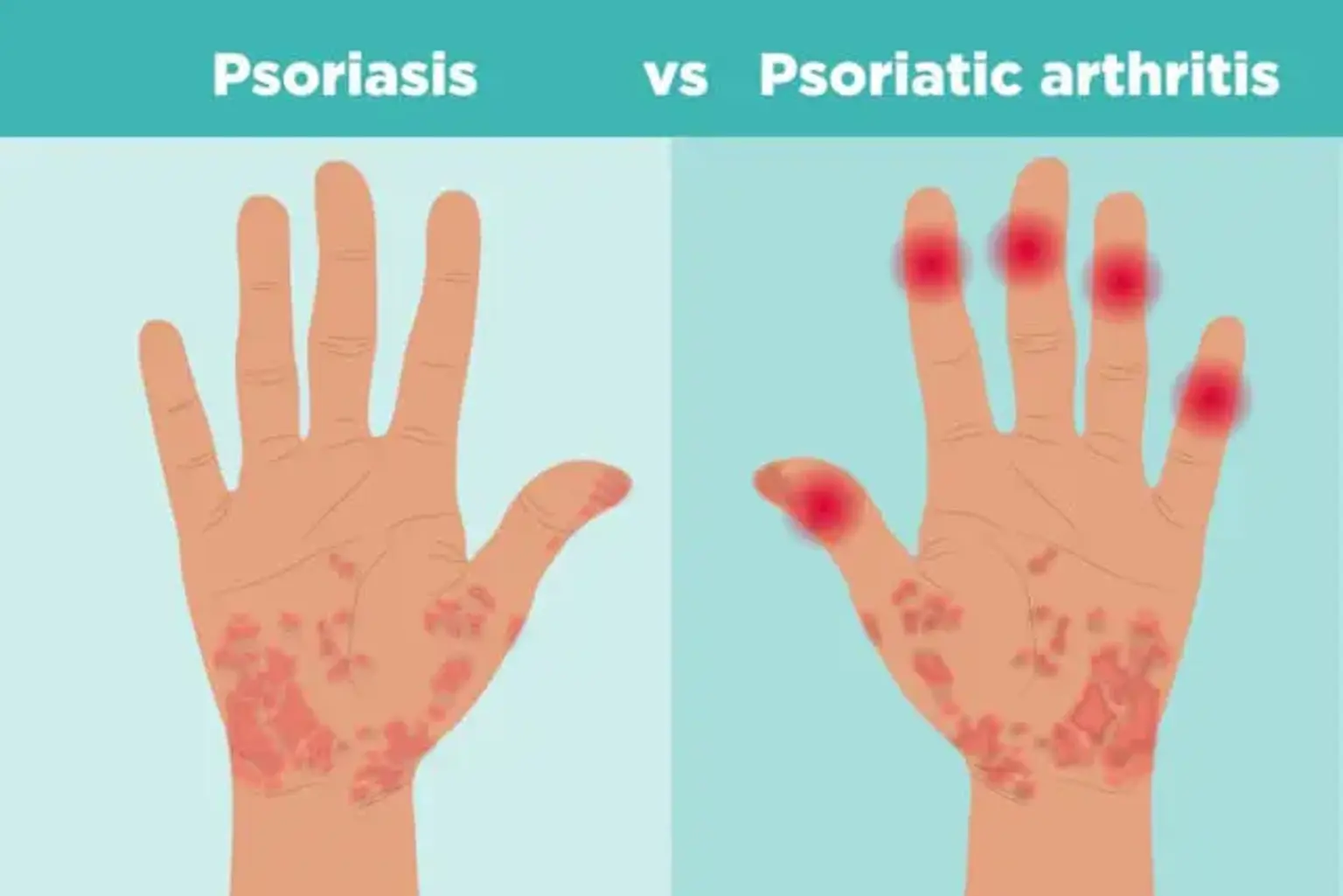
Psoriasis Arthritis
Psoriasis arthritis is a type of arthritis characterized by swelling, joint pain, and stiffness. It can affect people with psoriasis, a disorder that causes scaly and itchy red patches on the skin or scalp. Many individuals get psoriasis first before they are later detected with psoriasis arthritis. However, the joint issues may at times develop before the appearance of the skin patches.
