Understanding Hysterectomy
What is a Hysterectomy Surgery?
A hysterectomy is a surgical procedure that involves the removal of a woman’s uterus. It can be performed for various medical reasons, such as treating uterine fibroids, endometriosis, cancer, or persistent pelvic pain. Depending on the condition and surgical approach, the procedure may include the removal of other reproductive organs, like the ovaries or cervix.
Types of Hysterectomy
There are different types of hysterectomy, each suited to specific medical needs:
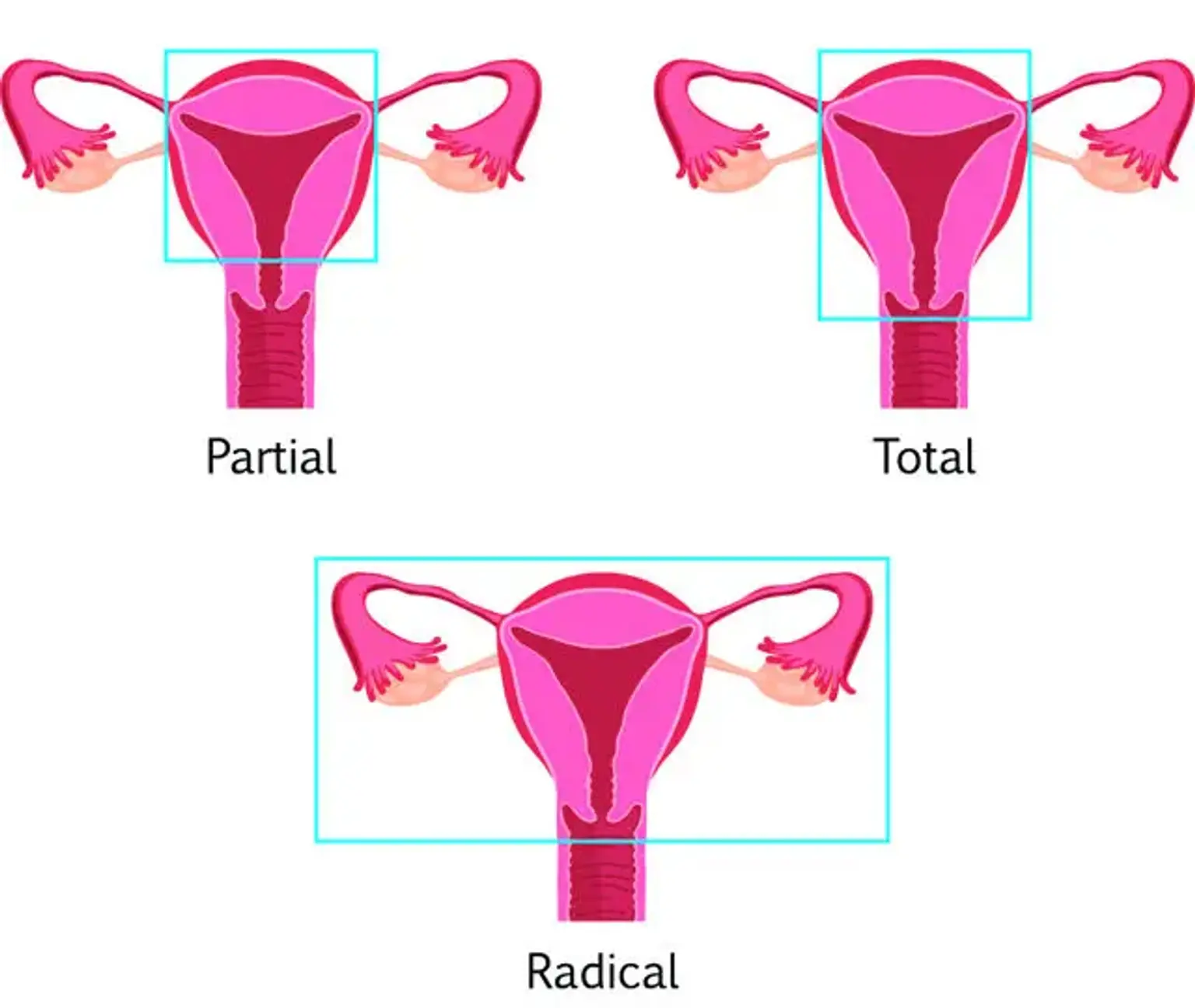
Total Hysterectomy: Removal of the entire uterus, including the cervix.
