Inflammatory Bowel Disease
Inflammatory bowel disease refers to an umbrella of intestinal disorders characterized by chronic inflammation of the digestive system. The digestive system comprises the mouth, esophagus, stomach, small intestine, and large intestine.
It plays a significant role in breaking down food products, extracting nutrients, and disposing of any unusable content or waste products. However, inflammation that occurs in any part within the digestive tract disrupts this natural process.
Generally, inflammatory bowel disease can be excruciatingly painful, debilitating, and disruptive. It can also even be fatal in extreme cases.
Types of Inflammatory Bowel Disease
Inflammatory bowel disease can be classified into the following types:
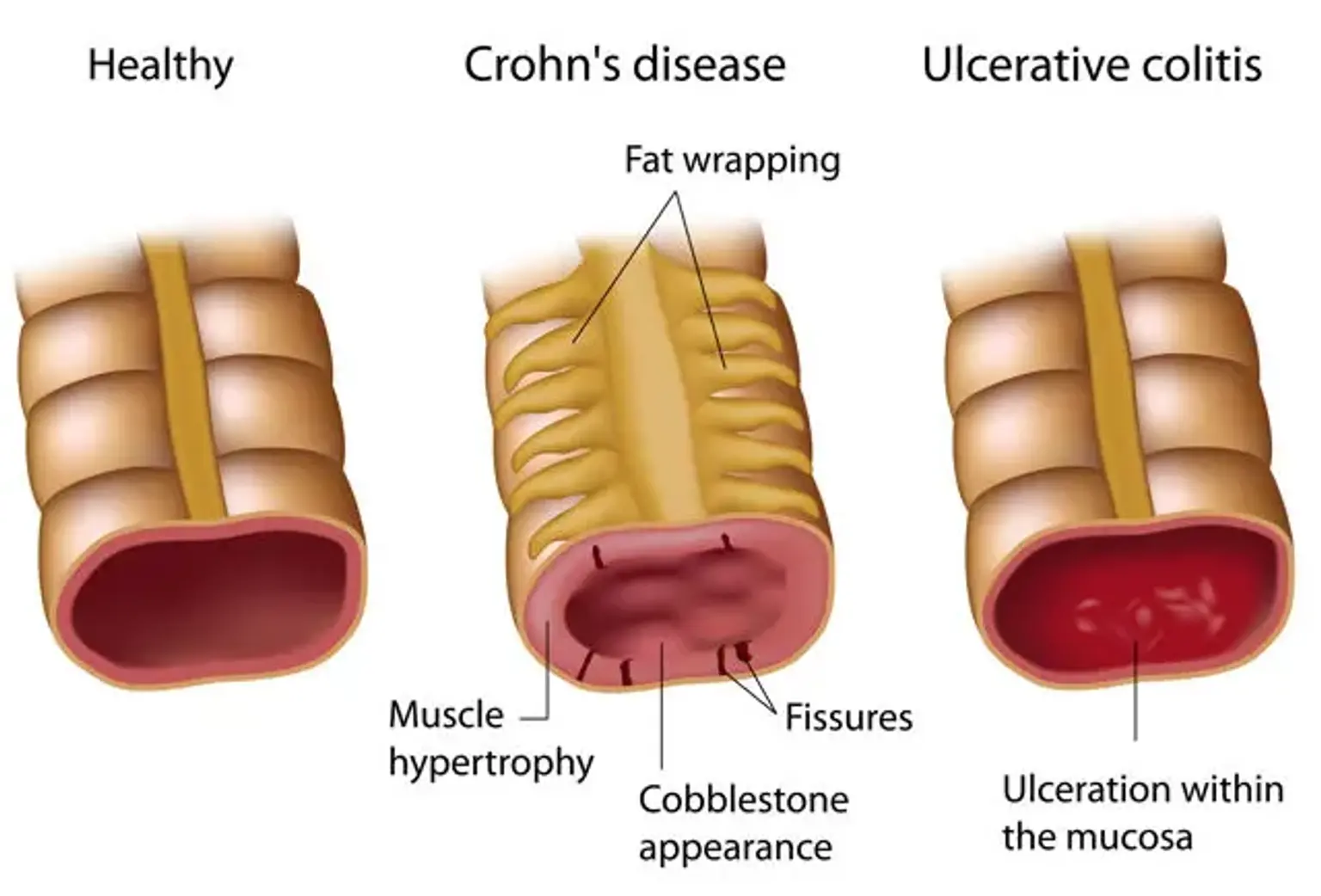
Ulcerative colitis: This disorder causes inflammation and sores (or ulcers) on the surface of the large intestine (colon) as well as the rectum.
