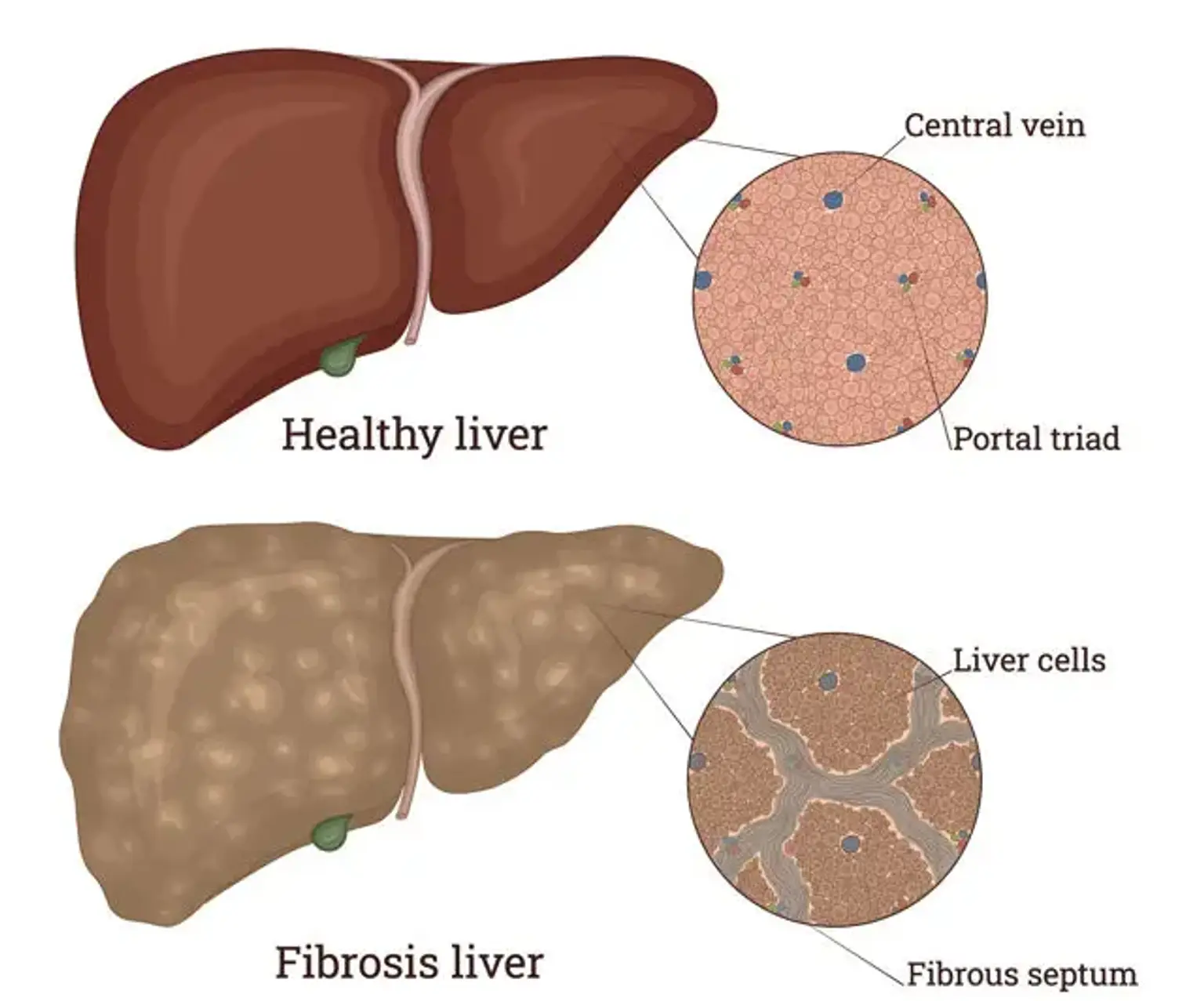
Liver Fibrosis
Liver fibrosis refers to scarring of the liver, one of the largest organs in the body. It is responsible for digestion, energy storage, formation of blood-clotting components, and removal of waste and bacteria, among other things. The liver can also repair injury or damage by regenerating or re-growing itself.
