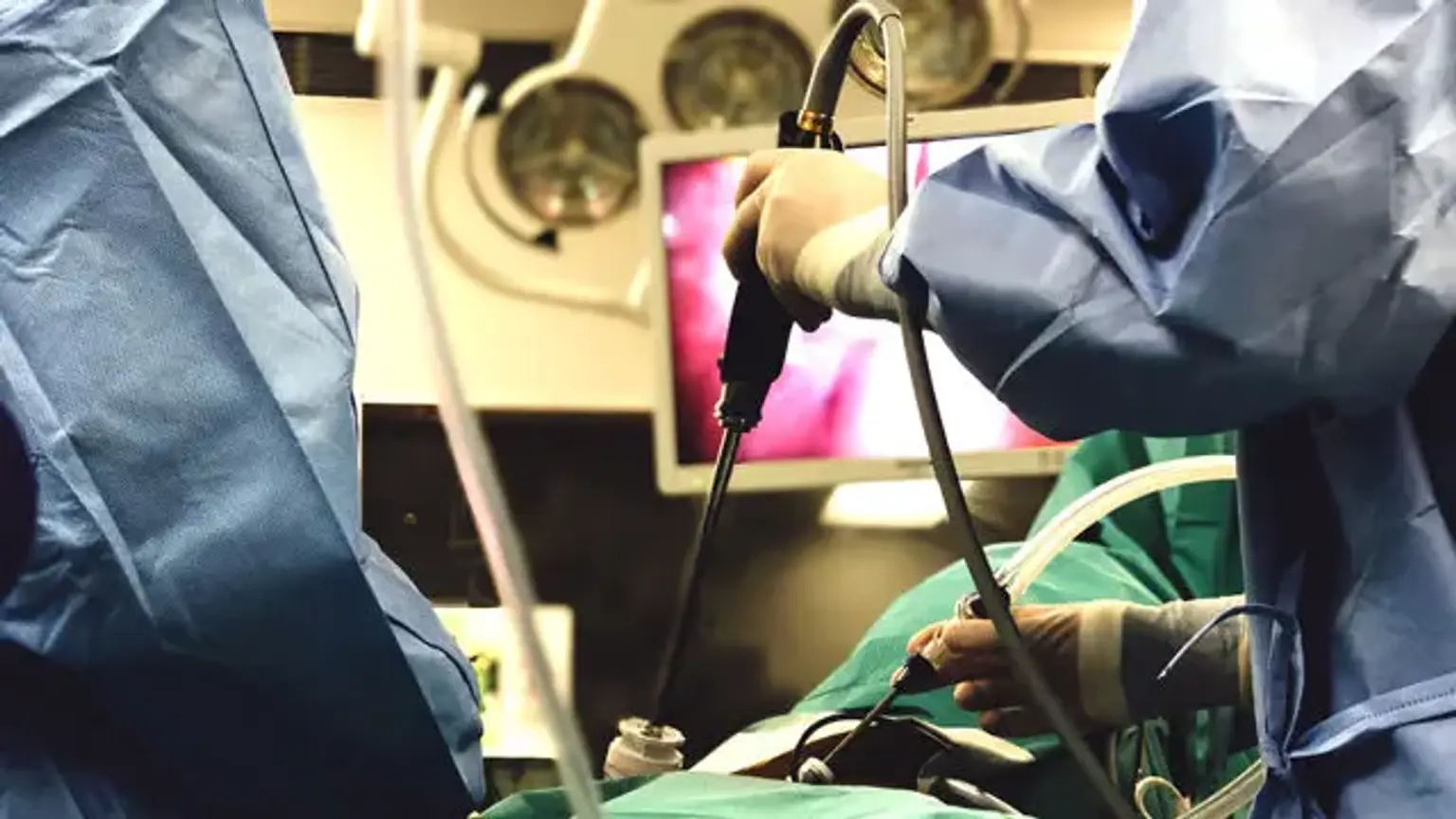
Laparoscopic Colorectal Surgery
In the last two decades, the advent of the laparoscopic method to cholecystectomy has been followed by the rapid adoption of this technique in a variety of surgical procedures. The laparoscopic revolution is an example of surgical innovation that has spread quickly through the academic community. Jacobs et al reported the first laparoscopically assisted colectomy in the 1990s. In comparison to open surgery, a large number of controlled trials and meta-analyses have indicated that laparoscopic colorectal surgery is related to reduced discomfort, faster bowel transit recovery, and shorter hospital stay. It's been proposed that laparoscopy's short-term benefits are linked to a reduced inflammatory response. Several studies have shown that laparoscopic colectomy results in lower serum levels of interleukin-6 and other proinflammatory cytokines, which are sensitive markers of tissue injury, than surgical resection.
