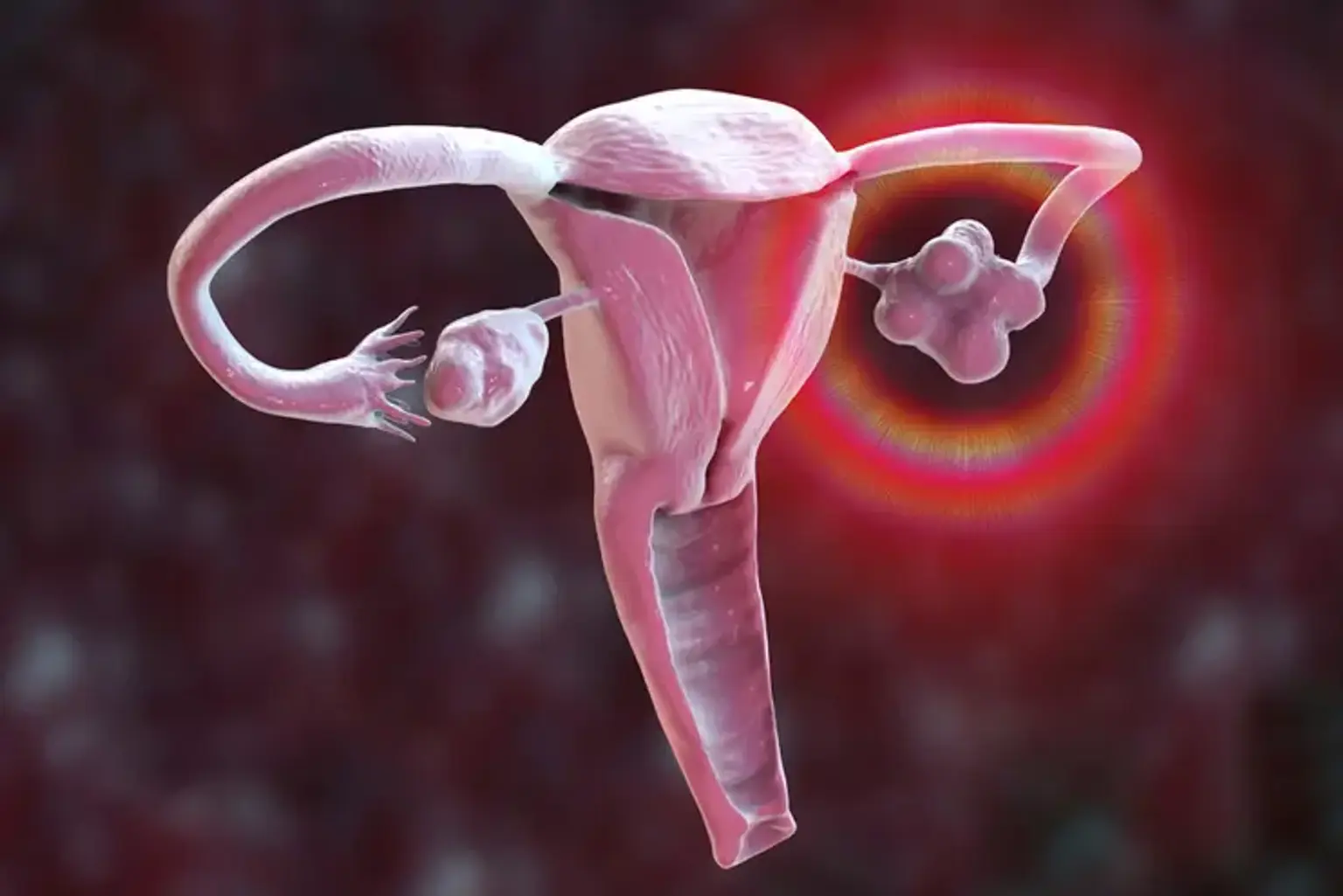
What is Polycystic Ovary Syndrome?
Polycystic Ovary Syndrome (PCOS) is a hormonal disorder affecting women of reproductive age. It causes a variety of symptoms, from irregular periods to excessive hair growth and acne. At its core, PCOS involves an imbalance of reproductive hormones like testosterone and insulin, which impacts ovarian function.
PCOS leads to polycystic ovaries, where multiple small cysts form. This condition disrupts normal ovulation and may result in infertility if left untreated. Though the exact cause of PCOS is not entirely understood, genetics and environmental factors play a significant role. Addressing the hormonal imbalance through lifestyle changes, medication, and sometimes fertility treatments can significantly improve symptoms.
