Introduction
What is Osgood-Schlatter Disease?
Osgood-Schlatter Disease (OSD) is a common cause of knee pain in growing children and adolescents, particularly those who are involved in sports or high-impact activities. It is characterized by inflammation of the growth plate at the tibial tuberosity, which is the bony prominence located just below the kneecap. While it may sound alarming, OSD is typically temporary and resolves once the child finishes their growth spurt.
Symptoms of OSD include pain, swelling, and tenderness just below the knee, which can worsen with physical activity. The pain is often aggravated by sports that involve running, jumping, or rapid directional changes. Although it’s most common in children between 10 and 15 years of age, it can also affect younger children and adults, especially those who have a history of high activity levels during childhood.
Anatomy of the Knee and Growth Plate
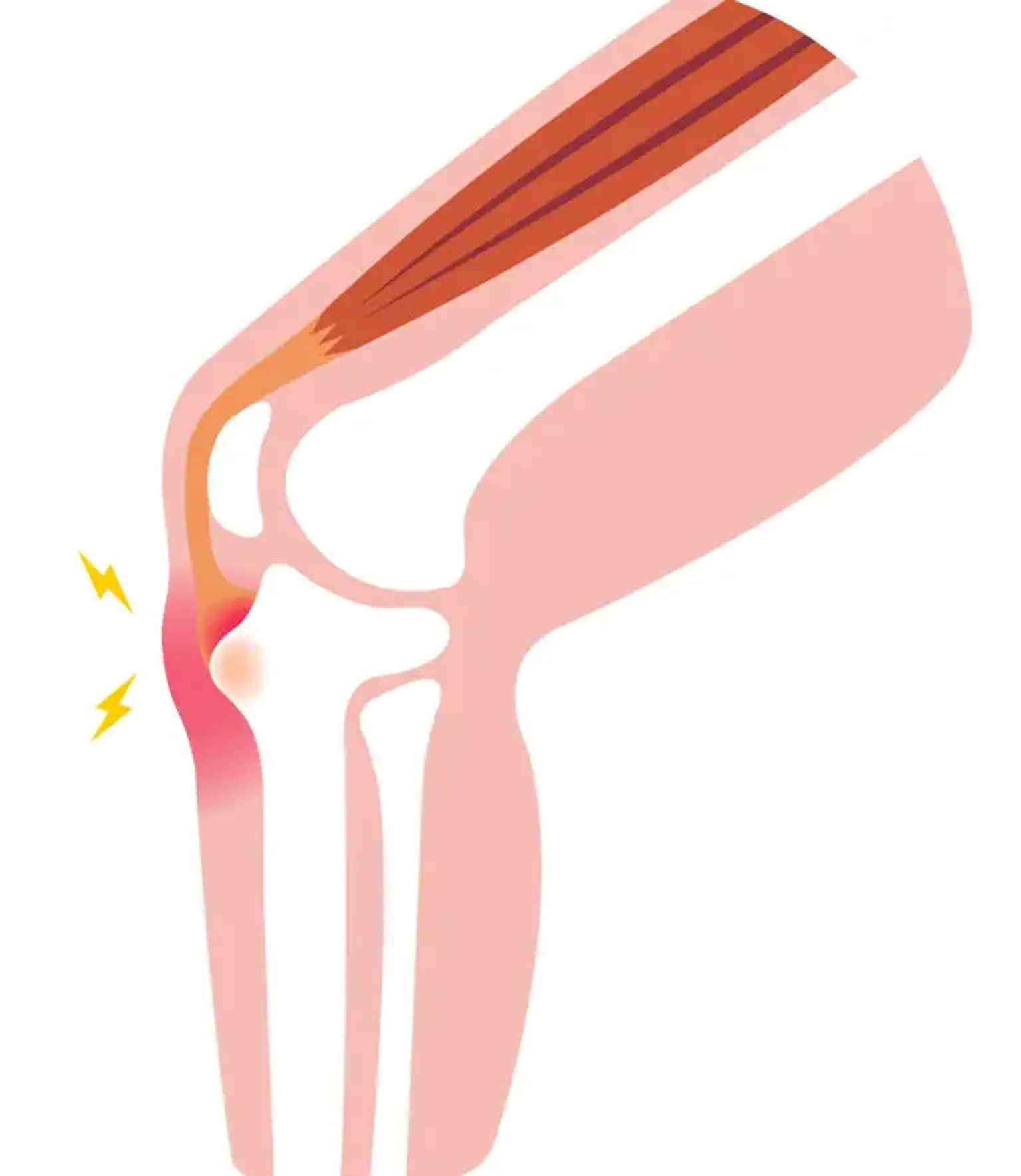
To understand Osgood-Schlatter Disease, it’s important to first look at the anatomy of the knee. The tibial tuberosity is a bony structure located at the top of the shinbone (tibia), just below the kneecap (patella). It is where the patellar tendon attaches, connecting the quadriceps (front thigh muscles) to the tibia.
