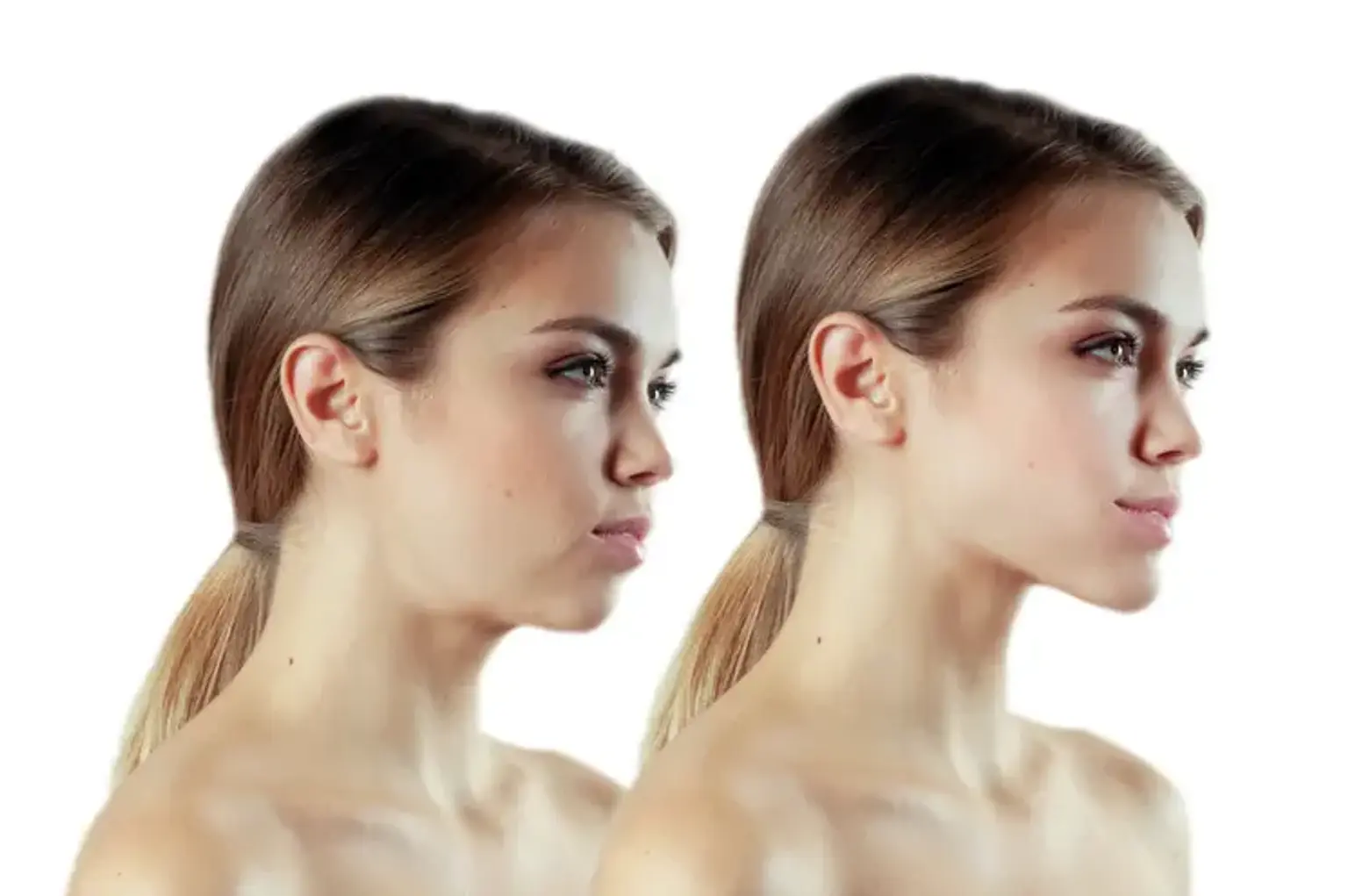Introduction
Jaw Realignment Surgery, also known as Orthognathic Surgery, is a procedure used to correct misaligned jaws, improving both function and appearance. This surgery is often recommended for people with issues such as malocclusion (misaligned bite), facial asymmetry, or problems with speaking, chewing, and breathing. By repositioning the upper and/or lower jaws, orthognathic surgery not only enhances facial aesthetics but also improves oral health and quality of life.
