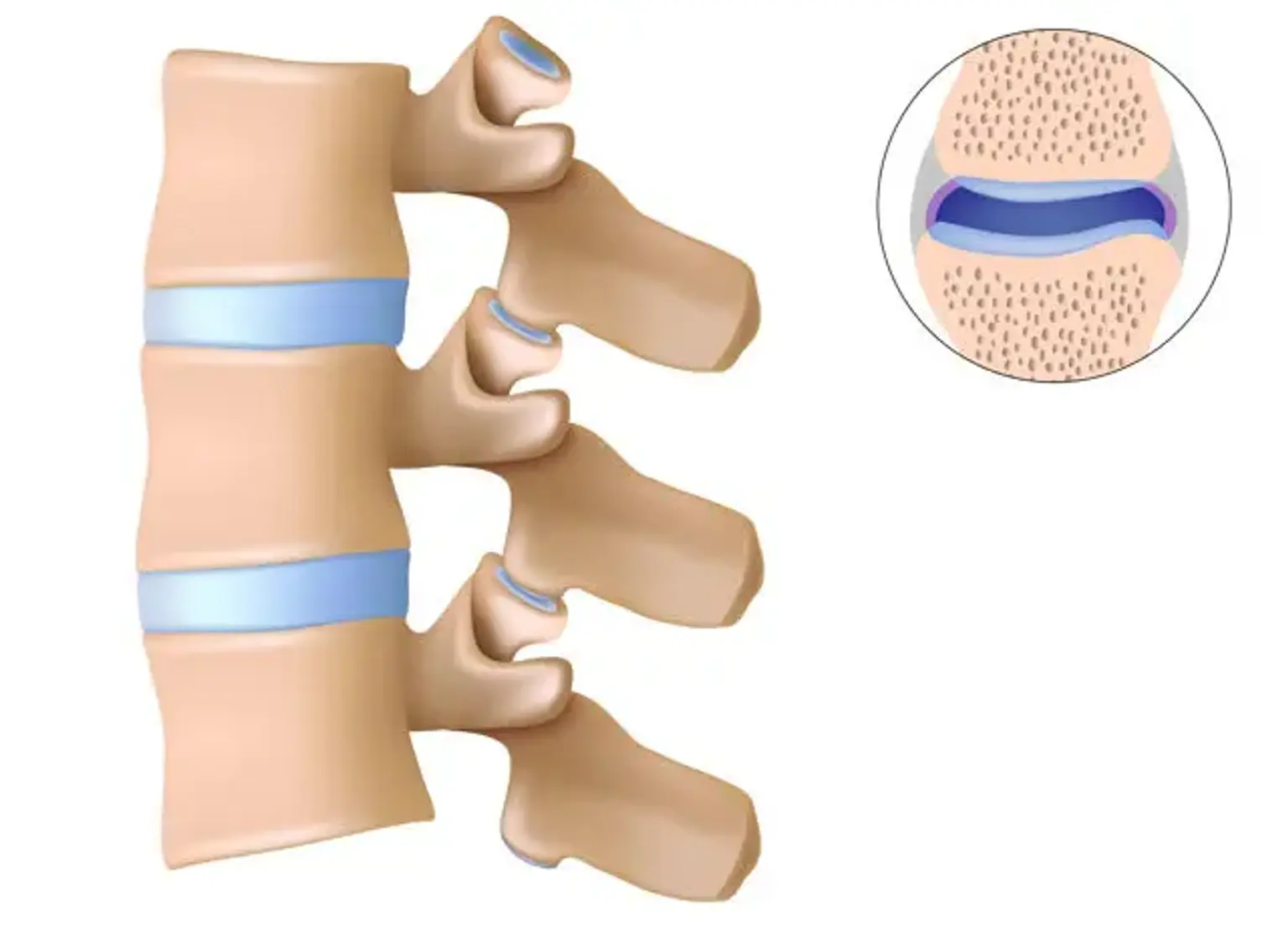
Synovial Cyst
Overview
Synovial cysts are abnormal fluid-filled sacs that develop in the joints of the spine. These cysts are not malignant, as they are benign. Synovial cysts often arise as a result of aging-related degenerative changes. They can be found all the way up the spine, although they are most frequent in the lower back.