During growth spurts, the bones, muscles, and tendons are developing rapidly. This growth puts increased tension on the patellar tendon, which can cause inflammation or even micro-tears at the tibial tuberosity. This is what leads to the pain and swelling characteristic of OSD. Since the condition involves the growth plate, it is more common in children and adolescents whose bones are still growing, making it a self-limiting condition in most cases.
Causes and Risk Factors of Osgood-Schlatter Disease
Growth Spurts in Adolescents
Osgood-Schlatter disease is closely linked to the rapid growth that occurs during puberty. As children enter their growth spurt, their bones grow faster than their muscles and tendons, which can cause an imbalance in the body. This results in increased tension on the patellar tendon, especially at the site where it attaches to the tibial tuberosity.
During this phase, children may be more susceptible to overuse injuries. The rapid bone growth can leave the tendon under strain, leading to irritation and inflammation at the attachment site. As such, children experiencing growth spurts are at the highest risk of developing OSD, which generally resolves once the growth plates close and the child reaches physical maturity.
Repetitive Stress from Physical Activity
Athletes, especially those who participate in high-impact sports like soccer, basketball, football, and running, are more likely to develop OSD. These activities involve repetitive stress on the knee joint, particularly the tendons, which can cause irritation at the tibial tuberosity. In fact, OSD is often referred to as an overuse injury.
Children and adolescents who engage in frequent jumping, running, or squatting movements are putting additional strain on their knees, making the condition more likely to develop. The more intense the activity and the higher the frequency, the greater the risk of OSD. This is why OSD is particularly common in young athletes who may not have yet developed proper techniques for protecting their joints.
Genetic Factors
Though not a primary cause, genetics can play a role in the development of Osgood-Schlatter disease. Studies suggest that children who have a family history of knee problems or OSD are at an increased risk of developing the condition themselves. Additionally, gender plays a role: OSD is more common in boys, though it can also affect girls, particularly those involved in athletic activities.
Diagnosing Osgood-Schlatter Disease
Clinical Diagnosis
The diagnosis of Osgood-Schlatter disease typically starts with a physical examination. A healthcare provider will look for the characteristic signs of the condition: swelling and tenderness just below the knee, especially at the tibial tuberosity. The pain may worsen when pressure is applied to the area or when the child performs activities like squatting, running, or jumping.
During the exam, the doctor may also assess the child's range of motion and knee stability to rule out other possible knee injuries. Since OSD is often associated with pain related to specific activities, your healthcare provider will likely inquire about the child's athletic activities and how the pain correlates with them.
Imaging Tests
While a physical exam is often enough to diagnose OSD, your doctor may order imaging tests to confirm the condition or rule out other possible causes of knee pain, such as fractures, infections, or tumors. An X-ray is typically the first imaging test performed, as it can reveal any abnormal bone growth or bone spurs at the tibial tuberosity.
In some cases, an MRI (magnetic resonance imaging) may be necessary if the diagnosis is unclear or if there are concerns about more severe injuries. MRIs provide detailed images of soft tissues like tendons and ligaments, which can help identify any associated damage to the patellar tendon or surrounding structures.
Differentiating from Other Knee Conditions
It’s essential to distinguish Osgood-Schlatter disease from other knee conditions that can cause similar symptoms, such as patellar tendonitis, jumper's knee, or even infections. A healthcare provider will consider the patient’s age, activity level, and the pattern of knee pain to determine whether OSD or another condition is causing the symptoms.
Treatment Options for Osgood-Schlatter Disease
Non-Surgical Treatments
In most cases, Osgood-Schlatter disease can be managed without surgery. The first line of treatment involves rest and activity modification. Reducing or temporarily stopping activities that cause knee pain, such as running, jumping, or sports, is essential to allow the knee to heal.