If you're struggling with chronic jaw pain, difficulty eating, or other dental issues, jaw realignment surgery could be the solution you've been looking for. This procedure helps create a balanced, functional bite that leads to improved confidence and comfort.
What is Orthognathic Surgery?
Orthognathic surgery is a surgical procedure designed to realign the upper and lower jaws. When the jawbones are misaligned, it can cause difficulties in biting, chewing, speaking, and even breathing. This misalignment can also impact facial symmetry.
The surgery involves repositioning the jawbones to achieve a more natural and functional bite. It can address several types of bite problems, such as overbites, underbites, crossbites, and open bites. For many patients, orthognathic surgery provides not only improved jaw function but also an enhanced appearance, boosting confidence.
Common Indications for Jaw Realignment Surgery
Jaw realignment surgery is typically recommended for patients who experience significant jaw misalignment, which may cause functional or aesthetic problems. Here are common reasons for considering the surgery:
Malocclusion (Bite Problems): Misalignment of teeth and jaws, such as overbites (upper teeth protrude) or underbites (lower teeth protrude), can cause discomfort and difficulty in biting or chewing.
Facial Asymmetry: When the upper and lower jaws are not in proportion, it can result in an uneven or unbalanced facial appearance.
TMJ Disorders: Jaw misalignment can contribute to temporomandibular joint (TMJ) dysfunction, leading to pain, clicking, or locking of the jaw.
Breathing Issues and Sleep Apnea: In some cases, sleep apnea and other breathing difficulties are linked to jaw misalignment, which can be corrected with surgery.
Orthognathic surgery is ideal for individuals who experience these issues and want a long-term solution that improves both function and appearance.
How Jaw Realignment Surgery Works: The Procedure
The process of jaw realignment surgery begins with a thorough consultation with an oral surgeon and an orthodontist. Imaging tests, such as X-rays and 3D scans, help plan the surgery by providing detailed views of your jaw structure.
Step-by-Step Overview of the Procedure:
Pre-Surgery Preparation: Before the surgery, patients usually wear braces for several months to align the teeth and prepare the jaw for realignment. The orthodontist will work with the surgeon to plan the procedure.
Surgical Process: During the surgery, the surgeon makes small incisions inside the mouth to access the jawbones. The upper and/or lower jaws are then repositioned and secured with plates, screws, or wires. This step improves both the bite and facial symmetry.
Post-Surgery Care: After the surgery, patients may need to follow a soft-food diet and avoid strenuous activities during recovery. Swelling and bruising are common, but these usually subside within a few weeks. Follow-up visits with the surgeon and orthodontist are essential to ensure proper healing.
Orthognathic surgery may require several months of post-surgical care, including continued orthodontic treatment to perfect the bite and ensure lasting results.
Benefits of Orthognathic Surgery
Orthognathic surgery offers both functional and cosmetic benefits, significantly improving a patient’s quality of life. For those suffering from jaw misalignment, the surgery can alleviate many daily challenges.
Improved Bite and Function: One of the most significant benefits of jaw realignment surgery is the correction of bite problems, such as overbite or underbite. A proper bite makes it easier to chew, speak, and breathe comfortably, often eliminating the need for compensatory behaviors like chewing on one side of the mouth.
Facial Aesthetics: Many patients experience a noticeable improvement in facial symmetry and profile after surgery. This is especially beneficial for individuals whose jaw misalignment has caused facial asymmetry, giving them a more balanced and attractive appearance.
Improved Confidence: By addressing both functional and aesthetic concerns, orthognathic surgery boosts self-esteem. Many patients report feeling more confident in social and professional situations after their surgery.
Real-life examples often highlight the transformation, with patients not only improving their bite and speech but also experiencing an increase in their overall sense of well-being.