Crohn's disease: This form of inflammatory bowel disease is associated with the inflammation of the digestive system lining. It frequently includes the digestive tract deeper layers.
Signs and Symptoms of Inflammatory Bowel Disease
The signs and symptoms of inflammatory bowel disease normally vary based on the severity of the inflammation and the location. The severity of the symptoms can range from mild to severe. There will most likely be episodes of active sickness, after which remission episodes follow.
The following signs and symptoms are prevalent in ulcerative colitis and Crohn's disease:
- Diarrhea: This happens if the affected areas of the bowel are unable to reabsorb water.
- Bleeding ulcers: This may result in blood in the stool, a disorder referred to as hematochezia.
- Because of bowel obstruction, you may experience cramping, stomach pain, and bloating.
- Weight loss and anemia: In children, this can result in physical growth and development delay.
Canker sores in the mouth are another symptom of Crohn's disease. At times, ulcers and fissures can form around the anus or genital area.
In addition, inflammatory bowel disease can be linked to other problems that are not part of the digestive system. They include inflammation of the eyes, skin problems, and arthritis.
Causes of Inflammatory Bowel Disease
The actual inflammatory bowel disease causes are unknown. Stress and diet were formerly suspected. However, doctors and gastroenterologists now understand that these factors might worsen. Besides, they are not the underlying cause of inflammatory bowel disease.
An immune system malfunction is one potential cause. The role of the immune system involves fighting off the invading bacteria and viruses. However, an abnormal reaction makes the immune system attack digestive tract cells as well.
Inflammatory bowel disease appears to be more popular among individuals with family members who have the disease. This indicates that heredity may play a role. Many people who have inflammatory bowel disease, on the other hand, do not usually have a family history.
Risk Factors of Inflammatory Bowel Disease
The following risk factors can contribute to the development of inflammatory bowel disease:
Age: The majority of people with inflammatory bowel disease are normally diagnosed before the age of 30. However, others do not develop the disorder until they are in their 50s or 60s.
Family history of the disease: If you have a blood relative with inflammatory bowel disease (a parent, child, or sibling), you probably have increased risks.
Ethnicity or race: Whereas whites are at the highest risk of contracting the disease, it can affect people of any race.
Nonsteroidal anti-inflammatory drugs (NSAIDs): Ibuprofen (Advil, Motrin IB, and others), naproxen sodium (Aleve), and diclofenac sodium, among others are examples of NSAIDs. These drugs can increase the likelihood of getting inflammatory bowel disease. It can also aggravate the condition for those who already have it.
Cigarette smoking: Smoking cigarettes is the most significant modifiable risk factor associated with Crohn's disease. Cigarette smoking may aid in the prevention of ulcerative colitis. Nonetheless, the damage to your overall health exceeds the benefit. Hence, quitting can enhance digestive tract health while also providing other various health benefits.
Inflammatory Disease Diagnosis
The gastroenterologist often diagnoses an inflammatory bowel disease by ruling out the potential reasons for the signs and symptoms. A combination of these tests and procedures may be necessary to help verify an inflammatory bowel disease diagnosis:
- Laboratory tests
Anemia and infection tests: The medical provider can order blood tests to look for anemia. This is a condition whereby there are no sufficient red blood cells to transport enough oxygen to tissues and organs. The tests also check for infection signs from viruses or bacteria.
Stool analysis: Your doctor can ask you to give a sample of your stool to check for hidden or occult blood in the stool and other organisms like parasites.
- Endoscopic procedures
Sigmoidoscopy:
The provider employs a sigmoidoscope, a thin, flexible tube attached to a camera, and illumination during this procedure. It visually analyzes the last parts of the large intestine, including the rectum and sigmoid colon.