Partial Hysterectomy: Only the uterus is removed, leaving the cervix intact.
Radical Hysterectomy: A more extensive procedure, often performed for cancer, where the uterus, cervix, surrounding tissues, and sometimes part of the vagina are removed.
Vaginal Hysterectomy: Performed through the vagina, offering faster recovery with fewer incisions.
Laparoscopic (Minimally Invasive) or Robotic Hysterectomy: Performed using small incisions and robotic tools, leading to less pain and a quicker recovery time.
Indications for a Hysterectomy
A hysterectomy is typically considered when other treatments have failed, or when a medical condition affects the uterus or reproductive organs significantly. Common reasons include:
Uterine Fibroids: Non-cancerous growths that can cause pain, heavy bleeding, or other complications.
Endometriosis: A painful condition where tissue similar to the uterine lining grows outside the uterus.
Cancer: Uterine, cervical, or ovarian cancers may require removal of the uterus.
Uterine Prolapse: When the uterus falls into the vaginal canal due to weakened pelvic muscles.
Chronic Pelvic Pain: If persistent pain from conditions like adenomyosis does not respond to treatment, a hysterectomy may be the solution.
While hysterectomy is a major surgery, it is often the most effective option for relieving symptoms and preventing serious complications in these cases.
3. Types of Hysterectomy
Total Hysterectomy
This is the most common form of hysterectomy, where the entire uterus and cervix are removed. It’s used for conditions such as fibroids, cancer, or endometriosis. The surgery is typically done through an abdominal incision or laparoscopically.
Partial (Subtotal) Hysterectomy
In this procedure, only the uterus is removed, and the cervix is left intact. It may be appropriate for benign conditions or when preserving the cervix is medically advisable.
Radical Hysterectomy
A radical hysterectomy is a more invasive procedure, often performed in cases of cancer. It involves removing the uterus, cervix, part of the vagina, and surrounding tissues such as the ligaments and lymph nodes.
Vaginal Hysterectomy
This type of hysterectomy is done through the vagina, eliminating the need for abdominal incisions. Recovery time is typically shorter, and the procedure is less invasive. However, it may not be suitable for all patients, especially those with large uteruses or specific medical conditions.
Laparoscopic/Robotic-Assisted Hysterectomy
Minimally invasive procedures that use small incisions and special instruments. Robotic-assisted hysterectomy allows for greater precision and may reduce blood loss, pain, and recovery time. It's particularly suitable for patients seeking faster recovery and minimal scarring.
The Hysterectomy Procedure: Step-by-Step
How is the Surgery Performed?
The exact steps of a hysterectomy depend on the type of surgery being performed. Here’s an overview of a typical procedure:
Preparation: The patient is placed under general anesthesia to ensure they are unconscious and pain-free during the surgery.
Incision: Depending on the type of hysterectomy, an incision is made either in the abdomen (traditional) or through the vagina (vaginal hysterectomy) or small abdominal incisions (laparoscopic or robotic hysterectomy).
Removal of the Uterus: The surgeon carefully removes the uterus, and if necessary, the cervix, ovaries, or other tissues. In cases of cancer, lymph nodes or surrounding tissues may also be removed.
Closing Incisions: After the uterus is removed, the incisions are closed with sutures, and the patient is taken to the recovery room.
Traditional vs. Minimally Invasive Surgery
Traditional (Abdominal): Involves a larger incision and longer recovery time. It may be necessary if the uterus is large or if the patient has certain medical conditions.
Minimally Invasive (Laparoscopic/Robotic): Uses smaller incisions and cameras, offering benefits like less pain, faster recovery, and fewer complications.
Though the procedure might sound daunting, advances in technology and surgical techniques have made it safer and more effective than ever. Always consult with a qualified surgeon to determine the best approach for your specific condition.
Risks and Complications
Potential Risks of Hysterectomy
While hysterectomy is generally safe, like any surgery, it carries certain risks:
Infection: A common concern after surgery, often treated with antibiotics.
Excessive Bleeding: Some bleeding is expected, but excessive bleeding may require additional intervention.
Damage to Surrounding Organs: Rarely, nearby organs such as the bladder, ureters, or intestines may be damaged during surgery.