Pre-Surgical Assessment and Planning
Before undergoing orthognathic surgery, a thorough evaluation is essential to ensure the procedure is right for you. The pre-surgical assessment involves collaboration between the oral surgeon, orthodontist, and possibly other specialists.
Initial Consultation: This involves a detailed discussion about your medical history, symptoms, and goals for surgery. The surgeon will assess the degree of misalignment and its impact on your jaw and facial features.
Imaging and Diagnostic Tests: X-rays, 3D scans, and dental impressions are used to get a clear view of your jaw structure. These images help to plan the precise movements of the jawbones during surgery.
Orthodontic Preparation: In many cases, braces are worn for several months or even years leading up to surgery. This allows the teeth to be aligned in a way that supports the correct position of the jaws post-surgery. Orthodontic treatment usually continues after surgery as well.
Having a well-coordinated team and proper preparation increases the likelihood of a successful outcome.
Risks and Complications
While orthognathic surgery is generally safe and effective, it’s important to be aware of the potential risks and complications. Understanding these will help you make an informed decision and be better prepared for the recovery process.
Infection: As with any surgery, there’s a risk of infection. Your surgeon will take precautions, such as prescribing antibiotics and ensuring sterile conditions, to minimize this risk.
Nerve Damage: In rare cases, the surgery may cause temporary or permanent nerve damage, leading to numbness or tingling in the lips, chin, or cheeks. This can usually be managed, but it’s important to discuss any concerns with your surgeon.
Jaw Relapse: Occasionally, the jaw may shift back toward its original position after surgery, requiring additional orthodontic treatment or even a second surgery to correct it.
Discomfort and Swelling: Post-surgical swelling and discomfort are normal and can last several weeks. It’s essential to follow post-operative care instructions to minimize these effects.
Most patients experience significant relief and positive outcomes, but it's important to discuss any risks with your surgeon before proceeding.
Recovery After Jaw Realignment Surgery
The recovery process after jaw realignment surgery can vary depending on the complexity of the procedure, but most patients can expect a gradual return to normal activities within a few months.
Immediate Post-Surgery: After the surgery, you will likely spend a few days in the hospital for observation. Your jaw may be bandaged, and you’ll need to follow a soft-food diet for several weeks. Swelling and bruising are common during the first few weeks.
Pain Management: Mild pain and discomfort are common after surgery, but pain medications prescribed by your surgeon can help manage this. Ice packs may also help reduce swelling.
Follow-Up Visits: You will need to attend follow-up appointments with your surgeon and orthodontist to monitor your recovery and ensure proper healing. Braces will likely remain on your teeth for some time after surgery to refine your bite.
Returning to Normal Activities: Most patients can return to school or work after about 2 to 4 weeks, but you should avoid strenuous physical activities for several months to allow for proper healing.
The recovery process requires patience, but most people experience a positive transformation and a significant improvement in their jaw function and appearance after healing.
Orthognathic Surgery and Facial Aesthetics
One of the most noticeable outcomes of jaw realignment surgery is the improvement in facial aesthetics. When the upper and lower jaws are misaligned, it can lead to an uneven or unbalanced appearance, affecting facial features such as the profile, chin, and jawline. By realigning the jaws, this surgery can restore facial harmony and improve the overall look of the face.
Symmetry and Proportions: Patients often report significant changes in facial symmetry, with a more proportionate appearance. For instance, those with recessed jaws may notice a more prominent chin, while those with an overly prominent jaw may experience a more balanced profile.
Confidence Boost: Many individuals experience a renewed sense of confidence following the surgery. The improved facial aesthetics can lead to enhanced self-esteem, as individuals feel better about their appearance in both personal and professional settings.
While the results are often dramatic, it’s important for patients to have realistic expectations. The changes are meant to enhance natural beauty, not completely transform facial features.
Jaw Surgery and Speech Improvement
Jaw misalignment can have a direct impact on speech, leading to issues like difficulty pronouncing certain words or sounds. In cases of severe overbite or underbite, patients may even struggle to speak clearly or comfortably. Fortunately, orthognathic surgery can provide significant improvements in speech.