Liver fibrosis develops when scar tissue accumulates in the organ as a result of repeated or long-term damage or inflammation. Compared to healthy liver cells, Scar tissue cells are unable to repair themselves or operate in any other way. Fibrosis can lower the overall function of the liver and impair its ability to regrow as a result of this.
Fibrosis scar tissue can as well obstruct or restrict blood flow within the liver. This could starve and finally destroy the healthy cells, resulting in additional scar tissue.
Signs and Symptoms of Liver Fibrosis
The signs and symptoms of liver fibrosis are rarely noticeable. Hence, the majority of people with fibrosis are normally not aware of their condition. However, when fibrosis advances to cirrhosis, people frequently begin to experience the symptoms.
The signs and symptoms of early cirrhosis might vary; nonetheless, the most prevalent ones include:
- Poor or lack of appetite
- A sensation of weakness
- Fatigue
- Vomiting and nausea
- Unexplainable loss of weight
- Upper right abdominal discomfort or slight soreness
The following are some of the most prevalent symptoms of advanced cirrhosis:
- A proclivity for bruising or easy bleeding
- Fluid retention in the lower legs, foot, or ankles (edema).
- A yellowing of the skin and eyes (jaundice).
- Ascites, a type of stomach bloating caused by a fluid buildup.
- Severe itchiness of the skin
- High sensitivity to drugs and their adverse effects
- Cognitive function problems, including memory, focus, and sleeping problems
- A change in the color of the urine
Causes of Liver Fibrosis
Liver fibrosis is typically a sign of a number of diseases. The following are the most common causes of liver fibrosis;
- Abuse of alcohol: Your liver tends to break down the alcohol you consume so that the body can eliminate it. This procedure generates toxic chemicals that impair liver cells. Therefore, the more alcohol you drink, the more harm you cause.
- Chronic hepatitis C infection: Hepatitis C virus affects the liver and causes inflammation as well as damage. After getting infected, the majority of people do not develop symptoms for years. Due to this, liver issues, particularly fibrosis, are common at the time of diagnosis. Effective treatments are, fortunately, available.
- Nonalcoholic fatty liver disease: This is a condition in which fat accumulates in the liver, causing damage and inflammation and eventually fibrosis. It has nothing to do with alcohol drinking. Instead, it primarily affects those who are obese or have obesity-related diseases, like type 2 diabetes.
Bile duct blockages, inherited metabolic problems, autoimmune conditions, disorders that induce reduced blood supply to the liver, and certain drugs are other possible underlying triggers of liver fibrosis. A type of liver fibrosis present right from birth is known as congenital liver fibrosis.
Risk Factors of Liver Fibrosis
Some of the factors that can contribute to the development of liver fibrosis include;
- Alcohol abuse (excessive consumption)
- Obesity with a disproportionate amount of fat in the belly
- Having some genetic conditions like alpha-1 antitrypsin deficiency, hemochromatosis, or Wilson disease
- Suffering from some medical problems, such as type 2 diabetes and chronic hepatitis C
- Using medications like amiodarone, isoniazid, corticosteroids, methyldopa, and methotrexate
Liver Fibrosis Staging
There are various scales that medical providers use to define liver fibrosis stages. METAVIR is one of the most common liver fibrosis score systems that comprise five stages:
F0: No fibrosis or scarring; despite liver inflammation or hepatitis, there is no evidence of the death of the liver cell (necrosis) and scarring.
F1: Portal fibrosis (mild fibrosis) is characterized by necrosis and scarring in the small and medium portal vein branches that transport blood from the small intestine. Liver structure and function remain normal.
F2: Periportal fibrosis (mild fibrosis) with necrotic foci growing, scarring, and decreased function.
F3: Bridging fibrosis (severe fibrosis). In this liver fibrosis stage 3, scarring has blocked standard blood supply via the liver, compromising the function further.
F4: Cirrhosis, which is characterized by chronic scarring and irreversible liver function loss.
Diagnosis of Liver Fibrosis
If the gastroenterologist suspects liver fibrosis, he or she can order the following diagnostic tests and procedures;
- Biopsy of the liver
Taking a liver biopsy was once thought to be the “gold standard” of diagnosing liver fibrosis. A biopsy is a surgical technique in which a doctor takes a small sample of the liver tissue. The sample is then sent to the lab for further examination by the pathologist to check for scarring or fibrosis.
