Ischemic Heart Disease
Overview
Ischemic heart disease is a dynamic process characterized by atherosclerosis of the coronary arteries or functional changes in coronary circulation that can be addressed via lifestyle changes, pharmaceutical treatments, and revascularization. The illness may be stabilized or regressed as a result of such therapy. The clinical manifestations of ischemic heart disease are now classified as either acute coronary syndrome or chronic coronary syndrome, using new nomenclature.
A decrease in the incidence of obstructive coronary artery disease in a symptomatic population results in a decreased pretest probability and clinical likelihood of disease, which influences the diagnostic work-up. Noninvasive functional or anatomic imaging for myocardial ischemia is indicated as the initial test to detect coronary artery disease in symptomatic individuals when clinical examination alone cannot rule out obstructive disease.
What is ischemic heart disease?
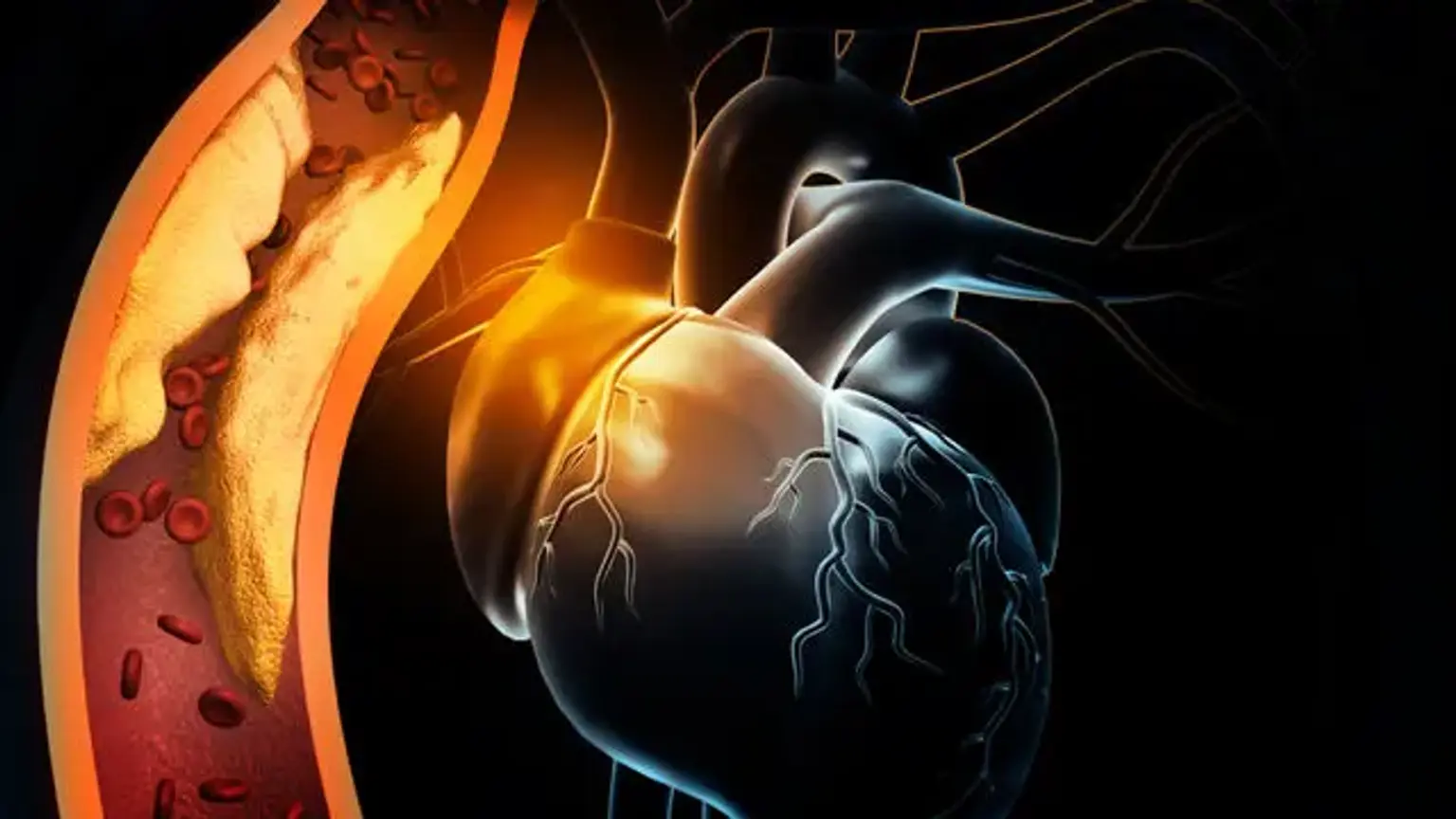
Ischemia is described as insufficient blood supply (circulation) to a particular area as a result of a blockage of the blood vessels feeding the area. Ischemic indicates that an organ (for example, the heart) is not receiving adequate blood and oxygen. Ischemic heart disease, also known as coronary heart disease (CHD) or coronary artery disease, refers to cardiac difficulties caused by constricted coronary arteries, which feed blood to the heart muscle. Although the narrowing might be caused by a blood clot or a constriction of the blood artery, it is most commonly caused by plaque formation, which is known as atherosclerosis.
