Introduction
Joint resurfacing surgery is a specialized procedure designed to treat joint pain and degeneration, particularly in the hip and knee. Unlike traditional joint replacement, which involves replacing the entire joint, joint resurfacing focuses on repairing and rebuilding the joint surface while preserving the underlying bone. This approach offers several benefits, including quicker recovery, less post-surgical pain, and the preservation of more natural joint function.
Joint resurfacing has grown in popularity globally, especially among younger, active patients who are looking to avoid full joint replacements. It’s an effective option for those suffering from conditions like osteoarthritis, which causes the cartilage in the joints to deteriorate, leading to pain and reduced mobility. The procedure provides a promising alternative to traditional replacements by offering pain relief and improved joint movement, without the need for extensive bone removal.
What is Joint Resurfacing Surgery?
Joint resurfacing surgery is a minimally invasive procedure aimed at repairing damaged joint surfaces, often in the hip or knee. The process involves removing the worn-out cartilage and resurfacing the joint with a specially designed implant. This allows the joint to regain smooth motion and reduces pain, while retaining more of the patient's natural bone structure compared to traditional joint replacement surgery.
The surgery typically uses metal, ceramic, or plastic materials for the implants, chosen based on the patient’s unique needs. Unlike full joint replacement, where the entire joint is removed and replaced, joint resurfacing leaves most of the bone intact. This is particularly beneficial for younger patients, who may face the need for future surgeries if they opt for a complete replacement. Resurfacing offers a more bone-conserving solution, promoting better long-term outcomes.
The Science Behind Joint Resurfacing: How It Works
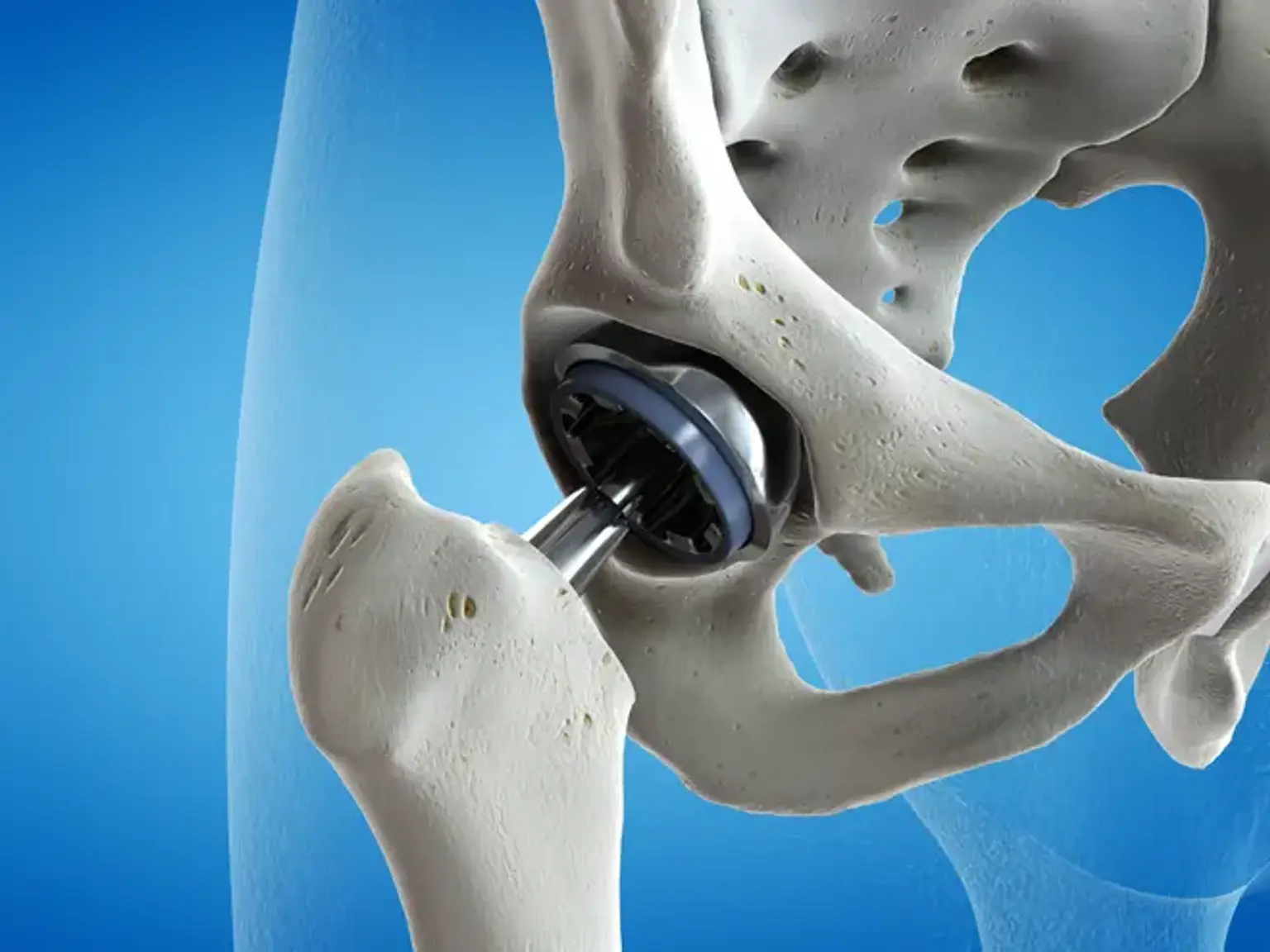
The primary goal of joint resurfacing is to restore the smooth, functional surface of the joint, allowing it to move with minimal friction and pain. In the case of hip resurfacing, for example, the damaged ball of the femur is shaved and covered with a metal cap, while the socket of the hip joint is lined with a durable metal or ceramic cup. In knee resurfacing, the damaged parts of the knee are resurfaced with implants that help restore smooth movement.