However, when compared to cholecystectomy, appendectomy, or Nissen fundoplication, laparoscopic colonic surgery is a much more difficult procedure because it frequently involves more than one abdominal quadrant, identification and transection of vascular structures, mobilization and resection of the bowel, retrieval of the surgical specimen, and anastomosis. Longer operational hours and a steep learning curve have been linked to the increasing difficulty of laparoscopic colectomy. Because of these factors, despite its benefits, laparoscopic colectomy has taken several years to gain popularity.
What is Laparoscopic Colorectal Surgery?
Laparoscopic ('keyhole') colon surgery is a type of minimally invasive surgery in which diseased sections of the colon and rectal areas are viewed, cut, and removed using equipment with long, narrow tubes. A videoscope, which is a unique camera on the end of a tube, allows the surgeon to see the problem areas. The videoscope and other equipment are placed into the abdomen through small incisions (cuts). Under general anesthesia, the procedure is performed while you sleep.
Laparoscopic Colorectal Surgery Indications
A benign polyp 25-50 cm from the anal ring, mobile, inflammatory large bowel disease, and palliation in the case of malignant disease, particularly of the left hemi-colon, are all reasonable grounds for laparoscopic colorectal surgery. It needs to be demonstrated that laparoscopic colectomy is superior to open colectomy, not just comparable. This is particularly true for colorectal cancer resections with the goal of curing cancer. As a result, a prospective, randomized cost-benefit analysis should be conducted.
Laparoscopic surgery is not appropriate for all patients. Previous abdominal surgery, malignancy, obesity, or severe heart, lung, or renal disease are all medical factors that may make you unsuitable for this procedure. If you are not a candidate for laparoscopic surgery, we will perform the procedure as an open procedure instead. Occasionally, a laparoscopic procedure will begin, but if complications arise, the procedure will need to be modified to an open procedure.
Benefits of Laparoscopic Colorectal Surgery
When compared to an open operation (which requires a wider incision), the advantages of laparoscopic surgery may include:
- Excellent cosmetic outcomes (cuts are performed on the abdomen (tummy) that heal to leave fewer scars when healed).
- You will spend less time in the hospital (4-5 days) than if you had an open surgery (8-12 days).
- After laparoscopic colorectal surgery, you'll be able to resume the normal activities in 3-4 weeks and the normal diet the same day. Patients who have an open operation normally need a bit longer to go back to normal.
- You will have less pain and discomfort following a laparoscopic procedure because the wound is smaller.
Before Laparoscopic Colorectal Surgery
Before the surgery, doctors will ask you to come to the pre-assessment clinic. This appointment gives you the chance to make sure you're ready for admission, treatment, and return home.
Additional tests, such as a colonoscopy, barium enema, ECG (electrocardiogram), chest X-ray, CT scan of the abdomen, and blood tests, may be required to determine the surgical readiness.
Better bring a list of all your prescription treatments to this visit. You have to inform the surgeon if you are using any blood-thinning medications (such as warfarin or aspirin) or if you have any pharmaceutical allergies.
The anesthesiologist who will put you to sleep for the procedure may visit you at this appointment to make sure you're ready for it. They will then request your written permission to administer general anesthesia.
Before the surgery, you will be given carbohydrate liquids to drink; the nurse expert will instruct you on this.
On the day of your surgery, doctors will transfer you to the ward. The nurses will take your temperature, blood pressure, respiration rate, height, weight, and urine to establish a baseline from which to work.
Doctors will take your measurements for special stockings to prevent blood clots from forming in your legs after surgery. These should be worn the entire time you are in the hospital. To help reduce this risk, the doctor will start you on anti-coagulant (blood-thinning) treatments.
If your surgery is planned for the morning, you will be instructed to drink the carbohydrate drink that the preassessment nurses have given you in the morning, and in the evening if the operation is scheduled for the afternoon.
Before your surgery, physicians may ask you to stop using some of your medications. Your surgeon will give you advice.
On the Day of Laparoscopic Colorectal Surgery
Before heading to the operation room, please shower or bathe at home. Remove all cosmetics, nail polish, jewelry (excluding wedding rings, which can be kept in place), piercings, and dentures. After that, one of the nurses will arrive and prepare you for the surgery room.