Hormonal Changes: If the ovaries are removed, the patient may experience early menopause with symptoms like hot flashes, mood swings, and vaginal dryness.
Emotional Impact: The loss of fertility can be emotionally challenging for some women.
How to Minimize Risks
Choosing a highly skilled surgeon is crucial. Pre-surgical assessments, including imaging and blood tests, help identify any complications early. Following post-surgery care instructions, such as avoiding heavy lifting and taking prescribed medications, can minimize risks.
Benefits of a Hysterectomy
Health Benefits and Long-term Relief
For many women, a hysterectomy brings significant relief:
Pain Relief: It is highly effective in treating chronic pelvic pain, often caused by fibroids, endometriosis, or adenomyosis.
Heavy Bleeding: Women suffering from abnormal bleeding patterns can find long-term relief after the procedure.
Cancer Prevention: In cases of cancer, hysterectomy removes the cancerous tissue, helping to prevent its spread.
Improved Quality of Life: Many women report improved quality of life post-surgery, free from the symptoms of their underlying conditions.
Long-Term Considerations
It’s important to note that if the ovaries are removed, patients may experience early menopause. Hormone replacement therapy (HRT) can help manage symptoms, but not all women opt for it. The decision should be discussed with a healthcare provider.
Preparation for Hysterectomy Surgery
How to Prepare for the Procedure
Proper preparation can ensure a smoother surgery and recovery:
Medical Evaluation: Before surgery, your doctor will assess your overall health through physical exams, blood tests, and imaging.
Medications: You may need to stop certain medications, such as blood thinners, and discuss any chronic conditions with your doctor.
Diet and Fasting: Typically, you will be instructed to fast for several hours before surgery to minimize the risk of complications during anesthesia.
Arrangements for Recovery: It’s essential to arrange for help at home post-surgery. A support system is crucial as you'll need rest and assistance with daily activities.
Lifestyle Adjustments
Avoid smoking and maintain a healthy diet before surgery. This can improve healing and reduce the risk of complications. A good night's sleep before the procedure also contributes to better recovery.
Recovery Process After Hysterectomy
What to Expect During Recovery
Recovery from a hysterectomy can vary depending on the type of surgery, but here are general expectations:
Initial Recovery: Most women stay in the hospital for 1-2 days, especially after an abdominal hysterectomy. Vaginal and laparoscopic hysterectomies often require shorter stays.
Pain Management: Pain is typically managed with medications. Most patients experience mild to moderate pain that subsides within a few days.
Returning to Normal Activities:
Abdominal Hysterectomy: Full recovery can take 6-8 weeks. Heavy lifting and strenuous activity should be avoided.
Minimally Invasive Surgery: Recovery time is faster—usually 2-4 weeks.
Post-Operative Care
You’ll need to follow specific guidelines to prevent complications:
Wound Care: Keep surgical wounds clean and dry to avoid infection.
Activity Restrictions: Gradually return to normal activities. Walking is encouraged, but avoid high-impact activities until cleared by your doctor.
Emotional Health: Hormonal changes, especially if the ovaries are removed, can lead to emotional shifts. Be mindful of this and seek support if needed.
Hysterectomy and Menopause
Impact of Hysterectomy on Hormonal Balance
When the ovaries are removed during a hysterectomy, it triggers immediate menopause, as the ovaries are responsible for hormone production. This can lead to symptoms such as hot flashes, night sweats, mood swings, and vaginal dryness. If the ovaries are left intact, natural menopause will still occur at the usual age.
Hormone Replacement Therapy (HRT)
HRT can help manage menopause symptoms by replacing the hormones the body no longer produces. However, HRT isn’t suitable for everyone and should be discussed with a healthcare provider to weigh the benefits and risks, particularly for women with a history of certain cancers or blood clots.
Long-term Health Considerations
Women who undergo a hysterectomy with ovary removal may face increased risks for osteoporosis and heart disease due to lower estrogen levels. It’s important to monitor bone health and heart health with your doctor after surgery.
Post-Hysterectomy Care
Essential Aftercare Tips
Post-surgery care is vital to ensure smooth recovery:
Follow-up Appointments: Regular check-ups with your doctor to ensure proper healing and address any concerns.
Pain Management: You may be prescribed pain medication in the days following surgery, along with recommendations for managing discomfort.
Incision Care: Keep surgical wounds clean and dry, and avoid activities that strain the body until cleared by your doctor.
