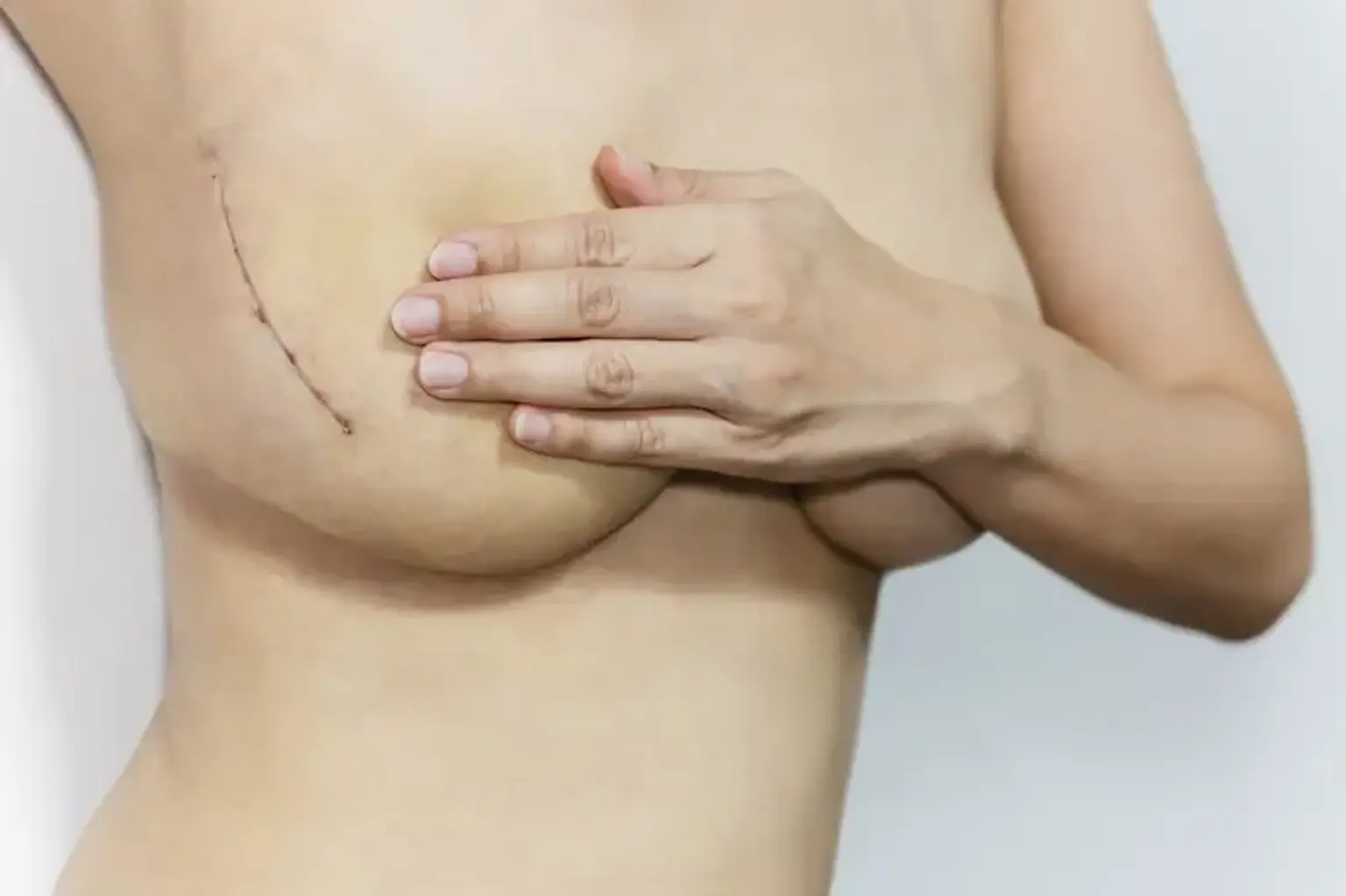
Partial Mastectomy
Overview
As the surgical management of breast cancer evolves, the medical community is providing the most up-to-date techniques, such as breast-conserving strategies such as partial mastectomy, as well as skin- and nipple-sparing approaches. A partial mastectomy is another name for a lumpectomy, which is a breast-conserving surgery that removes only the cancerous portion of the breast and a small rim around it to help prevent recurrence.