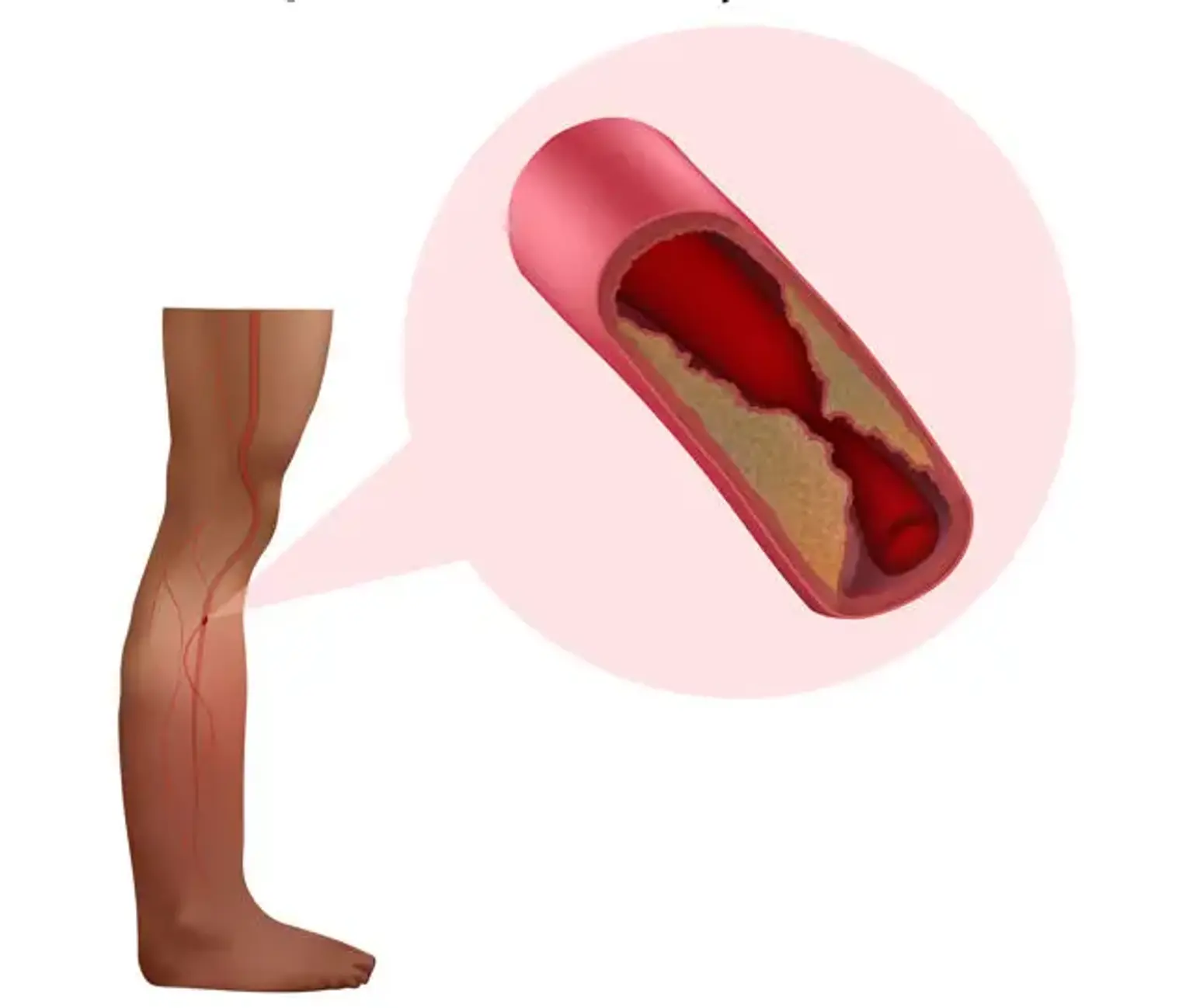
Peripheral artery disease
Overview
Peripheral artery disease (PAD) is a chronic, progressive atherosclerotic condition that results in partial or complete blockage of the peripheral vascular system. PAD usually affects the abdominal aorta, iliac arteries, lower limbs, and, in rare occasions, the upper extremities. PAD affects over 200 million people globally, and its global significance is growing as people live longer lives and are exposed to more risk factors.
