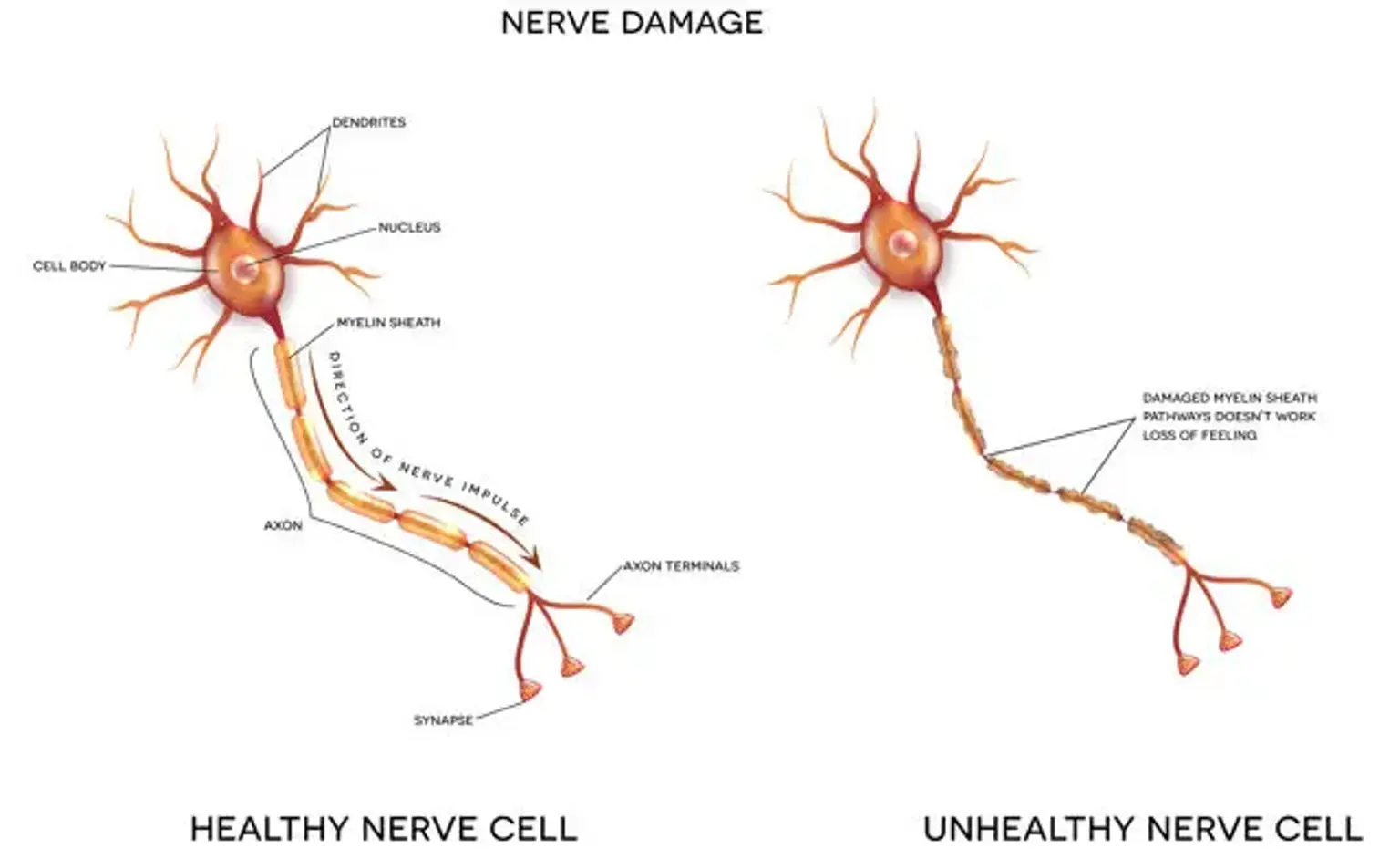
Neuropathy
Neuropathy is a general term that refers to a group of diseases, disorders, and malfunctions of the nerves. An illness, trauma, or injury can damage the nerves in any part of the body. This causes tingling, numbness, pain, and muscle weakness in the area.
