Introduction
Inverted nipple correction surgery is a procedure aimed at resolving the condition where the nipples retract inward instead of protruding outward. This can affect one or both nipples and can range from mild to severe cases. While inverted nipples aren't typically harmful to physical health, they can significantly impact one's self-esteem and body image.
For many, having inverted nipples may lead to feelings of self-consciousness, particularly in situations where the chest is exposed. Some people also experience difficulties with breastfeeding, depending on the severity of the inversion. Fortunately, this minimally invasive surgery offers a solution, improving both appearance and functionality.
The procedure is gaining popularity due to its quick recovery time, natural-looking results, and positive impact on confidence. It is an effective way to address a condition that can affect many aspects of a person’s life, from clothing choices to intimacy. In this article, we will explore the surgery in detail, including the process, risks, and benefits, to help you determine if it’s the right option for you.
Understanding Inverted Nipples: Causes and Impact
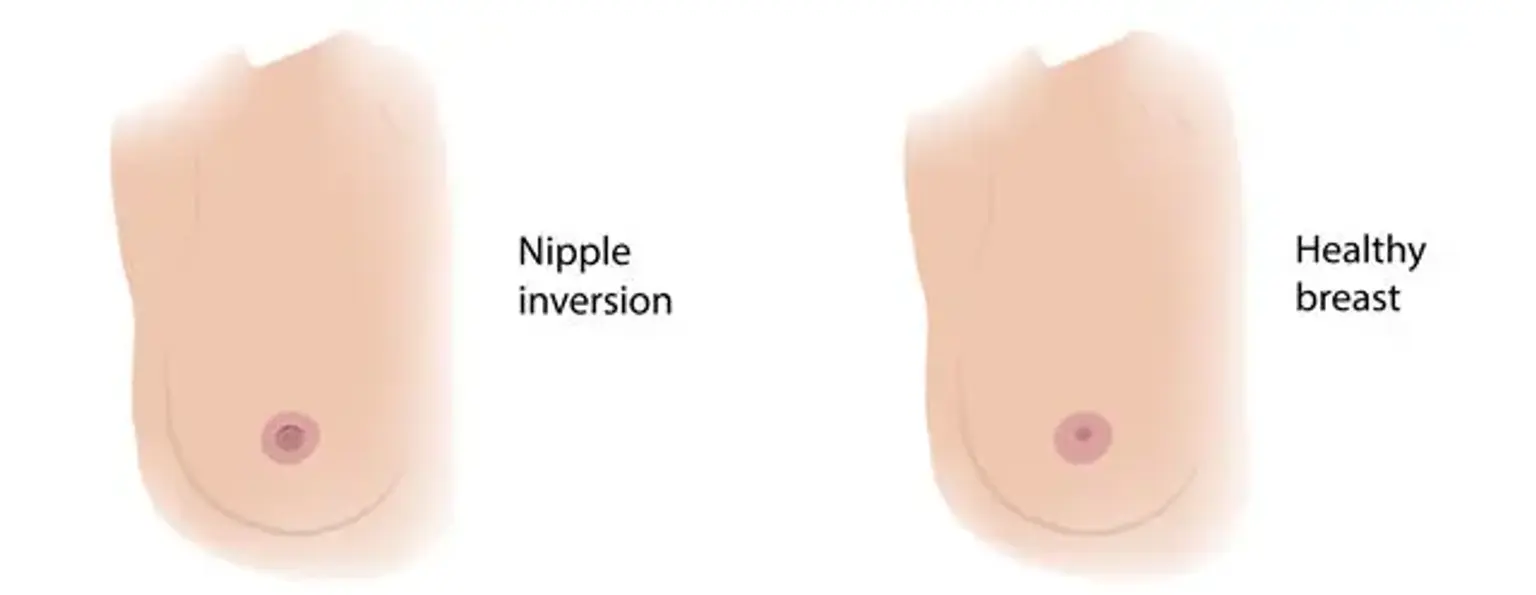
Inverted nipples occur when the nipple retracts into the breast rather than protruding outward. This can happen for several reasons. Genetics often play a role—some people are born with inverted nipples, while others develop the condition due to factors such as trauma, surgery, or breastfeeding difficulties. Hormonal changes during puberty or pregnancy can also contribute to the development of inverted nipples.
Although this condition is generally harmless, it can have a significant impact on one’s confidence. The appearance of inverted nipples can make people feel embarrassed or self-conscious about their body. For those who want to breastfeed, the inversion can create difficulties, as the milk ducts may be compressed or too short to allow for effective breastfeeding.
Addressing inverted nipples through surgery can improve both appearance and functionality. Patients often report a boost in self-esteem and a sense of relief after the correction, especially when the procedure allows them to breastfeed more easily.
Grades of Inverted Nipples: How Severe Is It?
Inverted nipples are classified into three grades based on their severity. This classification helps determine the best course of treatment and what patients can expect from surgery.
Grade 1: The nipple is mildly inverted but can protrude with gentle stimulation such as touch or temperature. This is typically the least severe form, and breastfeeding is usually not affected.
