Introduction
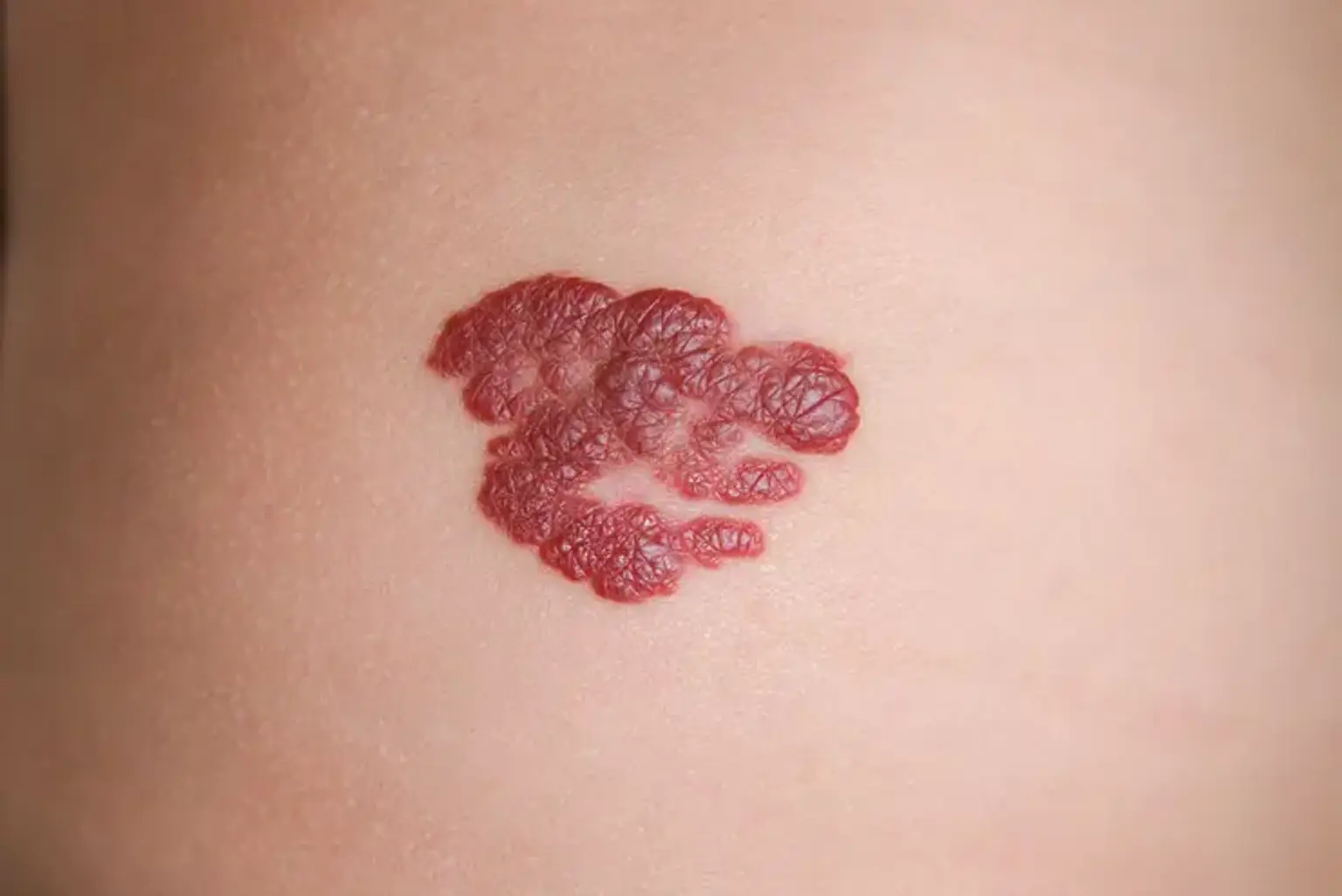
Hemangiomas are benign vascular tumors that commonly appear in infancy, often as a red or bluish raised lesion on the skin. These growths result from an abnormal proliferation of blood vessels and typically go through a cycle of rapid growth followed by gradual regression. While many hemangiomas resolve without intervention, some require medical treatment due to complications such as ulceration, obstruction of vital functions, or cosmetic concerns.
Early diagnosis and appropriate treatment are crucial to managing hemangiomas effectively. In some cases, hemangiomas can cause significant functional impairment, especially when located near the eyes, nose, mouth, or airways. Understanding the different types of hemangiomas, available treatment options, and potential complications can help caregivers and medical professionals make informed decisions about management strategies.
