Introduction
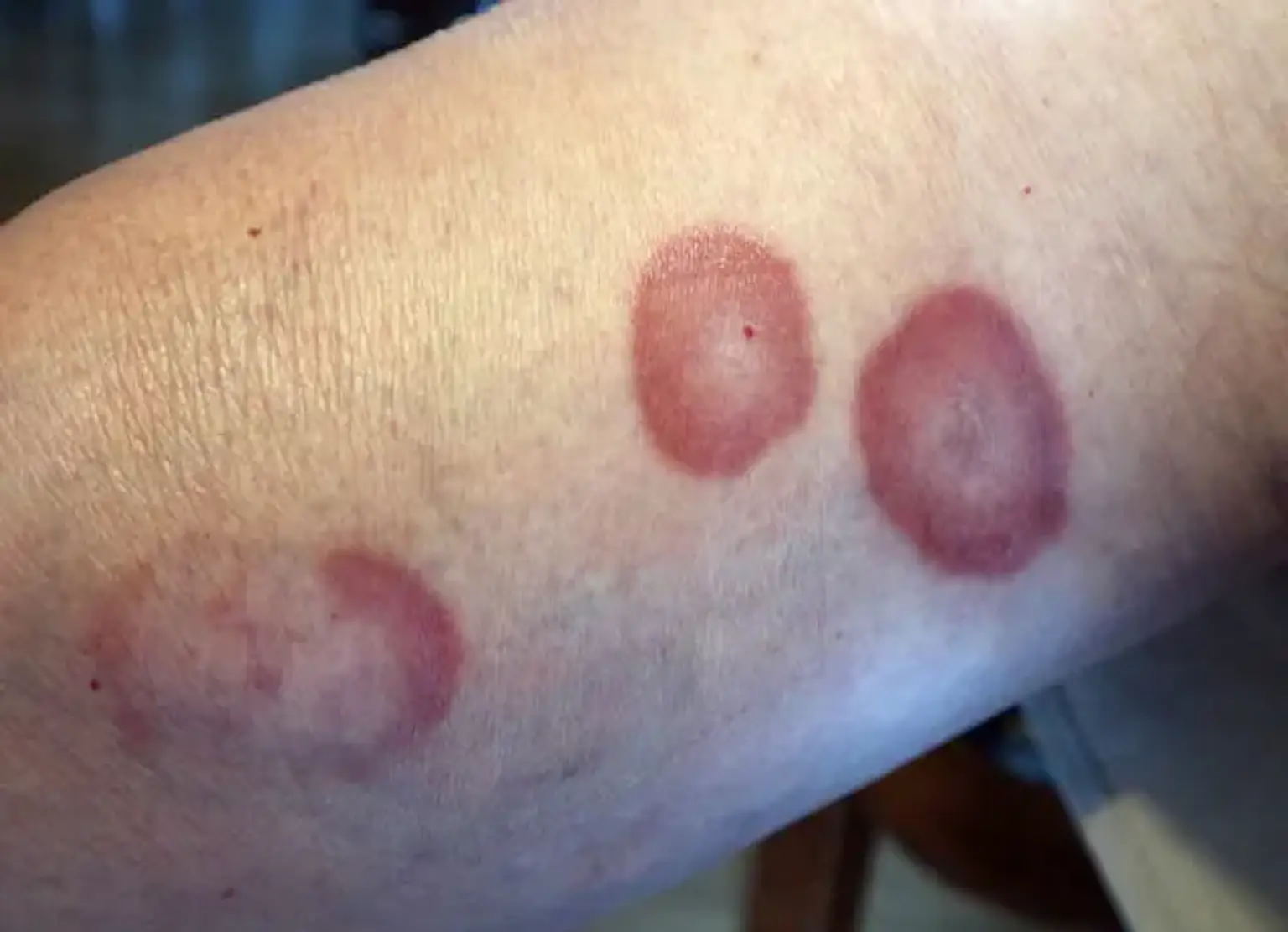
Granuloma Annulare (GA) is a benign, non-contagious skin condition that results in the appearance of ring-shaped lesions or bumps on the skin. Though the exact cause of GA remains unclear, it often affects the hands, feet, and sometimes the trunk. It is most commonly seen in children and adults under the age of 30. Although it can be alarming to see these distinctive rings on the skin, GA is typically not harmful, and it doesn’t pose any long-term health risks.
