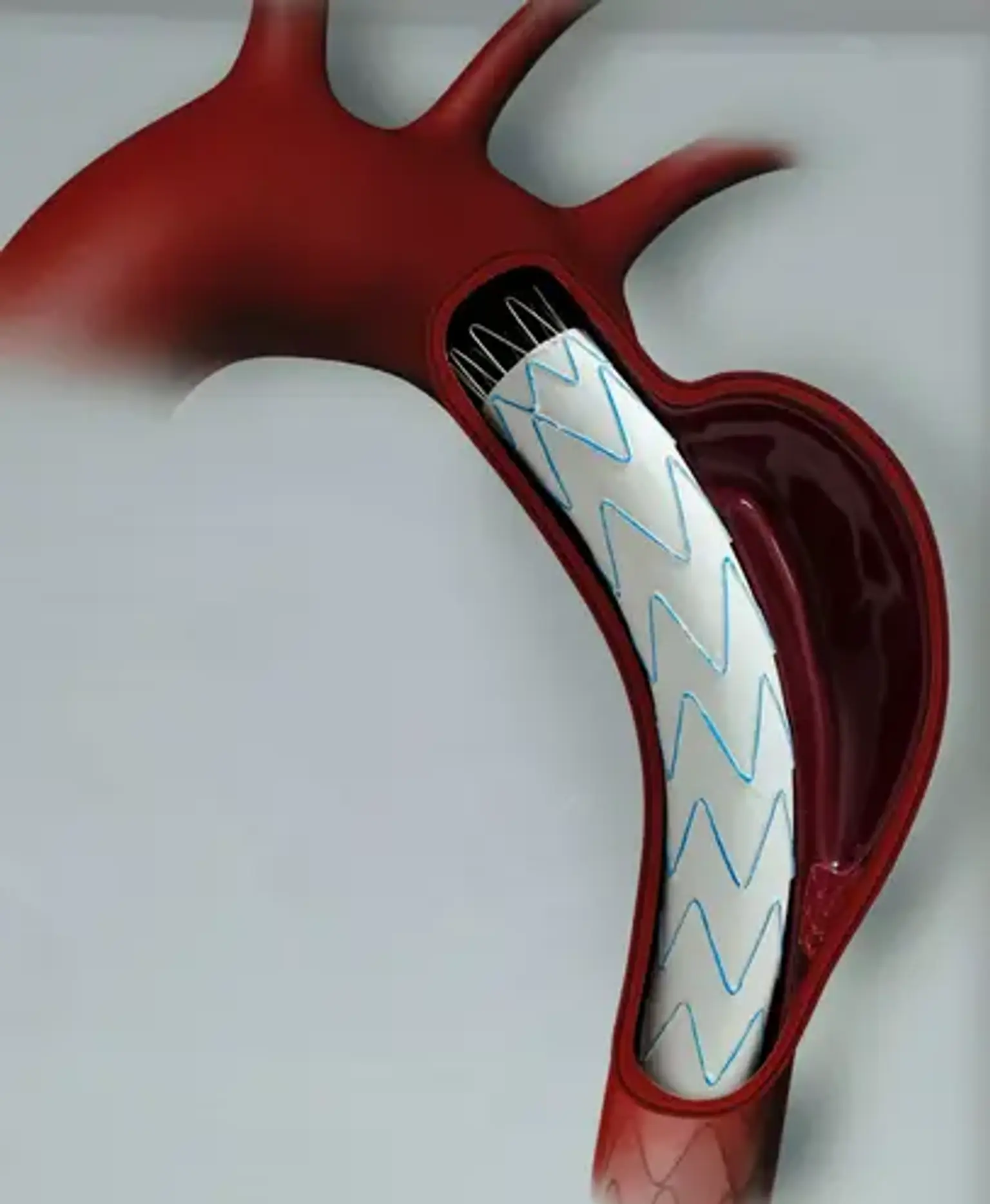
Thoracic Endovascular Aortic Repair (TEVAR)
Overview
The aorta is the biggest artery in your body. It is responsible for transporting oxygen-rich blood from your heart to the rest of your body. It travels from your heart to your chest and into your stomach (abdomen). It then separates into blood vessels, which supply blood to your legs.
A weak region of the aorta may bulge out at times. This is known as an aortic aneurysm. Aortic aneurysms are dangerous because they can rupture. As the aneurysm rises in size, the danger of rupture increases. Treatment is determined on the size of the aneurysm. Treatment is also determined by how quickly the aneurysm grows.
Your healthcare provider may recommend TEVAR to fix an aneurysm in the part of the aorta that is in your chest. This is called the thoracic area.