Hemangiomas are the most common benign tumors in infants, affecting approximately 4-5% of newborns. They are more prevalent in premature infants, females, and Caucasian populations. Although most hemangiomas are harmless, a small percentage require medical intervention due to their size, location, or growth pattern.
Types of Hemangiomas
There are two primary types of hemangiomas: infantile hemangiomas and congenital hemangiomas.
Infantile Hemangiomas: These are the most common type and typically appear within the first few weeks of life. They undergo a rapid proliferative phase (growth phase) for the first 6-12 months, followed by a gradual involution phase over several years.
Congenital Hemangiomas: Unlike infantile hemangiomas, these are fully developed at birth and do not go through a proliferative phase. They can be categorized as:
Rapidly Involuting Congenital Hemangiomas (RICH) – These shrink significantly within the first year of life.
Non-Involuting Congenital Hemangiomas (NICH) – These persist without shrinking and may require treatment.
Additionally, hemangiomas can be classified based on their depth:
Superficial Hemangiomas: Appear as bright red, raised lesions on the skin’s surface (also called "strawberry hemangiomas").
Deep Hemangiomas: Develop beneath the skin and may have a bluish or skin-colored appearance.
Mixed Hemangiomas: Contain both superficial and deep components.
While most hemangiomas do not cause complications, some can lead to ulceration, bleeding, infection, or functional impairment, requiring medical attention.
Diagnosis of Hemangiomas
The diagnosis of hemangiomas is primarily clinical, meaning that doctors can usually identify them based on appearance and growth pattern. However, in some cases, additional diagnostic tools are needed to confirm the diagnosis and assess potential complications.
Clinical Examination
Most hemangiomas are diagnosed by visual inspection and medical history.
The doctor evaluates the lesion’s size, color, texture, and location.
Parents may be asked about the growth pattern of the lesion.
Imaging Tests
For deeper or more complex hemangiomas, imaging may be necessary:
Ultrasound: A non-invasive, first-line imaging tool that helps differentiate hemangiomas from other vascular anomalies. It is particularly useful for deep hemangiomas that are not easily visible on the surface.
Magnetic Resonance Imaging (MRI): Used when hemangiomas involve internal organs or critical structures (e.g., airways, liver). MRI provides detailed images to assess the lesion’s depth and impact on surrounding tissues.
Biopsy (Rarely Needed)
In rare cases, if the lesion has atypical features or if there is uncertainty in diagnosis, a skin biopsy may be performed to rule out other vascular tumors or malignancies.
Treatment Options for Hemangiomas
The choice of treatment depends on several factors, including the size, location, growth rate, and associated complications of the hemangioma. While many small hemangiomas resolve on their own, others require medical intervention to prevent complications.
1. Observation ("Watch and Wait" Approach)
Many small, uncomplicated hemangiomas require no treatment.
Regular monitoring is essential to track growth and potential complications.
If the hemangioma does not interfere with function or cause cosmetic concerns, it may be left to resolve naturally.
2. Pharmacotherapy (Medication Treatment)
For hemangiomas that require intervention, medications can help reduce growth and improve appearance.
a. Beta-Blockers (First-Line Treatment)
Oral Propranolol:
Most effective and widely used treatment for problematic hemangiomas.
It reduces the size, color, and blood flow of the hemangioma.
Typically given for 6-12 months, with gradual tapering to prevent regrowth.
Side effects: Low blood sugar, low blood pressure, and sleep disturbances.
Topical Timolol:
A gel-form beta-blocker used for small, superficial hemangiomas.
Lower risk of systemic side effects compared to oral propranolol.
b. Corticosteroids
Used when beta-blockers are not effective or contraindicated.
Oral steroids can reduce hemangioma growth but have more side effects (e.g., weight gain, high blood pressure).
Intralesional steroid injections may be used for localized hemangiomas.
3. Laser Therapy
Pulsed Dye Laser (PDL) is used for:
Superficial hemangiomas (especially those causing ulceration).
Residual redness after hemangioma regression.
Best results occur when treatment is started early.
4. Surgical Intervention
Surgery is rarely needed but may be performed in cases where:
The hemangioma affects vital functions (e.g., vision, breathing).
There is significant disfigurement or non-resolving tissue damage.
Surgical excision may be done for residual skin changes after involution.
Managing Complications
While most hemangiomas are harmless and resolve independently, some can lead to significant complications that require medical intervention. The potential complications depend on the hemangioma’s size, location, and growth pattern.
a. Ulceration and Infection
Ulceration (skin breakdown) is the most common complication, occurring in about 15% of cases. It is more frequent in areas prone to friction, such as the lips, diaper region, and folds of the neck.