This procedure involves inserting a sigmoidoscope via the anus into the intestinal wall to check for ulcers, inflammation, and bleeding visually. The doctor can also remove samples of the intestinal lining (biopsies) using a device inserted in the tube. The sample is then examined under a microscope in the lab.
Colonoscopy:
This procedure is similar to a sigmoidoscopy, only that the doctor will examine the entire colon with a colonoscope. A colonoscope is a long flexible tube. It allows the doctor to see the extent of the condition within the colon.
Upper endoscopy:
The specialist examines the stomach, esophagus, and duodenum (the first section of the small intestine) during this procedure using a thin, flexible, illuminated tube. Although these areas are rarely affected by Crohn's disease, upper endoscopy may be ordered if you are experiencing nausea and vomiting, upper abdominal pain, and difficulty feeding.
Capsule endoscopy:
Another diagnosis option is capsule endoscopy. A person is required to swallow a capsule containing a camera in this procedure. This enables the medical provider to inspect the small intestine thoroughly.
- Imaging tests
X-ray: For symptoms that are severe, the doctor may perform a standard x-ray on the abdomen to rule out major complications like a perforated colon.
Computerized tomography (CT) scan: A CT scan (a type of x-ray) gives more details, unlike the standard x-ray. This exam examines the whole bowel and the tissues located outside the bowel.
Magnetic resonance imaging (MRI): This provided detailed pictures of tissues and organs using radio waves and magnetic fields. An MRI is most helpful in assessing a fistula in the anal area or the small intestine.
Inflammatory Bowel Disease Treatment
The aim of treating inflammatory bowel disease is to lessen the inflammation causing the signs and symptoms. In the best-case scenario, this may result in both symptom relief and long-term remission and reduced complications.
Inflammatory bowel disease treatment typically entails:
Medications:
Medical providers can prescribe some medications to treat inflammatory bowel disease. They normally start with milder treatments and progress to aggressive ones later. Examples of these medications are:
- Anti-inflammatory drugs: Typically, 5-ASA drugs are the first line of defense for the symptoms. They help lessen inflammation around the gut and can aid in the achievement and maintenance of remission.
- Corticosteroids: When the mild treatment of anti-inflammatories is ineffective, a doctor can recommend fast-acting anti-inflammatory steroids.
- Immune suppressors: They work by inhibiting the immune system against attacking the bowel cells. As a result, it reduces inflammation.
- Biologic therapies: These involve antibodies that focus on particular substances causing inflammation within the body.
Other medications that can help with the symptoms of inflammatory bowel disease are;
- Antibiotics
- Antidiarrheal medications
- Laxatives
- Vitamin and mineral supplements for the nutritional deficiency caused by the disease
Surgery:
Surgery might be required in some cases to treat inflammatory bowel disease and complications. Depending on the condition, the medical provider may advise a surgical procedure to expand a narrow bowel or take out any fistulas.
People who have ulcerative colitis may require an operation to take out the colon and rectum. On the other hand, those who have Crohn's disease may require surgery to remove some sections of their intestines.
Lifestyle changes:
Some dietary and lifestyle choices can aggravate inflammatory bowel disease symptoms. Making positive adjustments to such habits, on the other hand, can help manage symptoms, lessen flares, and maintain remission.
These inflammatory bowel disease diet changes are beneficial for those with the disease:
- Limit dairy products intake
- Restrict the consumption of high-fat foods
- Restrict the consumption of spicy foods, alcohol, and caffeine
- Limit the consumption of high fiber foods
- Take a lot of water
In addition, most people with inflammatory bowel disease report that their symptoms worsen during stressful times. As a result, learning how to manage stress can aid in reducing the frequency and seriousness of these flares.
Some of the stress-reducing techniques are:
- Exercise
- Meditation
- Breathing workouts
- Progressive muscle relaxation
- Taking up hobbies and other pleasurable activities
Conclusion
The majority of people with inflammatory bowel disease normally lead active and healthy lives. Nonetheless, Crohn's disease and ulcerative colitis symptoms can be debilitating. After taking medications, some people experience remission or episodes with no symptoms.
On the other hand, other people require surgery to address severe flare-ups symptoms. Generally, your healthcare provider may recommend dietary and lifestyle changes to help manage your inflammatory bowel disease.