Synovial cysts definition
Synovial cysts are prevalent extradurally detected in the lumbar spine and cause symptomatic radiculopathy and back discomfort. Repetitive motion and degenerative processes along the facet capsule might aggravate synovial cysts and intensify symptoms. Because these lesions might be confused for intradural nonenhancing lesions at times, a thorough preoperative workup is required to differentiate synovial cysts from a more serious diagnosis.
The symptomatology, position of the facet, and absence of augmentation can all aid in the rapid and correct diagnosis. These lesions are normally treated conservatively, but may need percutaneous aspiration or lumbar decompression and fusion.
How does a synovial cyst develop?
A facet joint in your spine might create more fluid than a healthy joint as it deteriorates. The fluid is beneficial to the injured joint. It adds lubrication and aids in the mobility of the joint. However, a cyst may form as a result of the additional fluid. As the fluid accumulates, it can become lodged in the synovial lining of the joint. A cyst may eventually develop.
The cyst fluid is not hazardous. It is not under any pressure and will not create any difficulties until it begins to press on the spine. Even very big cysts are rarely a source of concern.
Epidemiology
- Synovial cysts are frequent in the spine, especially in the lumbar spine. Spinal synovial cysts are most commonly seen in the spinal canal, near the lumbar spine's facet joints.
- Although the pathogenesis of synovial cysts is unknown, many theories have been proposed to explain the causes of spinal synovial cysts, including degenerative changes in the facet joints, trauma, metaplasia, the presence of developmental rests, excess stress inflicted at the facet joints coupled with synovial tissue herniation, and mucinous degeneration in the connective tissues.
- According to certain studies, trauma can cause cyst growth or bleeding into the synovial cyst cavity, resulting in epidural compression of the spinal cord.
Synovial Cyst Symptoms
The size, location, and influence of the cyst on the surrounding brain structures will all have an impact on the patient's symptoms. Typical symptoms will typically involve one or more of the following:
- There may or may not be lower back discomfort.
- Lumbar radiculopathy, often known as leg discomfort (also called sciatica). Leg discomfort can affect one or both legs and can spread down the back of the leg and into the foot.
- When the patient is sitting, the spinal canal opens up and there is less pressure on the spinal nerves, resulting in minimal or no discomfort. When you stand up straight or walk, the spinal canal closes, putting extra pressure on the nerves.
- Neurological deficiencies in one or both legs, such as numbness or tingling, or muscular weakness. Foot drop may be a weakness.
- Neurogenic claudication is characterized by a painful, cramping sensation in the legs.
Cauda equina syndrome can occur as a result of a synovial cyst in rare cases, and it is a dangerous illness that requires prompt medical treatment.
Stenosis Associated with Synovial Cysts
Facet joints are the most common site for intraspinal synovial cysts, however they can also grow from the ligamentum flavum or the posterior longitudinal ligament. They have been linked to an increase in the incidence and severity of facet joint osteoarthritis, as well as degenerative alterations in the ligamentum flavum. Synovial cysts are more common in the L4-5 region. Around half of all patients with lumbar synovial cysts also have degenerative spondylolisthesis at the same level.
Lumbar synovial cysts cause neurological symptoms in around 2.3 percent of LSS patients. Radicular pain is the most prevalent symptom, and one-third of patients have characteristic neurogenic claudication. Rapid cyst growth can occasionally result in acute cauda equina syndrome.
The spontaneous clearance of a synovial facet joint cyst is uncommon, and the efficacy of conservative therapy has been called into doubt. However, repeated CT-guided steroid injections into the afflicted joint have resulted in symptom relief in around 75% of patients. Because synovial cysts are frequently attached to the neighboring dura, surgery raises the chance of an inadvertent dural rupture.
Primary fusion's role is being contested, and the choice to conduct it should be taken on an individual basis. Concurrent instrumented fusion has been recommended for younger patients with mobility degenerative spondylolisthesis or minimal degenerative alterations at the afflicted level.
Additional stabilization may be required if a full facetectomy is required for safe excision of a big cyst. Following decompression alone, 6.2 percent of patients require reoperation within 25 months (typically a fusion treatment for mechanical back pain), and 1.8 percent had a synovial cyst recurrence at the same level. Same-level cyst recurrence has not been recorded following decompression and concurrent fusion.
Diagnosis
An MRI scan of the spine is the best way to see the synovial cyst. It manifests itself as a hyperintense lesion with the same signal intensity as water.