When blood supply to the heart muscle is entirely interrupted, the heart muscle cells die, resulting in a heart attack, also known as a myocardial infarction (MI). The majority of persons with early (less than 50% constriction) CHD do not have symptoms or blood flow limitations. However, symptoms may develop as the atherosclerosis advances, especially if left untreated. They are particularly likely to develop during physical activity or mental stress, when the demand for the oxygen transported by the blood increases.
Angina pectoris is the discomfort felt when the heart muscle does not receive enough oxygen. This is a clinical condition characterized by chest, jaw, shoulder, back, or arm pain that is increased by activity or mental stress and is quickly alleviated by rest or by taking nitroglycerin. Angina is most commonly seen in patients with CHD, although it can also occur in people with valvular disease, hypertrophic cardiomyopathy, and uncontrolled hypertension. Patients with normal coronary arteries may occasionally have angina due to coronary spasm or endothelial dysfunction.
Angina
The Canadian Cardiovascular Society (CCS) classification method is used to grade angina or an anginal analogue (e.g., exertional dyspnea) based on a description of the degree of activity that induces symptoms.
Angina in Class I is described as angina that develops during severe, fast, or protracted effort at work or recreation but not during normal physical activity. Chopping wood, climbing hills, cycling, aerobic ballet, ballroom (quick) or square dancing, jogging a 10-minute mile, rope skipping, skating, skiing, playing tennis or squash, and walking 5 miles per hour are all Class I activities.
Class II angina is defined as angina that slightly limits ordinary activity, such as walking or climbing stairs rapidly, walking or climbing stairs uphill, walking or climbing stairs after meals; in cold or wind; under emotional stress; only during the first few hours after awakening; or walking more than two blocks on level ground and climbing more than one flight of ordinary stairs at a normal pace and under normal conditions.
Walking one or two blocks on level ground, ascending one flight of stairs in normal conditions and at normal pace, playing a musical instrument, completing home chores, gardening, vacuuming, walking a dog, or taking out the garbage are all examples of Class III physical activity limitations.
Class IV is distinguished by the inability to engage in any physical activity without discomfort; anginal symptoms may be present even when resting. As many as 3 to 4 million Americans may suffer from silent ischemia, often known as ischemia without discomfort or a heart attack without warning. People suffering from angina may also have undetected periods of silent ischemia. Individuals who have had a heart attack or who have diabetes are also at risk of developing silent ischemia.
Epidemiology
The yearly incidence of MI is predicted to be 935,000, including 610,000 new and 325,000 recurring infarctions. The total prevalence of angina pectoris is 4.6 percent, with women having a greater age-adjusted prevalence than males. More than half of all cardiovascular events in men and women under the age of 75 are caused by CHD. After the age of 40, males have a 49 percent lifetime chance of getting CHD and women have a 32 percent lifetime risk.
Cardiovascular disease is the main cause of mortality in both men and women. In 2006, it was responsible for one out of every six fatalities in the United States; CHD mortality was 425,425, while MI mortality was 141,462. Every 25 seconds, an American will have a coronary event, and every minute, a person will die as a result of a coronary event. Every 34 seconds, an American will have a MI, and 15% will die as a result of it.