Ulceration can be painful, lead to bleeding, and increase the risk of secondary infections.
Treatment options:
Topical antibiotics (for infection prevention).
Moist wound care (petroleum jelly or antibiotic ointments).
Pain management (oral pain relievers, lidocaine gel).
Pulsed dye laser therapy to speed healing.
b. Functional Impairment
Periorbital Hemangiomas (Around the Eyes):
Can obstruct vision, leading to amblyopia (lazy eye) if untreated.
Early intervention with propranolol or steroids is crucial.
Subglottic Hemangiomas (Airway Involvement):
May cause breathing difficulties, stridor (wheezing), or airway obstruction.
Requires urgent treatment with propranolol, steroids, or surgical removal if severe.
c. Hemangiomas of Internal Organs
Liver Hemangiomas (Hepatic Hemangiomas):
Multiple or large liver hemangiomas can cause high-output heart failure due to excessive blood flow demands.
Severe cases may require propranolol, embolization, or surgery.
d. Long-Term Cosmetic Concerns
Some hemangiomas leave residual skin changes such as:
Excess skin and scarring.
Telangiectasias (dilated blood vessels).
Depigmentation or textural irregularities.
Treatment options include:
Laser therapy for residual redness.
Surgical excision for remaining bulky tissue.
Dermal fillers or cosmetic procedures for skin irregularities.
6. Case Studies & Real-Life Examples
Case Study 1: Successful Propranolol Treatment
Background: A 3-month-old girl developed a rapidly growing hemangioma on her eyelid, causing vision obstruction.
Treatment: She was prescribed oral propranolol at a pediatric dermatology clinic.
Outcome: The hemangioma began shrinking within weeks, and by 12 months, it had almost completely regressed, preventing vision loss.
Case Study 2: Laser Therapy for Ulcerated Hemangioma
Background: A 6-month-old baby had a painful ulcerated hemangioma on the lower lip, making feeding difficult.
Treatment: The child received pulsed dye laser therapy and topical wound care.
Outcome: The ulcer healed within 3 weeks, and the hemangioma faded significantly over time.
Case Study 3: Surgical Removal of a Large Facial Hemangioma
Background: A 4-year-old boy had a large, disfiguring hemangioma on his cheek that did not regress completely.
Treatment: A plastic surgeon performed excision and skin reconstruction.
Outcome: The child had minimal scarring, and his parents reported improved self-confidence.
Advances in Hemangioma Treatment
a. Development of Propranolol as First-Line Therapy
Before 2008, the standard treatment for complicated hemangiomas was corticosteroids, which had significant side effects.
The discovery of propranolol, a beta-blocker, revolutionized hemangioma treatment.
Benefits of Propranolol:
Faster shrinkage of hemangiomas.
Fewer side effects compared to steroids.
Effective for both superficial and deep hemangiomas.
b. Laser Therapy Innovations
Pulsed dye laser (PDL) technology has improved, allowing for better targeting of blood vessels.
Newer laser techniques help treat residual telangiectasias and reduce redness more effectively.
c. Future Directions in Research
Ongoing clinical trials are investigating:
New topical and systemic medications with fewer side effects.
Gene therapy approaches to control vascular growth.
Combination therapies using beta-blockers, lasers, and biologic agents.
Psychological and Emotional Impact of Hemangiomas
Although hemangiomas are benign and often temporary, they can have a significant psychological impact on both children and parents.
a. Parental Anxiety and Stress
Parents often worry about:
The growth and appearance of the hemangioma.
Social stigma and reactions from others.
The need for medical intervention and potential risks.
Support groups and counseling can help parents cope with these concerns.
b. Emotional Well-Being of the Child
Children with facial or large hemangiomas may experience self-esteem issues as they grow older.
Bullying and social stigma can affect their confidence.
Psychological support, including child-friendly counseling and positive reinforcement, is crucial for emotional development.
c. Role of Cosmetic Interventions
In cases where residual skin changes persist after hemangioma regression, cosmetic interventions such as:
Laser treatments for discoloration.
Surgical corrections for excess skin.
Makeup techniques for camouflage (especially for older children and teenagers).
Hemangiomas and Associated Syndromes
Although most hemangiomas occur as isolated skin lesions, some are associated with underlying syndromes, requiring additional evaluation.
a. PHACE Syndrome
PHACE stands for:
Posterior fossa malformations (brain abnormalities).
Hemangiomas (large segmental facial hemangiomas).
Arterial anomalies (abnormal blood vessels in the brain or neck).
