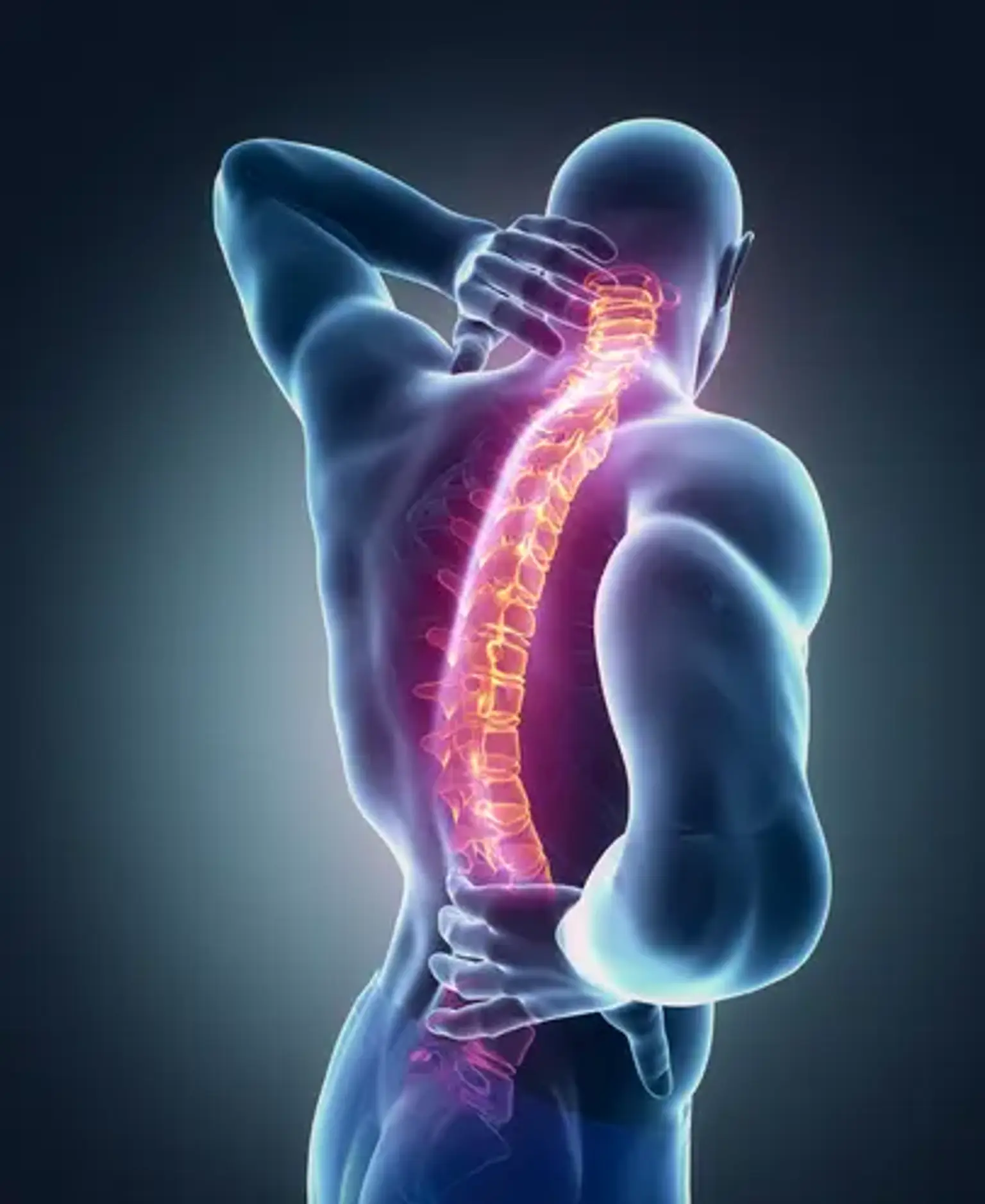
Spine Trauma
Overview
Spine trauma is caused by a sudden injury to the spinal cord or the bones that surround it. This condition most commonly affects the cervical spine (in the neck) or the thoracic spine (in the upper back). Fractures, crushing or compressing, and bone dislocation are all examples of trauma. Following the initial trauma, additional injury may occur as a result of swelling and inflammation, as well as internal bleeding and accumulation.