Psoriasis arthritis can occur in any area of the body, such as the spine and fingertips. They also range from fairly moderate to chronic. In both cases of psoriasis and psoriasis arthritis, the condition flares tend to alternate with remission periods.
Types of Psoriasis Arthritis
The major types of psoriasis arthritis include the following;
- Symmetric psoriasis arthritis
This form of psoriasis arthritis usually affects a similar joint on either side of the body. For example, your right and left knees. Typically, symmetric psoriasis arthritis is mild and leads to minor joint deformity compared to rheumatoid arthritis. On the other hand, it tends to be a disabling condition.
- Asymmetric psoriasis arthritis
This type affects one joint or the joints on a single side of the body. Generally, asymmetric psoriasis arthritis is a mild condition that makes the joints turn red and feel sore. Approximately 35% of people with psoriasis arthritis have this type.
- Distal interphalangeal predominant psoriasis arthritis
This mainly affects the joints nearest to the nails, referred to as the distal joints. It develops in approximately 10% of patients who have psoriasis arthritis.
- Spondylitis psoriasis arthritis
This type often affects the spine. It can include the whole spine right from the neck down towards the lower back. Moving can be excruciating as a result of this. It’s also possible that your feet, hands, legs, hips, and arms will be affected.
- Psoriatic arthritis mutilans
This is a deforming and severe form of psoriasis arthritis. It affects about 5% of individuals who have psoriasis arthritis. Psoriatic arthritis mutilans mostly develop in the feet and hands. It might as well cause pain and discomfort around the neck and lower back.
Signs and Symptoms of Psoriasis Arthritis
Psoriasis arthritis symptoms vary from one person to another. They can range in severity from mild to chronic. The condition may go into remission at times, and you are likely to feel better for a certain period. However, the symptoms may worsen during other times. The form of psoriasis arthritis you have affects your signs as well.
The following are some of the most common psoriasis arthritis early symptoms:
- Morning joint stiffness
- Swollen and tender joints on a single or either sides of the body
- Painful and sore tendons and muscles
- A flaky scalp
- Swollen toes and fingers
- Scaly patches on the skin that might worsen in the event of joint pain flares
- Fatigue
- Separation of the nail from the bed
- Nail pitting
- Uveitis (eye pain)
- Reddening of the eye
The symptoms associated with spondylitis psoriasis arthritis include;
- Pain and stiffness around the spine
- Swelling, weakening, and pain in the hips, ankles, knees, elbow, feet, hands, wrists, and other joints
Causes of Psoriasis Arthritis
When the immune system attacks the healthy body cells and tissue, psoriatic arthritis develops. Inflammation of the joints and too many skin cells are associated with an abnormal immune reaction.
It is unclear why the body's immune system strikes the healthy tissue. However, both environmental aspects and genetics are likely to play a major role. Psoriasis arthritis is common in people with a family history of psoriasis or psoriatic arthritis. According to studies, some gene markers appear to be linked to psoriatic arthritis cause.
Psoriatic arthritis can be triggered by physical trauma or environmental aspects, like a viral and bacterial infection. This is especially in individuals who have an inheritable tendency.
Risk Factors of Psoriasis Arthritis
The following factors can alleviate the likelihood of developing psoriasis arthritis;
Psoriasis: This is the single most important risk factor for getting psoriatic arthritis. It is more likely to occur in individuals with pitted and malformed nails.
Family background: Most people who have psoriasis arthritis have a sibling or parents who also suffer from the condition.
Age: Even though psoriasis arthritis can affect anybody, it is more common in individuals aging between 30 to 50 years.
Psoriasis Arthritis Diagnosis
There is no particular test to verify psoriasis arthritis diagnosis. However, doctors can perform some tests for psoriasis arthritis to rule out various triggers of joint pain, including rheumatoid and gout.
Physical examination:
During the examination, the physician can check for swelling and tenderness signs in your joints. They will also look for flaking, pitting, and some abnormalities in your fingernails. If necessary, they can try to locate delicate regions, press on the soles of the feet and near the heels.
Imaging tests:
X-ray: Basic x-rays can assist identify abnormalities in the joints that are specific to psoriatic arthritis and not to other types of arthritis.
Magnetic resonance imaging (MRI): This creates incredibly detailed pictures of both soft and hard tissues in the body using radio waves and a powerful magnetic field. This imaging examination can be performed to look for tendons and ligaments abnormalities in the lower back and feet.
