Portal Hypertension
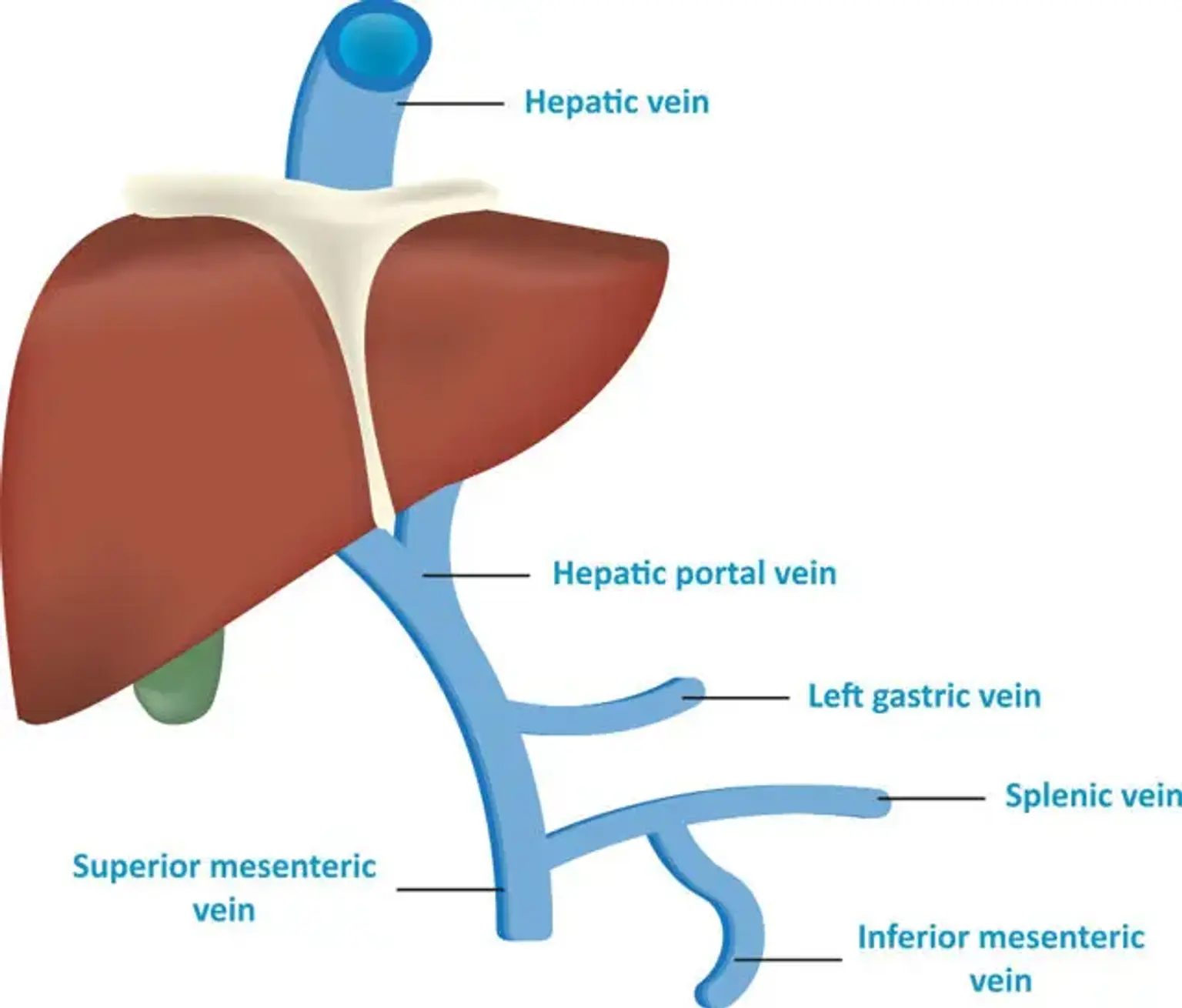
Portal hypertension is a medical condition that occurs due to increased blood pressure in the portal vein. This is a major vein that transports blood from the digestive organs, including the pancreas and the stomach, towards the liver. The portal vein is quite different from other veins that carry blood to the heart. Instead, it provides up to 75 percent of the blood supply to the liver.