Clearer Speech: By repositioning the jawbones, the surgery can correct the anatomical issues that make speaking difficult. For example, a person with an underbite might find it hard to form certain words, but once the jaw is realigned, speaking becomes easier and more natural.
Enhanced Communication: Many patients report feeling more confident in social situations after the surgery because they can speak more clearly, reducing frustration and embarrassment.
Speech therapy may also be recommended post-surgery to further enhance speech clarity and ensure optimal results.
Impact on Breathing and Snoring
Orthognathic surgery is not only a solution for cosmetic and functional jaw issues but can also help alleviate breathing problems, including sleep apnea and chronic snoring. For individuals with severe jaw misalignment, the airway may be obstructed, leading to difficulty breathing during sleep and poor-quality rest.
Improved Airway Function: By realigning the jaw, the surgery can open up the airway, improving airflow during sleep. This can significantly reduce or eliminate snoring and help people who suffer from sleep apnea breathe more easily throughout the night.
Better Sleep Quality: Correcting jaw misalignment often leads to improved sleep patterns, reducing the risks associated with sleep apnea, such as fatigue, high blood pressure, and cardiovascular problems. Patients frequently report feeling more rested and alert after recovery.
For those with breathing difficulties linked to jaw issues, this surgery can provide relief and lead to a better overall quality of life.
Global Popularity of Orthognathic Surgery
Over the years, orthognathic surgery has gained popularity worldwide as a solution to correct jaw misalignment and enhance both function and aesthetics. The surgery is widely performed in various countries, with its prevalence growing in regions such as North America, Europe, and Asia.
Growing Demand: As more people seek solutions for jaw issues that affect daily life—like difficulty eating, speaking, and breathing—the demand for jaw realignment surgery continues to rise. Advances in surgical techniques, better recovery protocols, and improved technology have made the procedure safer and more effective than ever.
Global Trends: In some countries, especially in Asia, jaw surgery is also sought after for purely cosmetic reasons, with many individuals choosing the procedure to improve their facial appearance and profile. In the U.S. and Europe, the focus is often on correcting functional issues such as bite problems and sleep apnea.
Affordability and Access: The availability of orthognathic surgery has also increased due to better access to healthcare services in many countries. Some regions offer more affordable options, making the surgery accessible to a broader population.
The growing popularity of this surgery reflects its ability to address a range of concerns, from functional issues to aesthetic enhancements, making it a sought-after procedure worldwide.
Before and After: Realistic Expectations
Before undergoing jaw realignment surgery (orthognathic surgery), it’s important for patients to understand both the process and the potential results. The procedure is transformative, but results vary depending on individual needs. Patients who seek this surgery often have concerns about the dramatic changes it can make to their facial appearance. While these changes can enhance both function and aesthetics, they can also be overwhelming initially. That’s why managing expectations is key. It’s helpful to consult with a qualified surgeon who will take precise measurements and offer insights into the improvements that can be made based on your unique case.
After surgery, you can expect noticeable changes not just in your appearance, but in how your jaw functions. For those who have struggled with misalignments like an overbite, underbite, or crossbite, orthognathic surgery can restore a natural, balanced bite. However, it’s important to remember that the final outcome might not be immediate. Swelling can last for several weeks, and the bone adjustments take time to heal fully. For the best results, be prepared for a recovery period, which may include eating soft foods, practicing oral hygiene carefully, and attending follow-up appointments to ensure proper healing.
How to Choose the Right Surgeon
Choosing the right surgeon for jaw realignment surgery is one of the most critical decisions in the entire process. This procedure is highly specialized, and selecting a qualified surgeon with experience in orthognathic surgery can significantly impact your outcomes. When searching for a surgeon, look for someone who is board-certified in oral and maxillofacial surgery. It’s also essential that the surgeon has experience with the specific procedure you require, as well as a history of successful outcomes with jaw realignment.