PAD patients have a varied disease presentation and history, with some remaining asymptomatic and others advancing to arterial ulceration, claudication, resting limb ischemia, and limb amputation.
PAD is a cardiovascular disease comparable, with high-risk deadly and non-fatal cardiovascular events such as myocardial infarction and stroke happening often. PAD is a severe, progressive systemic illness that necessitates interprofessional collaboration to enhance patient outcomes.
This article discusses the fundamentals of evaluating and managing peripheral vascular disease, as well as surgical and non-surgical treatment options.
Peripheral artery disease definition
Peripheral artery disease (PAD) refers to blood vessel disorders that occur outside of the heart and brain. They are most commonly caused by the accumulation of fatty deposits in the arteries. PAD is also known as peripheral arterial disease or peripheral vascular disease, and it affects both the arteries and the veins.
Epidemiology
Nearly 200 million individuals worldwide suffer from peripheral vascular disease, including 40 to 45 million Americans. The condition is uncommon in younger populations; nevertheless, its prevalence rises dramatically with age, with more than 20% of those over the age of 80 suffering with PAD. The data on gender disparities is contradictory.
Men were more likely than women to suffer from intermittent claudication (IC). This conclusion agreed with the Rotterdam research, which discovered that males were 1.83 times more likely than women to develop IC, with a frequency of 2.2 percent in men and 1.2 percent in women. However, when PAD is diagnosed using the ankle-brachial pressure measure, there is a gender change in prevalence.
There are also racial and socioeconomic differences. When controlling for established risk variables, the CHS discovered that African Americans had an odds ratio of 2.12 for PAD compared to non-Hispanic whites.
When correcting for covariates, a compilation of three studies addressing the influence of race on the incidence of PAD reported odds ratios of 2.3 to 3.1 African Americans compared to Non-Hispanic whites. A socioeconomic survey research discovered that patients with lower poverty-income ratios (PIR) had a nearly twofold increase in the incidence of PAD when compared to those with greater PIR. Furthermore, the study discovered that having a lower educational level was substantially connected with PAD.
Etiology
Peripheral vascular disease is generally caused by atherosclerotic disease, which results in decreased major organ blood flow and end-organ ischemia. Atherosclerosis is a complicated process involving several cells, proteins, and pathways. In the progression of atherosclerosis, significant non-modifiable and modifiable risk factors have been discovered.
Risk factors include:
- Tobacco use
- Diabetes mellitus
- Hypertension
- HIV
- High cholesterol
- Age more than 50 years
- Elevated homocysteine levels
- BMI greater than 30
- Family history of cardiovascular disease
Pathophysiology
The advancement of atherosclerotic disease, which leads to macro and microvascular dysfunction, is the primary cause of peripheral vascular disease. PAD most commonly affects the arterial beds of the lower extremities, but bigger arteries such as the abdominal aorta and iliac arteries are frequently implicated. Multilevel and/or diffuse illness can occur in more severe cases. Atherosclerosis pathogenesis is a complicated inflammatory response involving multiple vascular cells, thrombotic factors, cholesterol, and inflammatory chemicals.
Atherosclerosis begins with the buildup of lipoproteins in the intimal layer of big arteries. The presence of lipoproteins within the endothelium causes lipid oxidation and a cytokine response, as well as the infiltration of lymphocytes and macrophages. Macrophages devour oxidized lipids and produce foam cells, resulting in the formation of "fatty streaks."
Although these fatty streaks are not clinically relevant, they can ultimately grow into more advanced plaques with necrotic lipid centers and smooth muscle cells (SMC). SMC and endothelial cells produce cytokines and growth factors, causing SMC to migrate to the luminal side of the plaque, extracellular matrix creation, and ultimate fibrous plaque development. Fibrous plaque stability is mostly determined by its composition, with more susceptible plaques having a thinner fibrous cap and a greater number of inflammatory cells.
Atherosclerotic plaque accumulates slowly within the vessel wall over time. Plaque buildup causes arterial constriction and frequent vascular dilation in order to enhance end-organ perfusion. Once the arterial dilation capacity is achieved, the plaque continues to collect, occasionally compromising the lumen and resulting to critical artery restriction. As the artery narrows and becomes occluded, collateral circulatory beds commonly form to maintain distant perfusion and tissue viability.