Lifestyle Adjustments
Focus on rest during the initial recovery phase, but gentle walks and light activities will help promote circulation and healing. Avoid heavy lifting or strenuous exercises for about 6-8 weeks (longer for abdominal surgery).
Emotional Support
It’s normal to experience emotional changes due to hormonal shifts, loss of fertility, or changes in body image. Speaking to a counselor, joining support groups, or connecting with loved ones can provide emotional reassurance during recovery.
Cost and Accessibility of Hysterectomy
How Much Does a Hysterectomy Cost?
The cost of hysterectomy surgery can vary depending on factors like the surgical approach, healthcare provider, and geographical location. On average, the procedure ranges from $6,000 to $20,000 in the U.S. for an abdominal hysterectomy, while minimally invasive options may cost more due to advanced technology.
Insurance and Financial Considerations
Most health insurance plans cover the cost of a hysterectomy, especially if it’s medically necessary. It’s essential to check with your insurance provider to understand your coverage. Out-of-pocket expenses may still apply, depending on your plan.
Financial Assistance
Some hospitals offer payment plans or financial assistance programs to help ease the cost burden. Additionally, many patients explore alternative funding options or assistance programs, particularly if the procedure is deemed urgent or life-saving.
Hysterectomy vs. Other Treatment Options
Is Hysterectomy the Only Option?
While hysterectomy is a common and effective treatment, it is not the only option for certain conditions:
Fibroids and Endometriosis: Non-surgical treatments such as medications (e.g., hormone therapy or pain relievers) or less invasive procedures (like uterine artery embolization or endometrial ablation) may be alternatives.
Uterine Prolapse: Pelvic floor exercises, pessaries, or surgery may be used before opting for a hysterectomy.
Cancer: In cases of cancer, more conservative options like chemotherapy or radiation therapy may be explored before considering hysterectomy.
When is Hysterectomy the Best Option?
Hysterectomy is often recommended when other treatments have failed or when conditions like cancer, severe fibroids, or uncontrollable bleeding pose serious health risks. It’s important to discuss all available options with a healthcare provider to make an informed decision.
Emotional and Psychological Impact
Emotional Changes After Hysterectomy
The emotional effects of a hysterectomy can be significant, particularly for women who experience early menopause after ovarian removal. Many women feel a sense of loss due to infertility, changes in body image, or hormone fluctuations. It's common to have feelings of sadness or even grief, especially if the decision was not one they made voluntarily.
Coping Strategies
Talking to a counselor or psychologist can help manage emotional responses. Support groups, where women share similar experiences, can provide comfort and reassurance. Additionally, practicing stress-relief techniques such as mindfulness, yoga, or meditation can improve emotional well-being.
Impact on Relationships
The psychological and physical effects may also influence relationships. Partners should be supportive, communicate openly, and understand the emotional and physical recovery process. A couple's counselor or therapist can offer guidance on navigating these changes together.
Long-term Outlook and Life After Hysterectomy
What to Expect Long-Term
After the initial recovery period, most women experience a significant improvement in their quality of life. Chronic pain, heavy bleeding, or symptoms from conditions like fibroids or endometriosis are often eliminated. Many women feel empowered and relieved after surgery, having taken control of their health.
Post-Surgery Lifestyle
While a hysterectomy does not require any major changes to lifestyle, women who had their ovaries removed may need to monitor their bone health and cardiovascular function more closely. Regular exercise, a balanced diet, and routine check-ups can help maintain long-term health.
Maintaining Sexual Health
Sexual health is a concern for many women post-hysterectomy. If the ovaries are removed, vaginal dryness and changes in libido may occur, but lubricants and hormone therapy can help. Open communication with a partner and a healthcare provider is essential for navigating sexual health post-surgery.
Frequently Asked Questions (FAQs)
1. Can I Still Have Children After a Hysterectomy?
No, a hysterectomy removes the uterus, making pregnancy impossible. If you’re considering a hysterectomy but wish to preserve fertility, discuss alternatives like egg freezing or surrogacy options with your doctor.
2. How Soon Can I Return to Work After a Hysterectomy?
Recovery time depends on the type of surgery. For abdominal hysterectomy, it typically takes 6-8 weeks to return to work. For minimally invasive procedures, you may be able to return in 2-4 weeks, depending on your job and physical demands.