- Blood tests
The physician can ask for blood tests to look for indicators of liver fibrosis, including high bilirubin levels and some enzymes that signal liver damage. Creatinine levels in the blood are also measured to determine renal function. Hepatitis viruses will be tested as well.
- Imaging tests
The doctor can recommend magnetic resonance elastography (MRE) to diagnose liver fibrosis. The liver hardening or stiffening can be detected using this advanced non-invasive imaging technique. Other types of imaging tests like an MRI, CT scan, or ultrasound can be performed as well.
Liver Fibrosis Treatment
The best strategy for treating liver fibrosis is to treat the underlying cause of the problem. The majority, if not every, damage caused by early to mild liver fibrosis can be reversed if the cause of the fibrosis is successfully treated.
Because each chronic liver illness causes long-term inflammation within the liver, nearly all of them eventually lead to fibrosis. Scar tissue can form as a result of the inflammation, hence fibrosis.
As soon as the doctor determines the cause of liver fibrosis, he or she will recommend a suitable treatment plan. The following are some of the most prevalent treatment options;
- Quitting or limiting consumption of alcohol and utilizing supportive therapies to aid in long-term recovery.
- Using antiviral medicines to treat chronic viral hepatitis infections.
- Addressing nonalcoholic fatty liver disease by balancing the diet, decreasing at least 7 percent of body weight in a year, and managing cholesterol, fat, and sugar levels in the blood.
- Eliminating or dissolving bile duct blockages
- Using drugs that help get rid of heavy metals from the body, including copper and iron
- Ceasing the usage of fibrosis-related drugs
- Taking drugs that suppress the body immune system's activity
Additional treatments are frequently necessary for a person who has progressed liver fibrosis or cirrhosis, while liver damage is usually irreversible. The following are some of the most common therapeutic options for the more advanced condition:
- Taking drugs to help get rid of extra fluid in the body
- Restricting salt consumption
- Taking drugs to get rid of toxins in the brain
- Using drugs to lower the pressure in the stomach and esophageal veins
- Undergoing liver transplant surgery to replace the affected liver with a healthy donor liver
Complications of Liver Fibrosis
Cirrhosis, or chronic scarring of the liver that causes a person to get sick, is the most serious complication associated with liver fibrosis. This usually occurs over a long period, like one or two decades.
A person's liver is necessary for survival because it filters toxic compounds from the blood and performs a variety of other vital functions in the body. If fibrosis advances to cirrhosis or liver failure, a person may experience problems such as:
- Severe accumulation of fluid around the abdomen (ascites)
- Waste products buildup that leads to confusion (hepatic encephalopathy)
- Portal hypertension
- Hepatorenal syndrome
- Variceal bleeding
A person who has a liver disease is likely to die from any of these illnesses if not treated sooner.
Liver Fibrosis Outlook
Addressing the underlying cause or trigger of mild to moderate liver fibrosis can help reverse a portion or all of the damage. Depending on the source and degree of the fibrosis, the liver can repair more slowly or more quickly. Early detection and treatment of fibrosis can considerably increase a person's likelihood of having a full recovery.
While fibrosis is in its early stages, the damage could be localized and reversible. Nevertheless, as the disease progresses, it causes extensive, irreversible damage, which finally results in cirrhosis. More advanced fibrosis and cirrhosis can lead to serious health problems like liver cancer, liver failure, and even death.
Conclusion
Chronic damage or inflammation can result in scar tissue growing up in the liver. This restricts the organ's ability to operate and repair itself, resulting in liver fibrosis. The impacts of mild to moderate fibrosis can typically be reversed with treatment.
The illness, on the other hand, does not usually show symptoms till it has advanced. This causes irreparable damage and can lead to diseases like cirrhosis. As a result, identifying fibrosis at an early stage is critical.
If one has a number of risk factors and suspects they might have liver fibrosis, they need to seek medical advice. Moreover, if you have any indications of severe fibrosis or cirrhosis, consult your doctor immediately.