TEVAR (thoracic endovascular aortic repair) is a treatment used to treat an aneurysm in the upper aorta. The aorta is the biggest artery in your body. An aneurysm is a weak, bulging section of the aorta's wall. It can be fatal if it bursts (ruptures).
TEVAR is a minimally invasive surgical procedure. That is, it is completed with a little cut (incision). TEVAR uses a device known as a stent graft to strengthen the aneurysm. A stent graft is a fabric-covered metal tube. It aids in preventing the aneurysm from exploding.
What Causes Thoracic Aortic Aneurysm?
Ascending aortic aneurysms may be fatal due to their liability to dissect or rupture. Approximately 50% of patients with acute untreated ascending aortic dissections die within 48 hours, and those undergoing emergency surgery have 15%-26% mortality. Elective surgery lowers mortality to only 3%-5%. Understanding the pathophysiology of ascending aortic aneurysms can help reduce the morbidity and mortality from aortic dissections or ruptures by indicating timely elective endovascular surgery.
- Degenerative changes in elastic media
An ascending aortic aneurysm is a widening (or lengthening) of a weakened section of the ascending aorta. Whereas other aortic aneurysms are connected with atherosclerosis, ascending aortic aneurysms are usually associated with degenerative alterations in elastic media. Cystic medial degeneration affects the medial layer of the ascending aorta by different degrees of elastic fiber fragmentation and smooth muscle atrophy. Although elastic fiber fragmentation is a typical component of the aging process, it can occasionally accelerate and cause partial or full loss of elastic fibers and smooth muscle cells in the aortic medial layer. The aortic wall then loses strength and flexibility, becoming aneurysmal and potentially dissecting or rupturing. - Annulo-aortic ectasia and genetic connective tissue disorders
Annulo-aortic ectasia is caused by a combination of the following conditions: 1) ascending aortic aneurysm 2) dilation of the Valsalva sinuses and 3) dilatation of the aortic annulus. Annulo-aortic ectasia can occur as a freestanding condition or as part of a larger connective tissue problem, such as Marfan's syndrome, a genetic disorder that affects fibrillin production, with fibrillin and elastin being basic components of elastic fiber. The aorta with Marfan's syndrome has the classic hallmarks of cystic medial degeneration, including elastic fiber breakdown and medial fibrosis. Aortic root dilatation, with or without accompanying aortic regurgitation, affects up to 85% of people with Marfan's syndrome.
Ehlers-Danlos syndrome is another hereditary connective tissue condition that affects collagen production. Type IV is characterized by spontaneous arterial rupture, most notably in the mesenteric artery. This condition may potentially be linked to fatal results from ascending aortic rupture without dissection. However, ascending aortic aneurysms are less prevalent in Ehlers-Danlos syndrome. - Atherosclerosis and acute aortic dissection
Atherosclerosis can also produce aneurysmal degeneration of the ascending aorta; however, it affects the ascending aorta less frequently. Atherosclerotic processes in the aorta medium disrupt elastic fibers and smooth muscle cells, which are eventually replaced by extracellular matrix and lipids. As time passes, various invasive atheromas form, weakening the aorta wall.
In patients who survive acute aortic dissection, aneurysmal dilatation of the ascending aorta might occur later. These aneurysms develop mostly from the dissected aorta's false lumen and have a greater proclivity to enlarge and rupture than other forms of ascending aortic aneurysms. - Valve malformations and infections
Aortic valve abnormalities, such as bicuspid and unicuspid aortic valves, are related with ascending aortic aneurysms. The same developmental abnormality that emerges as an anomalous valve in ascending aortas of individuals with bicuspid or unicuspid aortic valves may be associated to aneurysmal formation. The fundamental structural defect of the aorta wall is also generated by the subsequent process of post-stenotic aortic dilatation in individuals with stenotic bicuspid or unicuspid aortic valves in this aneurysmal dilatation.
Infection-caused ascending aortic aneurysms are known as mycotic aneurysms. These aneurysms are uncommon and are most typically observed following an episode of valvular endocarditis. A mycotic aneurysm can develop from an infection of the aortic 'jet' lesion or an infection of the intraluminal clot in an atherosclerotic aneurysm. In the past, syphilis was the most prevalent cause of ascending aortic mycotic aneurysm, but it is now uncommon. Syphilitic infection causes aortitis and obliterative endarteritis, followed by vasa vasorum destruction and medial elastic fiber degeneration. Because there is no reversal of post-syphilitic vascular lesions, successful anti-syphilitic therapy typically does not prevent the establishment of an aortic aneurysm. - Arteritis, trauma and pseudoaneurysm
Systemic arteritis such as Takayasu's arteritis, Kawasaki disease, Behçet's disease or giant cell arteritis may involve ascending aorta and initiate formation of an aneurysm. An aseptic inflammatory process in the medial layer of the aorta is presumed to induce medial destruction, which leads to weakening of the aortic wall and potential aneurysm formation or dissection.