Ice therapy is another effective way to manage swelling and pain. Applying an ice pack to the knee for 15-20 minutes several times a day can help reduce inflammation. Additionally, over-the-counter pain relievers like ibuprofen or acetaminophen can alleviate pain and inflammation, especially in the initial stages of the condition.
Physical Therapy for Osgood-Schlatter Disease
Physical therapy plays a key role in the treatment of Osgood-Schlatter disease, focusing on improving flexibility, strength, and overall function of the knee. Stretching exercises that target the quadriceps, hamstrings, and calves are essential for reducing tension on the patellar tendon. Tight muscles can exacerbate the pain and discomfort associated with OSD.
Strengthening exercises for the muscles around the knee, especially the quadriceps and hamstrings, are also beneficial. These exercises help stabilize the knee joint and reduce strain on the tibial tuberosity. A physical therapist can design a program that is appropriate for the child’s age, activity level, and degree of pain.
Bracing and Support
In some cases, wearing a knee brace or sleeve can provide additional support and reduce the strain on the tibial tuberosity. These braces can also help stabilize the knee during physical activities and prevent further irritation. Bracing is particularly helpful for athletes who are transitioning back to sports or physical activity after a period of rest.
Management through Activity Modifications
It’s essential to modify the child’s activity level to prevent further strain on the knee. Instead of high-impact sports, children with OSD should engage in low-impact activities such as swimming or cycling, which do not place as much stress on the knee. As the condition improves, a gradual return to sports can be achieved by ensuring the child maintains proper technique and incorporates appropriate warm-up and cool-down routines.
Advanced Treatment Options
Corticosteroid Injections
In rare cases, when conservative treatments such as rest, ice, and physical therapy do not provide sufficient relief, corticosteroid injections may be considered as an option for managing inflammation. These injections can help reduce swelling and provide short-term relief from pain. However, they are generally not the first-line treatment for Osgood-Schlatter disease, as their effectiveness may diminish over time and they do not address the underlying cause of the condition.
Corticosteroid injections are typically used in cases where the inflammation is severe and persistent. However, they are more commonly used in conditions that involve long-term inflammation, such as arthritis, rather than for OSD. It’s important to discuss the potential risks and benefits of this treatment with a healthcare provider, as excessive use of steroids may lead to potential side effects, including tendon weakening.
Surgical Treatment for Severe Cases
Surgery is rarely needed for Osgood-Schlatter disease. The condition is typically self-limiting, meaning it resolves on its own once the growth plates close and the child reaches adulthood. However, in a small percentage of cases, surgery may be necessary if conservative treatments fail and the symptoms persist for an extended period.
Surgical intervention may be required when a bone spur at the tibial tuberosity causes persistent pain that interferes with everyday activities, or if there is significant damage to the patellar tendon. The most common surgical procedure involves the removal of the bone spur or excess bone at the tibial tuberosity. In some cases, tendon repair may be required if the tendon has been severely damaged.
Surgical treatment is typically considered only after all other non-invasive methods have been exhausted, and when the child’s bones have stopped growing. Post-surgery, physical therapy is crucial for recovery, focusing on restoring strength and flexibility to the knee joint.
Recovery and Rehabilitation Post-Surgery
Recovery time after surgery can vary, but most children can expect a gradual return to activity within a few months. A structured rehabilitation plan, including physical therapy, is essential to ensure proper healing and regain knee strength and flexibility. The child may need to avoid high-impact activities for several months after surgery and should only return to sports once the knee has fully healed.
Rehabilitation focuses on strengthening the muscles around the knee to prevent future injuries and improve overall knee function. Regular follow-up with the healthcare provider is important to monitor the healing process and ensure the child is progressing well.
Recovery Timeline and Prognosis
Expected Recovery Time for Osgood-Schlatter Disease
The recovery timeline for Osgood-Schlatter disease can vary from child to child, depending on the severity of the condition and the effectiveness of treatment. In most cases, OSD improves within 6 to 12 months with appropriate management. Since the condition is related to growth spurts, it tends to resolve on its own once the bones have stopped growing, typically around age 16 to 18.
For children undergoing physical therapy and following conservative treatment protocols, the pain should gradually subside as the knee heals. However, some children may experience residual symptoms or discomfort during high-impact activities until they fully mature. Once the growth plates close and the child reaches skeletal maturity, the pain and swelling typically disappear.