Changes in the portal vein pressure could result in extreme complications, including infections, kidney failure, and bleeding. Generally, portal hypertension can be a chronic condition; however, it’s treatable and manageable if diagnosed earlier.
Causes of Portal Hypertension
The leading cause of portal hypertension includes cirrhosis, which refers to the scarring of the liver. Cirrhosis occurs due to a range of health conditions, including hepatitis, excessive consumption of alcohol, and other liver-damaging conditions. With cirrhosis, the scarring tissue hinders blood circulation via the liver, hence slowing down the process functions.
Autoimmune disorders affecting the liver are also the common causes of portal hypertension and cirrhosis. These disorders include primary sclerosing cholangitis, primary biliary cholangitis, and autoimmune hepatitis.
When the liver is damaged or injured, it usually attempts to heal slowly by itself. This results in the formation of scar tissue. However, excessive scarring makes it difficult for the liver to perform its normal function.
Thrombosis, blood clotting that occurs in the portal vein, can also cause portal hypertension. Other potential causes and triggers of cirrhosis include;
- Cystic fibrosis
- Non-alcoholic fatty liver disorder
- Poor development of bile ducts
- Accumulation of iron in the body
- Infections of the liver
- Reactions of some drugs like methotrexate
Risks Factors of Portal Hypertension
Individuals who are at a higher risk of acquiring cirrhosis also have an increased risk of suffering from portal hypertension. Other risks factors that can increase the chances of cirrhosis or portal hypertension include;
- A long history of excessive use of alcohol
- Obesity or overweight
- Type 2 diabetes
Signs and Symptoms of Portal Hypertension
During the early stages, most individuals do not often experience any signs and symptoms. However, as the condition gradually advances, one begins to develop some symptoms and complications.
The common complications and symptoms associated with portal hypertension include;
Gastrointestinal bleeding: This is associated with blood vomiting, traces of blood in the stool, or black, tarry stool. It occurs due to impulsive rupture and bleeding of the varices.
Encephalopathy: This involves confusion and memory loss due to poor functions of the liver and blood flow diversion away from the liver.
Ascites: This is characterized by swelling of the abdomen due to fluid accumulation in the space between various organs and the inner abdomen wall.
Anemia: This is an iron deficiency disorder that develops because of extreme loss of blood.
Weak immune system: This occurs as a result of a limited amount of white blood cells.
Portal Hypertension Diagnosis
In most cases, the portal hypertension symptoms are overlooked and can be confused with other health conditions. However, medical providers often suspect the disease if the current health state and medical history of the patient indicate that they have an increased risk of cirrhosis.
To further assess the condition, doctors can opt for various tests and procedures to diagnose and screen for portal hypertension. These diagnostic tests and procedures include;
Ultrasound:
This is an imaging, non-invasive diagnostic procedure that utilizes high-frequency sound waves. It produces pictures of the internal organs and structures. With this technique, the physician can easily monitor the flow of blood via the portal vein. They can also analyze the health state of the spleen and stomach.
With the use of ultrasound, the doctors can as well conduct elastography, a procedure to measure liver tissue elasticity. The parts with minimal elasticity indicate the presence of scarring tissue.
Other imaging tests that doctors can use to assess the portal vein system include;
- Magnetic resonance imaging (MRI): This is a common diagnostic technique that uses radio waves and powerful magnetic fields. It produces detailed pictures of the portal vein, structures, and surrounding organs.
- Computed tomography (CT) scan: This procedure combines information from various x-rays to create a more detailed image of the internal body structures.
- X-ray: This test uses a small amount of radiation energy to produce images of the portal veins and surrounding structures or organs.
Endoscopic examination:
Doctors often recommend an endoscopic examination if they detect gastrointestinal bleeding. This diagnostic procedure uses small flexible equipment attached to a camera at one of the tips. It enables the doctor to view the internal organs and diagnose portal hypertension or cirrhosis.