Chronic traumatic aneurysms of the ascending aorta are quite uncommon. Patients with acute ascending aortic injuries have a very low mortality probability due to the development of cardiac tamponade and/or concomitant cardiac injuries, and blunt chest traumas most usually involve the descending rather than the ascending aorta. Pseudoaneurysms do not include all of the aortic wall layers. They can form in the ascending aorta as a result of trauma, surgical operations, or infections. Postoperative pseudoaneurysms can form at cannulation sites or along ascending aortic suture lines.
Indications for TEVAR Surgery
Aneurysm diameter is the main indication for elective surgical intervention because it correlates strongly with the risk of the ascending aortic aneurysm dissecting or rupturing. The diameter of an anormal aorta is influenced by age and body mass index. Indications for replacement of the ascending aorta are influenced by aetiology, diameter, and rate of growth of the aneurysm. The indications are as follows:
- Asymptomatic ascending aortic aneurysm >5.0 cm in diameter.
- Symptomatic aneurysm irrespective of size.
- Asymptomatic ascending aortic aneurysm >4.5 cm in patients with Marfan's syndrome.
- Acute dissection or rupture of the ascending aortic aneurysm.
- Pseudoaneurysm or traumatic aneurysm in the ascending aorta.
- Ascending aortic aneurysm >4.5 cm in patients undergoing aortic valve surgery.
- Growth rate of >0.5 cm/y when the ascending aorta is <5.0 cm in diameter.
How Do I Get Ready For TEVAR?
Inquire with your healthcare practitioner about what you should do before TEVAR. The following is a list of common steps you may be requested to do:
- Your healthcare expert will guide you through the procedure. You can ask him or her any concerns you have.
- You will be asked to sign a consent form authorizing the treatment. If anything is unclear, read the form carefully and ask questions.
- Your medical history will be taken, and you may be subjected to a physical exam. This is done to ensure that you are in excellent health before to the treatment. You may also be subjected to blood testing and other diagnostic procedures such as Chest CT.
- Tell your provider if you are pregnant or think you may be pregnant.
- Inform your healthcare practitioner if you are sensitive to or allergic to any medications, latex, iodine, tape, contrast dyes, or anesthetic medications (local and general).
- Inform your doctor about all of the medications you are taking. This covers both OTC and prescription medications. Vitamins, herbs, and other supplements are also included.
- Your doctor may prescribe medications to take in the days leading up to your surgery. These medications can aid in the relaxation of blood vessels, the reduction of blood pressure, and the reduction of the danger of your aortic aneurysm rupture.
- Tell your doctor whether you use any blood-thinning medications, such as warfarin or aspirin, before your operation. These may increase your chances of bleeding during the surgery. To lower your bleeding risk, you may need to discontinue these medications prior to the surgery.
- You will be instructed not to drink or eat anything for many hours before to operation. This usually means no eating or drink after midnight the night before your procedure.
- If you smoke, you should quit as soon as possible before your operation. This can increase your chances of a good surgical recovery. It may also benefit your overall health.
What Happens During TEVAR?
TEVAR is a non-invasive technique. This signifies that a little cut is used (incision). The procedure will be performed by a vascular surgeon and a team of expert healthcare providers. Your doctor can tell you exactly what to expect throughout your procedure. Here's an example of how to accomplish it:
- To avoid pain, you will be given anesthesia. This might be general anesthesia, which would put you to sleep during the surgery. It might also be localized anesthesia, which numbs a specific section of your body.
- During the procedure, a healthcare expert will closely monitor your vital indicators, such as heart rate and blood pressure.
- To access the aortic valve, your surgeon may make a tiny incision in the groin as well as the arm. A sheath, a tiny tube (catheter), will be inserted into the artery.
- A stent graft will be attached to the end of the catheter by your surgeon. The stent graft is a thin metal mesh tube (the stent). A thin polyester cloth covers it (the graft). The tube has been deflated to make it thin enough to fit through your blood artery.
- Your surgeon will thread the catheter with the stent graft connected through an artery in your groin to the damaged area of your aorta using X-rays as a guide.
- When the stent graft is in place, your surgeon will extend the metal frame and secure it.
- The metal frame expands like a spring and is tightly attached to the aortic wall. This creates a steady environment for blood flow. It also prevents the aneurysm from rupturing. The aneurysm's blood supply has now been severed. As a result, it shrinks with time.