Long-Term Outlook
One of the most reassuring aspects of Osgood-Schlatter disease is that, in the vast majority of cases, it does not cause long-term knee problems. After the growth plates close, the pain usually resolves completely, and most individuals experience full recovery with no lasting knee issues. Once healed, there is no permanent damage to the knee joint or the patellar tendon.
However, in rare cases, if OSD is left untreated or the child continues to engage in high-stress activities without addressing the condition, there may be an increased risk of chronic knee pain, inflammation, or development of osteoarthritis later in life. Therefore, it’s essential to address the symptoms early and follow a proper treatment plan to avoid long-term complications.
Preventing Recurrence
While Osgood-Schlatter disease typically resolves on its own, recurrence of symptoms is possible, especially if the child returns to high-impact sports too soon or does not follow recommended rehabilitation practices. To prevent recurrence, it is essential to:
Maintain Strength and Flexibility: Regular physical therapy can help ensure the muscles around the knee remain strong and flexible, reducing strain on the patellar tendon.
Gradual Return to Activity: Children should ease back into sports and physical activities with proper warm-ups, stretching, and avoiding high-impact movements until the knee is fully healed.
Use Supportive Gear: In some cases, wearing knee braces or sleeves during physical activity can provide additional support and help prevent further irritation to the tibial tuberosity.
FAQs About Osgood-Schlatter Disease Treatment
Can Osgood-Schlatter Disease Cause Permanent Damage?
One of the most common concerns about Osgood-Schlatter disease is whether it can lead to permanent knee damage. The good news is that, for the vast majority of children, OSD does not cause permanent damage. Once the growth plates close and the child reaches full skeletal maturity, the condition resolves. However, in rare cases where the condition is left untreated or not managed properly, there could be long-term knee problems, such as chronic pain or joint instability.
The key to preventing lasting damage is early intervention and adherence to a treatment plan. With appropriate care, including rest, physical therapy, and activity modifications, most children experience a complete recovery without any lasting issues.
How Common is Osgood-Schlatter Disease?
Osgood-Schlatter disease is quite common among active children and adolescents, especially those involved in sports. It is estimated that between 10% to 20% of children involved in sports experience symptoms of OSD. The condition is most frequently seen in children between the ages of 10 and 15, with boys being more commonly affected than girls.
It is particularly prevalent among those who participate in high-impact activities, such as soccer, basketball, and running. Due to the growth spurt associated with the condition, OSD is often seen during periods of rapid physical development, which typically occurs between ages 12 and 14 in boys and between ages 10 and 12 in girls.
When Should I Consider Surgery for Osgood-Schlatter Disease?
Surgery for Osgood-Schlatter disease is generally reserved for severe or persistent cases that do not improve with conservative treatments. Indications for surgery include:
Chronic, severe pain that interferes with daily activities.
Bone spurs or excess bone growth that cause persistent irritation or discomfort.
Damage to the patellar tendon or other knee structures.
Surgical intervention is usually considered once the child’s growth plates have closed and after all non-surgical options have been exhausted. It’s important to consult with a healthcare provider to determine if surgery is the right choice.
How Can I Manage Pain at Home?
Managing pain from Osgood-Schlatter disease at home is possible with several simple strategies:
Rest: Avoid activities that aggravate the knee pain, such as running or jumping.
Ice: Apply an ice pack to the knee for 15-20 minutes several times a day to reduce inflammation.
Pain Relievers: Over-the-counter pain medications like ibuprofen or acetaminophen can help manage discomfort and inflammation.
Stretching and Strengthening: Incorporating gentle stretching and strengthening exercises into the routine can prevent muscle tightness and reduce stress on the knee.
By adhering to these recommendations, most children and adolescents can find relief from pain and promote healing of the knee.
Conclusion
Final Thoughts on Osgood-Schlatter Treatment
Osgood-Schlatter disease is a common and treatable condition that affects many active adolescents. While it can cause discomfort and pain, it is typically a self-limiting condition that resolves once the child has finished their growth spurt. With appropriate treatment, including rest, physical therapy, and in some cases, surgical intervention, children can recover fully and return to their favorite activities without long-term knee problems.
Seeking Professional Help
It’s important for parents and caregivers to seek medical advice if they suspect their child may have Osgood-Schlatter disease. Early diagnosis and intervention can help manage symptoms effectively and prevent future complications. A healthcare provider can recommend the best course of treatment, whether it’s rest, physical therapy, or, in rare cases, surgery. With proper care, most children experience a complete recovery and resume their normal activities with little to no lasting effects.