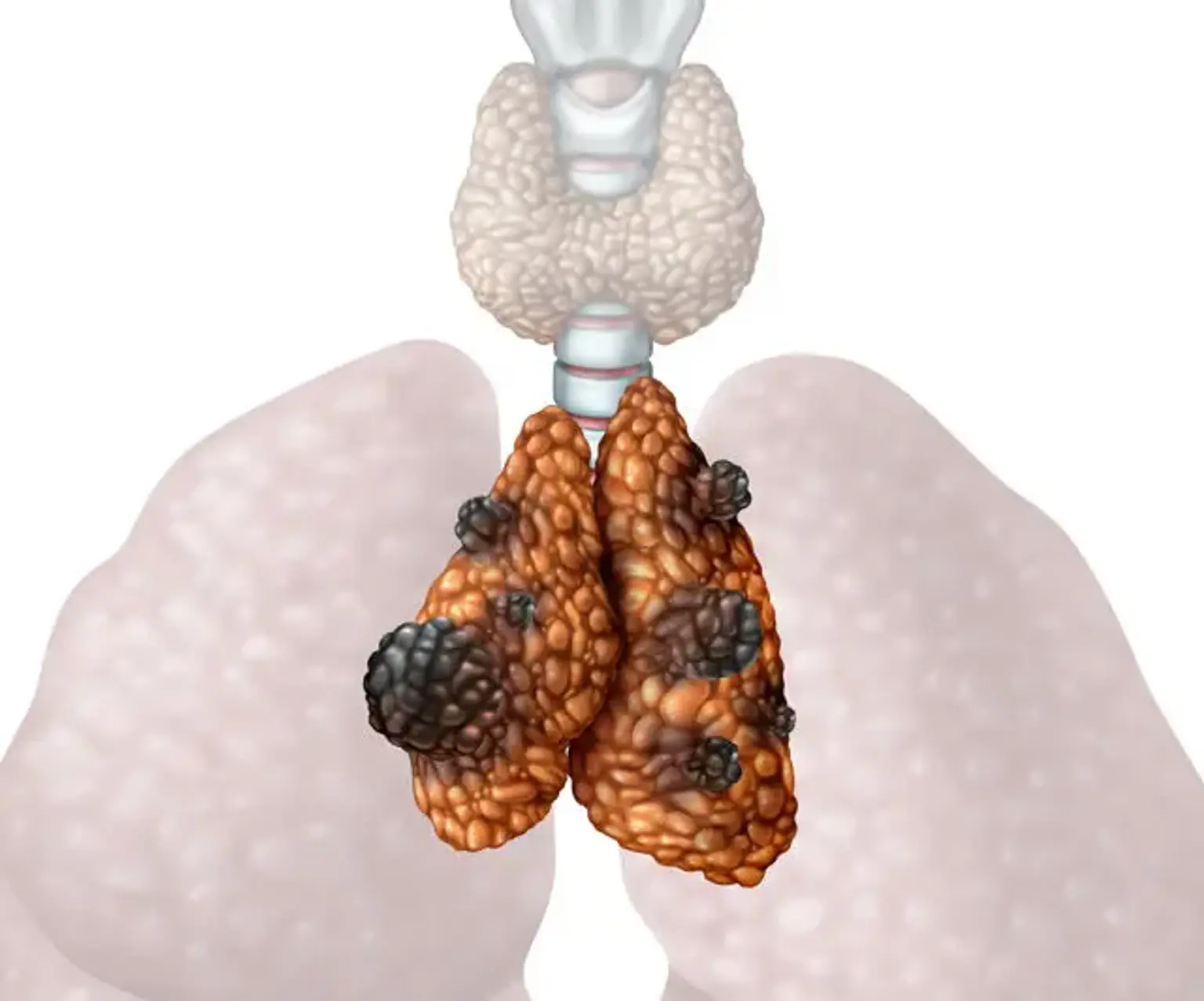
Pediatric thoracic tumor
Pediatric thoracic tumor is either malignant or benign tumors that occur and affect the chest cavity in children. Most forms of malignant or cancerous tumors include the thymus and can be categorized as thymic carcinomas or thymoma. However, various types of thymomas are non-cancerous or benign, although other thoracic tumors exhibit a certain degree of malignancy possibility.
The chest cavity is typically made up of the heart, thymus gland, trachea or windpipe, large blood vessels, and connective tissue of the lungs. The chest wall masses that develop among infants and children can be secondary tumors. Moreover, they can also be a result of other various cancers that have advanced and metastasize.