For many, GA resolves on its own without treatment. However, in some cases, the lesions can persist, leading patients to seek medical advice. In this article, we'll explore the various treatment options for GA, including both traditional and emerging therapies.
Understanding Granuloma Annulare: A Detailed Look
Granuloma Annulare is characterized by the appearance of circular, raised patches of skin that may have a red, pink, or flesh-colored hue. The lesions can range in size from small dots to large rings, sometimes resembling a target. They are generally painless and do not cause itching or other uncomfortable symptoms, though the appearance can be concerning.
The cause of GA is still not fully understood. Some theories suggest that the condition could be triggered by an immune response to infection, injury, or even certain medications. It is often seen in individuals with underlying conditions such as diabetes, thyroid disease, or autoimmune disorders. However, most cases occur in otherwise healthy individuals, and the exact trigger remains elusive.
While the condition may resolve without medical intervention, in some instances, it can recur, leading to ongoing concerns for patients.
Symptoms and Diagnosis of Granuloma Annulare
The hallmark symptom of Granuloma Annulare is the appearance of distinctive ring-shaped lesions on the skin. These rings usually have a raised edge and are often surrounded by normal skin in the center, giving them a "donut" appearance. The lesions may vary in size, but they are typically painless and not itchy, which can differentiate GA from other skin conditions such as eczema or psoriasis.
A diagnosis of GA is usually straightforward for dermatologists. Based on the appearance of the skin lesions, a healthcare professional can often diagnose the condition without additional tests. However, in some cases, a skin biopsy may be recommended to rule out other skin disorders or confirm the diagnosis.
It's important to consult a dermatologist if you suspect you have GA, especially if the lesions persist or cause cosmetic concerns. Early diagnosis helps ensure that the condition is correctly identified and managed.
Treatment Goals for Granuloma Annulare
The main goal of treatment for Granuloma Annulare is to reduce symptoms, prevent flare-ups, and improve the cosmetic appearance of the skin. In many cases, treatment is not necessary since the condition may resolve on its own within months or years. However, for patients with persistent or bothersome lesions, there are several treatment options available.
The primary objectives of treatment include:
Reducing inflammation: Many therapies focus on decreasing the inflammatory response that causes the characteristic lesions.
Preventing recurrence: Although GA often resolves, some individuals experience repeated flare-ups, making preventative strategies essential.
Improving appearance: As the lesions can be unsightly, especially in visible areas of the body, treatments are aimed at minimizing their appearance.
Treatment may also be tailored depending on the severity of the lesions, their location, and whether other underlying health issues are present. While many treatments are effective, no cure for GA has been established, and management often focuses on symptom control.
Topical Steroid Treatments for Granuloma Annulare
Topical steroids are one of the most commonly recommended treatments for Granuloma Annulare (GA). These corticosteroid creams or ointments help reduce inflammation, which can alleviate the appearance of the skin lesions. Topical steroids are often applied directly to the affected areas once or twice daily, depending on the severity of the lesions.
There are different strengths of topical steroids, ranging from mild to potent. Mild steroids are generally used for sensitive areas, like the face, while stronger steroids might be needed for thicker or more persistent lesions.
While effective, corticosteroid treatments do come with potential side effects, particularly if used long-term. These can include thinning of the skin or stretch marks. Therefore, it’s essential to follow a dermatologist’s instructions closely and avoid overuse. In most cases, short-term use is sufficient to improve the condition.
