic (stomach) ulcers.
- Expand an esophagus that is too narrow
Preparation for Gastroscopy
Eating and Drinking
The stomach must be entirely empty for the endoscopist performing the gastroscopy to get a proper view, so you must fast for at least 6 hours before the procedure. Small amounts of water can be taken up to 2 hours before your examination.
When you arrive at the unit, you will wait in the waiting room until a nurse sees you and asks about your health information. Inform the nurse if you have had any previous reactions or sensitivities to examinations.
You will not need to change for the procedure; however, nurses may ask you to cover your clothes with a gown to protect them. Then, You will be transferred to the waiting room.
Your endoscopist will go over the procedure with you and answer any questions you may have. Before your procedure, you should have had the opportunity to discuss any medications you're taking with one of the nurses or doctors.
Medications
Unless you've been told otherwise, take your regular medications with a few sips of water as usual.
If you have diabetes, whether it's controlled with pills or insulin, tell the doctor at least one week before the gastroscopy.
If you are using any blood thinning or antiplatelet treatment, such as Warfarin, Dabigatran, Apixaban, Rivaroxaban, or Clopidogrel, let the doctor know as soon as possible because you may need to discontinue taking these prescriptions for a short period of time before the procedure.
If you're using a strong anti-acid medication such as Omeprazole (Losec) Esomeprazole (Nexium), Lansoprazole (Zoton), Pantoprazole (Protium), and Rabeprazole (Pariet) discontinue using them two weeks before to the procedure.
If you are concerned that the symptoms will worsen, seek counsel from the doctor. If you've been informed you have an ulcer in your esophagus, stomach, or small bowel and need a repeat gastroscopy to see if it's healed, or if you've been diagnosed with Barrett's Esophagus and require a surveillance Gastroscopy, don't stop taking the anti-acid medication you've been recommended.
You will not be able to drive home or use public transportation if you choose to get sedation. You must have a family member or friend pick you up from the Endoscopy Unit and an adult stay with you overnight because anesthesia makes you forgetful and it lasts for a day in your bloodstream.
Arranging an Escort
If you decide on sedation, you must plan for a friend or relative to drive you home following the test, which should take around an hour. This person must be at least 18 years old.
Someone should stay with you overnight if possible. For the rest of the day, you won't be able to drive or operate any machinery, and you will need to sleep quietly at home. If you want to receive sedation but haven't arranged for an escort home, your procedure will be canceled on the day.
Preparation Checklist
- Arrange for a friend or relative (18 years of age or older) to accompany you home following the examination if you are planned or have been advised to receive sedation. If you do not arrange for an escort or if they are under the age of 18, the anesthesiologist will be unable to provide sedation and the treatment may be canceled.
- Make a note of the appointments' time and date.
- Before your appointment, if you are taking blood thinners, inform the doctor for advice.
- 6 hours before your visit, don't eat or drink anything.
- Sips of water are permitted up to 2 hours before your visit.
- On the day of the test, wear loose-fitting clothing.
What Options are Available to Help During Gastroscopy?
Anesthetic throat spray. This is a local anesthetic spray that is sprayed into the back of the throat and has the same effect as a dental injection. This medication will numb the throat, making it easier for the gastroscope to pass through.
The advantage of using throat spray is that you will be fully aware of the procedure and the Endoscopist will be able to communicate with you during the procedure. After the inspection, you will be free to go home unsupervised and continue with your day as usual.
Needle sedation. If you're nervous about the procedure, a sedative injection can help you relax. It can make you sleepy, which can help you bear the procedure better. A sedative differs from a general anesthetic in that its goal is to help you relax rather than to knock you out.
You will not be able to drive home or use public transportation if you choose to get sedation. You must have a friend or relative pick you up from the Endoscopy Unit, and an adult must stay with you overnight.
You can also have both a local anesthetic throat spray and sedation as part of the procedure, which is deemed safe. When you sign the consent form, you can explore these possibilities with the Endoscopy nurse.
The manner people react to this procedure and the sedation varies a lot. The technique is safe, but it can be unpleasant and slightly uncomfortable. Doctors intend to employ sedation to help you in relaxing within safe limits. They do not intend to put you to sleep, but they will do everything they can to make the treatment as painless as possible.
Before the Gastroscopy
Be aware that the endoscopist teams may be in charge of different procedure rooms at once. This implies that a patient who arrived later than you might be called in first. This does not indicate that you have been overlooked; rather, the other individual is on a different list than you.
Doctors try everything to keep you waiting as few as possible, but it's difficult to give specific times because each procedure takes a varying period of time. Doctors will keep you updated on how long you'll be in the department but plan on spending the entire morning or afternoon in the ward, depending on whether you're a morning or afternoon admittance.
Doctors also handle emergency situations. They may have to deal with them first, in which case they will ask you to wait. Accept their apologies if this occurs, however, if you are concerned, wait and check at the service counter.
Gastroscopy Procedure
The evaluation will take place in one of the procedure facilities, where you will be asked to remove the shoes, loosen any tight clothing, and remove any false teeth or spectacles. You'll need to maintain track of your belongings at all times.
For the evaluation, you will be offered either sedation or an anesthetic throat spray. The endoscopist will have already discussed the one you are getting with you. If you choose sedation, a tiny tube will be put into your arm or hand (cannula) with a needle and an injection will be administered via it.
If you need throat spray, you will be given a local anesthetic spray to numb the back of your throat and relieve the pain. Gagging and retching will continue to occur as a natural reaction to the endoscope contacting the back of the throat.