These collateral circulatory channels are incapable of totally matching the blood flow delivered by a healthy artery. When blood flow distal to the blockage is sufficiently disrupted, IC occurs, resulting in fixed oxygen supply that is insufficient to meet oxygen demand. Critical limb ischemia is the most severe type of PAD, characterized as limb discomfort at rest or approaching limb loss.
If in-situ vascular thrombosis occurs or a cardioembolic cause abruptly occludes the constricted channel, acute ischemia may result. Arterial thrombosis caused by progressive atherosclerotic disease and thrombosis accounts for 40% of all occurrences of acute limb ischemia (ALI). The rupture of an atherosclerotic fibrous plaque exposes subendothelial collagen and inflammatory cells, resulting in platelet adhesion and aggregation and fast in-situ thrombosis of the artery.
Because of the existence of substantial collateral circulation, patients with in-situ vascular thrombosis had better outcomes than those with embolic origins. Embolic ALI accounts for 30% of all ALI cases, with the femoral artery being the most prevalent location. ALI is a vascular emergency that needs prompt medical attention to preserve limb viability.
Clinical presentation
Diagnosis of peripheral vascular disease can be problematic due to the rising incidence of concomitant illnesses that show similarly and the vast number of patients who have an asymptomatic or atypical presentation. The degree of arterial insufficiency and the existence of concomitant diseases, which may modify or hide the symptoms of underlying vascular illness, frequently influence the clinical presentation of PAD.
Atypical PAD presentation arises when patients have pre-existing comorbidities such as lumbosacral illness, spinal stenosis, or severe diabetes mellitus, all of which can modify pain perception. Atypical pain is defined as pain that is unrelated to physical activity, pain that occurs both at rest and during effort, and pain that lasts more than 10 minutes after exercise is stopped.
Pseudo claudication is neuropathic pain seen in people with spinal stenosis that may be distinguished from PAD with a comprehensive history and physical examination. Patients with pseudo claudication have discomfort that is characterized by weakness and paresthesias regardless of physical activity level and is frequently eased by sitting down or altering body positions rather than rest.
Patients with hemodynamically significant PAD as shown by ABI testing are more likely to be asymptomatic rather than symptomatic. This demonstrates the significance of keeping a high clinical suspicion of underlying PAD for successful secondary prevention. Asymptomatic PAD affects more than half of all patients. The frequency of asymptomatic PAD may be explained in part by older people misinterpreting their symptoms as part of the normal aging process.
Furthermore, individuals with mild to severe PAD may be unable to exercise at a level that requires a substantial amount of oxygen. As a result, there is no mismatch between supply and demand, and patients stay asymptomatic.
The most common symptom of PAD is intermittent claudication, which is characterized by an exercise-induced cramping feeling accompanied by weariness, weakness, and/or pressure. Because individuals frequently deny pain, asking about discomfort while ambulating is a more relevant screening question.
Leg elevation aggravates symptoms and relieving the limb in a dependent posture alleviates them. Paresthesias, lower extremity weakness, stiffness, and chilly extremities are all possible. Anatomically, the degree of blockage is frequently evident one level above the place of pain; for example, individuals with aortoiliac illness would have symptoms in the buttocks and thighs.
Over a 10-year period, 70% to 80% of patients have stable intermittent claudication; nevertheless, a subset of patients may advance to excruciating ischemic rest discomfort, critical limb ischemia, and eventual amputation. Pain at rest, nonhealing sores or ulcers, and gangrene in one or both legs are symptoms of critical limb ischemia.
The physical exam begins with a general check, with special emphasis paid to fingernail tar, scars from past vascular procedures, and the existence of amputations. The first step in a targeted cardiovascular examination is a pulse examination to evaluate rate, rhythm, and strength.
Chest auscultation should be done to check for lung disorders such as chronic obstructive pulmonary disease (COPD) and pulmonary fibrosis, as well as heart sounds or murmurs. A neurological evaluation is required to rule out pseudo claudication.
The limbs should be examined for pulselessness, pallor, muscle atrophy, chilly or cyanotic skin, or discomfort with palpation. Lower extremity ulcers can be arterial, venous, neuropathic, or a mix of two or more of these types. Ulcers caused by vascular insufficiency are painful, with ragged edges, a dry foundation, and pale or necrotic cores.