Oral Medications for Granuloma Annulare
For more severe or persistent cases of Granuloma Annulare, oral medications may be prescribed. Oral corticosteroids, such as prednisone, can be effective in reducing inflammation and helping the skin lesions heal more quickly. These medications work by suppressing the immune system’s inflammatory response, which is believed to play a key role in the development of GA.
However, long-term use of oral steroids can come with side effects, such as weight gain, mood changes, and increased susceptibility to infections. Therefore, oral steroids are usually prescribed for short periods and under careful supervision.
In cases where corticosteroids aren’t effective or suitable, other oral medications such as retinoids (e.g., acitretin) or immunosuppressants (e.g., methotrexate) may be considered. These drugs can help regulate the immune system, reducing the frequency of flare-ups and promoting healing. As with all medications, these options should be discussed thoroughly with a healthcare provider, given their potential side effects.
Phototherapy for Granuloma Annulare
Phototherapy, or light therapy, is another treatment option for Granuloma Annulare, particularly for individuals with widespread or stubborn lesions. The therapy involves the use of ultraviolet (UV) light to target and reduce inflammation in the affected skin. The most common types of phototherapy used for GA are Narrowband UVB or PUVA (psoralen + UVA) treatments.
Narrowband UVB therapy is typically the first choice, as it has shown effectiveness in treating a variety of skin conditions, including GA. Phototherapy sessions usually last between 10 to 30 minutes and are performed multiple times a week, depending on the severity of the lesions. It can take several weeks of treatment before results are noticeable.
While phototherapy is generally safe, it does carry a risk of skin damage with prolonged exposure to UV rays. Over time, this may increase the risk of skin cancer, so the therapy should be carefully managed and monitored by a dermatologist.
Intralesional Injections for Granuloma Annulare
Intralesional injections, which involve injecting steroids directly into the skin lesions, are often used when topical treatments are ineffective. This method delivers a potent dose of medication directly to the affected area, allowing for faster and more localized relief.
The most common substance used for intralesional injections is corticosteroids, which help to reduce inflammation and shrink the lesions. This treatment is particularly helpful for thicker or more persistent lesions that do not respond to topical steroids.
Patients generally tolerate this procedure well, although it may cause some temporary pain or swelling at the injection site. Multiple sessions may be needed, especially for extensive lesions. As with other steroid treatments, there is a potential risk of skin thinning or scarring, so the number of injections should be limited and carefully managed by a healthcare provider.
Natural Remedies and Home Care for Granuloma Annulare
While medical treatments are often effective for managing Granuloma Annulare (GA), some individuals may seek natural remedies or home care options to complement their treatment. Though these alternatives should not replace professional medical advice, they can sometimes provide relief or help support skin health.
Aloe Vera is one of the most popular natural remedies for various skin conditions, including GA. Its anti-inflammatory properties may help soothe irritated skin and promote healing. Applying fresh aloe vera gel directly to the lesions a few times a day can provide cooling relief.
Turmeric, known for its anti-inflammatory and antioxidant properties, may also be beneficial. Some studies suggest that turmeric may help reduce the inflammation associated with GA. You can incorporate turmeric into your diet by adding it to food or making a paste to apply topically.
Other remedies, such as coconut oil, tea tree oil, and apple cider vinegar, are commonly mentioned for their skin-soothing properties. However, before trying any natural remedy, it's crucial to perform a patch test to ensure there are no allergic reactions. Always discuss with your dermatologist before beginning any home treatments.
Managing Granuloma Annulare Flares
Flare-ups of Granuloma Annulare (GA) can be frustrating, but there are ways to manage and minimize the occurrence of new lesions. Identifying potential triggers and incorporating preventive strategies can help keep flare-ups under control.
Avoiding Skin Trauma: Since GA can sometimes be triggered by injury or irritation to the skin, minimizing trauma to affected areas can help. Be gentle when washing or scrubbing your skin, and avoid tight clothing that may rub against the lesions.
Sun Exposure: While some sunlight can be beneficial for the skin, overexposure to the sun may exacerbate GA. It’s important to protect your skin with sunscreen (SPF 30 or higher) and wear protective clothing when spending time outdoors.