Ischemic heart disease causes
Ischemia-related heart disease is a complex condition. Non-modifiable and modifiable etiologic factors can be broadly classified. Gender, age, family history, and genetics are examples of non-modifiable elements. Smoking, obesity, cholesterol levels, and psychosocial variables are all modifiable risk factors. A faster-paced lifestyle in the Western world has caused individuals to eat more fast foods and unhealthy meals, leading to a rise in the prevalence of ischemic heart disease.
Better primary care in the middle and upper socioeconomic classes in the United States has moved the occurrence to later in life. Smoking is still the leading cause of cardiovascular disease. The frequency of smoking among adults in the United States was determined to be 15.5 percent in 2016.
The male gender is prone to be more susceptible than the female gender. Hypercholesterolemia is still a significant modifiable risk factor for coronary artery disease. Raised low-density lipoproteins (LDL) increased the risk of CAD, whereas increased high-density lipoproteins (HDL) decreased the risk of CAD.
Pathophysiology
The formation of atherosclerotic plaque is a hallmark of the pathogenesis of ischemic heart disease. Plaque is a fatty substance buildup that narrows the artery lumen and obstructs blood flow. The creation of a "fatty streak" is the first phase in the process. The formation of a fatty streak is caused by the subendothelial deposition of lipid-laden macrophages, often known as foam cells. When a vascular insult occurs, the intima layer ruptures, and monocytes move into the subendothelial region, where they differentiate into macrophages.
These macrophages absorb oxidized low-density lipoprotein (LDL) particles, resulting in the formation of foam cells. T cells are activated, and cytokines are released only to help in the pathogenic process. Released growth factors activate smooth muscles, which pick up oxidized LDL particles and collagen and deposit them alongside activated macrophages, increasing the number of foam cells. Subendothelial plaque is formed as a result of this procedure.
If the endothelium is not further harmed, this plaque may expand in size or become stable over time. If the lesion becomes stable, a fibrous cover will develop, and the lesion will calcify over time. With time, the lesion might become hemodynamically substantial enough that not enough blood reaches the cardiac tissue during times of elevated demand, resulting in angina symptoms.
At rest, however, symptoms would subside as the oxygen need decreases. A lesion must be at least 90% stenosed in order to elicit angina at rest. Some plaques can break, exposing tissue factor and resulting in thrombosis. Depending on the severity of the insult, this thrombosis might result in subtotal or complete blockage of the lumen and the development of acute coronary syndrome (ACS) in the form of unstable angina, NSTEMI, or STEMI.
Classification of ischemic heart disease is typically done as under:
- Stable ischemic heart disease (SIHD)
- Acute coronary syndrome (ACS)
- ST-elevation MI (STEMI)
- Non-ST elevation MI (NSTEMI)
- Unstable angina
Ischemic heart disease symptoms
Before proceeding with additional workup, it is critical to obtain a thorough history and physical examination. Coronary artery disease can present as either stable ischemic heart disease (SIHD) or acute coronary syndrome (ACS) (ACS). If not treated, it can lead to congestive heart failure (CHF). Patients should be questioned regarding chest discomfort, its relationship to physical exertion, and pain radiating into the jaw, neck, left arm, or back.
Dyspnea should be examined both at rest and during exercise. Inquire about syncope, palpitations, tachypnea, lower extremities edema, orthopnea, and exercise ability. A family history of ischemic heart disease, as well as dietary, smoking, and lifestyle behaviors, should be collected.
Inspection, palpation, and auscultation should all be part of the physical examination. Acute distress, jugular venous distention, and peripheral edema should all be looked for. When palpating, look for fluid thrills and heaves. If there is peripheral edema, the degree of it should be assessed. The jugular vein distension should be measured. The heart should be auscultated in all four places, and the lungs should be auscultated as well, with a specific emphasis on the lower zones.
Diagnosis
To mention a few, the major modalities for evaluating coronary artery disease include EKG, Echo, CXR, Stress test, cardiac catheterization, and blood tests. These examinations are performed based on the circumstances in which patients appear. The following are details on the many diagnostic methods we have for evaluating coronary artery disease:
- Electrocardiogram (EKG)
The electrocardiogram (EKG) is a simple but extremely useful test in the diagnosis of coronary artery disease. It detects electrical activity in the cardiac conduction system using ten leads placed to the skin at specified places. It explains the physiology as well as the architecture of the heart.