- The catheter will be removed by your surgeon. He or she will seal the incision and cover the wound with a tiny bandage.
What Happens After TEVAR?
You will be in a recovery room for many hours following the treatment. Your vital signs, such as heart rate and breathing rate, will be monitored by your healthcare staff. You may need to lie flat for several hours following the surgery to help avoid bleeding.
Expect to be in the hospital for at least 3 to 4 days following surgery. More information on what to expect will be provided by your healthcare provider.
When you leave the hospital, arrange for an adult family member or friend to drive you home.
Recovering at home:
- TEVAR recovery time is less than that of traditional open surgery for an aortic aneurysm.
- For at least four weeks, avoid heavy activities. Inquire with your doctor about when it will be safe to resume driving. Examine the incision site for symptoms of infection. These symptoms include redness, swelling, discomfort, and the formation of a protrusion.
- If you have a fever of 100.4°F (38.0°C) or higher, call your doctor straight once.
- Your doctor may request CT scans at regular intervals. These will look for leaks, graft disintegration, and other issues.
- To avoid blood clots, your physician may advise you to use blood-thinning medications.
- Ask your provider what types of foods to eat and what types of foods to avoid. The recommended diet will depend on all of your healthcare needs.
- Your healthcare team will tell you when to schedule your follow-up appointment to check your progress and recovery.
- Remember to take all your medicines as prescribed.
- Your healthcare provider may give you other instructions, depending on your situation.
Complications of TEVAR
As with any surgical therapy, complications may arise. The most severe complications of TEVAR include the following:
- Stroke (4%).
- Paraplegia/paraparesis (2-15%).
- Peripheral vascular injury.
Stroke can occur because the guide wires used to direct the endografts into position in the aortic arch can dislodge a thrombus or atheroma, which can embolize to the brain via the cerebral arteries. Similarly, emboli can cause limb and mesenteric ischemia.
SCI arises when the intercostal blood vessels supplying the spinal cord are blocked by the stent grafts. In patients who are preoperatively deemed to be at high risk for SCI, a bundled SCI prevention protocol that includes cerebrospinal fluid (CSF) drainage, blood pressure targets (mean arterial pressure >90 mm Hg), transfusion goals (hemoglobin >9 g/dL), and pharmacologic adjuncts (eg, steroids or naloxone) is used..
The passage of the stent grafts might harm the femoral and iliac arteries in individuals with tiny iliac arteries (access vessels). The most concerning problem is full artery avulsion, which can be managed by balloon occlusion; this is why guide wires must be retained in place until the very end of the case. Concerns about these infrequent but large vascular catastrophes are one of the reasons why TEVAR should only be done by surgeons who have expertise with open repair procedures.
Endoleaks occur when the aneurysm is not completely isolated from the bloodstream. In the TAG trial, such leaks were found in 6% of patients at 1 year and in 9% at 2 years. Although device improvements have led to significant reductions in endoleak rates, this potential complication remains a strong consideration in evaluating patients' anatomy and determining the appropriate device selection for each individual anatomic configuration. Accordingly, it is important to emphasize that patients undergoing TEVAR require lifelong follow-up with CT scans (eventually annually but initially more frequently).
Endoleaks are commonly classified into four types as follows:
- Type I endoleaks occur when the seal on either end of the stent graft is incomplete.
- Type II endoleaks occur because of back-bleeding from smaller vessels (typically intercostals) that are covered with the endograft.
- Type III endoleaks occur when leakage develops between overlapping stent grafts.
- Type IV endoleaks were seen with earlier stent grafts when porosity of the graft material led to seepage of blood components through the graft walls, resulting in tension within the excluded aneurysmal segment; they are rarely seen today.
Conclusion
Endovascular aneurysm repair (EVAR) is a form of minimally invasive endovascular surgery used to treat aortic disease, most often an abdominal aortic aneurysm (AAA). When performed to treat thoracic aortic disease, the operation is known as TEVAR, which stands for "thoracic endovascular aortic/aneurysm repair." The treatment includes inserting an expandable stent graft into the aorta to treat aortic disease without operating directly on the aorta.
TEVAR and endografts for aortic aneurysm and ulcer repair offer the advantages of minimally invasive surgery, including:
- Smaller incision.
- Less pain.
- Shorter recovery.
- Fewer medical complications, including infection.
While TEVAR is a minimally invasive procedure, you may still benefit from cardiac rehabilitation delivered by a team of specialists. Cardiac rehab occurs in an outpatient setting and includes exercise, nutrition, education and support.