Stress Management: Psychological stress is thought to potentially play a role in flare-ups of many skin conditions, including GA. Practicing relaxation techniques such as yoga, meditation, or deep breathing exercises can help manage stress and potentially reduce the frequency of flare-ups.
Tracking flare-ups in a symptom diary can also help identify specific triggers, whether it be dietary, environmental, or stress-related. Keeping a record and discussing it with your doctor can help tailor your treatment approach.
Granuloma Annulare Treatment for Children
Treating Granuloma Annulare (GA) in children presents unique challenges, as pediatric skin is more sensitive and requires careful handling. The condition is more common in younger individuals, and while it often resolves on its own, treatment may be necessary if the lesions are widespread, persistent, or causing distress.
Topical Corticosteroids are usually the first-line treatment for children, as they are effective and easy to apply. However, doctors tend to prescribe lower-potency steroids for young patients to minimize side effects, such as thinning skin.
If topical treatments are ineffective or if the condition is severe, oral medications like oral steroids or retinoids may be considered, but only under close supervision due to the potential for side effects. Phototherapy can also be an option for older children who are not responding to topical treatments, but again, this should be used cautiously and with careful monitoring.
Parents should consult with a pediatric dermatologist to ensure the most appropriate treatment plan is followed for their child's specific case.
Treatment During Pregnancy
Pregnancy adds a layer of complexity to the treatment of Granuloma Annulare (GA), as some medications may not be safe for the developing baby. Fortunately, GA is generally considered a low-risk condition during pregnancy, and treatment can often be managed safely with proper guidance.
Topical steroids are usually considered safe during pregnancy, as they are applied locally and have minimal systemic absorption. A dermatologist will likely recommend a mild to moderate strength steroid to avoid any potential complications.
Oral medications, however, are generally avoided during pregnancy unless absolutely necessary. Steroids and other systemic treatments, such as retinoids or immunosuppressants, can have harmful effects on the fetus and are only prescribed when the benefits outweigh the risks.
It's important for pregnant women with GA to work closely with both their dermatologist and obstetrician to ensure that any treatments used are safe for both the mother and the baby. Regular monitoring will also help track the condition's progress and ensure it does not worsen during pregnancy.
Granuloma Annulare and Its Impact on Mental Health
While Granuloma Annulare (GA) is typically a benign condition, its appearance can have a significant impact on a patient's mental and emotional well-being. The visible, ring-shaped lesions, especially if they are on the face, hands, or other exposed areas, may cause feelings of self-consciousness or embarrassment. This can lead to anxiety, depression, or a negative body image, particularly in individuals who experience persistent flare-ups.
Support groups, counseling, or therapy may help patients manage the emotional effects of GA. Educating patients about the benign nature of the condition and its low risk can also alleviate concerns and reduce stress. Many individuals find that addressing both the physical and emotional aspects of the condition leads to better overall outcomes.
The Role of Diet in Managing Granuloma Annulare
There is no definitive scientific evidence linking diet directly to the development or exacerbation of Granuloma Annulare. However, some individuals find that certain foods or nutritional changes may help in managing flare-ups.
Anti-inflammatory foods, such as omega-3 rich foods (salmon, flaxseeds), antioxidants (berries, leafy greens), and nuts, may support the body’s immune response and reduce skin inflammation. Additionally, staying hydrated can help maintain healthy skin.
Some people with GA have reported that avoiding processed foods, sugars, or dairy products may reduce flare-ups, though this varies from person to person. It's helpful for individuals with GA to keep a food diary and discuss their findings with a healthcare provider to determine any potential dietary triggers.
Prognosis and Long-Term Outlook for Granuloma Annulare
The prognosis for Granuloma Annulare is generally good. In most cases, the condition either resolves on its own or remains stable without causing significant health issues. The lesions may disappear within months to a couple of years, often without leaving scars.