Cardiac defects (heart abnormalities).
Eye abnormalities.
Key facts:
PHACE syndrome is suspected in infants with large hemangiomas on the face and scalp.
MRI and cardiac evaluations are recommended for diagnosis.
Multidisciplinary care involving neurologists, cardiologists, and dermatologists is necessary.
b. LUMBAR Syndrome
This rare condition is associated with:
Lower body hemangiomas.
Urinary tract anomalies.
Myelo-spinal defects (spinal cord abnormalities).
Bony abnormalities.
Anomalies of anorectal and genital areas.
Renal (kidney) anomalies.
Key facts:
Common in large lumbosacral hemangiomas (lower back region).
Requires imaging studies (MRI, ultrasound) for diagnosis.
Treatment depends on associated complications (e.g., urinary and spinal cord issues).
Hemangiomas in Adults
While hemangiomas are most common in infants, adult-onset hemangiomas can also occur. These differ from childhood hemangiomas in terms of growth patterns and treatment.
a. Types of Adult Hemangiomas
Cherry Angiomas: Small, red spots that appear on the skin with age.
Cavernous Hemangiomas: Deeper blood vessel growths found in the liver, brain, or spine.
Venous Malformations: Sometimes mistaken for hemangiomas but persist without spontaneous regression.
b. Diagnosis and Management
Cherry angiomas are harmless and often require no treatment.
Cavernous hemangiomas in internal organs may require imaging (MRI, CT scan) to assess their size and impact on organ function.
Treatment options:
Laser therapy for cosmetic concerns.
Surgical removal if they cause pain or complications.
Monitoring for stable, asymptomatic lesions.
Future Research and Emerging Treatments
The field of hemangioma research is evolving, with new treatments and diagnostic approaches on the horizon.
a. Investigating Alternative Medications
Researchers are exploring other beta-blockers (besides propranolol) with fewer side effects.
Targeted biologic drugs (e.g., VEGF inhibitors) could be an option for complicated cases.
b. Genetic and Molecular Studies
Advances in genetic testing are helping identify markers that predict hemangioma growth patterns.
Molecular research is focusing on how vascular endothelial growth factors (VEGF) contribute to hemangioma formation.
c. Stem Cell and Regenerative Medicine Approaches
Future therapies may involve stem cell treatments to accelerate hemangioma regression.
Tissue engineering and skin regeneration techniques may help improve post-hemangioma skin appearance.
Role of a Multidisciplinary Team
Managing hemangiomas often requires collaboration between specialists to ensure the best outcome.
a. Key Specialists Involved
Pediatric Dermatologists – Diagnose and monitor skin hemangiomas.
Ophthalmologists – Manage periocular hemangiomas affecting vision.
Otolaryngologists – Treat airway hemangiomas causing breathing issues.
Surgeons – Perform excision for large or complicated cases.
b. Coordinated Care Approach
Early referrals improve treatment success.
Regular follow-ups help monitor progress and adjust treatment.
Specialists work together to minimize complications and optimize cosmetic outcomes.
Cost and Accessibility of Hemangioma Treatments
Treatment costs vary based on location, severity, and healthcare system.
a. Medication Costs
Propranolol therapy can be expensive in some regions.
Generic versions and insurance coverage may reduce costs.
b. Laser and Surgical Costs
Laser therapy is often elective and may not be covered by insurance.
Surgical interventions can be costly, especially for cosmetic corrections.
c. Accessibility Challenges
Rural areas may lack specialized hemangioma treatment centers.
Telemedicine consultations help improve access in underserved regions.
Conclusion
Hemangiomas are common vascular birthmarks that often resolve naturally, but some require medical intervention to prevent complications. While many cases can be monitored without treatment, hemangiomas that obstruct vision, airways, or cause ulceration must be addressed early.
The introduction of propranolol has revolutionized treatment, offering a safe and effective solution for reducing hemangioma size and improving cosmetic outcomes. Laser therapy and surgery remain valuable options for persistent or residual skin changes. A multidisciplinary approach involving dermatologists, pediatricians, ophthalmologists, and surgeons ensures the best care for patients.
Beyond medical treatment, psychological and social support plays an essential role, especially for children with visible hemangiomas. Raising awareness about available treatments and improving access to specialized care can significantly enhance patient outcomes.
With ongoing research in genetics, biologic therapies, and regenerative medicine, the future of hemangioma management looks promising. Early diagnosis, timely treatment, and comprehensive care can help ensure that children with hemangiomas lead healthy, confident lives.
If you suspect a hemangioma requires attention, consult a medical professional early to explore the