Grade 2: The nipple is more noticeably inverted and may protrude temporarily with stimulation, but it quickly returns to its inverted position. Breastfeeding is still possible with some adjustments.
Grade 3: This is the most severe form, where the nipple remains inverted at all times and cannot be everted with any external stimulation. In these cases, breastfeeding may be very difficult or impossible, and the correction is more complex.
The degree of inversion impacts the approach to surgery and expected outcomes. Less severe cases (Grade 1 or 2) typically require simpler procedures and have shorter recovery times, while more severe cases (Grade 3) might require more extensive surgical intervention to ensure long-lasting results.
The Inverted Nipple Surgery Procedure: Step-by-Step
Inverted nipple correction surgery is usually performed under local anesthesia, making it a minimally invasive procedure. Here’s what you can expect during the surgery:
Consultation and Planning: Before the surgery, you will meet with your surgeon to discuss your goals, medical history, and the extent of your nipple inversion. This consultation ensures that your surgeon understands your needs and can tailor the procedure to suit you.
The Procedure: During surgery, small incisions are made at the base of the nipple. These incisions allow the surgeon to release the tight or shortened milk ducts that are causing the inversion. Once the ducts are freed, the nipple is repositioned and stitched into its new, protruding position. The incisions are usually very small and well-hidden, leading to minimal scarring.
Duration: The surgery typically takes about 30 to 60 minutes, depending on the severity of the inversion. Most patients can go home the same day after the procedure.
This surgery is effective for improving the appearance of the nipples and can also restore breastfeeding capability, especially in Grade 1 and Grade 2 cases. It is a relatively quick procedure with minimal downtime, making it a popular choice for those seeking aesthetic improvement or functional correction.
Minimally Invasive Techniques for Nipple Correction
Inverted nipple correction has evolved with modern, minimally invasive techniques. These methods use tiny incisions that reduce scarring and promote quicker recovery. By carefully releasing the tissue that causes the nipple to invert, surgeons can restore its natural position without extensive surgery.
This approach ensures less trauma to the surrounding tissues and a faster healing process, making the procedure a more attractive option for many patients. It also minimizes the need for large, noticeable scars, a common concern with traditional breast surgeries.
Techniques for Nipple Protrusion and Fixation
There are various surgical techniques to correct inverted nipples, and the choice depends on the severity of the condition. One common method is the use of internal sutures to hold the nipple in place. Another technique involves a “parachute flap,” which uses tissue from around the nipple to secure it in the desired position.
For more severe cases (Grade 3), additional procedures may be needed to help maintain the nipple’s new position long-term. Surgeons also ensure that these methods don’t disrupt the function of the milk ducts in cases where breastfeeding is a concern.
Combining Inverted Nipple Surgery with Other Breast Procedures
In some cases, inverted nipple correction is combined with other breast surgeries like breast augmentation or breast lifts. This is particularly beneficial for those who want both aesthetic improvement and nipple correction.
By addressing the nipple inversion during a breast lift or augmentation, the surgeon can make a single incision around the areola, which improves both the shape of the breast and the nipple's projection. This can also enhance the overall outcome, as it provides a more cohesive aesthetic result.
Post-Surgical Recovery: What to Expect
Recovery after inverted nipple correction surgery is typically swift, with most patients able to return to normal activities within 1-2 weeks. Initially, there may be swelling, bruising, and mild discomfort, which can be managed with prescribed medications.
Patients are advised to wear a special support garment to help the healing process and to avoid strenuous activities for a few weeks. Follow-up appointments are crucial to ensure proper healing and to address any concerns, such as scarring or complications. Full results are usually visible within a few months.
Expected Results: When Will You See Final Outcomes?
After inverted nipple correction surgery, most patients see initial improvements right away, but the final results may take a few months to fully develop. During this period, swelling and bruising will gradually subside, and the nipple will settle into its new position.
The full healing process can take up to six months, depending on the individual’s healing rate. Scarring is usually minimal, and the nipples typically maintain their new projection, offering long-term aesthetic benefits. Patients who follow post-operative care instructions closely are more likely to achieve optimal results.
Potential Risks and Complications
Like any surgery, inverted nipple correction carries some risks. These can include infection, excessive scarring, changes in nipple sensitivity, or, in rare cases, nipple retraction. While these complications are uncommon, choosing a skilled surgeon can significantly reduce the likelihood of such issues.
It’s also important to have realistic expectations. While the procedure generally offers excellent results, the outcome can vary depending on the severity of the inversion and the patient's health. Discussing potential risks with your surgeon will help you make an informed decision.
Inverted Nipple Surgery and Breastfeeding
One of the common concerns with inverted nipple surgery is whether it will affect breastfeeding. While surgery can improve the ability to breastfeed in some cases, the risk of complications, such as milk duct damage, remains. For patients who plan to breastfeed, it’s essential to discuss this concern with the surgeon ahead of time.