Metabolic Implications of PCOS
PCOS is closely linked to insulin resistance, where the body's cells become less responsive to insulin. This leads to higher blood sugar levels and an increased risk of type 2 diabetes. In fact, women with PCOS are 2 to 3 times more likely to develop diabetes than women without the condition.
The metabolic effects of PCOS extend beyond diabetes risk. Women with PCOS are also at a higher risk of developing cardiovascular diseases, such as hypertension and high cholesterol. These long-term health issues underscore the importance of managing PCOS through lifestyle changes, including a healthy diet and regular exercise.
Weight gain is another common issue for women with PCOS. Insulin resistance makes it more difficult to lose weight, and excess weight exacerbates other symptoms, such as irregular periods and fertility problems. Addressing insulin resistance through medication, like metformin, alongside diet and exercise can help reduce these risks.
PCOS and Its Effects on Fertility
PCOS can significantly affect a woman’s fertility, primarily because it disrupts ovulation. Women with PCOS may experience anovulation, meaning the ovaries do not release eggs regularly. This makes it harder to conceive naturally.
While infertility is a common concern, many women with PCOS can still become pregnant with proper treatment. Medications like Clomid are often prescribed to stimulate ovulation. In some cases, assisted reproductive techniques like intrauterine insemination (IUI) or in vitro fertilization (IVF) may be necessary.
The chances of pregnancy improve when PCOS is managed through weight loss, metformin, and hormonal therapy. Additionally, early intervention with a fertility specialist is key for better outcomes.
Treatment Options for Managing PCOS
There’s no one-size-fits-all treatment for PCOS, but several options are available to manage its symptoms. Medications play a key role in treatment:
Metformin is often prescribed to help improve insulin sensitivity, which can help manage weight and regulate menstrual cycles.
Hormonal contraceptives (birth control pills) are commonly used to regulate periods, reduce acne, and control excessive hair growth.
Anti-androgen medications, like spironolactone, can reduce hirsutism and help with acne.
Alongside medications, lifestyle changes are essential for managing PCOS. A healthy diet that focuses on low glycemic index foods can improve insulin resistance and reduce weight gain. Regular exercise helps maintain a healthy weight and reduces the risk of heart disease and diabetes.
For women looking to conceive, fertility medications like Clomid or letrozole are often used to induce ovulation. For more severe cases, IVF or intrauterine insemination (IUI) may be necessary.
Diet and Exercise for PCOS Management
One of the most effective ways to manage PCOS is through diet and exercise. A balanced diet, rich in fiber, lean protein, and healthy fats, helps manage insulin resistance, stabilize blood sugar, and reduce symptoms like weight gain and acne. Women with PCOS should focus on low glycemic index foods to keep blood sugar levels in check.
Incorporating regular exercise—aiming for at least 30 minutes a day, five days a week—helps with weight management and improves insulin sensitivity. Activities like walking, cycling, swimming, and strength training are all beneficial for managing PCOS symptoms.
In addition to physical health benefits, exercise can help reduce stress, a common issue for women with PCOS. Stress management practices, such as yoga or meditation, can also improve overall well-being.
The Common Symptoms of PCOS
The symptoms of PCOS vary from woman to woman but commonly include irregular periods, weight gain, and acne. Many women with PCOS experience excessive hair growth (hirsutism) on the face, chest, or back, caused by elevated testosterone levels.
Another common issue is insulin resistance, where the body's cells don't respond to insulin properly, leading to high blood sugar and eventually a higher risk of type 2 diabetes. Women with PCOS may also experience thinning hair or even hair loss on the scalp.
Beyond the physical symptoms, PCOS can take a toll on mental health. Studies show women with PCOS are more likely to experience anxiety, depression, and stress, which can further complicate symptom management.
Emotional and Psychological Impact of PCOS
Living with PCOS can take a significant emotional toll on women. The physical symptoms—such as acne, weight gain, and excessive hair growth—can affect self-esteem and body image. Many women with PCOS also face challenges related to infertility, which can cause stress, anxiety, and feelings of inadequacy.
PCOS has also been linked to higher rates of anxiety and depression. The hormonal imbalances associated with the condition can contribute to mood swings and emotional instability. Additionally, the stigma surrounding symptoms like hirsutism or acne can lead to social withdrawal or self-consciousness.
Addressing these emotional aspects is just as crucial as managing the physical symptoms. Therapy or counseling, support groups, and stress-reduction techniques like mindfulness or yoga can help women cope with the psychological impact of PCOS. Building a strong support network with friends, family, and healthcare providers can also improve overall well-being.
Long-term Health Risks of Untreated PCOS
If left untreated, PCOS can lead to several long-term health complications. One of the most significant risks is type 2 diabetes, as insulin resistance can worsen over time. The combination of insulin resistance, obesity, and inflammation can increase the risk of metabolic syndrome, which includes high blood pressure, high blood sugar, and abnormal cholesterol levels.