Diagnosis
Peripheral vascular disease may be diagnosed adequately based on patient risk factors, clinical presentation, and physical exam results. Patients may appear with odd symptoms on occasion, and objective evidence can help establish a diagnosis. The assessment process begins with taking into consideration established PAD risk factors such as smoking, diabetes, hypertension, hypercholesterolemia, and obesity.
Intermittent claudication must be separated from neurological, musculoskeletal, or vascular diseases, all of which can mimic PAD. Lower extremity physical exam findings may include glossy skin with palpable coldness, decreased or absent pulses, irregular capillary refill time, pallor with leg elevation, and auscultation of bruits in major vessels such as the femoral and popliteal arteries. Nonhealing ulcers or gangrene are symptoms of advanced illness.
The ankle-brachial index (ABI) is a low-cost, noninvasive objective tool for diagnosing PAD. The ABI is calculated by dividing the systolic ankle pressure by the systolic brachial pressure. A blood pressure cuff is placed above the ankle, and a Doppler ultrasonography probe is placed on the dorsalis pedis or posterior tibialis, followed by inflating the cuff until the signal from the probe stops.
After then, the cuff is gradually deflated, and the return of the Doppler probe signal indicates the systolic ankle pressure. The procedure is then performed for the other leg. The greatest systolic pressure of either brachial artery is then divided by the ankle pressure of each leg. A typical ABI ratio is between 0.9 to 1.2, with results less than 0.9 indicating PAD. Noncompressible vessels, such as those observed in diabetics and persons with severe renal disease, may have erroneously increased ratios.
Individuals with unusually high ABI ratios had a higher all-cause death rate when compared to individuals with normal ABI ratios. A toe-brachial index (TBI), which compares the toe systolic pressure to the greater systolic brachial pressure, is frequently indicated for these individuals. These individuals demonstrate the critical role of the clinical history and physical examination in the early assessment of patients with suspected PAD.
Duplex ultrasonography is a safe and cost-effective means of detecting the site of a PAD, the degree of the stenosis, and the length of the stenosis or occlusion. The combination of 2-dimensional imaging and color Doppler allows for a precise evaluation of lesion stenosis, hemodynamic severity, and plaque features. Doppler ultrasonography can be utilized in normal post-procedure follow-up to monitor patency. When additional intervention is envisaged, this diagnostic modality can aid in decision-making.
Both magnetic resonance angiography (MRA) and computed tomography angiography (CTA) offer high-quality vascular imaging. MRA has the benefit of being able to identify tiny runoff vessels that may not be seen using digital subtraction angiography (DSA). When compared to DSA, MRA has a sensitivity of 90% and a specificity of 97% in detecting hemodynamically relevant lesions. CTA has diagnostic accuracy comparable to MRA, and both imaging procedures are beneficial in assessing eligibility for bypass surgery vs angioplasty.
Management
Patients with peripheral vascular disease require a methodical strategy that takes into consideration age, risk factors, disease severity, and functional level. Management is organized into two major groups, both of which aim to reduce cardiovascular events and improve symptoms. As a result, PAD care begins with lifestyle changes to avoid disease progression, followed by medication and interventional therapy to improve symptom control and reduce the risk of cardiovascular events.
Cardiovascular Risk Factor Modification
Modifying risk factors aggressively is critical for minimizing cardiovascular risk. Quitting smoking lowers the risk of PAD development, cardiovascular events such as myocardial infarction and stroke, and critical limb ischemia. To stop smoking and improve cardiovascular outcomes, patient education can be combined with behavioral treatment, nicotine replacement therapy, or pharmaceutical therapy.
Statin treatment has been found to minimize cardiovascular events, all-cause mortality, and the requirement for revascularization and should be taken frequently in PAD patients. Blood pressure-lowering to less than 140/90 in nondiabetic individuals and 130/80 in diabetic patients has been found to enhance results.
Diabetes increases the risk of symptomatic and asymptomatic PAD by 1.5 to 4 times, and a hemoglobin A1c target of less than 7% should be attained, with less rigorous objectives for patients with severe comorbidities.
Exercise Therapy
Guided exercise therapy programs have been shown to significantly alleviate claudication symptoms. Exercise increased pain-free walking distance by 269 feet and overall walking distance by nearly 400 feet, according to a meta-analysis of 27 trials. Exercise programs are generally comprised of 30- to 45-minute sessions held four to five times per week for a period of 12 weeks.