Endoscopy:
With this procedure, the doctor can assess the stomach, duodenum, and esophagus. Endoscopy involves the use of an endoscope, a small, flexible tube with a camera at the tip. This enables the doctor to visualize the internal organs and make a diagnosis via the computer linked to the endoscope.
Biopsy:
Doctors can sometimes recommend a biopsy if other diagnostic tests and procedures fail to produce non-conclusive results. It involves the removal of a small section of the liver tissue. This is for further examination for inflammation, scarring, and other symptoms of portal hypertension.
Portal Hypertension Treatment
Most causes and triggers of portal hypertension are untreatable. Instead, the available treatment options aim at managing and preventing associated complications, including bleeding due to varices. The treatment to administer usually varies from one person to another, depending on several factors. This can include the seriousness of the symptoms and functionality of the liver.
Overall, portal hypertension treatment options can include the following;
- Medications
Medical providers can recommend using nonselective beta-blockers, including nadolol or propranolol. They can prescribe such mediations alone or combining them with endoscopic therapy. This is to help alleviate and manage pressure within the varices and minimize the risks of bleeding.
Doctors can also recommend the use of nonselective beta-blockers to avoid a first variceal hemorrhage. This is especially in patients with varices and who are at a higher risk of bleeding. In most cases, esophageal variceal banding can be used for this purpose, particularly among patients who don’t take beta-blockers.
Doctors can recommend the drug lactulose for individuals with confusion symptoms and various mental impacts related to encephalopathy. On the other hand, they can prescribe Diuretics to treat fluid accumulation in the abdomen.
- Endoscopic therapy
Endoscopic therapy is usually the most common and first choice of treating variceal bleeding. It often comprises either sclerotherapy or banding. Banding is a treatment procedure that involves the use of rubber bands to obstruct the blood vessels. This aims at stopping the bleeding and easing the portal hypertension symptom. On the other hand, sclerotherapy is an occasional alternative that doctors opt for when banding can’t be used. It involves injecting blood clotting content to the bleeding varices to manage and stop bleeding.
- Lifestyle changes
Maintaining a healthy lifestyle and adjusting to better nutritional habits can help avoid portal hypertension. The most recommended things to consider to help enhance the liver functions include;
- Avoiding excessive consumption of alcohol and other harmful drugs
- Avoiding the use of over-the-counter drugs or herbal medications without consulting a medical provider. This is because certain types of drugs can worsen liver disorder.
- Following diet guidelines as directed by the doctor. This includes consuming a low sodium foods and limiting protein intake if confusion is one of the symptoms.
- Quitting smoking if you are a smoker
- Exercising regularly
Other Treatment Alternatives
While dietary changes, medications, and endoscopic therapy can help treat and manage portal hypertension, it’s not always effective for every person. It can fail to control ascites or accumulation of fluid in the abdomen and variceal bleeding in some cases. In such situations, the doctor can recommend other effective treatment options to address portal hypertension and associated symptoms.
These treatment procedures aim at reducing the pressure in the portal veins. They include the following;
Transjugular intrahepatic portosystemic shunt (TIPS): This treatment approach involves the placement of tubular equipment, a stent, in the mid part of the liver. It helps link the portal vein with the hepatic vein and redirects the flow of blood in the liver. This also helps minimize pressure in the affected veins.
Distal splenorenal shunt (DSRS): Although this technique is less common, doctors can use it to address portal hypertension and associated symptoms. It links the vein in the spleen and the vein in the left kidney. This is to prevent bleeding and minimize pressure within the varices.
Conclusion
Portal hypertension is generally a chronic disease. It usually occurs due to an increase in the blood pressure in the portal venous system. While it’s impossible to reverse the damages associated with cirrhosis, treating and managing portal hypertension is the best alternative. The treatment can include a combination of medication, lifestyle changes, and other interventions. Furthermore, practicing a healthy lifestyle and avoiding alcohol can help prevent the condition from aggravating.
Cloud Hospital specializes in helping patients suffering from portal hypertension. It comprises a specialized medical team and professional physicians whose aim involves diagnosing, treating, managing, and even preventing the disease.