3. Will My Periods Return After Surgery?
No, once the uterus is removed, periods stop permanently. If the ovaries are removed, menopause symptoms will begin immediately. If the ovaries are preserved, menopause will occur at the typical age.
4. Is a Hysterectomy Covered by Insurance?
Most insurance plans cover the cost of a medically necessary hysterectomy. Be sure to check with your provider to understand your coverage and any out-of-pocket costs.
Global Popularity of Hysterectomy
Hysterectomy Rates Worldwide
Hysterectomy is a common procedure, but its popularity varies across the globe. In the United States, it is one of the most frequently performed surgeries for women, with over 500,000 procedures done each year. However, the rates are significantly lower in countries where alternative treatments, such as medication or less invasive procedures, are more accessible.
Global Trends and Advancements
Minimally invasive techniques, such as laparoscopic and robotic-assisted surgeries, are becoming more popular worldwide. These methods offer reduced recovery times, less scarring, and fewer complications, contributing to their growing use in both developed and developing countries.
Cultural Differences
In some cultures, the decision to undergo a hysterectomy may be influenced by social or cultural factors. In regions where fertility is highly valued, the decision can be more complex. Medical professionals must take these factors into account when discussing treatment options with patients.
Alternatives to Hysterectomy
Non-Surgical Options
For conditions like fibroids, endometriosis, or heavy bleeding, there are several alternatives to hysterectomy:
Medications: Birth control pills, hormone therapy, or anti-inflammatory drugs can help manage symptoms.
Uterine Artery Embolization: A non-invasive procedure to shrink fibroids by blocking blood flow.
Endometrial Ablation: A procedure to destroy the lining of the uterus to reduce heavy bleeding.
Myomectomy: Surgical removal of fibroids while preserving the uterus.
When to Choose Alternatives
These options are often considered before recommending a hysterectomy, especially if fertility preservation or avoiding the emotional impacts of surgery is a priority. However, for severe or life-threatening conditions, hysterectomy remains the best option.
Innovations in Hysterectomy Surgery
Minimally Invasive Techniques
Advancements in medical technology have made hysterectomies less invasive:
Laparoscopic Hysterectomy: Small incisions and a camera allow surgeons to remove the uterus with minimal tissue disruption.
Robotic-Assisted Hysterectomy: A surgeon uses a robot for increased precision, often leading to faster recovery and fewer complications.
Benefits of Minimally Invasive Surgery
These techniques reduce recovery time, hospital stays, and scarring, while offering quicker return to normal activities. Some women are able to return to work in just a few weeks.
Future Trends
As technology continues to evolve, it’s likely that recovery times will decrease even further, and procedures will become safer and more accessible worldwide.
Hysterectomy Surgery and Women's Empowerment
Taking Control of Health
For many women, a hysterectomy is not just a medical procedure but also a step toward regaining control over their health. It can offer relief from chronic pain, heavy bleeding, and conditions like cancer, improving overall quality of life.
Positive Patient Stories
Many women report feeling a sense of empowerment after their hysterectomy, especially when it resolves long-standing health issues. It’s important to focus on the positive impact the surgery can have, not just the loss of fertility or the emotional challenges.
Advocacy and Support
Advocacy groups and online communities play a significant role in empowering women by providing information, emotional support, and sharing experiences. These resources help women make informed decisions about their healthcare.
Conclusion
A hysterectomy can be a life-changing procedure, offering significant benefits such as relief from chronic pain, heavy bleeding, and conditions like fibroids, endometriosis, or even cancer prevention. However, it’s a deeply personal decision that requires careful consideration of all factors, including potential risks, recovery time, and emotional impact.
For many women, the procedure leads to improved quality of life, greater comfort, and relief from the symptoms that previously impacted their daily lives. The advent of minimally invasive techniques, such as laparoscopic and robotic-assisted surgeries, has made the procedure safer with quicker recovery times.
That said, it's crucial to explore all available options, including non-surgical treatments, and consult with a skilled healthcare provider to fully understand the best course of action for your unique situation. Emotional support and guidance during both the decision-making process and recovery are key to ensuring a smooth journey through this significant health decision.
Ultimately, the choice to undergo a hysterectomy should be informed, thoughtful, and empowering. Whether you are looking to relieve health issues, enhance your well-being, or simply regain control over your body, a hysterectomy may provide lasting benefits and a healthier future.