If you haven't done so before in the clinic, the surgeon will examine you, explain the operation in detail, and ask you to sign a consent form. This is to ensure that you are aware of the dangers and benefits of the procedure.
Laparoscopic Colorectal Surgery Procedure
Because of the extensive laparoscopic skills required, laparoscopic colectomy requires a steep learning curve. Colorectal surgeries, unlike other laparoscopic procedures like the Nissen fundoplication or cholecystectomy, require dissection and movement of intra-abdominal organs in numerous quadrants. A specialized camera and various laparoscopic equipment are inserted through several small incisions during laparoscopic colorectal surgery. An insufflator inflates the peritoneal cavity with carbon dioxide to create a pneumoperitoneum, which offers a working space for the surgery. During a surgery, leaning the operating room table in various orientations allows intra-abdominal organs to slip away from the dissection area, providing the required exposure that would otherwise be achieved with the use of retractors. Laparoscopic ligation of major vessels, mobilization and excision of a long floppy piece of the colon, and restoration of intestinal continuity are all required for intestinal resection. After the colon section has been fully mobilized and its blood vessels have been split, a tiny skin cut is made to exteriorize the colon, an extracorporeal resection and anastomosis are done, and the rejoined colon is inserted back into the abdomen.
Laparoscopic Colorectal Surgery Risks
The hazards of general anesthesia are the same as they are for any other operation. This operation is unique in that:
- There is a 10% chance of an adverse event to the anesthetic.
- There is a 5% chance of abdominal bleeding, which would necessitate a blood transfusion.
- Infection in the abdomen or wounds in less than 5% of the time.
- Scar tissue poses a less than 10 to 15 percent chance of intestinal obstruction (blockage).
- The chance of bowel leakage is less than 15%.
- General anesthesia carries a risk of heart attack or pneumonia of less than 15%.
- Blood clots in the legs or lungs are fewer than 5% of the time.
- Accidental injury to other organs is less than 5% of the time. The harm may be obvious at the moment of operation and repaired, or it may not be discovered until a few days later, when additional treatment may be needed.
- There is a less than 35% chance that the surgery cannot be completed safely using this technique, and the doctor will need to perform open operation with a larger incision (cut). This judgment may be made due to bleeding or the surgeon's inability to get an excellent view of the area to be operated on.
How will I Feel after Laparoscopic Colorectal Surgery?
If you are in pain or ill, let your surgeon know. Doctors have tablets/injections on hand that they can administer as needed to keep you comfortable and pain-free.
After the procedure, you may feel dizzy or tired. This is because of the anesthetic, and it could last till the next morning.
After general anesthesia, it is usual to have a painful throat for 2-3 days. This occurs because the anesthetist must insert a catheter into the epiglottis to administer the anesthetic gases that keep you sleeping during the procedure.
To monitor your recovery, the nurses will take your temperature, pulse, and blood pressure at regular intervals. It's critical that we keep track of your progress after your surgery, so be patient with the nurses at this time.
After the surgery, a catheter (tube) will be placed within the bladder to drain pee and allow the nurses to keep monitoring your urine output. When your situation is stable, the tube will be withdrawn, which is normally the next day.
To feed you with fluids and prevent dehydration, a 'drip' will be connected to a small plastic straw (cannula) placed in your arm vein. Doctors usually urge you to eat and drink as soon as possible after your procedure.
Dissolvable stitches, staples, or steri-strips will have been used to close the wound. Before you leave the ward, speak with the nursing staff to see which method was utilized to close the wound. The General practitioner will be able to remove these after the operation, according to the nurses on the ward.
Experts will assist you with getting out of bed and onto a chair the evening following your operation, and possibly walking a short distance. A member of the team will guide you through deep breathing exercises and how to move comfortably without pain. It is critical that you walk around as much as possible to lessen the risk of problems and expedite your recovery.
It is critical that you move around the ward with the assistance of the nurses/physiotherapist the day after the surgery. This will assist you recover more quickly.
When I Can Go Home after Laparoscopic Colorectal Surgery?
You'll be able to return home after you're eating, drinking, and walking around comfortably. It normally takes 4-5 days following laparoscopic colorectal surgery for this to happen.
If your surgery had to be changed to an open procedure, you should be able to return home after about 6-10 days in the hospital.
Please make arrangements for someone to come pick you up in a car on the day of your discharge home, as you will be unable to drive or take public transportation.