On a trolley, you will be put on the left side. During the procedure, you will be accompanied by a nurse. A mouthpiece will be put between the teeth to keep your mouth partially open. The nurse will likely place the mouthpiece in your mouth and use a sucker to remove any drool.
Through the mouthpiece, the gastroscope will be softly placed into the mouth and carried down into the stomach. To acquire a better view, the endoscopist will blow air down the gastroscope. This may cause you to feel bloated, but it will not be irritating.
A biopsy may be performed on occasion. Using small forceps, the tissue is extracted through the gastroscope. It's unlikely that this causes discomfort, but if it does, it should go away quickly. Most likely, you will merely feel a tugging feeling.
What Happens after Gastroscopy?
You will be brought to the recovery area following the procedure.
If you just had a local anesthetic spray, you will be requested to sit on a chair and have your blood pressure, pulse, and oxygen saturation measured. If you have diabetes, your blood sugar may need to be checked again. You must wait at least 30 minutes for the effects of the local anesthetic to wear off. You will then be provided tea/coffee and biscuits as a refreshment. If you prefer not to wait for the refreshments, a member of staff will send you home with information on when you can eat and drink. Inform a member of staff so that he can help you with your discharge. When you're ready to leave, a member of staff will take you to a private room where the doctor can go over the endoscopic results with you. You will receive a copy of the gastroscopy report.
If you've been sedated, you'll be kept on the trolley for at least an hour to allow you to recover. Every 15 minutes, the blood pressure, pulse, and oxygen saturation will be monitored. If you have diabetes, your blood sugar may need to be checked again. You will be served refreshments such as tea/coffee and biscuits once you have fully recovered from the sedation. The plastic cannula that was used to provide the anesthesia will be removed as well. Because the sedative can cause you to forget things and make you feel sleepy and drowsy for at least 24 hours, doctors strongly advise you to have someone stay with you overnight. You must not drive, consume booze, operate heavy machinery, or sign any legal documents for 24 hours after your sedation. If the person who was supposed to pick you up has left the department, a member of staff will call them when you're ready to leave. You will be transported to a private room where a member of staff will go over all of your discharge information with you once your escort arrives. You may be transferred from the department after this if you feel ready. Your endoscopy report will be provided to you.
Gastroscopy Complications
For the most part, a gastroscopy is a painless procedure with few major complications. Any issues that may arise are detected and treated by the endoscopy specialists. The following are some of the potential dangers:
- A tear in the lining of the esophagus, stomach, or duodenum (perforation). This happens to about one out of every 10,000 patients in the United States. If there is an abnormal narrowing (stricture) that needs to be expanded (dilated), the danger is increased. If a perforation is produced, you will be admitted to the hospital for additional treatment, which may include a surgical procedure.
- Bleeding may occur at the biopsy site, but it normally goes away on its own. If you're using blood thinners, you're at a higher risk.
- Breathing or cardiac problems. As a result of the anesthesia or unintentionally inhaling secretions such as saliva during the procedure, breathing difficulties or cardiac abnormalities may occur. Doctors will keep an eye on you throughout the treatment so that if any of these issues arise, they will be able to address them promptly.
- Teeth or bridgework damage. To secure your teeth, the nurse will put a plastic mouthpiece in your mouth.
- Incomplete procedure. This can occur if you are unable to withstand the procedure, if there is undigested food in your esophagus and stomach, or if a gastroscopy problem arises. If this occurs, the Endoscopist may need to schedule another gastroscopy or another test, such as a Barium meal.
Gastroscopy Results
You will be issued a written report outlining the procedure. When you leave the hospital, a doctor or nurse will discuss any endoscopic findings.
Keep in mind that this exam may be one of several that you are taking, so the outcome may not be conclusive.
If biopsies were taken, they will be evaluated in the laboratory before being assessed by clinical staff. The doctor will send you a letter outlining the findings and future actions. This can take anywhere from 8 to 10 weeks.
At your next visit, you should discuss the results and any necessary therapy with the doctor who suggested the test. You will not be able to get biopsy results from the endoscopic department.
If you've been given a sedative, it's a smart option to have someone with you when the findings are discussed, as you may not recall anything.
Caring for Yourself after You Leave Hospital
Sedation lasts longer than you might expect. You are not permitted to:
- Ride a bicycle and drive a car
- Handle machinery or perform any other task that demands expertise or judgment
- Consume alcoholic beverages
- Ingest sleeping pills
- Head to the workplace
- Sign any contracts or official documents that are vital to you.
After the procedure, you should remain at home and be able to resume your typical activities 24 hours later.
If you have severe belly discomfort or fever (high temperature), are unwell, or pass significant volumes of blood after the procedure, go to the nearest emergency department. It's a good idea to bring the endoscopic report with you.
Conclusion
In the diagnosis and treatment of esophageal, gastric, and small-bowel problems, gastroscopy has become an important tool. Assessment of dysphagia, gastrointestinal bleeding, peptic ulcer disease, medically resistant GERD, esophageal strictures, celiac disease, and unexplained diarrhea are among the many acknowledged reasons for gastroscopy. Diagnostic biopsies, as well as therapies to produce hemostasis and dilatation for severe strictures, can all be done during a gastroscopy examination. It is normally a safe and well-tolerated procedure when done correctly. The availability and utilization of gastroscopy in the pediatric population have grown. The conditions and timing of gastroscopy use in children are still more of an artwork than a science, and a more rigorous examination of this tool's use is recommended to maximize benefits while minimizing danger.