Lab tests:
Rheumatoid factor (RF): This is an antibody found in the blood of individuals who have rheumatoid arthritis. However, it is not present in the blood of a patient who has psoriasis arthritis. As a result, this test enables the doctor to differentiate between the two illnesses.
A joint fluid test: This involves removing a small fluid sample from one of the damaged joints with a syringe, usually the knee. If you have uric acid crystals in the joint fluid, you have gout instead of psoriatic arthritis.
Psoriasis Arthritis Treatment
There is no existing cure for psoriasis arthritis. However, the available treatment options aim at managing inflammation and improving the associated symptoms. This eventually prevents pain and disability of the joint.
Medications:
Doctors can recommend the following medication to address psoriasis arthritis;
Nonsteroidal anti-inflammatory drugs (NSAIDs): These are pain and inflammation relievers. Ibuprofen (Advil and Motrin IB) and naproxen sodium are examples of over-the-counter NSAIDs. Prescriptions are available for the potent NSAIDs.
Disease-modifying antirheumatic drugs (DMARDs): These medications help delay the progress of psoriasis arthritis. They also protect the joints and the other body tissues from long-term damage. Methotrexate (Trexall, Otrexup, and others), sulfasalazine(Azulfidine), and leflunomide (Arava) and are examples of DMARDs.
Biologic agents (biologic response modifiers): This is the new group of DMARDs. Abatacept (Orencia), certolizumab (Cimzia), and adalimumab (Humira) are some of the examples. These drugs work by targeting certain components of the immune system that cause inflammation and joint injury.
Immunosuppressants: These drugs work by calming down your immune system, which is overactive in people with psoriasis arthritis. Cyclosporine (Gengraf, Neoral, Sandimmune) and azathioprine (Imuran, Azasan) are common examples.
New oral drug: An example of this medicine is apremilast (Otezla). It reduces the action of an enzyme in the body regulating inflammation in the cells. Nausea, diarrhea, and headaches are all possible adverse effects.
Other treatment options and procedures:
Splitting:
The doctor can sometimes suggest splinting the joints to relieve inflammation and concerns with joint stability or alignment. The splints will be removed occasionally, and moderate range-of-motion workouts can be conducted to keep movement in the joints.
Surgical procedure:
The majority of people who have psoriasis arthritis don’t always require surgery. Joint replacement surgery may, however, be needed for severely injured joints. Physicians can perform the surgery to help restore functionality, ease discomfort, improve mobility, or enhance the aesthetics of the damaged area.
Heat and cold therapy:
Intermittent cold and heat therapy includes alternating between moist heat and cool treatment on the damaged joints. A hot pack, warm towel, or warm shower or bath will help calm aching muscles and reduce joint pain, soreness, and swelling. By freezing the affected joints, cold therapy can ease swelling and minimize discomfort. This is achieved using a bag of ice or a bag with frozen vegetables covered in a towel.
Exercise:
Psoriasis arthritis can cause joint pain and stiffness, which can be relieved with moderate, frequent activity. In addition to low-impact aerobics, range-of-motion and strengthening training as prescribed and directed by the occupational or physical therapist may be beneficial.
Discuss the workout alternatives with the healthcare professional before starting any new fitness program. Choose an exercise regimen that you will enjoy doing so that you will keep on doing it no matter what. Keep in mind that overly strenuous or ineffective fitness routines can aggravate psoriasis arthritis.
Complications of Psoriasis Arthritis
Arthritis mutilans is a painful, severe, and disabling form of psoriasis arthritis that affects a small percentage of patients. The tiny bones of the hands, particularly the fingers, are destroyed over time by arthritis mutilans, resulting in lasting deformity and incapacity.
Psoriasis arthritis patients may have eye problems like pink eye (conjunctivitis) or uveitis. This causes inflamed, aching eyes and obscured vision. They also have a high chance of heart disease.
Conclusion
Psoriasis arthritis is associated with psoriasis, a severe skin and nail condition. Some people experience relatively minor symptoms that only present issues on occasion. Others have symptoms that are more severe and incapacitating.
Psoriasis arthritis will have a greater impact on your ability to move around the more serious the symptoms are. Walking, climbing stairs, and doing other daily tasks may be difficult for people with many joint injuries.