It's critical that you make the required arrangements because you'll be expected to drive yourself home unless your doctor believes there are unusual circumstances that necessitate hospital transportation.
To take home with you, staff will provide you with a two-week supply of medication. Any additional drug will require a prescription from your doctor. Please make this appointment before your two-week supply runs out.
Laparoscopic Colorectal Surgery Recovery
Diet
You will eventually be able to continue your regular diet, but you should avoid foods that cause diarrhea or digestive problems right after the operation. Until you are able to eat regularly again, you may want to use a food supplement or drink (such as Ensure).
Constipation can be caused by prescription medications and some pain relievers. If you don't feel like you're back to normal after two weeks, ask your doctor for a stool softener like lactulose or contact your nurse specialist.
Bowel Movement
Bowel function can take a long time to recover to a manageable frequency. Your nurse specialist will talk to you about this because it depends on the type of operation you had and each patient's experience differs.
It's possible that your stools could become loose or that you'll become constipated. If you have loose stools more than four times a day for more than four days, experts recommend taking loperamide, which is available without a prescription from the pharmacy.
Driving
Do not drive until you have had your outpatient clinic visit unless your doctor advises otherwise. You must be able to conduct an emergency stop; thus, your strength and speed of movement must be restored. To guarantee that you are covered in the event of an accident, you must notify the insurance company that you have had surgery.
Exercise
It's usual to feel weak and fatigued right after being released from the hospital. Aim to progressively raise your level of activity. Every day, take a brief stroll, steadily increasing the distance and frequency of your walks.
Approximately 7-8 weeks after returning home, most patients are able to resume normal activities (including sports or exercise).
You should not swim until the wound has healed properly.
For the first six weeks, you should not carry anything heavier than 4 kg, however, this can be gradually raised. Stop lifting anything if it causes you pain or discomfort.
Sexual Activity
Sexual activity can usually be resumed once you've recovered from your surgery and your wound has healed completely.
Contusions around the nerves in the pelvis can sometimes make it difficult for men to get an erection. This is usually only transitory, and the doctor can help you with it.
Some women notice that their vaginal contour is changed and that it is dry. Experiment with different positions and lubricants to see what works best for you. It's natural to be nervous at first, but try to remain patient. If problems persist, speak to a doctor, who will be able to assist and advise you.
Regular Work
Patients who work in light occupations may be able to go to work after three weeks. If your job requires strenuous activity, you’ll got to take 4-6 weeks off.
If you're not sure, talk to your surgeon and your company. Please keep in mind that you may feel quite weary for several weeks after your surgery.
Looking After the Wound at Home
Unless your doctor tells you differently, it is okay to get your wound wet. Unless your doctor instructs you otherwise, do not use antiseptic, bubble bath, or anything else in the bathwater until the wound has healed.
Clean your wound gently with soap and water, then completely rinse it. Using a clean towel, wipe the wound dry.
If sutures were used to close your incision, they will disintegrate after six weeks and you will not need to remove them. Patients frequently see a little white string-like material coming out of their wound. Using a clean pair of scissors, cut and trim this string as close to the skin as feasible.
Staples that were used to seal your incision must be removed. Before you are discharged home, the ward nurse will inform you of this.
Steristrips are thin strips of tape that are sometimes used to keep wounds closed. If they were used in your situation, they can be removed as they begin to pull away from the incision. You should withdraw them yourself in the bath or shower if they are still in place 10 days after your surgery.
Other Things to Know
You may have the impression that your bladder is not emptying entirely after bowel surgery. This normally goes away after 2-3 weeks. If it doesn't, or if you're experiencing a lot of burning when passing urine, contact the doctor because you might have an infection.
Different sensations, such as stinging, itching, or numbing, may be felt in your wound. This is completely normal and a natural component of the healing process.
If you have any of the following symptoms, consult your doctor or a nurse specialist:
- Nausea or vomiting
- Bleeding from the rectum
- Fever or a high temperature
- Increased erythema or pus around the wound
- Pain is getting worse
- Diarrhea is getting worse
Conclusion
The use of minimally invasive techniques in the surgical treatment of colorectal problems is becoming more widespread. Laparoscopy offers obvious benefits and can be performed in the vast majority of patients at surgical facilities with qualified surgeons. In the operating room, hand-assist devices and CO2 colonoscopy are essential equipment. Newer procedures will continue to improve the quality of patient care as technology advances.