However, for some individuals, GA can be chronic, with recurrent flare-ups. In these cases, the lesions may persist for many years, though they typically don’t pose any significant health risks. Treatment can help manage the appearance of the lesions and reduce flare-up frequency.
In rare cases, GA may be associated with underlying health conditions, such as diabetes, thyroid disorders, or autoimmune diseases. If GA is persistent or associated with systemic symptoms, further evaluation by a healthcare provider may be necessary.
How to Prevent Granuloma Annulare Flare-Ups
While Granuloma Annulare is not entirely preventable, certain measures can help reduce the risk of flare-ups and manage the condition effectively.
Skin Care: Avoid skin trauma or injury, as it can trigger new lesions. Gentle cleansing and moisturizing can help maintain healthy skin.
Sun Protection: Use sunscreen and protective clothing to prevent sunburn, which can exacerbate GA.
Stress Management: Since stress can trigger flare-ups, practices like yoga, mindfulness, and relaxation exercises may help prevent new lesions from developing.
Regular Check-Ups: Regular visits to a dermatologist can help track the condition’s progress and adjust treatment plans if necessary.
By following these strategies, individuals with GA can improve their chances of preventing flare-ups and maintaining healthy, clear skin.
Granuloma Annulare and Its Global Prevalence
Granuloma Annulare (GA) is not a rare condition, but its global prevalence remains largely under-researched. It affects individuals of all ages, but it is most commonly seen in children and young adults, especially between the ages of 10 and 30. While it occurs in both men and women, it seems to affect women slightly more frequently. The condition is seen across various ethnicities and regions, though its frequency may vary based on genetic and environmental factors.
The prevalence of GA is higher in populations with autoimmune diseases, diabetes, and thyroid disorders, suggesting a possible link between these conditions. However, in the majority of cases, GA appears without any underlying systemic disease. As awareness of the condition increases, more research is needed to understand its global patterns, triggers, and potential links to other health issues.
How to Choose the Right Treatment for Granuloma Annulare
Choosing the right treatment for Granuloma Annulare (GA) can depend on a number of factors, including the severity of the condition, the location of the lesions, the patient’s age, and any underlying health issues. Treatment is often personalized, as different individuals may respond better to certain therapies.
For mild cases, topical steroids or natural remedies may be sufficient. If the condition is more persistent or widespread, oral medications or phototherapy might be necessary. For individuals who experience frequent flare-ups, a combination of treatments might be the best approach.
It is important to discuss treatment options with a healthcare provider who can help assess the individual’s specific case and recommend the most appropriate course of action. Dermatologists are particularly helpful in guiding treatment decisions based on their expertise in managing skin conditions like GA.
Frequently Asked Questions (FAQs) About Granuloma Annulare
Q: Is Granuloma Annulare contagious? A: No, Granuloma Annulare is not contagious. It cannot be spread from person to person through physical contact.
Q: Can Granuloma Annulare cause scarring? A: While GA usually does not leave scars, some individuals may experience mild scarring, particularly if the lesions are severe or if they are treated with more invasive therapies like intralesional injections.
Q: Does Granuloma Annulare go away on its own? A: Yes, in many cases, Granuloma Annulare resolves on its own over time. However, in some instances, the condition may persist for several years or require treatment to control symptoms.
Q: What is the outlook for Granuloma Annulare? A: The outlook for GA is generally good. Most cases improve or resolve over time, and the condition does not pose significant health risks. However, recurrent flare-ups can occur in some individuals.
Conclusion
Granuloma Annulare is a manageable condition that, although it can be visually distressing, does not pose serious health risks. With the right treatment plan, most individuals can control symptoms and prevent flare-ups. Whether through topical treatments, oral medications, phototherapy, or lifestyle adjustments, various options exist to help manage the condition effectively.
For individuals dealing with GA, it is important to focus on skin care, avoid potential triggers, and work closely with a dermatologist to find a treatment that works. With proper management, GA can be kept under control, allowing individuals to lead a healthy and confident life.