Before committing, schedule a consultation to discuss your concerns and goals. During this meeting, a surgeon should provide a thorough evaluation of your jaw alignment and explain the surgical options best suited to your needs. Ask for before-and-after photos of previous patients, read reviews from former patients, and inquire about their specific training and experience with complex jaw surgeries. Don’t be afraid to get a second opinion or seek referrals from trusted sources, such as other medical professionals or patient advocacy groups. The more informed you are, the better you can feel about your decision.
The Cost of Jaw Realignment Surgery
The cost of jaw realignment surgery can vary widely depending on a variety of factors. On average, the procedure can cost between $20,000 and $40,000, including pre-surgical evaluations, hospital or surgical center fees, surgeon’s fees, anesthesia, and follow-up care. However, the final cost will depend on the complexity of the surgery, geographical location, and whether additional treatments, such as dental work or orthodontic care, are required before or after the surgery.
In terms of insurance, some health insurance plans may cover jaw realignment surgery if it is deemed medically necessary. This could include cases where the surgery is needed to correct a functional issue like severe malocclusion or TMJ disorder that affects your ability to eat, speak, or breathe properly. It’s important to check with your insurance provider to confirm what is covered under your plan. If the surgery is purely cosmetic, it may not be covered. Many patients choose to finance the procedure through payment plans or medical loans if necessary. Be sure to factor in any additional costs for post-surgical care, such as physical therapy, medication, and follow-up visits.
Jaw Realignment Surgery for Functional Issues
Jaw realignment surgery isn’t just for cosmetic improvements — it’s also highly effective for treating functional issues. Many patients seek orthognathic surgery to correct problems with their bite, such as an overbite, underbite, or misaligned jaw that can cause difficulties in chewing, speaking, or breathing. For those with temporomandibular joint (TMJ) disorders or obstructive sleep apnea, jaw surgery can offer significant relief by improving jaw position and reducing stress on the jaw joints.
By realigning the jaw, the procedure helps restore proper function, allowing patients to experience better comfort in everyday activities like eating and speaking. For individuals with severe malocclusion or jaw pain, orthognathic surgery can be life-changing, improving not only their physical health but also their quality of life.
Global Popularity and Demand
Jaw realignment surgery has gained significant popularity worldwide, as people seek solutions for both functional and aesthetic concerns. In regions like North America, Europe, and Asia, more individuals are choosing orthognathic surgery to address issues like misaligned bites, jaw pain, and facial appearance. This increase in demand is partly due to advancements in surgical techniques, which have made the procedure safer and more effective.
The rise of social media and an increased focus on self-image has also contributed to the global appeal of jaw surgery, as people become more aware of how it can improve not just oral health, but facial aesthetics as well. Whether for functional reasons or to enhance facial balance, more patients are opting for this transformative procedure, recognizing its value in achieving both health and beauty goals.
The Cost of Jaw Realignment Surgery
The cost of jaw realignment surgery can vary, but it typically ranges from $20,000 to $40,000, depending on factors like location, complexity, and additional treatments required. This price usually includes the surgeon’s fees, anesthesia, hospital stay, and follow-up appointments. However, the total cost can be higher if the surgery involves orthodontic treatment before or after the procedure.
In some cases, insurance may cover the surgery if it’s deemed medically necessary, especially for conditions like severe malocclusion or TMJ disorder. If the surgery is purely for cosmetic reasons, insurance is less likely to provide coverage. Many patients also explore financing options to help manage costs. It's important to fully understand the financial aspects before proceeding with surgery.
Conclusion
Jaw realignment surgery offers significant benefits for those struggling with misalignments or functional issues such as pain or difficulty chewing. Whether you're seeking improved facial aesthetics or relief from jaw pain, orthognathic surgery can enhance both your quality of life and self-esteem. However, it's crucial to set realistic expectations about the results and recovery process.
If you're considering this surgery, speak with an experienced oral and maxillofacial surgeon to evaluate your needs and determine the best treatment plan. With proper care and preparation, jaw realignment surgery can provide lasting benefits and a healthier, more confident smile.