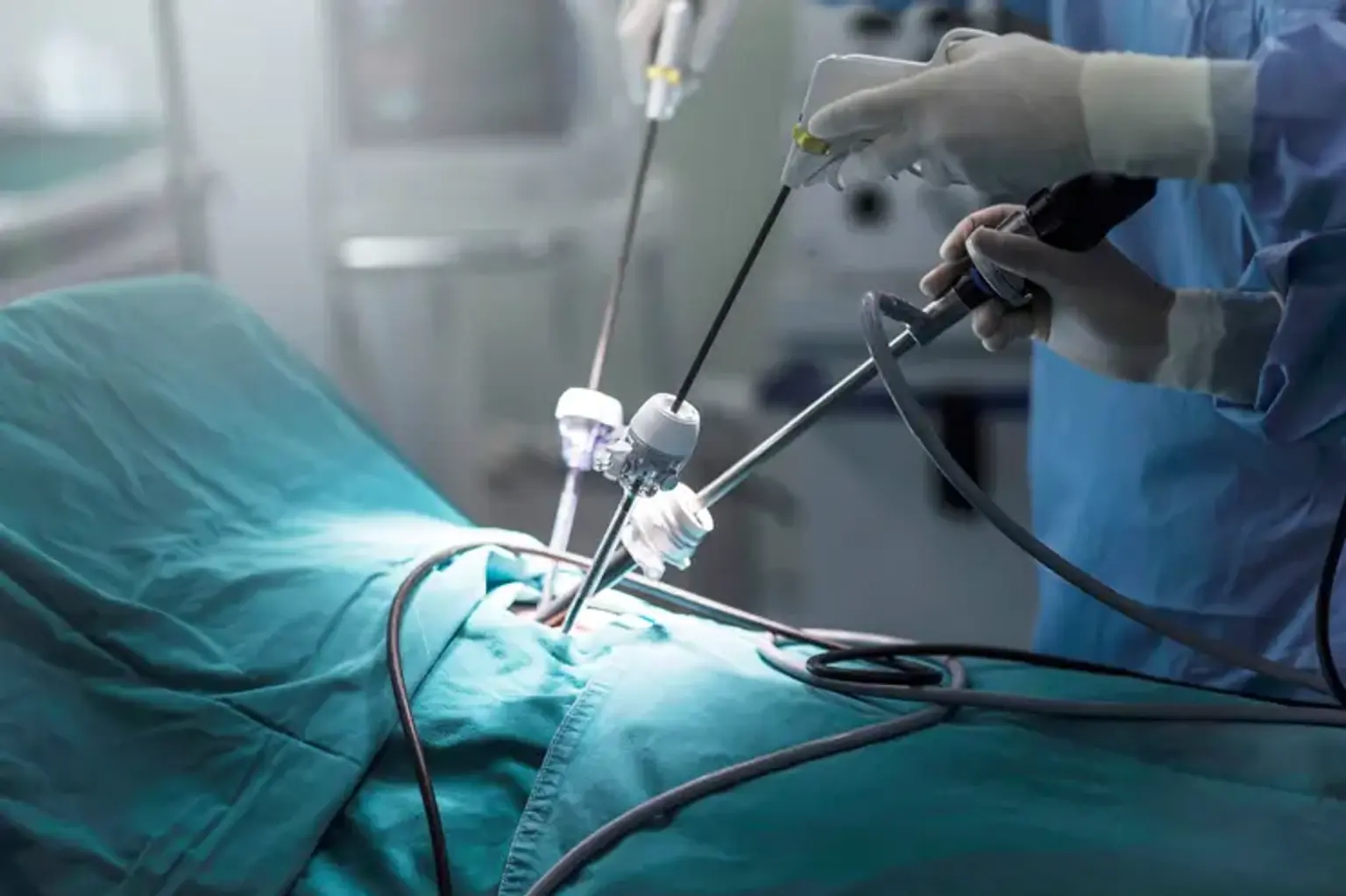
Laparoscopic Solid Organ Surgery
Overview
Laparoscopy is a surgical technique performed to examine the organs in the belly. It can also examine a woman's reproductive organs. Laparoscopy employs a narrow, illuminated tube equipped with a video camera. The tube is known as a laparoscope. It is inserted through a small cut or incision in your abdomen. The images from the video camera may be seen on a computer screen.
Laparoscopy has the advantage of being less intrusive. That is, it makes a very little cut in the stomach. Laparoscopy often takes less time and produces faster results than open surgery. A tiny tissue sample for testing may be obtained by laparoscopy (a biopsy). It can also be used to remove organs such as the appendix (appendectomy) or the gallbladder (cholecystectomy).