Women with PCOS also face a higher likelihood of developing endometrial cancer due to irregular menstruation and lack of ovulation. This can result in thickening of the uterine lining, leading to a higher risk of cancerous changes.
Other long-term health issues include sleep apnea, fatty liver disease, and cardiovascular diseases. Early intervention and regular monitoring of these conditions are essential to reducing long-term risks and maintaining a good quality of life.
How PCOS is Diagnosed
PCOS is diagnosed based on clinical symptoms and medical tests. The Rotterdam criteria, the most widely used diagnostic tool, suggests that a woman must have at least two of the following three symptoms:
Irregular periods or absent periods.
Excess androgen levels, causing hirsutism, acne, and scalp hair thinning.
Polycystic ovaries, visible on an ultrasound.
To confirm the diagnosis, blood tests are essential to check hormone levels. Elevated testosterone and an imbalanced LH/FSH ratio are common indicators. Ultrasound helps detect the presence of cysts in the ovaries, although not all women with PCOS have visible cysts.
Since the symptoms of PCOS overlap with other health issues, it is important to rule out other conditions like thyroid disorders, which can mimic PCOS symptoms.
Fertility Preservation and PCOS
For women with PCOS who are concerned about future fertility, there are options for fertility preservation. Since PCOS can impact ovulation, some women may choose to freeze their eggs at a younger age to ensure the possibility of having children later in life.
Egg freezing, or oocyte cryopreservation, allows women with PCOS to preserve their eggs before they experience age-related declines in fertility. The process involves stimulating the ovaries to produce multiple eggs, which are then harvested and frozen for future use.
For women who are trying to conceive now, treatments like ovulation induction (using medications like Clomid or letrozole) can help stimulate ovulation. If these treatments are unsuccessful, more advanced options like in vitro fertilization (IVF) may be recommended.
The Global Popularity of PCOS Treatments
PCOS is a global health concern, affecting women across all ethnicities and regions. While the prevalence of PCOS is around 8-13% of women worldwide, cultural, socioeconomic, and healthcare factors can influence the availability and accessibility of treatment.
In countries with robust healthcare systems, treatments like metformin, birth control, and fertility treatments are commonly prescribed and widely accessible. However, in low-income countries, access to these treatments may be limited, making it more difficult for women to receive proper care.
Despite these challenges, the awareness and demand for PCOS treatments are growing globally. Social media, patient advocacy groups, and awareness campaigns have helped reduce stigma and educate women about PCOS. Increased knowledge about PCOS management has led to better resources and support for women in various parts of the world.
The Role of Birth Control in PCOS Management
For many women with PCOS, birth control pills are an essential part of treatment. Hormonal contraceptives regulate menstrual cycles, reduce acne, and help manage excessive hair growth (hirsutism) by lowering testosterone levels. By providing steady doses of hormones like estrogen and progestin, birth control helps restore hormonal balance, which can alleviate many of the common symptoms of PCOS.
For women who do not want to become pregnant, birth control can also serve as an effective method of contraception. Some women with PCOS may also experience mood swings or other side effects, so it’s important to discuss options with a healthcare provider to find the most suitable method.
However, birth control doesn’t address the underlying cause of PCOS, such as insulin resistance, so it is often used alongside other treatments like metformin and lifestyle changes for comprehensive management.
Managing PCOS During Pregnancy
Pregnancy can be a challenge for women with PCOS due to potential complications like gestational diabetes and pre-eclampsia, which are more common in those with PCOS. However, with proper management, most women with PCOS can have a healthy pregnancy.
For women who conceive naturally, early prenatal care is essential. Regular monitoring of blood sugar levels and blood pressure can help manage the risks of gestational diabetes and hypertension. If insulin resistance is present, medication like metformin may be continued to prevent gestational diabetes.
Women with PCOS who struggle with infertility may require fertility treatments like Clomid, IUI, or IVF. Once pregnant, it’s crucial to maintain a balanced diet, stay active, and monitor weight gain to minimize pregnancy-related complications. A holistic approach, including emotional support and mental health care, is equally important.
Alternative and Complementary Treatments for PCOS
While traditional treatments like birth control and metformin are commonly prescribed for managing PCOS, some women may explore alternative or complementary therapies. These treatments can include herbal remedies, acupuncture, and dietary supplements.
Herbs such as spearmint tea (known for its anti-androgen effects), saw palmetto, and cinnamon are often used to help balance hormones and manage symptoms like hirsutism and insulin resistance. However, the effectiveness of these treatments varies, and they should always be discussed with a healthcare provider to ensure safety and avoid interactions with prescribed medications.