In many cases, surgeons take care to preserve the milk ducts during surgery. However, in severe cases of nipple inversion, breastfeeding may still be challenging, despite the correction. Each case is unique, so it’s important to have a personalized consultation.
Who is a Good Candidate for Inverted Nipple Surgery?
Inverted nipple surgery is suitable for individuals who experience psychological or physical challenges due to their inverted nipples. The procedure is ideal for those whose nipple inversion is moderate to severe (Grade 2 or 3) and who are in good overall health.
It is particularly beneficial for women who are not planning to have children in the near future, as pregnancy and breastfeeding can alter the results. However, some women who wish to breastfeed in the future may still choose the surgery, depending on their goals and the surgeon’s recommendations.
Preparing for Your Nipple Correction Surgery
Preparing for inverted nipple correction surgery is essential for ensuring a smooth procedure and recovery. During your consultation, your surgeon will assess your overall health and medical history, and they may request a physical exam. You may also need to stop certain medications, like blood thinners, a few weeks before surgery to reduce the risk of bleeding.
Before the surgery, your surgeon will provide instructions on how to care for your skin, what to wear on the day of the surgery, and any dietary restrictions. It’s important to arrange for someone to drive you home after the procedure since the anesthesia may make you feel drowsy.
Aftercare: Ensuring a Smooth Recovery
Proper aftercare is crucial for the success of the surgery and minimizing complications. After inverted nipple correction surgery, you will need to wear a supportive bra or compression garment for several weeks to reduce swelling and support healing.
It’s also important to avoid any strenuous activity, such as lifting heavy objects or exercising, for about 4-6 weeks. Your surgeon will schedule follow-up appointments to check on your progress and remove any stitches, if necessary. During this time, you should also be mindful of any signs of infection, like increased redness, swelling, or unusual pain.
Understanding Costs and Financing Options
The cost of inverted nipple correction surgery can vary widely depending on the surgeon's experience, the complexity of the procedure, and the location of the clinic. On average, the procedure can cost between $3,000 and $5,000.
Many clinics offer financing options or payment plans to help make the surgery more affordable. It’s important to check with your insurance provider, as some plans may cover part of the cost if the procedure is deemed medically necessary, particularly if it’s affecting breastfeeding or causing significant psychological distress.
Patient Testimonials: Real Experiences with Inverted Nipple Surgery
Patient testimonials offer valuable insight into the real-life outcomes of inverted nipple correction surgery. Many patients report feeling a significant boost in confidence and improved body image after the procedure. The ability to wear certain clothing, engage in activities like swimming, or simply feel more comfortable with their appearance is a common positive result.
Before-and-after photos shared by patients can show the dramatic transformation in nipple projection. These real experiences emphasize that the surgery not only addresses a cosmetic concern but also has a lasting impact on a person's quality of life.
What to Look for in a Surgeon: Finding the Right Expert
Choosing the right surgeon is crucial to achieving the best possible results from your inverted nipple correction surgery. Look for a board-certified plastic or reconstructive surgeon who specializes in breast procedures. Experience in nipple correction and a strong track record with similar surgeries is key to ensuring a safe and effective outcome.
When selecting a surgeon, consider factors like their before-and-after photos, patient reviews, and comfort level during your consultations. The best surgeons will listen to your concerns, offer realistic expectations, and prioritize your safety. Don't hesitate to ask about their experience with inverted nipple surgeries and their approach to managing complications.
Inverted Nipple Surgery Around the World: Popularity and Trends
Inverted nipple correction surgery has gained widespread popularity, not just in the United States, but globally. Countries with high demand for cosmetic breast procedures, like Brazil, South Korea, and the United Kingdom, have seen a rise in patients seeking nipple correction surgery.
The trend reflects an increased focus on body positivity and cosmetic surgery as a means of improving self-esteem. While the surgery itself is standard across many countries, some regions may offer more affordable options or shorter wait times. It’s important to research the standards and regulations in each country before considering international surgery.
Common Misconceptions about Inverted Nipple Correction
There are several misconceptions surrounding inverted nipple correction surgery that can cause confusion or hesitation for potential patients. One common myth is that the procedure is extremely painful. In reality, the surgery is performed under local anesthesia, and recovery pain is typically manageable with over-the-counter medications.
Another misconception is that the surgery always results in noticeable scarring. While there will be some scarring, modern techniques often involve small incisions that heal well, leaving minimal visible marks. Additionally, many people worry that the surgery will impact breastfeeding ability, but in most cases, skilled surgeons can preserve milk ducts and enable breastfeeding.
Concluaion
Inverted nipple correction surgery offers both cosmetic and functional benefits, helping individuals feel more confident and comfortable with their appearance. It can also improve breastfeeding ability in some cases, making it a worthwhile consideration for those affected by nipple inversion.
Ultimately, whether the surgery is right for you depends on your personal goals, the severity of the inversion, and your overall health. A thorough consultation with a qualified surgeon will help you understand what to expect, the risks involved, and the potential benefits. If you’re self-conscious about your inverted nipples and want to explore your options, this procedure could significantly improve both your physical and emotional well-being.