These symptoms tend to improve in most cases, especially when the underlying cause is a curable condition. The medical providers can also recommend taking measures to prevent neuropathy or managing it through diet and lifestyle adjustments or medications.
Types of Neuropathy
Neuropathy is classified depending on the types and locations of the affected nerves. The four types of neuropathy include;
- Peripheral neuropathy
Peripheral neuropathy occurs when a nerve disorder affects the nerves located outside the brain and spinal cord. These nerves form part of the peripheral nervous system. On the other hand, peripheral neuropathy is a type of neuropathy that affects the nerves in the extremity, such as the toes, legs, feet, hands, arms, and fingers.
Proximal neuropathy is a term used to describe the nerve injury that causes pain in the shoulders, hips, thighs, and buttocks.
- Cranial neuropathy
Cranial neuropathy develops following an injury or damage in one of the twelve cranial nerves. These are the nerves that directly exit the brain. Optic neuropathy and auditory neuropathy are the two forms of cranial neuropathy.
Optic neuropathy is when the optic nerve, which sends visual signals from the retina towards the brain, is damaged or diseased. Auditory neuropathy affects the nerve that transmits impulses from the inner ear to the brain and plays a significant role in hearing.
- Autonomic neuropathy
Autonomic neuropathy refers to the damage of the involuntary nervous system nerves. These nerves regulate the heart and blood flow (including blood pressure), perspiration, digestion, functions of the bowel and bladder, and sexual response. Other organs' nerves may also be damaged.
- Focal neuropathy
Focal neuropathy is a type of neuropathy that affects only a single nerve, a set of nerves, or only one part of the body. It is a less common type that mostly affects individuals with diabetes.
Signs and Symptoms of Neuropathy
The signs and symptoms of neuropathy can vary based on the type and nerves location. Acute neuropathy is when symptoms arise suddenly, whereas chronic neuropathy is when the symptoms occur progressively with time.
The following are some of the most common neuropathy symptoms and signs:
- Falling and losing one's balance and coordination
- Inability to feel things with the feet and hands (as if you are wearing gloves or socks when you aren't).
- Muscle cramping, twitching, or spasms
- Muscle weakness, trouble walking or moving the legs or arms.
- Paralysis (being unable to move a section of the body). It can include muscle control loss, muscle tone loss, or dropping items in your hand.
- Reduced blood pressure or an irregular heart rhythm might lead to dizziness, fainting, or lightheadedness while standing.
- Sensational shifts, including chronic pain during the night, impaired senses of pain, temperature, pressure, and touch. Touch sensitivity is too high.
- Sharp, stabbing, throbbing, burning, or electric-like pain
- Sweating excessively or insufficiently in accordance with the temperature, degree, or intensity of effort.
- Disorders of the bladder (urination), digestion (bloating, nausea and vomiting), and bowel (diarrhea, constipation).
- Tingling or numbness in the hands and feet. At times, the sensations may extend to the arms and legs.
- Problems with sexual function.
- Loss of weight (unintentional).
Consult the neuropathy doctor near you right away if you experience any of these symptoms.
Causes of neuropathy
Neuropathy refers to nerve damage that occurs due to a variety of disorders. Some of the medical conditions that can contribute to neuropathy are;
- Autoimmune disorders: Sjogren's disease, rheumatoid arthritis, lupus, Guillain-Barre syndrome, vasculitis, and chronic inflammatory demyelinating polyneuropathy are examples of these conditions.
- Diabetes: This is usually the most common reason for neuropathy. More than half of persons with diabetes will develop a certain form of neuropathy.
- Infections: Lyme disease, Epstein-Barr virus, shingles, hepatitis B and C, HIV leprosy, and diphtheria are examples of infections that can damage the nerves.
- Genetic disorders passed down through the generations: Hereditary forms of neuropathy include Charcot-Marie-Tooth disease and others.
- Trauma or injury: Injuries or traumas to the nerves, as well as persistent pressure on a nerve or a set of nerves, are the major causes of neuropathy. Ischemia (low blood flow) on the nerves can also cause long-term harm.
- Tumors: Cancerous and noncancerous tumors of the nerves or surrounding structures can lead to neuropathy by directly getting into the nerves or putting pressure on them.