It usually contains 12 leads on the paper that is printed after the test, and each lead corresponds to a distinct place of the heart. The rate, rhythm, and axis of the heart are all important things to look for on an EKG. Following that, data on acute and chronic pathologic processes can be acquired. ST-segment and T-wave abnormalities can be seen in acute coronary syndrome.
It is also possible to observe if an ACS has developed into arrhythmias. In chronic situations, EKG might reveal axis deviation, bundle branch blockages, and ventricular hypertrophy. EKG is also a low-cost, easily accessible testing modality that is not user-dependent.
- Echocardiography
Echocardiography is a type of heart ultrasonography. It is a non-invasive way of testing that is used in both acute and chronic situations, as well as inpatient and outpatient settings. It might reveal information on wall motion, valvular regurgitation and stenosis, infective or autoimmune diseases, and chamber diameters in acute circumstances.
It can also be used to diagnose acute pulmonary diseases such as pulmonary embolism. The pericardial cavity is also assessed. It may be done in chronic situations to see the same information indicated above as well as a response to therapy. It is also utilized as part of stress testing in an outpatient environment. In addition to diagnostics, it has a therapeutic purpose; for example, pericardiocentesis might be done with a needle guided by echocardiography. This test is user-dependent and may be more expensive than an EKG.
- Stress Test
The stress test is a non-invasive method of assessing coronary artery disease. When read in an appropriate situation, it is useful in ruling in or ruling out cardiac disease in the case of suspected angina or angina similar. The heart is artificially stressed throughout the test, and if the patient has specific abnormal EKG abnormalities in ST segments or symptoms of angina, the test is terminated and coronary artery disease is confirmed.
- Chest X-ray
A chest X-ray is an important part of the first assessment of heart illness. Standing posteroanterior (PA) and left lateral decubitus imaging images are typical. Anteroposterior (AP) projection is occasionally acquired, particularly in inpatient settings with the patient laying down; nevertheless, the interpretation of AP films is severely constrained. Analyzing PA and AP views correctly gives important and cost-effective information on the heart, lungs, and vasculature. Interpretation should be done in a step-by-step manner to avoid overlooking vital information.
- Blood Work
Blood testing assists in making a diagnosis and evaluating therapy responses. In emergency situations, cardiac enzymes and B-type natriuretic peptides are frequently performed in addition to complete blood counts and metabolic panels. BNP offers information on cardiogenic volume overload, however it has limits.
It can be exaggerated in renal illness and exaggerated in obesity. Cardiac enzymes such as CK and troponin can detect an acute ischemia event. In chronic conditions, a lipid panel can give valuable prognostic information. C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) can be used to diagnose diseases such as acute pericarditis.
Liver function tests (LFTs) can be used to screen for an infiltrative process that can damage both the liver and the heart at the same time, such as hemochromatosis. Liver tests are also used to examine elevated right heart pressures, particularly in chronic cases.
- Cardiac Catheterization
Cardiac catheterization is the gold standard and most reliable method of assessing ischemic coronary heart disease. However, it is an intrusive treatment with potential risks. The technique is not appropriate for everyone. Patients with an intermediate pretest likelihood for CAD are typically the best candidates for it in non-ACS settings.
All STEMI patients and chosen NSTEMI patients are given an urgent cardiac catheterization in the ACS situation. This technique is performed in a cardiac catheterization lab, requires competence, and is performed under mild sedation. The technique includes contrast exposure, which might result in severe allergic responses and renal damage.
Ischemic heart disease treatment
Coronary artery disease can manifest itself as either stable ischemic heart disease (SIHD) or acute coronary syndrome (ACS) (ACS). The former appears in a chronic situation, whereas the latter appears in an acute setting. The treatment is determined on the type of sickness. We shall go over each subtype's management separately:
Stable Ischemic Heart Disease
The most common symptom of stable ischemic heart disease is stable angina. Stable angina is defined as substernal chest discomfort or pressure that increases with effort or mental stress and is eased by rest or nitroglycerin and lasts for at least two months. It is vital to understand that conventional anginal symptoms may be missing and that it may show differently with atypical symptoms and exertional dyspnea in particular demographic groups such as women, the elderly, and diabetics.