Acupuncture is another alternative treatment that may help manage stress, improve insulin sensitivity, and promote ovulation. Some women also use vitamin D and omega-3 fatty acids supplements, as these can help regulate hormonal balance and improve overall health.
The Role of Support Systems in Managing PCOS
PCOS can be a challenging condition to manage, especially when it affects various aspects of a woman’s life—physical, emotional, and mental. One of the most important factors in managing PCOS is having a strong support system.
Support from family and friends can provide emotional relief and encouragement throughout the treatment process. Women with PCOS often benefit from connecting with others who share similar experiences. Online support groups, social media communities, and PCOS-focused organizations offer spaces to share stories, ask questions, and find resources.
Additionally, healthcare providers play a crucial role in providing guidance and empathy. A compassionate team that understands the complexity of PCOS can help a woman feel heard and supported. Regular consultations with specialists like endocrinologists, gynecologists, and nutritionists can create a tailored treatment plan that addresses both medical and emotional needs.
The Future of PCOS Research and Treatment
The future of PCOS research is promising, with ongoing studies focused on improving diagnostic tools, treatment options, and understanding the condition’s underlying causes. New advancements in genetics and hormonal research may lead to more precise ways to diagnose and treat PCOS.
One area of focus is personalized medicine, where treatments are tailored to a woman’s unique hormonal profile, lifestyle, and symptoms. Researchers are also looking into new medications that target insulin resistance, ovarian function, and androgen levels with fewer side effects.
Additionally, non-invasive treatments such as gene therapy and stem cell research are being explored for their potential to treat PCOS at the root cause. As awareness of PCOS increases, more funding and resources are being directed toward finding better solutions for women worldwide.
Navigating Insurance and Healthcare Costs for PCOS
One of the significant challenges many women with PCOS face is navigating healthcare costs and insurance coverage. Since PCOS requires ongoing care, including medications, fertility treatments, and sometimes surgeries, the financial burden can be substantial.
Insurance plans may cover some aspects of PCOS treatment, such as birth control or metformin, but coverage can vary widely. For fertility treatments like IVF or IUI, coverage is often limited or not included in many plans, depending on the country or region. This can make treatments like these unaffordable for women who need them to conceive.
It's important for women with PCOS to work with their healthcare provider to understand what is covered by insurance and explore other options for reducing costs, such as patient assistance programs or generic medications. For those without insurance, community health centers and nonprofit organizations may offer financial assistance or sliding-scale fees for treatment.
Empowering Women with PCOS Through Education and Awareness
Education and awareness are key to empowering women with PCOS. Many women go undiagnosed or misdiagnosed for years due to a lack of knowledge about the condition or its symptoms. Raising awareness about PCOS helps women recognize their symptoms earlier and seek treatment before the condition leads to more severe complications.
Global awareness campaigns, online resources, and educational materials play a significant role in providing women with the tools they need to manage PCOS effectively. Medical professionals also have a critical role to play in educating their patients and communities about the signs, risks, and treatments associated with PCOS.
In addition, advocacy organizations are working to ensure that PCOS gets the attention it deserves in both medical and public health arenas. With greater awareness comes better access to care and support, ultimately leading to improved health outcomes for women with PCOS.
Addressing PCOS Stigma and Social Challenges
Despite the growing awareness of PCOS, stigma still surrounds the condition, especially due to symptoms like excessive hair growth (hirsutism) and acne. This stigma can cause women to feel embarrassed or isolated, affecting their mental health and overall quality of life.
Society’s emphasis on beauty standards can lead to feelings of inadequacy or self-consciousness for women who experience visible symptoms of PCOS. To combat this, it's essential to create supportive, inclusive environments where women with PCOS are celebrated for their strength and resilience.
Social media platforms and patient advocacy groups have been instrumental in shifting the narrative, helping women with PCOS feel more comfortable sharing their experiences and finding solidarity with others. Creating more inclusive conversations around PCOS can help reduce stigma and foster a sense of community.
Conclusion
While PCOS presents challenges, it is entirely possible to live a fulfilling, healthy life with proper management and support. Early diagnosis, appropriate treatment, lifestyle changes, and a strong support system are key components in effectively managing the condition.
By understanding the hormonal imbalances, managing metabolic risks, and addressing emotional well-being, women with PCOS can lead active, vibrant lives. The future of PCOS research offers hope for more targeted treatments, but in the meantime, the empowerment of women through education, support, and awareness remains essential.
Whether it’s managing weight, seeking fertility treatments, or dealing with emotional struggles, women with PCOS have the opportunity to improve their quality of life and take control of their health. With the right approach, PCOS doesn’t have to define who you are, and the path to a balanced, healthy life is within reach.