Other possible causes of neuropathy can include;
- Alcoholism
- Bone marrow diseases
- Certain medications
- Exposure to poisons and toxins
- Vitamin deficiencies
Neuropathy Diagnosis
Your medical provider can recommend the following tests and procedures during neuropathy diagnosis;
Physical exam and medical history: Your doctor will begin by taking a detailed medical history and performing a physical examination. He or she will then examine your symptoms and inquire about your present and previous medications, trauma history, hazardous substance exposure, line of work or social routines (in search for repetitive motions), family history of nervous system diseases, diet, and alcohol consumption.
Neurological examination: Here, your doctor will examine your reflexes, coordination and balance, muscular strength and tone, and the capacity to feel sensations, including cold or light touch.
Blood tests: Your doctor can order blood tests to look for diabetes, vitamin deficiencies, abnormal immunological function, and other signs of diseases that can cause neuropathy.
Imaging tests: The doctor can recommend imaging tests such as CT scan and MRI to check for tumors, herniated disks, compressed or pinched nerves, and other anomalies affecting the bones and blood vessels.
Nerve conduction study: In this test, tiny patches (electrodes) are put on the skin above the nerves and muscles in various areas of your body, mainly the arms and legs. A short electrical pulse is administered to the patch on the nerve being examined. It measures reaction size and the speed with which the nerve transmits the electric signal.
Needle electromyography: By detecting the electric activity in the muscle while in use, an EMG test can show the health of a muscle and determine whether there is a disconnection between the muscle and nerve.
Biopsy: A nerve, muscle, or skin biopsy may be necessary in some cases to verify the diagnosis. A biopsy involves the removal of a small sample of the tissue for assessment under a microscope.
Neuropathy Treatment Options
Neuropathy treatment aims to manage the problem causing neuropathy while alleviating the symptoms. Depending on the type and location of neuropathy, the treatment can include one or a combination of the following options;
- Medications
The neuropathy doctor can prescribe certain medications to help treat the underlying cause of neuropathy and ease the associated symptoms. Examples of these drugs are;
Pain relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) and other over-the-counter pain relievers can help with minor symptoms. Your doctor may also prescribe pain relievers if your symptoms are severe.
Anti-seizure drugs: Nerve pain may be relieved with medications like pregabalin (Lyrica) and gabapentin (Gralise, Neurontin, Horizant) designed to address epilepsy.
Topical treatments: Your doctor can recommend capsaicin cream containing a compound present in hot peppers to help relieve the symptoms of neuropathy. Skin irritation and burning may occur where the cream is applied, although this normally subsides with time.
Antidepressants: Amitriptyline, doxepin (Silenor and Zonalon), and nortriptyline (Pamelor) are tricyclic antidepressants that have been shown to help reduce pain. They work by altering the chemical processes within the brain and spinal cord that generate pain.
- Other treatment procedures and therapies
The following therapies and treatment procedures can also help manage neuropathy and relieve the symptoms;
Transcutaneous electrical nerve stimulation (TENS): This type of treatment includes inserting electrodes on the skin near or on the nerves that cause pain. The electrodes provide a moderate, low-level electric current to the skin. The aim of TENS treatment is to interfere with the pain impulses so that they don’t get to the brain.
Intravenous immune globulin and plasma exchange: People who have certain inflammatory disorders may benefit from these procedures. They aim at suppressing body immune system activity. Plasma exchange is the process of extracting your blood, eliminating antibodies and other proteins from it, and then restoring it to your body. With immune globulin therapy, you get high proteins levels that function as antibodies.
Physical therapy: This is a type of treatment that might help in improving your movements if you have muscle weakness. It can include the use of a cane, hand or foot braces, a walker, or even a wheelchair.
Surgery: Neuropathies caused by nerve pressure, such as tumors, may require a surgical procedure to relieve the pressure.
Conclusion
When the nerve cells, known as neurons, are destroyed or injured, neuropathy develops. The way neurons communicate with each other as well as with the brain is disrupted as a result of this. Neuropathy can affect a single nerve or a type of nerve, a group of nerves in a small location, or various nerves across the body.
The symptoms can range from moderate to disabling and can be fatal in rare cases. Various treatment options such as medications, lifestyle changes, and other therapies can help treat the underlying condition and ease the symptoms.