Non-pharmacologic and pharmacologic therapies are used to treat SIHD. Smoking cessation, regular exercise, weight loss, good diabetes and hypertension control, and a balanced diet are all examples of lifestyle changes. Cardioprotective and antianginal medicines are examples of pharmacologic treatments.
Every patient should get combination of low-dose aspirin, beta-blockers, as-needed nitroglycerin, and a moderate to high-intensity statin. If this does not manage the symptoms, beta-blocker medication should be increased to heart rates of 55-60, and the addition of calcium channel blockers and long-acting nitrates should be investigated.
To alleviate refractory anginal symptoms, ranolazine might be added. If maximum management fails to relieve angina, cardiac catheterization should be performed to view the coronary architecture, and a choice for percutaneous coronary intervention (PCI) or coronary artery bypass graft (CABG) should be made depending on the patient profile.
Acute Coronary Syndrome
Acute coronary syndrome is characterized by sudden onset substernal chest discomfort or pressure that generally radiates to the neck and left arm and is often accompanied by dyspnea, palpitations, disorientation, syncope, cardiac arrest, or new-onset congestive heart failure. Prompt EKG is required for all ACS patients to assess for STEMI, and is often performed pre-hospital by an emergency medical services team.
STEMI is identified by the presence of 1 mm ST elevation in contiguous limb or precordial leads (excluding V2 and V3). To be diagnosed with STEMI in V2 and V3, men must have 2 mm elevations and women must have 1.5 mm elevations.
High-dose statin medication and beta-blockers should also be started as soon as possible. Based on the patient's characteristics, P2Y12 inhibitors (prasugrel, ticagrelor, or prasugrel) should be begun. Patients with NSTE ACS should be treated with anticoagulants such as heparin or enoxaparin. For patients with intermediate to high TIMI values (>2), early invasive treatment within 24 hours is recommended for NSTEMI.
Regular visits to cardiologists and family doctors are essential for the long-term care of coronary artery disease. Medication adherence and lifestyle changes are critical.
Differential Diagnosis
Because of the closeness of the heart to surrounding organs such as the lungs, stomach, large veins, and musculoskeletal organs, coronary artery disease has a wide variety of differential diagnoses. Acute anginal chest pain may be mistaken for acute pericarditis, myocarditis, prinzmetal angina, pericardial effusion, acute bronchitis, pneumonia, pleuritis, pleural effusion, aortic dissection, GERD, peptic ulcer disease, esophageal motility abnormalities, and costochondritis.
Stable ischemic heart disease may also be mistaken for GERD, Peptic ulcer disease, costochondritis, and pleuritis. To narrow the differential diagnosis and achieve an appropriate diagnosis, the history, physical examination, and diagnostic investigations should be carefully performed.
Prognosis
The disease's prognosis is determined by a number of variables, some of which may be altered while others cannot. Some of the determinants are the patient's age, gender, family history and genetics, ethnicity, food and smoking habits, medication compliance, healthcare access and financial situation, and the number of arteries affected. Diabetes mellitus, hypertension, dyslipidemia, and chronic renal disease are all comorbid diseases that influence the overall result.
Complications
The most common complications linked with coronary artery disease are arrhythmias, acute coronary syndrome, congestive heart failure, mitral regurgitation, ventricular free wall rupture, pericarditis, aneurysm development, and mural thrombi.
Ischemic Heart Disease in Children
Ischemic heart disease in children is frequently caused by anatomical defects of the proximal coronary arteries, coronary fistulae, Kawasaki illness, or coronary artery damage during cardiac surgery. Ischemia can be diagnosed in children using stress or resting echocardiography, radionuclide perfusion tests, or cardiac magnetic resonance imaging, however two anomalies in two regions are not required. Ischemia treatment may include surgical or cardiac interventional procedures.
Conclusion
Ischemic heart disease (IHD) is one of the most serious cardiac conditions, characterized by a lack of oxygen flow to the myocardial cells.
Ischemia of the heart is caused by a mix of changeable and unmodifiable causes. On each routine appointment, primary care physicians should focus on modifiable risk factor modification. Controlling diabetes, hypertension, and cholesterol levels, as well as quitting smoking, losing weight, and exercising, can make a significant impact. Because it is a worldwide public health problem, greater awareness has to be generated in school curricula and various media outlets.