Pharmacotherapy
Patients who have not benefitted from exercise treatment and risk factor reduction might be given pharmacological therapy for intermittent claudication (IC). Cilostazol and naftidrofuryl are two medicines licensed for the treatment of IC. Cilostazol inhibits phosphodiesterase type 3 and possesses antiplatelet, vasodilatory, and smooth muscle cell proliferation inhibitory effects.
Cilostazol users had considerably greater pain-free and total walking lengths. Naftidrofuryl is a 5-hydroxytryptamine-2 receptor antagonist that reduces glucose absorption while increasing adenosine triphosphate levels. It has fewer negative effects than cilostazol and should be used whenever possible.
Revascularization
Patients with disabling symptoms who have failed to respond to risk factor adjustment, exercise, and pharmaceutical treatment may be candidates for endovascular, surgical, or combination endovascular and surgical surgery. Individuals with incapacitating claudication interfering with everyday function are candidates for intervention, as are patients with severe limb ischemia characterized by ischemic discomfort at rest, ulceration, and gangrene.
Many factors influence the decision between surgical and percutaneous intervention, including the patient's functional state and surgical risk, the operator's abilities, the anatomic location and degree of illness, the existence of multifocal vascular lesions, and patient desire. To increase results and patient satisfaction, an interdisciplinary team strategy combining an internist, interventionalist, and vascular surgeon should be used for tailored patient treatment.
Differential Diagnosis
When a patient exhibits the above-mentioned signs and symptoms, a physician must consider a number of differential diagnoses. Here are a few of the most important:
Neurological
- Nerve root compression
- Spinal stenosis
- Peripheral neuropathy
- Nerve entrapment
Musculoskeletal
- Medial tibial stress syndrome
- Osteoarthritis
- Muscle strain
- Baker cyst
Vascular
- Chronic venous insufficiency
- Thrombophlebitis
- Deep venous thrombosis
- Raynaud phenomenon
- Thromboangiitis obliterans
Prognosis
Patient risk factors, cardiovascular health, and disease severity must all be considered in the overall prognosis of individuals with peripheral vascular disease. In terms of limb health, over 80% of patients will have stable claudication symptoms after 5 years. In 5 years, only 1% to 2% of patients will proceed to critical limb ischemia. Within 5 years, 20% to 30% of people with PAD will die, with cardiovascular causes accounting for 75% of those fatalities.
Complications
Peripheral vascular disease can affect several systems in the body leading to a number of complications as listed below:
- Acute coronary syndrome
- Stroke
- Nonhealing ulcer
- Gangrene
- Amputation
- Deep vein thrombosis
- Erectile dysfunction
Atherosclerosis and PAD
If you have atherosclerosis, a plaque has accumulated within your arterial walls. Plaque is made up of fat, cholesterol, and other chemicals that have accumulated over time. The most prevalent cause of PAD is atherosclerosis in the peripheral arteries.
First, plaque accumulates to the point of narrowing an artery, reducing blood flow. If the plaque becomes brittle or inflammatory, it may rupture, resulting in the formation of a blood clot. A clot might constrict the artery further or entirely shut it.
If the blockage continues in the legs' peripheral arteries, it can cause discomfort, skin changes, trouble walking, and sores or ulcers. Gangrene and limb loss can result from complete lack of circulation to the legs and feet.
A stroke can develop if the blockage occurs in the carotid artery. It is critical to understand the facts concerning PAD. The more you know, the better you can assist your doctor in making an early diagnosis. PAD has typical symptoms, although many patients with PAD have no symptoms at all.
Conclusion
Peripheral vascular disorders are a major source of morbidity and limb loss. To improve outcomes in individuals with peripheral vascular disease, early detection and risk factor reduction are critical. Peripheral vascular disease has been linked to a number of risk factors, including smoking, diabetes, past coronary artery disease, and leading a sedentary lifestyle.
A comprehensive history and physical exam, particularly the ankle-brachial index, are essential for the diagnosis of peripheral vascular disease. This exercise covers the interprofessional team's involvement in evaluating and diagnosing a patient with suspected peripheral vascular disease. It serves as a guideline for interpreting ankle-brachial-index measurements.
As the cornerstone of care in these individuals, the treatment of peripheral vascular disease comprises risk factor management, antiplatelet therapy, and exercise. Endovascular, surgical, or combination interventional techniques are routinely used to treat patients with severe illness or symptoms that impede their ability to live a normal life.