To rule out any spinal instability, x-rays, especially flexion/extension motion x-rays, are also necessary. It is critical to screen for spinal instability because the joint is degenerating, and there is frequently an associated degenerative spondylolisthesis (vertebral body slips forward), indicating that the joint is unstable and incompetent.
It is critical to discover any instability prior to surgery for the synovial cyst, since if the instability is not treated at the time of surgery, a revision operation will frequently be necessary later.
CT scan
CT, CT myelography, or MRI can identify synovial cysts; MRI is regarded to be the most sensitive. Calcified cysts are seldom seen on plain radiographs. The histology of synovial cysts varies greatly, as does the appearance of the cysts on imaging. Synovial cysts can be simple thin-walled collections of synovial fluid, or they can be complicated by chronic or acute bleeding and inflammation.
With a thin, low-signal wall, pure cysts show a strong T2 signal that is equivalent to or greater than that of cerebrospinal fluid (CSF). Chronic bleeding can cause cyst contents to generate a strong T1 signal (methemoglobin) and a fluctuating T2 signal; the wall frequently enhances with gadolinium. The wall may grow relatively thick in the context of persistent inflammation and calcification, with very low T1 and T2 signals.
On CT, calcification is seen in varying degrees, and cyst contents range from hypodense to slightly hyperdense in comparison to muscle. Arthrosis changes in the neighboring facet joint are common, as are aberrant marrow signals (T2 hyperintensity, T1 hypointensity) in the articular processes and pedicle.
On CT or MRI, direct connection with the facet joint is not usually visible. Because synovial fluid recedes into the joint space, compressing the cyst, synovial cysts may not be seen on recumbent CT or MRI imaging; when the patient accepts axial load, the joint surfaces are opposed, forcing the fluid into the cyst, which subsequently exerts mass impact on neural components.
Despite the absence of indication of their existence on recumbent advanced imaging, synovial cysts usually fill when the joint is compressed by intra-articular injection.
Lumbar synovial cysts
Lumbar synovial cysts are cystic dilatations of synovial sheaths that protrude into the spinal canal directly from facet joints. When magnetic resonance (MR) scans were compared to surgical findings in 18 individuals with synovial cysts, the cysts measured an average of 16 mm (ranged 10–28 mm), with 3 (17%) including hemorrhages.
These cysts include two kinds of fluid. The most common gelatinous cysts are difficult to aspirate, although the less common serosanguinous cysts, which contain less viscous fluid, may be more susceptible to percutaneous aspiration. Regardless of whether fluid can be evacuated from inside these cysts, the fibrous capsule that remains contributes to clinically significant compression of the thecal sac and nerve root.
MRI studies show that the massive, thick, fibrous, and frequently calcified capsules enclosing the fluid within the synovial cysts are primarily responsible for the bulk of neural/dural compression and neurological impairment. Furthermore, improved MR investigations show extensive adhesions between the cyst capsules and the underlying dura and nerve roots, both cephalad/foraminally leaving and caudad/lateral recess exiting nerve roots.
Management
There are three primary non-surgical therapy options for lumbar spine synovial cysts:
- Observation and activity modifications
- General non-surgical treatments for pain relief
- Injections
Observation and Activity Modification
If the synovial cyst does not cause significant dysfunction or pain in the patient's everyday life, no medical treatment may be required. Because pain is generally induced by certain postures, shifting positions is a legitimate technique to cope with pain as long as a patient can still function normally.
General Non-Surgical Treatments
In addition to activity modification, patients may often receive pain alleviation from a variety of nonsurgical options, including but not limited to:
- Application of ice and/or heat, which is especially useful for pain and discomfort caused by physical activity
- Pain relievers, such as nonsteroidal anti-inflammatory drugs (such as ibuprofen), acetaminophen, and/or prescription pain relievers
- Rest is most useful for short periods of time, such as a few hours or a day or two.
Almost every treatment plan will incorporate some sort of workout and stretching practice. Because the patient should be somewhat comfortable in the sitting posture (leaning forward) for aerobic exercise, stationary riding may be preferred than walking.
Injections for Synovial Cysts
There are two types of injections that can be helpful to alleviate the pain: facet injections or epidural injections.
- Facet injection. A tiny needle can be used to enter the facet joint, and the cyst can occasionally be emptied by aspirating it via the joint. The joint is then injected with steroids to reduce inflammation.
- Epidural steroid injection. The most typical injection approach is to inject steroid around the cyst in the epidural area, which is known as an epidural injection. It does not shrink the cyst, but it can alleviate discomfort. Although the cause of pain reduction is unknown, it is considered to be attributable to a decrease in inflammation. It works approximately half of the time and not so well half of the time, and regrettably, the pain alleviation is just short.
Even if each injection is not very dependable in the long run, it is appropriate to attempt because the only other option is surgery. In general, no more than three injections per year are advised.
If injections do not offer adequate pain relief or return to a functional level that is acceptable, surgery may be considered.
Spine Surgery for Synovial Cysts
The most frequent types of spine surgery for synovial cysts are decompression alone or decompression combined with spine fusion.
Microdecompression Spine Surgery
If there is no accompanying instability with the cyst (for example, no degenerative spondylolisthesis as observed on flexion/extension x-rays), then a microdecompression of the nerve root with cyst removal is appropriate. This is essentially the same procedure as a microdiscectomy, and it is a minimally invasive operation with a reasonably short recovery.
However, because the initial joint disease that created the synovial cyst still exists, the cyst might re-form at a later period.
Decompression with Spine Fusion Surgery
The most dependable approach of treating a synovial cyst is to remove the cyst and then fuse the joint. Fusing the joint prevents all mobility at that level of the spine, therefore the cyst should not renew if there is no motion.
This is the most dependable therapy, but it is also the most invasive for the patient. It alters the biomechanics of the back because one of the joints ceases to function. The L4-L5 level has the most mobility, thus fusing it puts additional strain on the lower spine's other non-fused levels. Furthermore, the operation is more difficult since a fusion is an open procedure, and the fusion takes six to nine months or more to recover.
Decision-Making Factors for Patients
When deciding which treatment to pursue, patients need to base their decisions on three primary factors:
- The amount of pain they are having
- The length of time of their symptoms
- The amount of dysfunction it causes in their life
If the pain is reasonably intense and manageable, the patient should probably modify his or her activity. If the discomfort is severe, an injection may be more appropriate. If the pain is severe and has persisted for a long time (e.g., years), or if injections have failed, surgery may be a better option.
A trial of a microdecompression is certainly a valid idea for younger, more active individuals, as long as there is no significant instability of the joints. A microdecompression operation is performed with the understanding that a fusion may be required in the future. For more senior or less active individuals, it may be more rational to proceed to the ultimate treatment of fusion, because the stress transfer created by the fusion to the other joints is not as large in these people, and only one procedure would be required.
Surgery Considerations and Success Rates
Surgery is only required for those who want to conduct greater activities with less discomfort. For the therapy of this illness, surgery is quite beneficial.
The most effective operation is usually a decompression followed by a fusion. (A 90-95 percent success rate is to be predicted, implying a considerable reduction in pain but not necessarily complete elimination). However, this is the most difficult form of surgery to have since it alters the biomechanics of the spine. It should be considered for those who have moderate to severe activity limits, joint instability, and have failed non-surgical therapies such as injections.
Difference between ganglion and synovial cysts?
A ganglion cyst is a fluid-filled sac that frequently appears in the wrists and ankles. Doctors can seldom distinguish between ganglion and synovial cysts with the naked eye. Only after your doctor has removed and examined the cyst will they be able to identify the difference.
A synovial cyst is surrounded by a thin layer of tissue (synovium). This tissue does not exist in a ganglion cyst. Your doctor, however, will not need to distinguish between them because they are being treated the same manner.
Conclusion
Synovial cysts are fluid-filled sacs that form as a result of degeneration in the facet joints of the lumbar spine (low back). If these sacs get large enough, they can induce spinal stenosis, which is a narrowing of the spinal canal that puts pressure on spinal nerves and produces discomfort.
The fluid-filled sac causes pressure inside the spinal canal, which can cause all of the symptoms of spinal stenosis. Spinal stenosis is a disorder that arises when facet joint deterioration puts pressure on the nerves as they depart the spine.
The therapy for synovial cysts that produce symptomatic lumbar stenosis is generally the same as for other types of lumbar spinal stenosis, with the exception that there is frequently associated spinal instability at the same joint that must be considered if surgery is required.